Abstract
Purpose
Venous congestion is a pathophysiologic state that can result in organ dysfunction, particularly acute kidney injury (AKI). We sought to evaluate the feasibility of performing a definitive observational study to determine the impact of venous congestion quantified using point-of-care ultrasound (POCUS) in patients with septic shock.
Methods
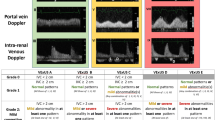
We conducted a prospective observational feasibility study at two intensive care units (ICUs). We recruited adult patients with septic shock within 12 hr of ICU admission. Using the validated Venous Excess Ultrasound Score (VEXUS), we quantified venous congestion on day 1 and day 3 of ICU admission. The primary feasibility outcome was successful completion rate of the two VEXUS scores. We performed a survival analysis to quantify the hazard of renal replacement therapy (RRT).
Results
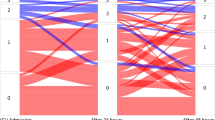
We enrolled 75 patients from January 2022 to January 2023. The success rate of completion for VEXUS scans was 94.5% (95% confidence interval [CI], 89.5 to 97.6). Severe venous congestion was present in 19% (14/75) of patients on ICU admission day 1 and in 16% (10/61) of patients on day 3. Venous congestion on ICU admission may be associated with a higher risk of requiring RRT (unadjusted hazard ratio, 3.35; 95% CI, 0.94 to 11.88; P = 0.06).
Conclusions
It is feasible to conduct a definitive observational study exploring the association between venous congestion quantified with POCUS and clinical outcomes in patients with septic shock. We hypothesize that venous congestion may be associated with an increased hazard of receiving RRT.
Résumé
Objectif
La congestion veineuse est un état physiopathologique qui peut entraîner un dysfonctionnement des organes, en particulier une insuffisance rénale aiguë (IRA). Nous avons cherché à évaluer la faisabilité de la réalisation d’une étude observationnelle définitive pour déterminer l’impact de la congestion veineuse quantifiée à l’aide de l’échographie ciblée (POCUS) chez des patient·es en choc septique.
Méthode
Nous avons réalisé une étude de faisabilité observationnelle prospective dans deux unités de soins intensifs (USI). Nous avons recruté des patient·es adultes souffrant d’un choc septique dans les 12 heures suivant leur admission aux soins intensifs. À l’aide du score VEXUS (score d’échographie de l’excès veineux) validé, nous avons quantifié la congestion veineuse au jour 1 et au jour 3 de leur admission aux soins intensifs. Le principal critère de faisabilité était le taux de réussite des deux scores VEXUS. Nous avons réalisé une analyse de survie pour quantifier le risque de thérapie de substitution rénale (TSR).
Résultats
Nous avons recruté 75 patient·es de janvier 2022 à janvier 2023. Le taux de réussite des scores VEXUS était de 94,5 % (intervalle de confiance [IC] à 95 %, 89,5 à 97,6). Une congestion veineuse sévère était présente chez 19 % (14/75) des patient·es au jour 1 d’admission aux soins intensifs et chez 16 % (10/61) des patient·es au jour 3. La congestion veineuse lors de l’admission aux soins intensifs peut être associée à un risque plus élevé de nécessiter une TSR (rapport de risque non ajusté, 3,35; IC 95 %, 0,94 à 11,88; P = 0,06).
Conclusion
Il est possible de mener une étude observationnelle définitive explorant l’association entre la congestion veineuse quantifiée par POCUS et les devenirs cliniques chez les patient·es en choc septique. Nous émettons l’hypothèse que la congestion veineuse peut être associée à un risque accru de recevoir une thérapie de substitution rénale.




Similar content being viewed by others
References
Brown RM, Semler MW. Fluid management in sepsis. J Intensive Care Med 2019; 34: 364–73. https://doi.org/10.1177/0885066618784861
Mouncey PR, Osborn TM, Power GS, et al. Trial of early, goal-directed resuscitation for septic shock. N Engl J Med 2015; 372: 1301–11. https://doi.org/10.1056/nejmoa1500896
Hernández G, Ospina-Tascón GA, Damiani LP, et al. Effect of a Resuscitation strategy targeting peripheral perfusion status vs serum lactate levels on 28-day mortality among patients with septic shock: the ANDROMEDA-SHOCK randomized clinical trial. JAMA 2019; 321: 654–64. https://doi.org/10.1001/jama.2019.0071
Yealy DM, Kellum JA, Huang DT, et al. A randomized trial of protocol-based care for early septic shock. N Engl J Med 2014; 370: 1683–93. https://doi.org/10.1056/nejmoa1401602
Silversides JA, Fitzgerald E, Manickavasagam US, et al. Deresuscitation of patients with iatrogenic fluid overload is associated with reduced mortality in critical illness. Crit Care Med 2018; 46: 1600–7. https://doi.org/10.1097/ccm.0000000000003276
Messmer AS, Zingg C, Müller M, Gerber JL, Schefold JC, Pfortmueller CA. Fluid overload and mortality in adult critical care patients—a systematic review and meta-analysis of observational studies. Crit Care Med 2020; 48: 1862–70. https://doi.org/10.1097/ccm.0000000000004617
Granado R, Mehta RL. Fluid overload in the ICU: evaluation and management. BMC Nephrol 2016; 17: 109. https://doi.org/10.1186/s12882-016-0323-6
Pouska J, Tegl V, Astapenko D, Cerny V, Lehmann C, Benes J. Impact of intravenous fluid challenge infusion time on macrocirculation and endothelial glycocalyx in surgical and critically ill patients. Biomed Res Int 2018; 2018: 8925345. https://doi.org/10.1155/2018/8925345
Milford EM, Reade MC. Resuscitation fluid choices to preserve the endothelial glycocalyx. Crit Care 2019; 23: 77. https://doi.org/10.1186/s13054-019-2369-x
Beaubien-Souligny W, Rola P, Haycock K, et al. Quantifying systemic congestion with point-of-care ultrasound: development of the venous excess ultrasound grading system. Ultrasound J 2020; 12: 16. https://doi.org/10.1186/s13089-020-00163-w
Sun R, Guo Q, Wang J, et al. Central venous pressure and acute kidney injury in critically ill patients with multiple comorbidities: a large retrospective cohort study. BMC Nephrol 2022; 23: 83. https://doi.org/10.1186/s12882-022-02715-9
Lee CW, Kory PD, Arntfield RT. Development of a fluid resuscitation protocol using inferior vena cava and lung ultrasound. J Crit Care 2016; 31: 96–100. https://doi.org/10.1016/j.jcrc.2015.09.016
Rola P, Miralles-Aguiar F, Argaiz E, et al. Clinical applications of the venous excess ultrasound (VExUS) score: conceptual review and case series. Ultrasound J 2021; 13: 32. https://doi.org/10.1186/s13089-021-00232-8
Bhardwaj V, Vikneswaran G, Rola P, et al. Combination of inferior vena cava diameter, hepatic venous flow, and portal vein pulsatility index: venous excess ultrasound score (VEXUS score) in predicting acute kidney injury in patients with cardiorenal syndrome: a prospective cohort study. Indian J Crit Care Med 2020; 24: 783–9. https://doi.org/10.5005/jp-journals-10071-23570
Beaubien-Souligny W, Benkreira A, Robillard P, et al. Alterations in portal vein flow and intrarenal venous flow are associated with acute kidney injury after cardiac surgery: a prospective observational cohort study. J Am Heart Assoc 2018; 7: e009961. https://doi.org/10.1161/jaha.118.009961
Benkreira A, Beaubien-Souligny W, Mailhot T, et al. Portal hypertension is associated with congestive encephalopathy and delirium after cardiac surgery. Can J Cardiol 2019; 35: 1134–41. https://doi.org/10.1016/j.cjca.2019.04.006
Spiegel R, Teeter W, Sullivan S, et al. The use of venous Doppler to predict adverse kidney events in a general ICU cohort. Crit Care 2020; 24: 615. https://doi.org/10.1186/s13054-020-03330-6
von Elm E, Altman DG, Egger M, et al. Strengthening the Reporting of Observational Studies in Epidemiology (STROBE) statement: guidelines for reporting observational studies. BMJ 2007; 335: 806–8. https://doi.org/10.1136/bmj.39335.541782.ad
Prager R, Wu K, Bachar R, et al. Blinding practices during acute point-of-care ultrasound research: the BLIND-US meta-research study. BMJ Evid Based Med 2020; 26: 110–1. https://doi.org/10.1136/bmjebm-2020-111577
Thabane L, Ma J, Chu R, et al. A tutorial on pilot studies: the what, why and how. BMC Med Res Methodol 2010; 10: 1. https://doi.org/10.1186/1471-2288-10-1
Denault A, Couture EJ, De Medicis É, et al. Perioperative Doppler ultrasound assessment of portal vein flow pulsatility in high-risk cardiac surgery patients: a multicentre prospective cohort study. Br J Anaesth 2022; 129: 659–69. https://doi.org/10.1016/j.bja.2022.07.053
Author contributions
Ross Prager and John Basmaji contributed to the conception, design, and implementation of the research; acquisition, analysis and interpretation of the data; and preparation and writing of the manuscript. Michelle Y. S. Wong contributed to data acquisition, data analysis, data interpretation, and manuscript preparation. Robert Arntfield, Ian Ball, Kimberley Lewis, and Bram Rochwerg contributed to the interpretation of the data and manuscript preparation.
Disclosures
No authors have conflicts of interest to declare.
Funding statement
A resident PSI Foundation (North York, ON, Canada) research grant was awarded to support this work.
Editorial responsibility
This submission was handled by Dr. Patricia S. Fontela, Associate Editor, Canadian Journal of Anesthesia/Journal canadien d’anesthésie.
Author information
Authors and Affiliations
Corresponding author
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Prager, R., Arntfield, R., Wong, M.Y.S. et al. Venous congestion in septic shock quantified with point-of-care ultrasound: a pilot prospective multicentre cohort study. Can J Anesth/J Can Anesth 71, 640–649 (2024). https://doi.org/10.1007/s12630-024-02717-1
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12630-024-02717-1