Abstract
In this paper, we share our experience in designing and developing a mobile health (mHealth) infrastructure for non-communicable diseases (NCD) in rural areas in Indonesia called NusaHealth. The NusaHealth project builds a digital healthcare infrastructure involving universities, healthcare providers, and communities in an mHealth approach that puts patients at the center of health care. The Design Science Research Methodology (DSRM) framework was adopted in designing the mHealth application. The infrastructure to connect the mobile device network with the hospital information system was also developed. Our finding indicates that designing and developing an mHealth solution for rural areas in developing countries needs comprehensive approach and the implementation process should involve related partners and stakeholders. The NusaHealth was implemented in rural areas in Yogyakarta province in Indonesia. While Yogyakarta province successfully implemented the NusaHealth in rural areas, different activities need to be conducted to enhance community health by developing a formal mHealth system supported by local health district offices’ policies and regulations.
Similar content being viewed by others
Explore related subjects
Find the latest articles, discoveries, and news in related topics.Avoid common mistakes on your manuscript.
1 Introduction
Mobile devices such as smartphones and tablets have changed how the general population seeks medical and health information. As one of the new middle-income countries, Indonesia has Internet penetration of 73.7% of its population have at least one smartphone with Internet connection. These percentages are expected to keep increasing. Most Indonesians use mobile phones to access the Internet (98.3%), while tablets are the second most commonly used mobile devices after smart TV and smart watches. Only 23.4% of the users are using the Internet to access health information through health applications (Hootsuite and Social 2021).
As defined by the World Health Organization (WHO), eHealth (aka digital health) activities are when healthcare services use all means of information and communication technology (ICT) to improve their quality of care. The primary purpose of eHealth programs is to utilize ICT to improve health care service delivery and health outcomes through the strategic use of technologies such as computers, mobile devices, Internet access, and wireless technologies. Mobile health (mHealth), recognized as a subcategory of eHealth, refers to the concept of utilizing eHealth programs on mobile devices. mHealth can be used in most basic mobile phones such as for telephone reminders and short messaging services (SMS). With the increasing trend of smartphones, the innovations could come in the form of applications, a self-contained program or software that is designed for a particular purpose or function (Krishnamoorthy et al. 2021).
Many eHealth initiatives in developing countries are focused on computer-based health information systems and using the Internet to promote the organization of and access to health-related information. Growing interest in the mHealth potential started as wireless networks expanded throughout these countries and mobile devices have become more affordable. Mobile technologies enable eHealth systems to decentralize and extend their reach to remote areas (Hoque et al. 2020).
Morbidity rates related to non-communicable diseases (NCD) have been increasing in the past years. Currently, NCD has dominated the top causes of mortality among Indonesians (Vos et al. 2020). Inactivity trends among the urban population and the doubling of the health burden with the increased elderly population have become serious concerns in Indonesia. More than a quarter of Indonesian adults are overweight or even morbidly obese. Remarkably, 37% of Indonesian children are diagnosed with stunting status (Haddad et al. 2015).
One approach to support NCD eradication programs is to use mobile technology or mHealth. Several mHealth innovations have been developed globally, such as monitoring physical activity, wearable devices, personal health records, and telemedicine (such as teleconsultation and tele-electrocardiogram (ECG) (Royston et al. 2015). These innovations facilitate the interaction between patients and healthcare providers. This is further supported by the increasing number of mobile technology users, both for social media and e-commerce. Some researchers have discussed the mHealth needs and opportunities in developing countries (Chib 2013; Eze et al. 2016). Aside from supporting NCD management, mHealth is also in line with the development of the national health insurance system, tiered referral services, and community-based health approaches where health services are expected to promote a more patient-centered care. Despite the importance of mHealth, its implementation in developing countries has not been widely used (Hoque et al. 2020).
The main contributions of the study are as follows:
-
Design and implementation of a mobile health infrastructure targeting NCD patients using Design Science Research Method.
-
Developing and implementing mobile health application for NCD patients.
-
Share and evaluate the experience and challenges during the implementation in rural areas in Indonesia, which can be used as a reference to another similar project.
-
Survey on mobile health implementation for NCD patients.
The paper studies the design and technical implementation of mHealth in rural areas in Indonesia, discusses the potential of mHealth in developing countries, and considers how early experiences can inform the way forward.
The remainder of the paper is organized as follows. Section 2 presents related work. Section 3 explains our research methodology. In Sect. 4, we present our implementation results. The discussion is presented in Sect. 5. Section 6 presents future directions. Finally, the conclusion of this paper is described in Sect. 7.
2 Related work
Several efforts have been made in implementing mHealth programs in real world settings. A review by Mbuthia et al. revealed at least 11 studies have been using mHealth to strengthen the communication of post-natal care (PNC) in rural areas. Mobile phone messaging services are the most used method for communicating health information. The results of the systematic review show that various mHealth communications can be used to strengthen PNC in rural areas. One-way cell phone messages are the most commonly used type of mHealth communication to strengthen PNC uptake in various rural areas. This is a clear indication that mobile messaging may be the communication of choice for most users than other mHealth communication tools (Mbuthia et al. 2019).
Shahid et al. studied the use of mobile phone intervention to improve diabetes care in rural areas in Pakistan. The study call patients on their mobile phones every 15 days to remind them to self-monitor blood glucose levels, to take their medication on time, and to take a physical exercise. The study shows that after 4 months, the participants’ HbA1c are decreased from 10.09 to 8.63% (Shahid et al. 2015).
A study by Liu et al. demonstrated mHealth is adequate to control the risk of stroke, such as monitoring and controlling glycemic index and smoking cessation education. The prior study shows that mhealth has potential in managing key stroke risk factors through enhance smoking cessation (Liu et al. 2017).
The use of design science for informing the development of a mHealth app for HIV patients is implemented by Schnall et al. The usability inspection methods are used to evaluate the findings. The study revealed the effective use of design science method in the development of mHealth app for people living with HIV (Schnall et al. 2014, 2015).
Bin Abbas et al. investigated the effect of text messaging to educate patients on glycemic control in type 2 diabetes. The study had enrolled 100 participants. The participants received five to seven text messages every week. The study shows that HbA1c decreased from 9.9 to 9.5% among participants (Abbas et al. 2015).
Steinhubl et al. studied the effect of a home-based wearable continuous ECG monitoring patch on detection of undiagnosed atrial fibrillation (AF). There were 2659 cardiovascular disease (CDV) patients in the US that participated in the clinical trial. The study shows that immediate monitoring with a home-based wearable ECG resulted in a higher rate of AF after 4 months, compared with delayed monitoring (Steinhubl et al. 2018).
A study describes the potential implementation of m-health for maternal care in Namibia, comparing another country in South Africa that has implemented m-health for the same case. The findings of the study conclude that short message service and mobile apps is a popular technology used. Future direction for m-health adoption in Namibia for maternal care is improving the health policy and public health sector (Iyawa and Hamunyela 2019).
HATICE project investigated the use of interactive Internet counseling to provide support to cardiovascular disease patients in Netherlands, Finland, and France. Participants are provided with interactive Internet platform providing educational materials. The study shows that after 18 months the primary outcome improved in the intervention group compared to the control group (9 vs. 4%, respectively) (Richard et al. 2019).
Olmen et al. studied the barriers of implementing mHealth for disease management in low- and middle-income countries by reviewing the scope and field views of the implementers. This study states that barriers to implementing mHealth for non-communicable diseases include security/legal issues, access, infrastructure, intervention delivery/content, and usability/user view. The study noted that the most used technology in implementing mHealth for NCD management is Short Message Service (SMS). This technology can be combined with personal phone calls or with interactive feedback on patients input (van Olmen et al. 2020).
Viljoen et al. designed an NCD mHealth application for rural areas in Kenya (Viljoen et al. 2021). The method used is the Design Science Research with a rigor cycle approach. The study shows that the developed application can help health workers to control the patient's sugar and blood pressure levels in patients suffering from diabetes and hypertension.
Nedjai‑Merrouche et al. proposed outdoor multimodal system based on smartphone for health monitoring and incident detection (Nedjai-Merrouche et al. 2021). They showed that the proposed solution can detect falls from walking or standing with 97.77% precision (Table 1).
3 Methodologies
This research adopts Design Science Research (DSR) methodology of Information System (IS). Unlike the behavioral science methodologies that attempts to explain and predict, based on the observational activities, the impact of IS adoption to individual, group or organization, the DSR aims to create an IS artefact: model, method, construct, and instantiation to be an innovative solution for a particular issue. This methodology by default is seen as the most natural and appropriate one for this typical research. This is due to the aim of this research to develop a concrete solution, the mHealth application in the prevention and controlling endeavors for the NCDs, particularly in the context of Yogyakarta Province. It is worth noting, nevertheless, that both paradigms are inseparable in IS research. Both seek to extend the boundaries of human and organizational capabilities.
3.1 Study settings
University A seeks to address the challenges of developing a technology-based health management program by looking at the potential of health data that can be processed and enriched to become health information. The Indonesian mHealth project involves collaboration among experts (doctors, health informatics, ethicists, and hospital managers) in University A and other partners to achieve the goals.
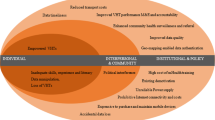
The proposed concept is to improve the community health status. It realizes social change by using technology that can reach a wide range of geographically and demographically. It is also integrated with the Indonesian health system (see Fig. 1). This concept is implemented in an mHealth application named NusaHealth. The solution consists of a digital healthcare infrastructure using an mHealth approach that puts patients at the center of health care.
In general, the data management architecture in the NusaHealth system is illustrated in Fig. 2. It shows how the generated data can be processed and used for monitoring, evaluation, and decision making for all stakeholders.
3.2 NusaHealth project management
The core project team invited District Health Officers to understand the actual health problems in the community. Several meetings were conducted to define the problems that NusaHealth could solve. Primary Health Care (PHC) officers from four districts were then invited to participate in Focus Group Discussions (FGD) to clarify those problems.
In parallel, the NusaHealth team recruited a field team consisting of 18 people with health-related education backgrounds, including a medical doctor, and members from nursing, pharmacy, public health, and medical record keeping. The team members were facilitated with technical training to conduct field implementation and evaluations.
Lastly, the NusaHealth team and the field team defined the pilot project implementation timeline, which was arranged for two months period. The field team was divided into two groups and then distributed to all selected 21 Primary Health Cares (PHCs) in four districts of Yogyakarta province.
3.3 Mobile health application development
The Design Science Research Methodology (DSRM) framework was adopted to design a mobile health application for addressing NCD and physical inactivity problems among users. DSRM incorporates procedures, principles, and practices to research the application of information systems. The DSRM process includes six steps: problem identification and motivation, the definition of goals for solutions, design, and development, demonstration, evaluation, and communication (Peffers et al. 2007) (see Fig. 3).
Design science research methodology process model (Peffers et al. 2007)
There are various approaches in software development, such as agile methodology which also suitable for mHealth application development. Interested readers can refer to (Hussain et al. 2009; Memmel et al. 2007; Peischl et al. 2015).
3.4 Problem-centered approach
This study was conducted using a Problem-Centered approach. The problem-centered approach to the research proposed by Peffers et al. is the basis of research activities in activity 1 (Peffers et al. 2007). The problem-centered approach shows that the research idea conducted is based on observing the problems experienced (see Fig. 4). The lack of equal distribution of health in Indonesia has made public awareness of NCDs’ dangers. NCDs are preventable and are greatly influenced by lifestyle. Therefore, individual interventions to stimulate a healthier lifestyle are essential. Thus, the use of mobile technology or mHealth is needed to support NCD programs.
3.5 DRSM process
-
(1)
Problem identification and motivation
WHO data in 2016 showed that the death rate of Indonesia's population due to NCD is 73% (WHO 2016). This percentage indicates that more than ¾ of the Indonesian population still have minimal awareness of NCD dangers. Furthermore, the WHO data showed that cardiovascular disease dominates the highest death rate in NCD in Indonesia. It can be overcome by changing people's lifestyles to become healthier, so a mHealth system is needed to increase public awareness of healthy living habits.
-
(2)
Objective of the solution
The objective was to develop an mHealth application to increase patients' self-efficacy in treating NCD implemented in Yogyakarta province. The major challenges included the diversity of Internet services for each location in Yogyakarta and limitations of the infrastructure of healthcare services. The mHealth application developed provides a series of activities that implement a healthy lifestyle packaged in the form of gamification, thus users can monitor their health while playing a game challenge.
-
(3)
Design and development
The artifact is the mHealth application that provides a series of activities that implement a healthy lifestyle packaged in the form of gamification. This application development refers to a paper written by Olla et al. which covers: Medical Use Cases, Technical Modalities, and Policy Consideration (see Fig. 5) (Olla and Shimskey 2015). In this study, we are focusing only on designing the technical modalities perspective.
mHealth taxonomy (Olla and Shimskey 2015)
-
(4)
Demonstration
After developing the prototype, 424 adult participants (age > 18 years old) were given the artifact to test the application. The population was randomly selected from four districts in Yogyakarta (Sleman, Bantul, Kulon Progo, Gunungkidul). The population subjects are mixed from different subpopulations: public health office staff, health workers, and the general population. The participants were trained on how to use the application. The users were observed for at least one month.
-
(5)
Evaluation
The mHealth application was evaluated using Technology Acceptance Model (TAM) framework (Venkatesh and Davis 1996). The TAM concept developed by Davis (Davis 1989), offers a theory as a basis for studying and understanding user behavior in receiving and using an information system. The expansion of the TAM concept is expected to help predict a person's attitude and acceptance of technology and can provide the necessary basic information about the factors that drive the individual's attitude. TAM describes a causal relationship between beliefs and behavior, goals/needs, and the actual use of users/users of an information system. This model places the trust factor of each user behavior with two variables: usefulness and ease of use. TAM framework and its extension are widely used to evaluate mHealth applications (Jacob et al. 2020).
Qualitative and quantitative evaluation instruments were built according to the TAM framework. Quantitative data were collected using a self-administered questionnaire. The self-administered questionnaire was created on three TAM topics: perceived usefulness, perceived ease of use, and user acceptance. The qualitative data were collected using a semi structured FGD format in each of the groups. Then, each group was asked questions concerning their experience using the NusaHealth prototype, perceived benefits when using the prototype, shortfalls or drawbacks when using the application, and suggestions for further development of the prototype.
The evaluation result shows that both groups of respondents (health worker and general population) feel confused about the usage of the application. However, other variables such as ease of use and user acceptance get a positive response. Some respondents think that the content presented cannot be trusted.
FGD were conducted to add quantitative data results by conducting discussions facilitated by one expert to conclude participant comments. The key themes that emerged in the thematic analysis were about the benefits of obtaining health information and as a motivation for a healthy lifestyle. The target user of the application attracts the middle age more than the elderly or teenagers because middle age has an increased health risk. Regarding the sustainability of the application, users are unsure whether the application will continue to be used without proper reminders from the health care provider. Finally, regarding the barrier, users have doubts about the application, whether it's data security or the truth of the information provided. We also noted the effect of previous exposure to technology on acceptance and its importance in usability and accessibility engineering as mentioned in (Holzinger et al. 2011).
-
(6)
Communication
In this paper we focused on the technical development of the prototype, fundamental requirements of the prototype, building features, and user flow. A detailed description on mHealth application development and the evaluation results are beyond the scope of this paper.
-
(7)
Contribution
This study contributes to the variety of evidence related to the development of mHealth applications, especially in developing and low-middle income countries. This study also describes an innovation that uses mHealth technology for the management of patients with NCD. However, the usage of the application not only focuses on people who already have NCD, but also on people who are at risk to develop NCD. Furthermore, the architecture could serve as a model for the development of mHealth services in Indonesia or other developing countries.
4 Results
4.1 Technical description of NusaHealth components
The technical considerations of the NusaHealth application are shown in Table 2.
4.2 How the NusaHealth system works
The descriptions of each component in the NusaHealth system are shown in Fig. 6. University A’s Information System and Resources Server 1 does not contain patient identifiable information and the purpose is to handle the anonymized lab data from Hospital A. Users initiate the import of lab data from the mHealth application by matching their Result ID (generated from blood test results) with the Laboratory ID (both are IDs generated by the system) with Date of Birth (DOB) as a third check. This server must sync with the Hospital A lab system on a nightly basis to bring the test results up to date.
University A’s Information Systems and Resources Server 2 does contain patient health data and the purpose is to provide identifiable patient information such as name, address, email, and phone numbers. It will help the team monitor operational metrics such as the current number of users, which one does not yet import lab data, etc. and create the most accurate operational report. This server is connected to the SMS Gateway to send Register ID to all users which is needed to import the laboratory test results into the application. The application then will verify the Register ID by matching the data to the laboratory and Result ID.
Figure 7 shows how the servers communicate with each other using an Application Programming Interface (API) developed by the NusaHealth team.
Examples of NusaHealth app is shown in Figs. 8, 9 and 10. Figure 8 shows how the applications handle challenges and rewards. Figure 9 illustrates how the applications can interact with users through daily challenges. In this case, the app asks the patient to measure the heart rate. If the user performed the daily challenges, the user would receive Nusa Points as a reward (see Fig. 10).
5 Discussion
In the development stage, the selection of the Android operating system was the best choice. This is supported by data from the International Data Corporation (IDC) in 2021 which stated that mobile devices are dominated by Android operating systems [25]. Some cases of mHealth with Android are used in many studies such as: (1) In South Africa for data collection of HIV positive pregnant women (Karageorgos et al. 2018); (2) mobile technology for health information dissemination (Angula and Dlodlo 2017); (3) the use of mHealth for smoking cessation interventions (Wibowo et al. 2019).
In this project, we identified several challenges and open issues:
-
(1)
Technical issues
There are several technical issues during the implementation of NusaHealth. The first problem is integrating mHealth systems with other hospital information systems because the current system can only connect with a single hospital information system. A flexible system architecture should be developed to connect the variety of hospital information systems in the province. Standards and interoperability are still significant challenges in health information systems in developing countries (Brailer 2005; Editors 2013).
There is a need to develop customer care centers using the SMS gateway and a communication feature in the application, such as a messaging system. This is because many problems (technical and non-technical) cannot be solved properly and in a timely manner due to the shortage of resources.
-
(2)
Network connection issues
The application needs a good network connection. However, the network availability varies from one district to another, and it became an issue in the project implementation. Since some areas do not have good data network coverage, the synchronization process cannot be done successfully every day. The application should have scheduled updates based on the store-and-forward technique to synchronize with the server when users have good data network coverage. In their research, Lloret et al. confirmed that better data service provides better data transmission by comparing patient monitoring with various network speeds (Lloret et al. 2017).
Further aspects of network infrastructure and utilization cover some indicators such as broadband penetration, regular internet users, electronic data exchange, etc. Some research showed the importance of network infrastructure quality in supporting mHealth systems (Aranda-Jan et al. 2014).
-
(3)
Security and privacy issues
Security and privacy are other issues to be dealt with since the sensitivity of healthcare information and its accessibility via the Internet and mobile technology systems is causing severe concerns (Ahmed et al. 2021; Vithanwattana et al. 2017). Arora et al. identified common mHealth risks and provided solutions for each risk (Arora et al. 2014). New technology such as Blockchain can be implemented to improve security and privacy issue. The use of Blockchain to secure batch verification protocol is studied in (Xiong et al. 2021). Some issues relevant to NusaHealth and their proposed solutions are shown in Table 3.
6 Future directions
Equally important to the cost-effectiveness and scalability of mHealth is its ability to provide an effective tool for addressing emerging health needs. In the near future, policymakers and health providers in the developing world will be forced to turn their focus to prevention and early detection rather than late-stage treatment of NCDs, such as diabetes and cancer, as well as to the health needs of an aging population. Late detection of these diseases leads to lower survival rates and reduced life expectancy and has negative consequences for social and economic development. Developing countries are therefore being confronted with a double burden of treating and containing the spread of communicable diseases while combating a wide range of unfamiliar health challenges.
Addressing future health needs will be facilitated by the development of mobile technologies and network expansion. The key technology trends in mobile technology continue to be the same trends that have characterized technological progress previously: miniaturization, greater speed, and cost reduction. A greater range of services becomes possible with more uniform, faster, and more affordable broadband access; greater access and coverage expands the ‘subscriber’ base, building volume, creating incentives for players, and helping push sustainable mHealth applications beyond simple one-way data services. mHealth technologies will cover more sophisticated diagnoses/consultation, e.g., telemedicine/telehealth, more effective use of healthcare workers, more ‘personal’ mHealth services and services for travel-restricted (e.g., during COVID19 pandemic).
Artificial Intelligence (AI) will play a big role in the next generation of mHealth applications. AI has shown to be able to improve the quality of medical diagnosis and treatments of many illnesses (Alshehri and Muhammad 2021; Rajput et al. 2021). AI has been used in computer-assisted diagnosis, to provide better prediction to reduce false alarms, to provide mentoring platform for elderly, etc.
7 Conclusion
mHealth programs as an extension of eHealth often begin with small pilot projects that, if successful and well-funded, may then be replicated and scaled up to larger populations or sets of facilities. NusaHealth initially has proved that our pilot project can be replicated and enhanced on a larger scale in the community.
However, more formal applications and comprehensive studies that can support and enhance larger health programs and policies are needed. To make it happen, projects will need to be implemented at a large enough scale to generate conclusive and generalizable results, using research protocols that can demonstrate where, how, and why mHealth works best.
Mobile technologies are not objectives but are tools that should be applied to achieve health objectives and help improve individuals' lives. More data are needed to understand how mobile technologies are influencing health outcomes. Future research should be conducted to answer the remaining challenges.
References
Abbas BB, Al Fares A, Jabbari M, El Dali A, Al Orifi F (2015) Effect of mobile phone short text messages on glycemic control in type 2 diabetes. Int J Endocrinol Metab. https://doi.org/10.5812/ijem.18791
Ahmed W, Rasool A, Javed AR, Kumar N, Gadekallu TR, Jalil Z, Kryvinska N (2021) Security in next generation mobile payment systems: a comprehensive survey. IEEE Access. https://doi.org/10.1109/ACCESS.2021.3105450
Alshehri F, Muhammad G (2021) A comprehensive survey of the Internet of Things (IoT) and AI-based smart healthcare. IEEE Access 9:3660–3678. https://doi.org/10.1109/ACCESS.2020.3047960
Angula N, Dlodlo N (2017) Mobile technology for healthcare information dissemination to low resource areas of Namibia. Int J Sci Res 6:662–274
Aranda-Jan CB, Mohutsiwa-Dibe N, Loukanova S (2014) Systematic review on what works, what does not work and why of implementation of mobile health (mHealth) projects in Africa. BMC Public Health 14:1–15
Arora S, Yttri J, Nilsen W (2014) Privacy and security in mobile health (mHealth) research Alcohol research. Curr Rev 36:143
Brailer DJ (2005) Interoperability: the key to the future health care system: interoperability will bind together a wide network of real-time, life-critical data that not only transform but become health care. Health Aff. https://doi.org/10.1377/hlthaff.w5.19
Chib A (2013) The promise and peril of mHealth in developing countries. Mobile Media Commun 1:69–75
Davis FD (1989) Perceived usefulness, perceived ease of use, and user acceptance of information technology. MIS Q 13(3):319–340
Editors PM (2013) A reality checkpoint for mobile health: three challenges to overcome. PLoS Med 10:e1001395
Eze E, Gleasure R, Heavin C (2016) Reviewing mHealth in developing countries: a stakeholder perspective. Procedia Comput Sci 100:1024–1032
Haddad L, Cameron L, Barnett I (2015) The double burden of malnutrition in SE Asia and the Pacific: priorities, policies and politics. Health Policy Planning 30:1193–1206
Holzinger A, Searle G, Wernbacher M (2011) The effect of previous exposure to technology on acceptance and its importance in usability and accessibility engineering. Univ Access Inf Soc 10:245–260
Hootsuite, Social WA (2021) Digital in Indonesia: All the Statistics You Need in 2021. DataReportal - Global Digital Insights
Hoque MR, Rahman MS, Nipa NJ, Hasan MR (2020) Mobile health interventions in developing countries: a systematic review. Health Info J 26(4):2792–2810
Hussain Z, Slany W, Holzinger A Current state of agile user-centered design: a survey. In: Symposium of the Austrian HCI and Usability Engineering Group, 2009. Springer, pp 416–427
Iyawa GE, Hamunyela S mHealth apps and services for maternal healthcare in developing countries. In: 2019 IST-Africa Week Conference (IST-Africa), 2019. IEEE, pp 1–10
Jacob C, Sanchez-Vazquez A, Ivory C (2020) Understanding clinicians’ adoption of mobile health tools: a qualitative review of the most used frameworks. JMIR Mhealth Uhealth 8:e18072. https://doi.org/10.2196/18072
Karageorgos G, Andreadis I, Psychas K, Mourkousis G, Kiourti A, Lazzi G, Nikita KS (2018) The promise of mobile technologies for the health care system in the developing world: a systematic review. IEEE Rev Biomed Eng 12:100–122
Krishnamoorthy S, Dua A, Gupta S (2021) Role of emerging technologies in future IoT-driven Healthcare 4.0 technologies: a survey, current challenges and future directions. J Ambient Intell Human Comput. https://doi.org/10.1007/s12652-021-03302-w
Liu S, Feng W, Chhatbar PY, Liu Y, Ji X, Ovbiagele B (2017) Mobile health as a viable strategy to enhance stroke risk factor control: a systematic review and meta-analysis. J Neurol Sci 378:140–145
Lloret J, Parra L, Taha M, Tomás J (2017) An architecture and protocol for smart continuous eHealth monitoring using 5G. Comput Netw 129:340–351
Mbuthia F, Reid M, Fichardt A (2019) mHealth communication to strengthen postnatal care in rural areas: a systematic review. BMC Pregnancy Childbirth 19:1–10
Memmel T, Reiterer H, Holzinger A (2007) Agile methods and visual specification in software development: a chance to ensure universal access. In: Stephanidis C (ed) Universal acess in human computer interaction. Coping with diversity. Springer, Berlin, pp 453–462
Nedjai-Merrouche I, Saadia N, RamdaneCherif A, Makhlouf A (2021) Outdoor multimodal system based on smartphone for health monitoring and incident detection. J Ambient Intell Human Comput 12:10699–10721
Olla P, Shimskey C (2015) mHealth taxonomy: a literature survey of mobile health applications. Health Technol 4:299–308
Peffers K, Tuunanen T, Rothenberger MA, Chatterjee S (2007) A design science research methodology for information systems research. J Manage Info Syst 24:45–77
Peischl B, Ferk M, Holzinger A (2015) The fine art of user-centered software development. Software Qual J 23:509–536
Rajput DS, Basha SM, Xin Q, Gadekallu TR, Kaluri R, Lakshmanna K, Maddikunta PKR (2021) Providing diagnosis on diabetes using cloud computing environment to the people living in rural areas of India. J Ambient Intell Human Comput 13:2829–2840
Richard E et al (2019) Healthy ageing through internet counselling in the elderly (HATICE): a multinational, randomised controlled trial. The Lancet Digital Health. https://doi.org/10.1016/S2589-7500(19)30153-0
Royston G, Hagar C, Long L-A, McMahon D, Pakenham-Walsh N, Wadhwani N (2015) Mobile health-care information for all: a global challenge. Lancet Glob Health 3:e356–e357
Schnall R, Mosley JP, Iribarren SJ, Bakken S, Carballo-Diéguez A, Brown W III (2015) Comparison of a user-centered design self-management app to existing mHealth apps for persons living with HIV. JMIR mHealth uHealth 3:e91. https://doi.org/10.2196/mhealth.4882
Schnall R, Rojas M, Travers J, Brown W 3rd, Bakken S (2014) Use of design science for informing the development of a mobile app for persons living with HIV. AMIA Annu Symp Proc 2014:1037–1045
Shahid M, Mahar SA, Shaikh S, Shaikh Z (2015) Mobile phone intervention to improve diabetes care in rural areas of Pakistan: a randomized controlled trial. J Coll Physicians Surg Pak 25:166–171
Steinhubl SR et al (2018) Effect of a home-based wearable continuous ECG monitoring patch on detection of undiagnosed atrial fibrillation: the mSToPS randomized clinical trial. JAMA 320:146–155. https://doi.org/10.1001/jama.2018.8102
van Olmen J et al (2020) Implementation barriers for mHealth for non-communicable diseases management in low and middle income countries: a scoping review and field-based views from implementers. Wellcome Open Res 5:7
Venkatesh V, Davis FD (1996) A model of the antecedents of perceived ease of use: development and test decision. Sciences 27:451–481
Viljoen A, Klinker K, Wiesche M, Uebernickel F, Krcmar H (2021) Design principles for mhealth application development in rural parts of developing countries: the case of noncommunicable diseases in Kenya. IEEE Trans Eng Manag. https://doi.org/10.1109/TEM.2021.3072601
Vithanwattana N, Mapp G, George C (2017) Developing a comprehensive information security framework for mHealth: a detailed analysis. J Reliable Intell Environ 3:21–39
Vos T et al (2020) Global burden of 369 diseases and injuries in 204 countries and territories, 1990–2019: a systematic analysis for the Global Burden of Disease Study. The Lancet 396:1204–1222
WHO (2016) Indonesia - Risk of premature death due to NCDS
Wibowo MF, Kumar AA, Surahyo Sumarsono RR (2019) Perceived usefulness of receiving a potential smoking cessation intervention via mobile phones among smokers in Indonesia. Wellcome Open Res 4:94
Xiong H et al (2021) On the design of blockchain-based ECDSA with fault-tolerant batch verication protocol for blockchain-enabled IoMT. IEEE J Biomed Health Info. https://doi.org/10.1109/JBHI.2021.3112693
Author information
Authors and Affiliations
Corresponding author
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Sumarsono, S., Sakkinah, I.S., Permanasari, A.E. et al. Development of a mobile health infrastructure for non-communicable diseases using design science research method: a case study. J Ambient Intell Human Comput 14, 12563–12574 (2023). https://doi.org/10.1007/s12652-022-04322-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12652-022-04322-w