Abstract
Objectives
Objectives were to examine subjective sleep quality and daytime sleepiness of the German ice hockey junior national team prior to the world championship to identify athletes of concern and areas of optimization with the intention of equally preventing injury and enhancing performance.
Methods
Twenty-one athletes (Mage = 18.5 ± 0.6 years, Mheight = 181.7 ± 4.3 cm, Mweight = 81.4 ± 7.1 kg), playing for national (n = 13) and international (n = 8) home clubs, answered the Pittsburgh Sleep Quality Index (PSQI) and Epworth Sleepiness Scale (ESS) before training camp (T1, day 1) and prior to tournament (T2, day 11).
Results
Overall, 9 players at T1 and 7 at T2 were identified as bad sleepers (PSQI > 5), while high sleepiness (ESS > 10) was found for 6 athletes at each measurement time. Group means and standard deviations reduced descriptively for PSQI (T1 = 5.38 ± 2.31, T2 = 4.57 ± 2.36) and ESS (T1 = 9.24 ± 3.74, T2 = 8.48 ± 3.28). Tendential differences were visible for PSQI in international-based players (Z = −1.7, p = 0.09) and ESS in first-national-league players (Z = −1.73, p = 0.08) over time. Higher PSQI values for international-based players (6.25 ± 2.6) were found compared to first-national-league (5.83 ± 1.60) and lower-league players (4.00 ± 2.08), with large effect sizes for lower-league compared to international (d = 0.95) and national players (d = 0.98) at T1 and small effect sizes compared to first-league players (d = 0.24) at T2.
Conclusion
Findings emphasize great vulnerability and individuality and underline the importance of intraindividual sleep monitoring to meet the requirements needed to equally obtain health and enhance overall performance.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Successful elite athletes do not only need to be dedicated to a hard and focused training, but also attain a sufficient balance between individual training stress and adequate recovery (Kellmann et al., 2018). In this manner, sleep is becoming broadly credited as vital for optimal heath, well-being and athlete performance (Halson, 2019), as it is an essential factor for physiological and psychological recovery (Adam & Oswald, 1984; Halson, 2014; Lastella et al., 2018), which athletes name as one of their main means of recovery (Venter, 2014). Overall, better self-reported sleep quality is evident with higher total quality of recovery (Wilke et al., 2020). Furthermore, an athlete’s total amount of sleep, his or her sleep quality, and the timing of sleep periods are considered to be essential components influencing the ability to train, to maximize the training response, and to recover and perform (Sargent, Halson, & Roach, 2014). On the other hand, shortened sleep can lead to sleepiness (Axelsson et al., 2009), an increase in reaction time (Postolache et al., 2005), a decline in psychomotor performance (Reilly & Edwards, 2007), unstable mood, difficulties in memory and learning processes, troubled metabolism, and even higher risk of illness and injury (Halson, 2014). In addition, improvement of pretraining sleep quality is believed to have a positive impact on players’ well-being and movement strategy (Lalor, Halson, Tran, Kemp, & Cormack, 2020). Altogether, sleep is a key element of obtaining health and enhancing performance. Yet, poor sleep quality is found in a large number of athletes (Caia, Kelly, & Halson, 2018; Silva et al., 2019).
There are a variety of explanations for poor sleep in athletes. Some can be tackled through appropriate education and behaviour change strategies (Driller, Lastella, & Sharp, 2019); others mostly relate to the overall elite athlete’s lifestyle and are more difficult to manage, as they are influenced by the elite sports system itself (Halson, 2019). Troubling factors may not only be nervousness or rumination ahead of competition (Juliff, Halson, & Pfeiffer, 2015), but also a lack in consistent bed time hours and routines, sleep in unfamiliar environment and early rising times due to training and competition schedules (Caia et al., 2018; Kölling, Duffield, Erlacher, Venter, & Halson, 2019). Furthermore, travel may induce sleep disruption (Halson, Romyn, & Cort, 2020) and increase perceptual fatigue and suppressed lower-body power (Fowler, Duffield, Morrow, Roach, & Vaile, 2015) and influence an athlete’s circadian rhythm, while late-night start-up, bright stadium lighting and result-dependent mood might influence an athlete’s circadian rhythm and lead to prolonged sleep onset (Fullagar et al., 2016). Other factors such as nutritional intake, caffeine consumption, muscle soreness, injury, and social media/video games are anecdotally reported to have a profound impact on an athlete’s sleep if not managed proficiently (Halson, 2019; Halson et al., 2020).
Ice hockey is a rapid, intermittent contact sport, characterized by high-intensity load phases with explosive dynamic movement sequences (Lignell, Fransson, Krustrup, & Mohr, 2018). It is further known for its speed, skill, and aggression and consequently labelled as a high-risk sport (Adams, Mason, & Robidoux, 2015). Thus, ice hockey athletes are highly vulnerable to severe injuries like concussions. As these kind of head injuries can cause serious and at times debilitating short- and long-term effects on players, injury prevention should be a highly prioritized aim for athletes and coaches (Caron, Bloom, Johnston, & Sabiston, 2013; Johnson, 2011). For this reason, physical and mental readiness is of tremendous importance within the sport, in order to not only stabilize the quality of performance, but also prevent injury (Loch, Hof zum Berge, Kölling, & Kellmann, 2020). Yet, sports requiring speed, tactical strategy, and technical skill are most sensitive to sleep duration manipulations (Kirschen, Jones, & Hale, 2018) and for many ice hockey players sleep disturbing factors like late-night start up, bright stadium lightning, and pressure to perform are part of their everyday life as professional athletes. Further, most athletes are obligated to undertake significant travel in order to reach their competition venues, with potential consequences for both physiological and psychological status and potential harm to their performance capability (Halson et al., 2020). In a study by Tuomilehto et al. (2017) 107 professional ice hockey players participated in an exploratory observational 1‑year follow-up study which consisted of a questionnaire-based sleep assessment followed by a general sleep counselling and, when needed, polysomnography and an individual treatment plan. As a result, one in every four players was found to have a significant problem in sleeping and three in every four players considered that counselling would improve their performance (Tuomilehto et al., 2017). Nevertheless, studies assessing sleep in ice hockey players are scarce and further studies are urgently needed in order to understand the specific needs and demands of the sporting discipline itself and its specific competition set-ups in order to implement sport specific interventions.
During the junior world championship, a team plays five games within one week. A well-balanced recovery-stress state prior to competition, therefore, is essential to successfully sustain this intense competition phase (Kellmann & Kölling, 2019). Furthermore, travel to competition venue may vary within a national team as players arrive directly from national or international clubs and previous sleep-environments and conditions may differ due to different competition schedules. Henceforth, differences in fatigue within a national team may occur. Consequently, it is particularly interesting to examine to what extent sleep disturbances prior to a world championship may occur. However, as the importance of the competition limits the possibilities to assess sleep quality without interfering with the players’ routines, the implementation of a subjective sleep questionnaires and sleep-logs seems to be a compromising option to be utilised due to their ease of administration (Halson, 2019; Kölling & Hof zum Berge, 2020).
Thus, the aim of the study is to subjectively assess sleep, its quality, and overall daytime sleepiness of the German male ice hockey junior national team during a training camp prior to the IIHF (International Ice Hockey Federation) U20 division IA world championship. It is hypothesised that values differ depending on location and league of home clubs, with players arriving from overseas having more trouble sleeping than those already stationed in Germany.
Materials and methods
Participants
Of the 28 male players on the preselective German squad, 21 players were included in the study results (Mheight = 181.7 ± 4.3 cm, Mweight = 81.4 ± 7.1 kg). Two players had missed the first assessment because of obligations at their home clubs, four players had to leave the team before the second assessment as they were not selected for the final squad, and one player left early due to an injury. All players were under the age of 20 (Mage = 18.5 ± 0.6 years).
Six players of the team were contracted within the German first national league, seven players were part of a lower league team, and eight athletes were playing for internationally based teams in North America (n = 7) and Sweden (n = 1). Players arrived directly from their national and international home clubs. As the world championship was held in Germany, players stayed at the same hotel for training camp and tournament and no further travel was required at any point. Participants shared rooms in pairs of two. Time in bed and wake-up time in the morning were delimited, as mandatory breakfast time and night-time curfew were predetermined by the coach. Meals were at all times provided for the athletes within the team hotel or training facilities and athletes were encouraged to keep nutrition habits stable. Yet, athletes did not have to follow a specific nutrition protocol. Furthermore, athletes were encouraged to weigh-in before and after ice-times in order to prevent dehydration.
Procedure
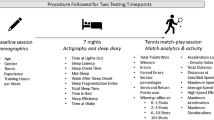
While the camp was set up to acclimate athletes within the tournament environment and aims to improve overall recovery, the study procedure was implemented to identify athletes of concern and areas of optimisation to efficiently target sleep optimisation in preparation for future competitions in order to prevent injury and enhance performance. Therefore, athletes were asked to answer German paper–pencil versions of the Pittsburgh Sleep Quality Index and Epworth Sleepiness Scale at arrival of preparational training camp (T1, day 1) and on the evening before the first game of the tournament (T2, day 11), as well as a short sleep-log prior to falling asleep and right after waking up in the morning. Questionnaires and logs were answered pseudonymised to secure confidentiality and compliance of athletes without the fear of results being used as nomination criteria. Written informed consent from all players was obtained and purpose and procedure were explained prior to assessment. Further, the study was approved by the local ethics committee.
Pittsburgh Sleep Quality Index
Overall sleep quality was assessed with the 19 items of the Pittsburgh Sleep Quality Index (PSQI). The PSQI is a retrospective, self-reported measure with overall values ranging from 0–21 and higher values indicating a decline in sleep quality. The original version of the PSQI is set-up to assess overall sleep in the period of the last month. In order to meet the specific requirements of the study set-up, however, the questionnaire instruction was adapted to a period of the last 10 days. Participants rate several aspects of their sleep, which add up to six specific component scores (e.g., sleep onset latency) and one summary global Sleep Quality Index (SQI). Its original cut-off value is set to five and divides good from bad sleepers. Previous studies have documented reliability and validity of the PSQI with a sensitivity of 89.6% and a specificity of 86.5% for detecting sleep insomnia (Backhaus, Junghanns, Broocks, Riemann, & Hohagen, 2002; Buysse, Reynolds, Monk, Berman, & Kupfer, 1989). It is perhaps the most commonly used subjective sleep measure not only in the research literature, but also in the sleep community (Driller et al., 2019). Further, the PSQI has been applied in various types of sport and is therefore not limited to a clinical sleep setting only (Ehrlenspiel & Erlacher, 2018; Hoshikawa, Uchida, & Hirano, 2018; Swinbourne, Gill, Vaile, & Smart, 2016). According to Driller, Mah, and Halson (2018), the average score for athletes is 5.1 ± 2.5 (in comparison to nonathletes; 6.1 ± 2.9).
Epworth Sleepiness Scale
The Epworth Sleepiness Scale (ESS) measures likelihood of falling asleep in eight common settings (on a scale 0–3) with higher values indicating a superior chance of dozing off. It is a self-reported, 8‑item questionnaire with a global score from 0–24 and scores greater than ten suggesting significant daytime sleepiness (Johns, 1991; Pilcher et al., 2018). The ESS is a simple and reliable method with a high level of internal consistency (Johns, 1992) and has been used to assess daytime sleepiness in various individual and team sports. A study with collegiate basketball players uncovered relatively high scores with a mean value of 9.64 ± 3.80 at baseline measurement in comparison to a mean value of 3.36 ± 1.69 at the end of a 5- to 7‑week sleep extension period (Mah et al., 2011). A recent sample by Driller et al. (2018) revealed means of 5.7 ± 3.4 for athletes, compared to 5.2 ± 3.3 for nonathletes.
Statistical analysis
Descriptive statistics are presented as means ± standard deviation. Statistical analysis was performed using SPSS V.25 (IBM Corporation; Chicago, IL, USA). Global scores for each questionnaire were normally distributed, as assessed by Kolmogorov–Smirnow test (p > 0.05), and homogeneity of variances was assessed by Levene’s test for equality of variances (p > 0.05). Comparison of pre- to postmeasurements were performed for each questionnaire using paired t-tests, with statistical significance set at p < 0.05. Cohen’s effect sizes (d) were calculated between T1 and T2 for each questionnaire and interpreted using thresholds of 0.2, 0.5, 0.8 for small, moderate, and large, respectively (Cohen, 1988). Confidence limits for, and inferences about, the true values of effect statistics were assessed via magnitude-based inferences according to Hopkins and Batterham (2018) with threshold values of 0.00–0.19, 0.20–0.59, 0.60–1.19, ≥1.20 being considered trivial, small, moderate, and large. Test–retest reliability was assessed with Pearson correlations. As group sizes were too small to use parametric tests, Kruskal–Wallis tests were used for differences in-between groups and Mann–Whitney U‑tests were performed for differences within groups over time.
Results
Results indicate no significant change in PSQI values between the two measurements, with only small effect size. As seen in Table 1, however, means and standard deviations reduce descriptively from T1 to T2. Of the 21 athletes, 9 players at T1 (42.9%) and 7 players at T2 (33.3%) were identified as bad sleepers using the PSQI cut-off value of five (Buysse et al., 1989). In this manner, 5 athletes changed from bad to good sleepers (23.8%) when comparing T1 and T2, 13 athletes were categorized equally at both measurements (61.9%) and 3 athletes transitioned from good to bad sleepers (14.3%). Individual discrepancies between T1 and T2 are represented in Fig. 1, with positive values showing an increase in sleep quality and negative values implying a decline. Correspondingly, small effects of qualitative inference of effect magnitude within 90% confidence intervals (0.81 ± 1.1) were found, with an 84.9% chance of true value of effect statistic being beneficial.
Individual differences in PSQI and ESS values between T1 and T2. PSQI Pittsburgh Sleep Quality Index, ESS Epworth Sleepiness Scale, T1 before training camp, T2 before competition. Positive values indicate an increase in sleep quality for PSQI and decrease in daytime sleepiness for ESS. The dotted lines represent the mean difference (PSQI = 0.81; ESS = 0.76), the area of trivial effect size is highlighted in grey
ESS values appear to be concerningly high (> 10) for 6 athletes (28.6%) at both T1 and T2, with, however, rather small test–retest reliability (r = 0.46). While 15 players were categorized equally (71.4%) at both measurements, 3 athletes reduced (14.3%) and 3 athletes increased (14.3%) their daytime sleepiness with the result of being categorized differently. Individual differences between measurements are represented in Fig. 1, showing an increase in daytime sleepiness for negative values and a decrease of sleepiness for positive values. Unclear effects of qualitative inference of effect magnitude within 90% confidence intervals (0.76 ± 2.9) were observed, with a 50.8% chance of true value of effect statistic being beneficial, 39.6% being trivial and 9.5% being harmful. While a mean difference of 0.76 between ESS measurements T1–T2 indicates an overall decline in daytime sleepiness, no significant change in values was found.
When divided by league, tendential differences over time are visible for PSQI in international players (Z = −1.7, p = 0.09), with moderate effects of qualitative inference of effect magnitude within 90% confidence intervals (1.9 ± 1.7) and a most likely beneficial development from T1 to T2. For ESS, tendential differences are visible in national-league players (Z = −1.73, p = 0.08), with small effects of qualitative inference of effect magnitude (1.2 ± 0.9) as represented in Fig. 2. Yet, no group differences were found for either questionnaire, neither at the first nor at the second measurement. Descriptive data, as represented in Fig. 3, however, show higher PSQI values for internationally-based players (6.25 ± 2.6) compared to first-national league players (5.83 ± 1.60) and lower-leagued athletes (4.00 ± 2.08), with large effect sizes for lower-leagued players compared to international players (d = 0.95) and national players (d = 0.98) at T1. At T2, only small effect sizes were found compared to first-league players (d = 0.24).
Standardised differences in T1 to T2 changes (±90% confidence intervals) when divided by level and location of home-clubs (lower-leagued players: n = 7, first league players: n = 6; international players: n = 8). PSQI Pittsburgh Sleep Quality Index, ESS Epworth Sleepiness Scale, T1 before training camp, T2 before competition. Positive values indicate an increase in sleep quality for PSQI and decrease in daytime sleepiness for ESS. The dotted lines represent the overall mean difference (PSQI = 0.81; ESS = 0.76), the area of trivial effect size is highlighted in grey
Discussion
The aim of the study was to observe subjective sleep quality and daytime sleepiness in German ice hockey players at arrival and prior to the world championship to efficiently target sleep optimisation in preparation for future competitions to likewise prevent injury and enhance performance. Results imply that sleep is highly vulnerable, with international and first-league players showing higher sleepiness and reduced sleep quality prior to training camp. Intense training schedules and tightly scheduled travelling might be influencing factors for this. Longer travelling distances and time-zone changes for international players might have a further impact on reduced sleep quality at first measurement (Caia et al., 2018). Although one of the international players did not arrive from overseas, he was still included in the study results, as no significant changes were found when excluded from analysis. Similarities to North American players might be explainable by requirements of the Swedish Hockey League to travel beyond the arctic circle for league games and the general fact that international travel to competition venue had taken place, as general home advantage for players travelling within a country seems to occur (Balmer, Nevill, & Williams, 2001). Thus, an overall strength of the study is the variety of travelling distances within one single team, which can only be attained during an international but home-based tournament. By and large, it can be hypothesized that travel might have had an influence on the circadian rhythm, the overall comfort as well as the nutritional intake with consequences for both physiological and psychological status (Halson et al., 2020). Yet, this study did not examine the specific reasons for lower sleep quality in athletes from overseas. Hence, further studies should have a more detailed look on the specific reasons in order to implement an individually tailored sleep management.
The descriptive decline in PSQI and ESS values at the second measurement time might be due to the reduced training sessions during preparation and short distances between ice rink and hotel without additional travelling required. Further, descriptive decline in standard deviations indicate an approximation of sleep behaviour within the team. Yet effect sizes were small, indicating that sleep quality was not only influenced by acute factors such as travelling to training camp. Still, some players, contrarily to group means, showed an increase in either ESS or PSQI, or even both questionnaires. A possible explanation might be that those players are more sensitive to shared rooms, adaptation to new environment, or they experienced an actual individual increase in training intervals or intensity. Furthermore, the nomination bouts for the world championship during the preparational training camp might have been more stressful for some players compared to those already having a rather stable spot on the team, with nervousness having a negative impact on sleep quality. Athletes experiencing pressure to perform or emotional tension should, therefore, always reflect whether it is a performance enhancing or inhibiting state of tension (Ehrlenspiel & Erlacher, 2018; Ehrlenspiel, Erlacher, & Ziegler, 2018). While grouping of athletes might help to delimit causes for insatiable sleep, results underline that sleep is highly individual and must always be examined on the personal level as well.
As there has not been a baseline measurement or follow-up during off-season, chances are that sleep quality and sleepiness were further influenced by seasonal circumstances and the upcoming championship and do not represent stable values throughout the year. In addition to the small group size, quick adaptation to and changes in sleep environment might explain relatively low test–retest reliability for both questionnaires and underline high vulnerability of sleep even more. Further work with the athletes should therefore target the reasons for occasionally reduced sleep quality to implement purposeful interventions like sleep education, the practice of sleep hygiene rules, detachment strategies or cognitive restructuring of thoughts to equip athletes with functioning tools to counteract intermittently appearing sleep disturbances (Driller et al., 2019). Additionally, the education of coaches on sleep hygiene could help to address and improve sleep knowledge (Miles, Clark, Fowler, Miller, & Pumpa, 2019).
Nonetheless, one limitation of the study is that sleep questionnaires are always subjectively recaptured and therefore influenced by patient expectations, recall bias, or memory impairments (Martin & Hakim, 2011). Therefore, they do not replace an objective sleep recording to identify clinical sleep tendencies or even disorders. Yet, the implementation of a sleep disorder screening included into the medical check of athletes, as suggested by Hoshikawa et al. (2018), may be desirable to identify players with severe values right away and to initiate further objective sleep analysis to either diagnose or exclude a sleep disorder that might need specific treatment. Both ESS and PSQI therefore seem to be a reliable fit, as they have been correlated to objective sleep measurements and hence are efficient indicators to identify players who might need further attention. Yet, the adaptation of the PSQI to fit the study set-up should be kept in mind when interpreting the data. Further, both questionnaires do not provide questions specifically tailored to professional athletes and therefore do not include challenges faced by elite athletes only (Driller et al., 2018).
While questionnaires can detect concerning sleep behaviours, they do not show to what extent those disturbances have an actual impact on the player’s performance. However, an increasing body of research documents global performance impairments and negative health effects following sleep loss, which directly link to athletic performance potential (Fullagar et al., 2015; Simpson, Gibbs, & Matheson, 2017). New study results further stress the bidirectional associations between sleep, mental strain, and training load and exhibit the detrimental effects of mental strain on sleep, likely caused by mental activation incompatible with sleep. For this reason, an increased need for recovery is associated with subsequent self-regulatory reduction of training loads by the athletes with increasing deep sleep in poor sleepers suggesting an elevated need for physiological recovery (Hrozanova, Klöckner, Sandbakk, Pallesen, & Moen, 2020). Yet, although a third of all players showed severe lack in sleep quality and highly increased daytime sleepiness was found in almost a third of the team, the German team won the tournament. Therefore, the question needs to be raised whether improved values in sleep could further improve performance or if otherwise, sleep quality might even be neglectable during a limited time of a tournament. Future research, therefore, should aim for an assessment of both precompetition and off-season assessment to differentiate between short-term and long-term sleep restriction and sleepiness.
Although the influence of sleep on the competition result remains unknown, adolescents with restricted sleep are found to be 1.7 times more likely to experience a significant injury (Milewski et al., 2014). A decrease in reaction time and cognitive abilities due to reduced sleep is likely to contribute to this increased injury risk (Simpson et al., 2017). Therefore, an efficient recovery-stress state, both mentally and physically, is fundamental not only to stabilize the quality of performance, but also to prevent injury. As a greatly impacting factor, sufficient sleep in elite athletes, therefore, is a key element.
Perspective work with athletes of concern should, therefore, target the implementation of an adequate and individual sleep monitoring as a first step, to later introduce effective tools to counteract and obstruct sleep disturbances (Hof zum Berge, Ferrauti, Meyer, Pfeiffer, & Kellmann, 2020; Hof zum Berge et al., 2020). Moreover, raising awareness in coaches and athletes for the wide-ranging consequences of inadequate sleep may encourage athletes to priorities obtaining optimal sleep with the consequence of reducing daytime sleepiness in the future.
References
Adam, K., & Oswald, I. (1984). Sleep helps healing. British Medical Journal, 289(6456), 1400–1401. https://doi.org/10.1136/bmj.289.6456.1400.
Adams, S., Mason, C. W., & Robidoux, M. A. (2015). ‘If you don’t want to get hurt, don’t play hockey’: the uneasy efforts of hockey injury prevention in Canada. Sociology of Sport Journal, 32(3), 248–265. https://doi.org/10.1123/ssj.2014-0092.
Axelsson, J., Kecklund, G., Åkerstedt, T., Donofrio, P., Lekander, M., & Ingre, M. (2009). Sleepiness and performance in response to repeated sleep restriction and subsequent recovery during semi-laboratory conditions. Chronobiology International, 25(2), 297–308. https://doi.org/10.1080/07420520802107031.
Backhaus, J., Junghanns, K., Broocks, A., Riemann, D., & Hohagen, F. (2002). Test-retest reliability and validity of the Pittsburgh Sleep Quality Index in primary insomnia. Journal of Psychosomatic Research, 53(3), 737–740. https://doi.org/10.1016/s0022-3999(02)00330-6.
Balmer, N. J., Nevill, A. M., & Williams, A. M. (2001). Home advantage in the Winter Olympics (1908–1998). Journal of Sports Sciences, 19(2), 129–139. https://doi.org/10.1080/026404101300036334.
Buysse, D. J., Reynolds, C. F., Monk, T. H., Berman, S. R., & Kupfer, D. J. (1989). The Pittsburgh sleep quality index: a new instrument for psychiatric practice and research. Psychiatry Research, 28(2), 193–213. https://doi.org/10.1016/0165-1781(89)90047-4.
Caia, J., Kelly, V. G., & Halson, S. L. (2018). The role of sleep in maximising performance in elite athletes. In M. Kellmann & J. Beckmann (Eds.), Sport, recovery, and performance: interdisciplinary insights (pp. 151–167). London: Routledge.
Caron, J. G., Bloom, G. A., Johnston, K. M., & Sabiston, C. M. (2013). Effects of multiple concussions on retired national hockey league players. Journal of Sport & Exercise Psychology, 35(2), 168–179. https://doi.org/10.1123/jsep.35.2.168.
Cohen, J. (1988). Statistical power analysis for the behavioral sciences. Mahwah: Lawrence Erlbaum.
Driller, M. W., Mah, C. D., & Halson, S. (2018). Development of the athlete sleep behavior questionnaire: a tool for identifying maladaptive sleep practices in elite athletes. Sleep Science, 11(1), 37–44. https://doi.org/10.5935/1984-0063.20180009.
Driller, M. W., Lastella, M., & Sharp, A. P. (2019). Individualized sleep education improves subjective and objective sleep indices in elite cricket athletes: a pilot study. Journal of Sports Sciences, 37(17), 2021–2025. https://doi.org/10.1080/02640414.2019.1616900.
Ehrlenspiel, F., & Erlacher, D. (2018). Sleep, dreams, and athletic performance. In M. Kellmann & J. Beckmann (Eds.), Sport, recovery, and performance: interdisciplinary insights (pp. 168–182). Abingdon: Routledge.
Ehrlenspiel, F., Erlacher, D., & Ziegler, M. (2018). Changes in subjective sleep quality before a competition and their relation to competitive anxiety. Behavioral Sleep Medicine, 16(6), 553–568. https://doi.org/10.1080/15402002.2016.1253012.
Fowler, P. M., Duffield, R., Morrow, I., Roach, G., & Vaile, J. (2015). Effects of sleep hygiene and artificial bright light interventions on recovery from simulated international air travel. European Journal of Applied Physiology, 115(3), 541–553.
Fullagar, H. H. K., Duffield, R., Skorski, S., White, D., Bloomfield, J., Kölling, S., & Meyer, T. (2016). Sleep, travel, and recovery responses of national footballers during and after long-haul in-ternational air travel. International Journal of Sports Physiology and Performance, 11(1), 86–95. https://doi.org/10.1007/s00421-014-3043-2.
Fullagar, H. H. K., Skorski, S., Duffield, R., Hammes, D., Coutts, A. J., & Meyer, T. (2015). Sleep and athletic performance: the effects of sleep loss on exercise performance, and physiological and cognitive responses to exercise. Sports Medicine, 45(2), 161–186. https://doi.org/10.1007/s40279-014-0260-0.
Halson, S. L. (2014). Sleep in elite athletes and nutritional interventions to enhance sleep. Sports Medicine, 44(Suppl 1), S13–S23. https://doi.org/10.1007/s40279-014-0147-0.
Halson, S. L. (2019). Sleep monitoring in athletes: motivation, methods, miscalculations and why it matters. Sports Medicine. https://doi.org/10.1007/s40279-019-01119-4.
Halson, S. L., Romyn, G., & Cort, M. (2020). Travelling athletes. In R. Belski, A. Forsyth & E. Mantzioris (Eds.), Nutrition for sport, exercise and performance (pp. 321–335). Abingdon: Routledge.
Hof zum Berge, A., Ferrauti, A., Meyer, T., Pfeiffer, M., & Kellmann, M. (2020). Portable polysomnography for sleep monitoring in elite youth rowing: an athlete’s gain or the sleep’s thief? Translational Sports Medicine. https://doi.org/10.1002/tsm2.205.
Hof zum Berge, A., Kellmann, M., Kallweit, U., Mir, S., Gieselmann, A., Meyer, T., Ferrauti, A., Pfeiffer, M., & Kölling, S. (2020). Portable PSG for sleep stage monitoring in sports: assessment of SOMNOwatch plus EEG. European Journal of Sport Science, 20(6), 713–721. https://doi.org/10.1080/17461391.2019.1659421.
Hopkins, W. G., & Batterham, A. M. (2018). The vindication of magnitude-based inference. Sportscience, 22, 19–29.
Hoshikawa, M., Uchida, S., & Hirano, Y. (2018). A subjective assessment of the prevalence and factors associated with poor sleep quality. Sports Medicine Open. https://doi.org/10.1186/s40798-018-0122-7.
Hrozanova, M., Klöckner, C. A., Sandbakk, Ø., Pallesen, S., & Moen, F. (2020). Reciprocal associations between sleep, mental strain, and training load in junior endurance athletes and the role of poor subjective sleep quality. Frontiers in Psychology. https://doi.org/10.3389/fpsyg.2020.545581.
Johns, M. W. (1991). A new method for measuring daytime sleepiness: the Epworth Sleepiness Scale. Sleep, 14(6), 540–545. https://doi.org/10.1093/sleep/14.6.540.
Johns, M. W. (1992). Reliability and factor analysis of the Epworth Sleepiness Scale. Sleep, 15(4), 376–381. https://doi.org/10.1093/sleep/15.4.376.
Johnson, L. S. (2011). Concussion in youth ice hockey: It’s time to break the cycle. Canadian Medical Association Journal, 183(8), 921–924. https://doi.org/10.1503/cmaj.110282.
Juliff, L. E., Halson, S. L., & Pfeiffer, J. J. (2015). Understanding sleep disturbance in athletes prior to important competitions. Journal of Science and Medicine in Sport, 18(1), 13–18. https://doi.org/10.1016/j.jsams.2014.02.007.
Kellmann, M., & Kölling, S. (2019). Recovery and stress in sport: a manual for testing and assessment. Abingdon: Routledge.
Kellmann, M., Bertollo, M., Bosquet, L., Brink, M., Coutts, A. J., Duffield, R., Erlacher, D., Halson, S. L., Hecksteden, A., Heidari, J., Kallus, K. W., Meeusen, R., Mujika, I., Robazza, C., Skorski, S., Venter, R., & Beckmann, J. (2018). Recovery and performance in sport: consensus statement. International Journal of Sports Physiology and Performance, 13(2), 240–245. https://doi.org/10.1123/ijspp.2017-0759.
Kirschen, G. W., Jones, J. J., & Hale, L. (2018). The impact of sleep duration on performance among competitive athletes. Clinical Journal of Sport Medicine. https://doi.org/10.1097/jsm.0000000000000622.
Kölling, S., & Hof zum Berge, A. (2020). The effects of subjective and objective sleep monitoring on sleep patterns and attitudes. OBM Neurobiology. https://doi.org/10.21926/obm.neurobiol.2001052.
Kölling, S., Duffield, R., Erlacher, D., Venter, R., & Halson, S. (2019). Sleep-related issues for recovery and performance in athletes. International Journal of Sports Physiology and Performance, 14, 144–148. https://doi.org/10.1123/ijspp.2017-0746.
Lalor, B. J., Halson, S. L., Tran, J., Kemp, J. G., & Cormack, S. J. (2020). A complex relationship: Sleep, external training load, and well-being in elite Australian footballers. International Journal of Sports Physiology and Performance. https://doi.org/10.1123/ijspp.2019-0061.
Lastella, M., Vincent, G. E., Duffield, R., Roach, G. D., Halson, S. L., Heales, L. J., & Sargent, C. (2018). Can sleep be used as an indicator of overreaching and overtraining in athletes? Frontiers in Physiology. https://doi.org/10.3389/fphys.2018.00436.
Lignell, E., Fransson, D., Krustrup, P., & Mohr, M. (2018). Analysis of high-intensity skating in top-class ice hockey match-play in relation to training status and muscle damage. Journal of Strength and Conditioning Research, 32(5), 1303–1310. https://doi.org/10.1519/jsc.0000000000001999.
Loch, F., Hof zum Berge, A., Kölling, S., & Kellmann, M. (2020). Stress states, mental fatigue, and the concept of mental recovery in sports. In M. C. Ruiz & C. Robazza (Eds.), Feelings in sport: theory, research, and practical implications for performance and well-being (pp. 235–245). London: Routledge.
Mah, C. D., Mah, K. E., Kezirian, E. J., & Dement, W. C. (2011). The effects of sleep extension on the athletic performance of collegiate basketball players. Sleep, 34(7), 943–950. https://doi.org/10.5665/sleep.1132.
Martin, J. L., & Hakim, A. D. (2011). Wrist actigraphy. Chest, 139(6), 1514–1527. https://doi.org/10.1378/chest.10-1872.
Miles, K. H., Clark, B., Fowler, P. M., Miller, J., & Pumpa, K. L. (2019). Sleep practices implemented by team sport coaches and sports science support staff: a potential avenue to improve athlete sleep? Journal of Science and Medicine in Sport. https://doi.org/10.1016/j.jsams.2019.01.008.
Milewski, M. D., Skaggs, D. L., Bishop, G. A., Pace, J. L., Ibrahim, D. A., Wren, T. A., & Barzdukas, A. (2014). Chronic lack of sleep is associated with increased sports injuries in adolescent athletes. Journal of Pediatric Orthopaedics, 34(2), 129–133. https://doi.org/10.1097/bpo.0000000000000151.
Pilcher, J. J., Switzer, F. S., Munc, A., Donnelly, J., Jellen, J. C., & Lamm, C. (2018). Psychometric properties of the Epworth Sleepiness Scale: a factor analysis and item-response theory approach. Chronobiology International, 35(4), 533–545. https://doi.org/10.1080/07420528.2017.1420075.
Postolache, T. T., Hung, T. M., Rosenthal, R. N., Soriano, J. J., Montes, F., & Stiller, J. W. (2005). Sports chronobiology consultation: from the lab to the arena. Clinics in Sports Medicine, 24(2), 415–456. https://doi.org/10.1016/j.csm.2005.01.001.
Reilly, T., & Edwards, B. (2007). Altered sleep-wake cycles and physical performance in athletes. Physiology & Behavior, 90(2), 274–284. https://doi.org/10.1016/j.physbeh.2006.09.017.
Sargent, C., Halson, S., & Roach, G. D. (2014). Sleep or swim? Early-morning training severely restricts the amount of sleep obtained by elite swimmers. European Journal of Sport Science, 14(Suppl 1), 310–315. https://doi.org/10.1080/17461391.2012.696711.
Silva, A., Narciso, F. V., Rosa, J. P., Rodrigues, D. F., Cruz, A., Tufik, S., Viana, F., Bichara, J. J., Pereira, S. R. D., da Silva, S. C., & Mello, M. T. (2019). Gender differences in sleep patterns and sleep complaints of elite athletes. Sleep Science, 12(4), 242–248. https://doi.org/10.5935/1984-0063.20190084.
Simpson, N. S., Gibbs, E. L., & Matheson, G. O. (2017). Optimizing sleep to maximize performance: implications and recommendations for elite athletes. Scandinavian Journal of Medicine and Science in Sports, 27(3), 266–274. https://doi.org/10.1111/sms.12703.
Swinbourne, R., Gill, N., Vaile, J., & Smart, D. (2016). Prevalence of poor sleep quality, sleepiness and obstructive sleep apnoea risk factors in athletes. European Journal of Sport Science, 16(7), 850–858. https://doi.org/10.1080/17461391.2015.1120781.
Tuomilehto, H., Vuorinen, V.-P., Penttilä, E., Kivimäki, M., Vuorenmaa, M., Venojärvi, M., Airaksinen, O., & Pihlajamäki, J. (2017). Sleep of professional athletes: underexploited potential to improve health and performance. Journal of Sports Sciences, 35(7), 704–710. https://doi.org/10.1080/02640414.2016.1184300.
Venter, R. E. (2014). Perceptions of team athletes on the importance of recovery modalities. European Journal of Sport Science, 14(Suppl 1), S69–S76. https://doi.org/10.1080/17461391.2011.643924.
Wilke, C. F., Wanner, S. P., Santos, W. H. M., Penna, E. M., Ramos, G. P., Nakamura, F. Y., & Duffield, R. (2020). Influence of faster and slower recovery-profile classifications, self-reported sleep, acute training load, and phase of the microcycle on perceived recovery in futsal players. International Journal of Sports Physiology and Performance. https://doi.org/10.1123/ijspp.2019-0201.
Funding
The study was initiated and funded by the German Federal Institute of Sport Science and realized within “RegMan – Optimization of Training and Competition: Management of Regeneration in Elite Sports [grant number IIA1-081901/12-20].
Funding
Open Access funding enabled and organized by Projekt DEAL.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
A. Hof zum Berge, F. Loch, K. Schwarzenbrunner, A. Ferrauti, T. Meyer, M. Pfeiffer and M. Kellmann declare that they have no competing interests.
All procedures performed in studies involving human participants or on human tissue were in accordance with the ethical standards of the institutional and/or national research committee and with the 1975 Helsinki declaration and its later amendments or comparable ethical standards. Informed consent was obtained from all individual participants included in the study.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Hof zum Berge, A., Loch, F., Schwarzenbrunner, K. et al. Assessment of sleep quality and daytime sleepiness in German national ice hockey players preparing for the world championship. Ger J Exerc Sport Res 51, 94–101 (2021). https://doi.org/10.1007/s12662-020-00693-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12662-020-00693-4