Abstract
Purpose
Biomarkers can aid in perioperative risk stratification. While preoperative copeptin has been associated with adverse events, intraoperative information is lacking and this association may rather reflect a baseline risk. Knowledge about correlations between postoperative copeptin measurements and clinically relevant outcomes is scarce. We examined the association of perioperative copeptin concentrations with postoperative all-cause mortality and/or major adverse cardiac and cerebrovascular events (MACCE) at 12 months and 30 days as well as with perioperative myocardial injury (PMI).
Methods
We conducted a prospective observational cohort study of adults undergoing noncardiac surgery with intermediate to high surgical risk in Basel, Switzerland, and Düsseldorf, Germany from February 2016 to December 2020. We measured copeptin and cardiac troponin before surgery, immediately after surgery (0 hr) and once between the second and fourth postoperative day (POD 2–4).
Results
A primary outcome event of a composite of all-cause mortality and/or MACCE at 12 months occurred in 48/502 patients (9.6%). Elevated preoperative copeptin (> 14 pmol·L−1), immediate postoperative copeptin (> 90 pmol·L−1), and copeptin on POD 2–4 (> 14 pmol·L−1) were associated with lower one-year MACCE-free and/or mortality-free survival (hazard ratio [HR], 2.89; 95% confidence interval [CI], 1.62 to 5.2; HR, 2.07; 95% CI, 1.17 to 3.66; and HR, 2.47; 95% CI, 1.36 to 4.46, respectively). Multivariable analysis continued to show an association for preoperative and postoperative copeptin on POD 2–4. Furthermore, elevated copeptin on POD 2–4 showed an association with 30-day MACCE-free survival (HR, 2.15; 95% CI, 1.18 to 3.91). A total of 64 of 489 patients showed PMI (13.1%). Elevated preoperative copeptin was not associated with PMI, while immediate postoperative copeptin was modestly associated with PMI.
Conclusion
The results of the present prospective observational cohort study suggest that perioperative copeptin concentrations can help identify patients at risk for all-cause mortality and/or MACCE. Other identified risk factors were revised cardiac risk index, body mass index, surgical risk, and preoperative hemoglobin.
Trial registration
ClinicalTrials.gov (NCT02687776); first submitted 9 February 2016.
Résumé
Objectif
Les biomarqueurs peuvent aider à la stratification du risque périopératoire. Bien que la copeptine préopératoire ait été associée à des événements indésirables, les informations peropératoires font défaut; plutôt, cette association pourrait refléter un risque de base. Les connaissances sur les corrélations entre les mesures postopératoires de la copeptine et les résultats cliniquement pertinents sont rares. Nous avons examiné l’association entre les concentrations de copeptine périopératoires et la mortalité postopératoire toutes causes confondues et/ou les événements indésirables cardiaques et cérébrovasculaires majeurs (EICCM/MACCE) à 12 mois et 30 jours ainsi qu’en cas de lésion myocardique périopératoire (LMP/PMI).
Méthode
Nous avons réalisé une étude de cohorte observationnelle prospective d’adultes bénéficiant d’une chirurgie non cardiaque à risque chirurgical intermédiaire à élevé à Bâle, en Suisse, et à Düsseldorf, en Allemagne, de février 2016 à décembre 2020. Nous avons mesuré la copeptine et la troponine cardiaque avant la chirurgie, immédiatement après la chirurgie (0 h) et une fois entre le deuxième et le quatrième jour postopératoire (JPO 2-4).
Résultats
Un événement constituant un critère d’évaluation principal d’un composite de mortalité toutes causes confondues et/ou de MACCE à 12 mois est survenu chez 48/502 patient·es (9,6 %). Une élévation de la copeptine préopératoire (> 14 pmol·L−1), de la copeptine postopératoire immédiate (> 90 pmol·L−1) et de la copeptine aux JPO 2 à 4 (> 14 pmol·L−1) était associée à une survie sans MACCE et/ou sans mortalité à un an plus faible (rapport de risque [RR], 2,89; intervalle de confiance [IC] à 95 %, 1,62 à 5,2; RR, 2,07; IC 95 %, 1,17 à 3,66; et RR, 2,47; IC 95 %, 1,36 à 4,46, respectivement). L’analyse multivariée a aussi montré une association entre la copeptine préopératoire et postopératoire aux JPO 2 à 4. De plus, un taux élevé de copeptine aux JPO 2 à 4 a montré une association avec la survie sans MACCE à 30 jours (RR, 2,15; IC 95 %, 1,18 à 3,91). Au total, 64 des 489 patient·es présentaient une LMP (13,1 %). Un taux élevé de copeptine préopératoire n’a pas été associé à la LMP, tandis que la copeptine postopératoire immédiate était modestement associée à la LMP.
Conclusion
Les résultats de la présente étude de cohorte observationnelle prospective suggèrent que les concentrations périopératoires de copeptine peuvent aider à identifier les personnes à risque de mortalité toutes causes confondues et/ou de MACCE. Les autres facteurs de risque identifiés étaient l’indice de risque cardiaque révisé, l’indice de masse corporelle, le risque chirurgical et l’hémoglobine préopératoire.
Enregistrement de l’étude
ClinicalTrials.gov (NCT02687776); première soumission le 9 février 2016.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Cardiac complications are a common cause of postoperative morbidity and mortality.1,2 In addition, perioperative myocardial injury (PMI) has emerged as a relevant adverse event with a 30-day mortality of 7.8%2 despite most of these patients being asymptomatic.2,3,4 In this context, the role of biomarkers has greatly increased.5,6 Preoperatively, biomarkers may be useful in detecting subclinically manifest disease or risk; intra and postoperatively, they may indicate an early state of pathology or beginning of cardiac ischemia or decompensation.
Several established biomarkers have been examined with a primary focus on cardiac troponin and natriuretic peptides.7,8,9,10,11 Copeptin, however, may be a promising early marker of cardiac risk as it is secreted in a 1:1 fashion with vasopressin on account of a common precursor peptide.12 Together with troponin, copeptin has been suggested for the early rule-out and diagnosis of cardiac events in the nonsurgical population,13,14,15,16,17,18,19 leading to the endorsement of a dual biomarker strategy.16 Compared with cardiac troponin representing manifest damage, copeptin representing distress may be more sensitive and detectable earlier on.20
Data regarding the utility of copeptin in the perioperative period is not firmly established. Although some data have suggested an association of copeptin and cardiac injury,21,22,23 the association of perioperative (particularly postoperative) copeptin concentrations and 12-month morbidity and mortality and PMI are much less clear. Furthermore, the timing of measurements remains uncertain.
We hypothesized that copeptin concentrations measured prior to surgery, immediately after surgery, and after postoperative days 2–4 (POD 2–4) are associated with the composite of major adverse cardiac and cerebrovascular events (MACCE) and/or all-cause mortality within 12 months.
Methods
Study design, setting, and patients
Ethical approval for the study in Basel (approval number, 2015-275) was provided by Ethikkommission Nordwest- und Zentralschweiz, Basel, Switzerland (Chairperson Prof A. Perruchoud, 13 October 2015). Ethical approval for the study in Düsseldorf (approval number, V7) was provided by Ethikkommission der Heinrich Heine Universität Düsseldorf, Düsseldorf, Germany (Chairperson Prof T. Hohlfeld, 1 October 2018).
Written informed consent was obtained from all patients. This prospective dual centre cohort study adheres to the Strengthening the Reporting of Observational Studies in Epidemiology (STROBE) guidelines for the reporting of observational studies.24
Consecutive adult patients undergoing elective surgery at two university hospitals (Basel and Düsseldorf) from February 2016 to December 2020 were included. Patients undergoing emergent surgery or presenting with either an acute coronary syndrome or congestive heart failure (both identified by clinical assessment or documentation in the clinical record) were not eligible. Patients with kidney dysfunction (creatinine clearance < 50 mL·min−1), severe aortic stenosis (valve area documented < 1 cm2), or an ejection fraction below 40% (documented) were also excluded. These inclusion and exclusion criteria were applied to reduce the effect of possible confounders.
The primary aim of this study was to examine whether elevated immediate postoperative copeptin concentrations are associated with 12-month all-cause mortality and MACCE in patients undergoing elevated risk surgery (intermediate- and high-risk as defined by the European Society of Anaesthesiology guidelines based on Glance et al.5,25).
Biomarker measurements
Copeptin and high-sensitive cardiac troponin T (hsTnT) were each sampled at three perioperative time points: at induction of anesthesia, immediately after surgery, and on POD 2–4. The sampling time on POD 2–4 was selected for two reasons: 1) many patients are discharged on these days, and 2) the vast majority of PMI are observed during this time.4,26
Samples were sent to the internal university hospital laboratories for analysis. Copeptin was measured by a time-resolved amplified cryptate emission immunoassay with a lower detection limit of 0.4 pmol·L−1 (Thermo Fisher Scientific Clinical Diagnostics B.R.A.H.M.S. GmbH, Henningsdorf, Germany), hsTnT by a high-sensitivity assay (Elecsys®; Roche Diagnostics, Rotkreuz, Switzerland) with a 99th percentile or upper limit of normal of 14 ng·L−1 with a coefficient of variation of 9%.27,28 Treating clinicians and study personnel were blinded to biomarker measurements.
Outcomes
The primary outcome was a composite of MACCE and/or all-cause mortality at 12 months. MACCE was predefined to include nonfatal cardiac arrest, acute myocardial infarction, congestive heart failure requiring hospitalization or transfer to a higher-level care unit, and stroke as previously defined.29 The secondary outcome was PMI, defined as an increase in cardiac troponin > 14 ng·L−1 from a baseline cardiac troponin by POD 2–4 presumably due to myocardial ischemia (i.e., no evidence of a nonischemic etiology). An ischemic feature was not required.30 We also evaluated MACCE and/or all-cause mortality at 30 days.
Routine electrocardiograms (ECGs) were performed in all patients before surgery and on POD 2–4 to identify possible signs of ischemia including new left branch bundle block or ST-segment elevation, ST-depression, or T-wave inversion in two continuous leads.31 Two independent blinded assessors adjudicated ECG with initial differences resolved by consensus.
Patients were followed up after 12 months by a mailed questionnaire. In the absence of a response, patients, their next of kin, or their primary care physician were contacted by phone.32 Hospital charts were used to extract in-hospital complications, and postdischarge events were confirmed by the patient’s primary care physician or treating hospital.
Statistical analyses
Data are presented as mean (standard deviation) for normally distributed continuous data, median [interquartile range (IQR)] for nonnormally distributed continuous data, and number (%) for count data.
For the primary endpoint all-cause mortality and/or MACCE at 12 months, we plotted Kaplan–Meier curves and performed a log-rank test for elevated copeptin. Elevated copeptin was defined as > 14 pmol·L−1 for preoperative measurements, by Youden’s optimum of a receiver operator characteristics curve for immediate postoperative copeptin, and as > 14 pmol·L−1 for measurements on POD 2–4. Although previous measurements had suggested that copeptin levels return to near normal on POD 2–4, we examined this by Youden’s optimum for all-cause mortality and/or MACCE at 12 months. We also plotted Kaplan–Meier curves and performed a log-rank test for elevated copeptin and all-cause mortality and/or MACCE at 30 days.
We furthermore examined a possible association of elevated copeptin concentrations and all-cause mortality and/or MACCE at 12 months by univariable hazard ratios (HRs). Then, in the event of a significant association, we adjusted elevated copeptin for the revised cardiac risk index (RCRI)11 as predefined and for all significant variables in the univariable analysis (not predefined). All models were described with events and the Akaike Information Criterion (AIC). For the analysis on POD 2–4, patients with events prior to blood withdrawal were excluded.
For the secondary outcome, PMI, we examined a possible association of preoperative and immediate postoperative copeptin using logistic regression. Copeptin concentrations on POD 2–4 were not examined as PMI was determined at the same time. Again, we first performed a univariable analysis and then a multivariable analysis as described above.
We performed a Bonferroni P adjustment for each of the three time points (P = 0.05/3) with P < 0.017 considered to be significant for the primary outcome. No adjustment was made for secondary and explorative analyses.
Our sample size analysis was based on the rule of thumb that 10–12 events are required per estimator in the multivariate Cox regression.33 We estimated the event rate to be 10% based on published and own data, yielding some 50 events and allowing for up to four estimators in a multivariable analysis. Although literature published after our sample size estimation has suggested that more events per predictor may be required,34,35 our analysis still allows for a multivariable analysis.
Results
Descriptive analysis
A total of 517 patients undergoing elevated risk surgery were enrolled. Two patients (< 1%) were lost to follow-up, 12 (2%) were excluded because of missing immediate postoperative copeptin, and one was erroneously included (< 1%). This left 502 patients for inclusion in the analysis (Fig. 1). Copeptin measurements were available preoperatively in 490 patients (97.2%), immediately postoperatively in 502 patients (100%), and on POD 2–4 in 463 patients (91.9%).
A primary outcome event of a composite of all-cause mortality and/or MACCE at 12 months occurred in 48/502 patients (9.6%). The first MACCE were 33 (7%) all-cause mortalities, four (1%) cases of congestive heart failure, six (1%) acute myocardial infarctions, and five (1%) strokes.
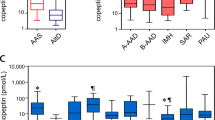
Median [IQR] copeptin concentrations were 7.2 [4.0–12.6] preoperatively (elevated > 14 pmol·L−1, 107/490 [21.8%]), 64.0 [23.4–145.1] immediately postoperatively (elevated > 90 pmol·L−1, 199/502 [39.5%]), and 9.3 [5.6–19.2] on POD 2–4 (elevated > 14 pmol·L−1, 159/463 [34.3%]).
The Youden’s optimum values for copeptin and MACCE were 9 pmol·L−1 preoperatively, 90 pmol·L−1 immediately postoperatively, and 11 pmol·L−1 on POD 2–4 (Electronic Supplementary Material eFigure).
Table 1 shows patient characteristics stratified by patients with MACCE and/or all-cause mortality. Patients showing MACCE and/or all-cause mortality at 12 months tended to exhibit a higher surgical risk, a higher American Society of Anesthesiologists Physical Status score,36 a higher RCRI,1 and lower preoperative hemoglobin levels, and were more likely to receive continuous norepinephrine in the operating theatre. Postoperative characteristics also differed.
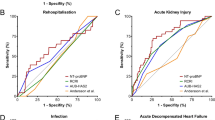
Figure 2 shows the Kaplan–Meier survival curves for 12-month MACCE-free survival for elevated preoperative copeptin (> 14 pmol·L−1), immediate postoperative copeptin (> 90 pmol·L−1), and copeptin on POD 2–4 (> 14 pmol·L−1). Elevated copeptin concentrations were associated with lower MACCE-free survival at each of the time points (P = 0.001, P = 0.010, and P = 0.002; P < 0.017 considered to be significant). Exploratively, elevated copeptin at both postoperative timepoints showed a possible relationship with 30-day MACCE-free survival, while elevated preoperative copeptin did not.
Table 2 shows univariable hazard ratios (HRs), and adjusted HRs for copeptin (preoperative, immediate postoperative, and POD 2–4) as well as for other preoperative and intraoperative variables. An elevated preoperative copeptin concentration of > 14 pmol·L−1 was significantly associated with all-cause mortality and/or MACCE at 12 months when adjusting solely for the RCRI (Model 1A: HR, 2.55; 95% confidence interval [CI], 1.42 to 4.58) as well as when adjusting for the RCRI, body mass index (BMI), surgical risk, and preoperative hemoglobin (Model 1B: HR: 2.54; 95% CI, 1.41 to 4.58). Model improvement from 1A to 1B was modest (AIC, 549 vs 543). Immediately postoperatively, elevated preoperative copeptin concentrations > 90 pmol·L−1 showed a significant association when adjusting solely for the RCRI (Model 2A: HR, 2.84; 95% CI, 1.33 to 6.1), but not when adjusting for the RCRI, BMI, surgical risk, preoperative hemoglobin, and the intraoperative need for continuous norepinephrine (Model 2B: HR, 1.73; 95% Cl, 0.97 to 3.09). After 2–4 postoperative days, elevated preoperative copeptin concentrations > 14 pmol·L−1 showed a significant association when adjusting solely for the RCRI (Model 3A: HR, 2.15; 95% CI, 1.18 to 3.91) as well as when adjusting for the RCRI, BMI, surgical risk, preoperative hemoglobin, and the intraoperative need for continuous norepinephrine (Model 3B: HR, 1.88; 95% CI, 1.02 to 3.46).
Table 3 shows the association of copeptin with PMI, which a total of 64/489 patients showed (13.1%). Of these, 25 fulfilled the criteria of PMI during immediate postoperative sampling and 39 developed PMI afterwards. Preoperative elevated copeptin was not associated with any postoperative PMI, while immediate postoperatively elevated copeptin was associated with any postoperative PMI. Body mass index, preoperative hemoglobin, and the need for continuous intraoperative norepinephrine were also associated with any postoperative PMI (n = 64; odds ratio [OR], 1.08; 95% CI, 1.01 to 1.15). In the multivariable model, the OR of elevated postoperative copeptin and PMI remained statistically significant, but of modest magnitude (adjusted OR, 1.08; 95% CI, 1.01 to 1.15).
Discussion
In this prospective observational cohort study, elevated copeptin measured preoperatively, immediately after surgery, and on POD 2–4 were all associated with 12-month mortality and morbidity. Elevated copeptin measured preoperatively and on POD 2–4 remained significantly associated when adjusting for other variables. Immediate postoperative copeptin was modestly associated with PMI, while preoperative copeptin was not. Other risk factors associated with MACCE and/or all-cause mortality were a higher RCRI, BMI, surgical risk, and preoperative hemoglobin. Body mass index, preoperative hemoglobin, and the need for continuous intraoperative norepinephrine were also associated with PMI.
Comparison with previous studies
Preoperative copeptin3
Our study shows that there was an association between preoperatively elevated copeptin and MACCE and/or all-cause mortality at 12 months. Prior studies have shown that elevated preoperative copeptin values are associated with poor postoperative outcomes.9,21,22
In terms of mortality and MACCE, Jarai et al.21 examined 198 patients undergoing vascular surgery and concluded that a preoperative copeptin threshold of 14 pmol·L−1 was associated with a two-year incidence of MACCE with an HR of 2.8 (95% CI, 1.5 to 5.5) when accounting for type of surgery, history of myocardial infarction, preoperative cardiac troponin, and preoperative N-terminal pro-B-type natriuretic peptide (NT-proBNP). Investigating the incremental value of copeptin in addition to NT-proBNP, subgroup analyses revealed that especially patients at low estimated risk according to plasma NT–pro-BNP levels were at significantly higher risk for worse outcomes with higher copeptin levels (HR, 5.983; 95% CI, not reported). Schrimpf et al.22 examined 477 patients undergoing vascular surgery and found preoperative copeptin to be associated with 30-day MACCE (n = 41) defined as cardiac death (n = 1) or perioperative myocardial infarction, or elevation of cardiac troponin with measurements prompted by clinical suspicion (n = 46, subdivision unclear). The breakdown of MACCE supports an association with myocardial injury, but not necessarily with mortality. Preoperative copeptin concentrations were higher in patients with MACCE than in those without (median [range], 18.89 [≤ 4.8–180.7] vs 9.75 pmol·L−1 [≤ 4.8–321.6]; P < 0.001; 95% CI not reported). The area under the receiver operating characteristic of postoperative copeptin and the RCRI for predicting MACCE was 0.752 (95% CI not reported) (RCRI only, 0.714; DeLong P = 0.04; 95% CI not reported).
In terms of myocardial injury, an earlier study9 of 190 adult patients undergoing elevated risk noncardiac surgery (general, orthopedic, and vascular), showed that preoperative copeptin concentrations greater than 10 pmol·L−1 were associated with significantly higher rates of myocardial injury with an OR of 4.67 (95% CI, 2.06 to 11.19) when adjusted for age, sex, and the RCRI. Even when additionally accounting for (NT-proBNP), copeptin remained similarly predictive of myocardial injury. This study, which used a slightly higher cut-off (14 pmol·L−1 as employed in the Jarai study) in another population but largely at the same institution, and with a more stringent definition of ischemia, failed to find as association of preoperative copeptin with PMI.
In comparison with other studies, the patients in our study had no significant differences in the baseline characteristics. Unfortunately, the baseline characteristics in the other studies were not as detailed as in the current study, so a lot of factors could not be compared. For example, the mean age of participants in the studies was between 69 and 73 yr, most of the population were male, and the operations lengths were more or less the same. The study of Mauermann et al. included significantly more patients with a history of coronary heart disease and in the study of Schrimpf et al. the mean preoperative creatinine clearance was lower compared with the others. Our study was more heterogenous in terms of the types of surgery included.9,21,22
Taken together with the above studies, our study suggests that preoperative copeptin is indeed associated with midterm cardiac events in a wide variety of patients. Although only an explorative outcome, the lack of a difference in 30-day survival for elevated preoperative copeptin may be due to a limited number of events and/or may suggest that copeptin is a marker of underlying disease and disease severity rather than of postoperative risk. This interpretation may also explain why preoperative copeptin in this study was not associated with PMI (defined as a delta increase in this study, i.e., a dynamic increase from surgery), while previous studies had found preoperative copeptin to be associated with myocardial injury after noncardiac surgery (defined as an elevated postoperative troponin regardless of preoperative measurements, i.e., also including patients with troponinemia, i.e., a baseline state).
Postoperative copeptin and timing of measurement
Unlike preoperative measurements, uncertainty remains regarding the value and timing of postoperative copeptin in predicting adverse events. Only the study by Schrimpf et al.22 examined postoperative copeptin concentrations (on POD 1) in vascular patients. They found copeptin concentrations to be higher on POD 1 than preoperatively (median [IQR], 23.55 [11.50–59.9] vs 10.16 pmol·L−1 [5.67–18.07], 95% CI not reported), which is also supported by our data. The results of this study also confirm that copeptin levels generally return to near preoperative levels by POD 2–4.
In terms of mortality and MACCE, this study also shows that implementing the preoperative copeptin cut-off of 14 pmol·L−1 on POD 2–4 may be justified. For simplicity, we used the preoperative cut-off in this study, which was very similar to our Youden’s optimum for copeptin on POD 2–4 and all-cause mortality and/or MACCE. In addition, while the association with MACCE and/or all-cause mortality at 12 months was similar between preoperative and postoperative measurements, only postoperative copeptin was associated with MACCE and/or all-cause mortality during the first 30 postoperative days. Although there were a limited number of events, this finding may also underscore that postoperative measurements dynamically reflect changes occurring during the perioperative period (e.g., blood loss, fluid administration, surgical time, use of vasoactive agents, transfusion, hypotension, osmolality,12,37,38 physiologic stress,16 etc.).
In terms of myocardial injury, we had previously measured copeptin and cardiac troponin at 0 hr, 2 hr, 4 hr, 6 hr, 8 hr, and on POD 1 and 3 in a small pilot study.20 This pilot study suggested copeptin immediately after surgery to be most promising for identifying myocardial injury. As suggested by the pilot, we found a statistically significantly higher OR for PMI in immediate postoperative copeptin, but not for preoperative copeptin. Nevertheless, the magnitude of effect was modest and based on an internally derived cut-off, which may have led to overfitting.
Clinical relevance
This study clearly shows that copeptin measured preoperatively, immediately postoperatively and on POD 2–4 may be used to risk stratify a broad group of patients for MACCE-free survival at 12 months. This association remained robust when adjusting for a number of variables, particularly for preoperative copeptin and copeptin on POD 2–4. Interestingly, postoperative measurements were associated with 30-day MACCE-free survival, suggesting that these may better reflect perioperative factors, while preoperative copeptin may better mirror baseline risk. Additionally, we showed that the preoperative cut-off of 14 pmol·L−1 may be justified for postoperative measurements on POD 2–4.
No robust association between perioperative copeptin and PMI was found, suggesting that PMI may be a different rather than a surrogate endpoint for all-cause mortality and/or MACCE. The clinical utility of immediate postoperative copeptin for predicting myocardial injury was limited in this study.
Limitations
While our study had several strengths (size, mixed population, high degree of completeness, hard outcomes), it also has some important limitations.
First, despite being a prospective study with the largest sample and event sizes examining copeptin, data were only collected in two centres and extrapolation to other settings may be difficult. As a result, findings should be extrapolated to other patient populations with caution and further studies are needed to confirm our findings.
Second, some other useful indicators of surgical stress (such as C-reactive protein or the neutrophil-lymphocyte-ratio) as well as some other biomarkers of cardiac stress (NT-proBNP) were not uniformly collected. Nevertheless, our intention was to evaluate the prognostic value of copeptin in addition to routinely measured clinical values.
Third, our model was powered to adjust for the RCRI and up to two other variables (models 1A, 2A, and 3A), which seemed reasonable given the clinical value of the RCRI as in line with previous copeptin publications. Nonetheless, the association was robust even when adding a number of additional variables (models 1B, 2B, and 3B).
Fourth, the timing of postoperative copeptin in this study (POD 2–4) was broadly defined as we wanted to attain the last reasonable measurement prior to discharge rather than define a specific timepoint.
Summary and conclusion
The results of the present prospective observational cohort study suggest that perioperative copeptin concentrations can help identify patients at risk for all-cause mortality and/or MACCE. Other identified risk factors were revised cardiac risk index, body mass index, surgical risk, and preoperative hemoglobin.
References
Lee TH, Marcantonio ER, Mangione CM, et al. Derivation and prospective validation of a simple index for prediction of cardiac risk of major noncardiac surgery. Circulation 1999; 100: 1043–9. https://doi.org/10.1161/01.cir.100.10.1043
Devereaux PJ, Sessler DI. Cardiac complications in patients undergoing major noncardiac surgery. N Engl J Med 2015; 373: 2258–69. https://doi.org/10.1056/nejmra1502824
Devereaux PJ, Biccard BM, Sigamani A, et al. Association of postoperative high-sensitivity troponin levels with myocardial injury and 30-day mortality among patients undergoing noncardiac surgery. JAMA 2017; 317: 1642–51. https://doi.org/10.1001/jama.2017.4360
Devereaux PJ, Xavier D, Pogue J, et al. Characteristics and short-term prognosis of perioperative myocardial infarction in patients undergoing noncardiac surgery: a cohort study. Ann Intern Med 2011; 154: 523–8. https://doi.org/10.7326/0003-4819-154-8-201104190-00003
Kristensen SD, Knuuti J, Saraste A, et al. 2014 ESC/ESA Guidelines on non-cardiac surgery: cardiovascular assessment and management: the Joint Task Force on non-cardiac surgery: cardiovascular assessment and management of the European Society of Cardiology (ESC) and the European Society of Anaesthesiology (ESA). Eur Heart J 2014; 35: 2383–431. https://doi.org/10.1093/eurheartj/ehu282
Duceppe E, Yusuf S, Tandon V, et al. Design of a randomized placebo-controlled trial to assess dabigatran and omeprazole in patients with myocardial injury after noncardiac surgery (MANAGE). Can J Cardiol 2018; 34: 295–302. https://doi.org/10.1016/j.cjca.2018.01.020
Roth S, Huhn R, Jung C, Polzin A, De Hert S, Lurati Buse G. Cardiac biomarkers in noncardiac surgery patients : review of cardiac biomarkers for risk stratification and detection of postoperative adverse cardiac events [German]. Med Klin Intensivmed Notfmed 2021; 117: 381–8. https://doi.org/10.1007/s00063-021-00788-2
Ryding AD, Kumar S, Worthington AM, Burgess D. Prognostic value of brain natriuretic peptide in noncardiac surgery: a meta-analysis. Anesthesiology 2009; 111: 311–9. https://doi.org/10.1097/aln.0b013e3181aaeb11
Mauermann E, Bolliger D, Seeberger E, et al. Incremental value of preoperative copeptin for predicting myocardial injury. Anesth Analg 2016; 123: 1363–71. https://doi.org/10.1213/ane.0000000000001635
Rodseth RN, Biccard BM, Le Manach Y, et al. The prognostic value of pre-operative and post-operative B-type natriuretic peptides in patients undergoing noncardiac surgery: B-type natriuretic peptide and N-terminal fragment of pro-B-type natriuretic peptide: a systematic review and individual patient data meta-analysis. J Am Coll Cardiol 2014; 63: 170–80. https://doi.org/10.1016/j.jacc.2013.08.1630
Vernooij LM, van Klei WA, Moons KG, Takada T, van Waes J, Damen JA. The comparative and added prognostic value of biomarkers to the Revised Cardiac Risk Index for preoperative prediction of major adverse cardiac events and all-cause mortality in patients who undergo noncardiac surgery. Cochrane Database Syst Rev 2021; 12: CD013139. https://doi.org/10.1002/14651858.cd013139.pub2
Bolignano D, Cabassi A, Fiaccadori E, et al. Copeptin (CTproAVP), a new tool for understanding the role of vasopressin in pathophysiology. Clin Chem Lab Med 2014; 52: 1447–56. https://doi.org/10.1515/cclm-2014-0379
Szarpak L, Lapinski M, Gasecka A, et al. Performance of copeptin for early diagnosis of acute coronary syndromes: a systematic review and meta-analysis of 14,139 patients. J Cardiovasc Dev Dis 2021; 9: 6. https://doi.org/10.3390/jcdd9010006
Möckel M, Searle J. Copeptin-marker of acute myocardial infarction. Curr Atheroscler Rep 2014; 16: 421. https://doi.org/10.1007/s11883-014-0421-5
Möckel M, Searle J, Hamm C, et al. Early discharge using single cardiac troponin and copeptin testing in patients with suspected acute coronary syndrome (ACS): a randomized, controlled clinical process study. Eur Heart J 2015; 36: 369–76. https://doi.org/10.1093/eurheartj/ehu178
Mueller C, Giannitsis E, Möckel M, et al. Rapid rule out of acute myocardial infarction: novel biomarker-based strategies. Eur Heart J Acute Cardiovasc Care 2017; 6: 218–22. https://doi.org/10.1177/2048872616653229
Mueller C, Möckel M, Giannitsis E, et al. Use of copeptin for rapid rule-out of acute myocardial infarction. Eur Heart J Acute Cardiovasc Care 2018; 7: 570–6. https://doi.org/10.1177/2048872617710791
Mueller C. Biomarkers and acute coronary syndromes: an update. Eur Heart J 2014; 35: 552–6. https://doi.org/10.1093/eurheartj/eht530
Raskovalova T, Twerenbold R, Collinson PO, et al. Diagnostic accuracy of combined cardiac troponin and copeptin assessment for early rule-out of myocardial infarction: a systematic review and meta-analysis. Eur Heart J Acute Cardiovasc Care 2014; 3: 18–27. https://doi.org/10.1177/2048872613514015
Kamber F, Mauermann E, Seeberger E, et al. Peri-operative copeptin concentrations and their association with myocardial injury after vascular surgery: a prospective observational cohort study. Eur J Anaesthesiol 2018; 35: 682–90. https://doi.org/10.1097/eja.0000000000000815
Jarai R, Mahla E, Perkmann T, et al. Usefulness of pre-operative copeptin concentrations to predict post-operative outcome after major vascular surgery. Am J Cardiol 2011; 108: 1188–95. 0.1016/j.amjcard.2011.06.024
Schrimpf C, Gillmann HJ, Sahlmann B, et al. Renal function interferes with copeptin in prediction of major adverse cardiac events in patients undergoing vascular surgery. PLoS One 2015; 10: e0123093. https://doi.org/10.1371/journal.pone.0123093
Lipinski MJ, Escárcega RO, D'Ascenzo F, et al. A systematic review and collaborative meta-analysis to determine the incremental value of copeptin for rapid rule-out of acute myocardial infarction. Am J Cardiol 2014; 113: 1581–91. https://doi.org/10.1016/j.amjcard.2014.01.436
von Elm E, Altman DG, Egger M, Pocock SJ, Gøtzsche PC, Vandenbroucke JP. The Strengthening the Reporting of Observational Studies in Epidemiology (STROBE) statement: guidelines for reporting observational studies. Lancet 2007; 370: 1453–7. https://doi.org/10.1016/s0140-6736(07)61602-x
Glance LG, Lustik SJ, Hannan EL, et al. The Surgical Mortality Probability Model: derivation and validation of a simple risk prediction rule for noncardiac surgery. Ann Surg 2012; 255: 696–702. https://doi.org/10.1097/sla.0b013e31824b45af
Botto F, Alonso-Coello P, Chan MT, et al. Myocardial injury after noncardiac surgery: a large, international, prospective cohort study establishing diagnostic criteria, characteristics, predictors, and 30-day outcomes. Anesthesiology 2014; 120: 564–78. https://doi.org/10.1097/aln.0000000000000113
Jaffe AS, Ordonez-Llanos J. High sensitivity troponin in chest pain and acute coronary syndromes. A step forward? Rev Esp Cardiol 2010; 63: 763–9. https://doi.org/10.1016/s1885-5857(10)70160-2
Giannitsis E, Kurz K, Hallermayer K, Jarausch J, Jaffe AS, Katus HA. Analytical validation of a high-sensitivity cardiac troponin T assay. Clin Chem 2010; 56: 254–61. https://doi.org/10.1373/clinchem.2009.132654
Jammer I, Wickboldt N, Sander M, et al. Standards for definitions and use of outcome measures for clinical effectiveness research in perioperative medicine: European Perioperative Clinical Outcome (EPCO) definitions: a statement from the ESA-ESICM joint taskforce on perioperative outcome measures. Eur J Anaesthesiol 2015; 32: 88–105. https://doi.org/10.1097/eja.0000000000000118
Devereaux PJ, Szczeklik W. Myocardial injury after non-cardiac surgery: diagnosis and management. Eur Heart J 2020; 41: 3083–91. https://doi.org/10.1093/eurheartj/ehz301
Thygesen K, Alpert JS, Jaffe AS, et al. Fourth universal definition of myocardial infarction (2018). J Am Coll Cardiol 2018; 72: 2231–64. https://doi.org/10.1016/j.jacc.2018.08.1038
Lurati Buse GA, Bolliger D, Seeberger E, et al. Troponin T and B-type natriuretic peptide after on-pump cardiac surgery: prognostic impact on 12-month mortality and major cardiac events after adjustment for postoperative complications. Circulation 2014; 130: 948–57. https://doi.org/10.1161/circulationaha.113.007253
Peduzzi P, Concato J, Feinstein AR, Holford TR. Importance of events per independent variable in proportional hazards regression analysis. II. Accuracy and precision of regression estimates. J Clin Epidemiol 1995; 48: 1503–10. https://doi.org/10.1016/0895-4356(95)00048-8
Riley RD, Snell KI, Ensor J, et al. Minimum sample size for developing a multivariable prediction model: PART II—binary and time-to-event outcomes. Stat Med 2019; 38: 1276–96. https://doi.org/10.1002/sim.7992
Riley RD, Ensor J, Snell KI, et al. Calculating the sample size required for developing a clinical prediction model. BMJ 2020; 368: m441. https://doi.org/10.1136/bmj.m441
Fleisher LA, Fleischmann KE, Auerbach AD, et al. 2014 ACC/AHA guideline on perioperative cardiovascular evaluation and management of patients undergoing noncardiac surgery: a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines. Circulation 2014; 130: e278–333. https://doi.org/10.1161/cir.0000000000000105
Ball SG. Vasopressin and disorders of water balance: the physiology and pathophysiology of vasopressin. Ann Clin Biochem 2007; 44: 417–31. https://doi.org/10.1258/000456307781646030
Christ-Crain M. Vasopressin and copeptin in health and disease. Rev Endocr Metab Disord 2019; 20: 283–94. https://doi.org/10.1007/s11154-019-09509-9
Author contributions
Firmin Kamber and Eckhard Mauermann contributed to all aspects of this manuscript, including conception and design; acquisition, analysis, and interpretation of data; and drafting the article. Sebastian Roth contributed to the acquisition of data and to the conception and design of the study. Esther Seeberger and Johannes Nienhaus contributed to the acquisition of data. Daniel Bolliger, Christian Muelle, and Giovanna Lurati Buse contributed to the conception and design of the study and to the interpretation of data.
Acknowledgements
We would like to thank Allison Dwileski for editorial assistance as well as the statisticians from the Clinical Trials Unit.
Disclosures
Christian Mueller has received research grants from Abbott, ALERE, Astra Zeneca, Brahms, Biomerieux, Critical Diagnostics, Nanosphere, Roche, Siemens, Singulex, and speaker or consulting honoraria from Abbott, ALERE, Astra Zeneca, Biomerieux, BMS, Brahms, Cardiorentis, Daiichi Sankyo, Novartis, Roche, Sanofi, Siemens and Singulex.
Funding statement
This work was supported by the Clinic for Anaesthesia, Intermediate Care, Prehospital Emergency Medicine and Pain Therapy, University Hospital Basel, Switzerland. Copeptin kits were provided free of charge by Thermo Fisher Scientific. Christian Mueller has received research grants from Abbott, ALERE, Astra Zeneca, Brahms, Biomerieux, Critical Diagnostics, Nanosphere, Roche, Siemens, Singulex, and speaker or consulting honoraria from Abbott, ALERE, Astra Zeneca, Biomerieux, BMS, Brahms, Cardiorentis, Daiichi Sankyo, Novartis, Roche, Sanofi, Siemens and Singulex.
Prior conference presentations
Preliminary data were presented at the 2022 Jahreskongress der Deutschen Gesellschaft für Anästhesiologie und Intensivmedizin (12–14 May, Hamburg, Germany).
Editorial responsibility
This submission was handled by Dr. Stephan K. W. Schwarz, Editor-in-Chief, Canadian Journal of Anesthesia/Journal canadien d’anesthésie.
Funding
Open access funding provided by University of Basel.
Author information
Authors and Affiliations
Corresponding author
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License, which permits any non-commercial use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc/4.0/.
About this article
Cite this article
Kamber, F., Roth, S., Bolliger, D. et al. Perioperative copeptin: predictive value and risk stratification in patients undergoing major noncardiac surgery—a prospective observational cohort study. Can J Anesth/J Can Anesth 71, 330–342 (2024). https://doi.org/10.1007/s12630-023-02677-y
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12630-023-02677-y