Abstract
Purpose
During peripheral nerve block procedures, needle visibility decreases as the angle of needle insertion relative to skin increases due to loss of reflective signals. The primary aim of our study was to compare the effect of beam steering on the visibility of echogenic and non-echogenic block needles.
Methods
PAJUNK® non-echogenic and echogenic needles were inserted into pork meat at 20°, 40°, 60°, and 70° angles, and electronic beam steering was applied at three different angles (shallow, medium, and steep) to obtain the best possible needle images. Eleven anesthesiologists blinded to the type of needle or use of beam steering scored the images obtained (0 = needle not visible; 10 = excellent needle shaft and tip visibility). Mean scores were used to classify the needles as poor visibility (mean score 0-3.3), intermediate visibility (mean score 3.4-6.6), or good visibility (mean score 6.7-10).
Results
At 20°, the visibility scores were intermediate to good in all groups. At 40°, the mean (SD) visibility score for the non-echogenic needle improved significantly from 3.1 (1.4) to 7.9 (1.8) with application of beam steering (difference = 4.8; 95% confidence interval [CI]: 3.1 to 6.6; P < 0.001). At 60°, the mean (SD) visibility score for the non-echogenic needle was poor 0.6 (0.7) and remained poor 2.4 (1.1) with beam steering. One the other hand, the echogenic needle without beam steering 6.5 (1.8) scored significantly better than the non-echogenic needle with beam steering 2.4 (1.1) (difference = 4.2; 95% CI: 2.7 to 5.6; P < 0.001). At 70°, the mean needle visibility score was poor for the non-echogenic needle with or without beam steering. In contrast, the echogenic needle attained an intermediate visibility score with or without beam steering. Beam steering did not significantly change the visibility scores of either the echogenic or the non-echogenic needle (P = 0.088 and 0.056, respectively) at a 70° angle.
Conclusion
The PAJUNK echogenic needle, with or without beam steering, was more visible when compared with the non-echogenic needle at 60° and 70° angles of insertion. In contrast, at a 40° angle of needle insertion, the non-echogenic needle with beam steering was more visible compared with the echogenic needle.
Résumé
Objectif
Au cours des procédures de bloc nerveux périphérique, la visibilité de l’aiguille diminue lorsque l’angle d’insertion de l’aiguille par rapport à la peau augmente, du fait d’une perte des signaux réfléchis. L’objectif principal de notre étude était de comparer l’effet de l’orientation du faisceau sur la visibilité des aiguilles échogènes et non-échogènes utilisées pour des blocs.
Méthodes
Des aiguilles échogènes et non-échogènes PAJUNK® ont été insérées dans de la viande de porc selon des angles de 20°, 40°, 60° et 70° et une orientation électronique de l’angle a été appliquée selon trois angles différents (peu profond, moyen et profond) pour obtenir les meilleures images possibles des aiguilles. Onze anesthésiologistes tenus dans l’ignorance du type d’aiguille utilisé ou de l’orientation du faisceau ont coté les images obtenues sur une échelle de 0 à 10 (0 = aiguille non visible; 10 = excellente visibilité du corps et de la pointe de l’aiguille). Les scores moyens ont servi à classer les aiguilles selon une mauvaise visibilité (score moyen 0 à 3,3), visibilité intermédiaire (score moyen 3,4 à 6,6), ou bonne visibilité (score moyen 6,7 à 10).
Résultats
À 20°, les scores de visibilité étaient intermédiaires à bons dans tous les groupes. À 40°, le score moyen (ET) de visibilité pour l’aiguille non-échogène a été significativement amélioré de 3,1 (1,4) à 7,9 (1,8) avec l’application de l’orientation du faisceau (différence = 4,8; intervalle de confiance à 95 % [IC]: 3,1 à 6,6; P < 0,001). À 60°, le score moyen (ET) de visibilité de l’aiguille non-échogène était mauvais 0,6 (0,7) et est resté mauvais à 2,4 (1,1) avec l’orientation du faisceau. D’un autre côté, le score de l’aiguille échogène sans orientation du faisceau a été significativement meilleur à 6,5 (1,8) que celui de l’aiguille non-échogène avec orientation du faisceau à 2,4 (1,1) (différence = 4,2; IC à 95 %: 2,7 à 5,6; P < 0,001). À 70°, le score moyen de visibilité était mauvais pour l’aiguille non-échogène, avec ou sans orientation du faisceau. En revanche, l’aiguille échogène atteignait un score de visibilité intermédiaire avec ou sans orientation du faisceau. L’orientation du faisceau n’a pas significativement modifié les scores de visibilité de l’aiguille échogène ou de l’aiguille non-échogène (respectivement P = 0,088 et 0,056) à un angle de 70°.
Conclusion
L’aiguille échogène PAJUNK, avec ou sans orientation du faisceau, a été davantage visible que l’aiguille non-échogène avec des angles d’insertion de 60° et 70°. En revanche, à un angle d’insertion de l’aiguille de 40°, l’aiguille non-échogène avec orientation du faisceau a été plus visible que l’aiguille échogène.
Similar content being viewed by others
Visualization of the needle is important for safe and effective ultrasound-guided peripheral nerve block (PNB).1 The most common error of novice and experienced operators while performing ultrasound-guided PNBs is failure to visualize the needle prior to advancement.2 Previous studies have shown that needle visibility becomes poor as the angle of needle insertion increases in relation to the ultrasound probe due to reflective signal losses.3,4 Several techniques are now available to improve needle visibility, including echogenic needle design and electronic beam steering.5-8 Echogenic needles have reflective surfaces like Cornerstone reflectors that increase the number of ultrasound waves returning to the transducer; however, they are more expensive than the corresponding non-echogenic needles. Electronic beam steering is a technique that steers the incident ultrasound beam perpendicular to the angle of needle insertion to increase the amount of reflected ultrasound waves and can be an alternative to the use of echogenic needles. According to the law of reflection, the angle of incidence equals the angle of reflection; therefore, by directing the ultrasound beam perpendicular to the needle, the ultrasound waves can be reflected back to ultrasound probe, leading to enhanced needle visibility. Electronic beam steering, a software upgrade (known as EMB for the SonoSite ultrasound machine) for a multibeam transducer, entails a one-time installation cost. Beam steering has yet to be evaluated for its applicability in regional anesthesia as compared with the echogenic needle design. The aim of our study was to compare the effect of beam steering on the visibility of the echogenic and non-echogenic needles.
Methods
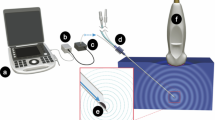
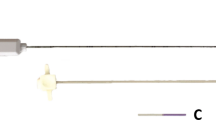
The University of Western Ontario Health Sciences Research Ethics Board (HSREB) deemed that ethical approval was unnecessary for this laboratory-based study (April 2013). Previous studies have shown that the PAJUNK® (NanoLine PAJUNK, Medizintechnologie GmbH, Geisingen, Germany) echogenic needles scored the best amongst all current commercially available echogenic needles.9,10 We therefore chose to compare the PAJUNK UniPlex NanoLine (non-echogenic, 22G, 80 mm) and PAJUNK SonoPlex Stim (echogenic, 22G, 80 mm) needles for the study. While the PAJUNK SonoPlex Stim echogenic needles were obtained from the manufacturer, the manufacturer had no influence on any aspect of the study design or data analysis. Electronic beam steering was already installed in the ultrasound machine available in our institution and was not specifically purchased for the purpose of the study. Both the echogenic and non-echogenic needles were inserted into uncooked pork meat (pork roast) at 20°, 40°, 60°, and 70° angles to a length of 60 mm. The angle of needle insertion was defined as the angle between the needle and the surface of pork meat. A high-frequency linear probe (7-13 MHz) was prepared using transparent Tegaderm™ dressing, taking care that no air was trapped between the ultrasound probe and the dressing. Using ultrasound gel as a coupling medium, the ultrasound probe was positioned on the surface of the pork meat in such a manner that the needle shaft and the tip were visible in-plane to the ultrasound beam. An experienced clinician (S.G.) performed all needle insertions and aligned the ultrasound probe to obtain the best possible needle images (snapshots) for storage to reduce the confounding factors of image acquisition. This ensured the best possible needle visibility results during the study. The angle of needle insertion was confirmed by using the built-in protractor of the ultrasound machine (SonoSite M-Turbo®, Bothel, WA, USA) as shown in Fig. 1. The ultrasound image of the non-echogenic needle was recorded to serve as a control. Beam steering was then applied at shallow, medium, and steep angles to obtain the best possible needle images. The same process was repeated for the echogenic needle.
At each angle of needle insertion, eight ultrasound images of the needle were obtained:
-
1.
Non-echogenic needle without beam steering (one image);
-
2.
Non-echogenic needle with beam steering: shallow, medium, and steep (three images);
-
3.
Echogenic needle without beam steering (one image);
-
4.
Echogenic needle with beam steering: shallow, medium, and steep (three images).
Four needle insertion angles (20, 40, 60, and 70°) were studied, producing a total of 32 images. The images were transferred to a laptop computer and evaluated by eleven anesthesiologists (five consultants, five fellows, and one resident) who were blinded to the type of needle and use of beam steering. All anesthesiologists who regularly worked in the block room during the time of the study were approached for participation in the study. The sample size was one of convenience.
To enable the blinding process, multiple ultrasound images were presented to the anesthesiologists for scoring needle visibility. The experience of the evaluators in performing ultrasound-guided nerve blocks was as follows: consultants > 500; anesthesia fellows < 200, but routinely used ultrasound for central venous catheter insertions; and the anesthesia resident < ten. This allowed scoring by anesthesiologists of varied levels of experience with use of ultrasound guidance for needle visualization. The anesthesiologists were asked to score needle visibility in the recorded images (0 = no needle visible; 10 = excellent needle tip and shaft visibility). They were shown an example of an image that would score 10 and an example that would score 0. They were asked to give a higher score if they considered the needle tip to be clearly visible. Mean scores were used to classify needles as poor visibility (mean score 0-3.3), intermediate visibility (mean score 3.4-6.6), and good visibility (mean score 6.7-10).
In clinical practice, when the angle of needle insertion is approximately 20°, use of a shallow angle of beam steering is likely to be optimal to achieve best return of the ultrasound beam; whereas, for steeper angles of needle insertion, such as 60° or 70°, beam steering at a steep angle may optimize the image. Therefore, for analysis, shallow beam steering was used for a 20° angle of needle insertion, medium beam steering was used for a 40° angle of needle insertion, and steep beam steering was used for 60° and 70° angles of needle insertion. Thus, at each angle of needle insertion four images were analyzed: non-echogenic needle without beam steering, non-echogenic needle with beam steering, echogenic needle without beam steering, and echogenic needle with beam steering.
For each angle of needle insertion, needle visibility scores were analyzed using 2 × 2 repeated-measures analysis of variance to evaluate the use of needle type (echogenic or non-echogenic) and beam steering (yes or no). Pairwise comparisons were evaluated using Tukey’s test, for which corrected confidence intervals and P values are reported. All reported P values are two-sided. Statistical analyses were performed using SAS® version 9.3 (SAS Institute Inc., Cary, NC, USA).
Results
Eleven anesthesiologists with varied levels of experience in performing ultrasound-guided PNBs and central venous catheter insertions scored the images obtained. Visibility scores were similar for experienced (consultants) and less experienced (trainees) anesthesiologists (results not shown).
Figure 2 shows the individual needle trajectory visibility scores over the different angles for each factor combination, i.e., beam steering (BS) and echogenic needle (E). Solid lines represent visibility scores for experienced (consultants) and dashed lines represent visibility scores for less experienced (trainees) anesthesiologists.
The individual trajectories of outcome over different angles for each factor combination, BS (beam steering) and E (echogenic needle). Solid lines represent visibility scores for experienced (consultants), and dotted lines represent visibility scores for less experienced (trainees) anesthesiologists. 1 = Non-echogenic needle, no beam steering 2 = Non-echogenic needle, beam steering used. 3 = Echogenic needle, no beam steering. 4 = Echogenic needle, beam steering used
The visibility scores for 20°, 40°, 60°, and 70° angles are shown in Fig. 3 and are summarized in Table 1. Pairwise comparisons for the four angles of needle insertion are reported in Table 2.
Dot plots for needle visibility score at 20°, 40°, 60°, and 70° angles of needle insertion. Connecting lines indicate mean value. NE/NBS = non-echogenic needle, no beam steering; NE/BS = non-echogenic needle, beam steering used; E/NBS = echogenic needle, no beam steering; E/BS = echogenic needle, beam steering used
Needle visibility at a 20° angle of needle insertion
For the 20° angle of needle insertion, the control group (non-echogenic needle with no beam steering) had an intermediate visibility score, while the mean needle visibility score for all other groups was good (Table 1). There was a statistically significant interaction between beam steering and needle type (P = 0.028), and pairwise comparisons showed that the control group was significantly different from the other three groups, while differences among the other three groups were not statistically significant (Table 2).
Needle visibility at a 40° angle of needle insertion
For the 40° angle of needle insertion, the non-echogenic needle with beam steering had a good visibility score (Table 1). The echogenic needle with or without beam steering had intermediate visibility scores. The control group scored poorly at this angle. There was a statistically significant interaction between beam steering and needle type (P < 0.001). Pairwise comparison showed that the non-echogenic needle with beam steering group was significantly different from the other three groups, while differences among the other three groups were not statistically significant (Table 2).
Needle visibility at a 60° angle of needle insertion
The echogenic needle with or without beam steering had an intermediate visibility score. The mean visibility scores of the non-echogenic needle were poor with or without beam steering. There was a statistically significant interaction between beam steering and needle type (P = 0.045). Pairwise comparison showed that the visibility scores of the echogenic needle were significantly higher than those of the non-echogenic groups (Table 2). Application of beam steering to the echogenic needle did not change visibility scores of this needle (P = 0.068). For the non-echogenic needle, application of beam steering made a statistically significant change in the visibility scores (0.013).
Needle visibility at a 70° angle of needle insertion
The mean needle visibility scores were poor for the non-echogenic needle with or without beam steering, while the echogenic needle showed intermediate visibility scores with or without beam steering. There was no interaction between beam steering and needle type (P = 0.821). Pairwise comparison showed that the visibility scores of the echogenic needle with or without beam steering were higher than those of the non-echogenic needle with or without beam steering (Table 2). Beam steering did not influence the visibility scores of either the echogenic or the non-echogenic needles.
Discussion
This study shows the effect of different angles of beam steering on the visibility of echogenic and non-echogenic needles at various angles of needle insertion. The visibility of the PAJUNK echogenic needle, with or without beam steering, was better than that of the non-echogenic needle at 60° and 70° angles of insertion. At a 40° angle of insertion, the visibility of the non-echogenic needle with beam steering was better than that of the echogenic needle with or without beam steering.
It is well known that needle visibility decreases as the angle of needle insertion increases.3,4 Various methods have been used to improve needle visualization, including use of a needle with a larger diameter, use of an echogenic needle, mechanical and optical needle guides, Doppler signals, oscillating air columns, electronic beam steering, and spatial compound imaging.11-15 When direct needle visualization is difficult, surrogate markers of needle tip location have to be used, such as tissue movement, hydrolocation, colour Doppler, and microbubble injection.16-18 Nevertheless, surrogate markers have their own disadvantages. For example, the use of microbubbles can cause deterioration of the image quality of target structures. Therefore, it is reasonable to use currently available technology to optimize needle visualization to facilitate regional anesthesia procedures.
These findings may have important implications regarding the selection of block needles and use of beam steering technology while performing ultrasound-guided needling procedures (PNBs and other clinical procedures, including needle-localized breast biopsy). At a 20° angle of needle insertion, both echogenic and non-echogenic needles had moderate to good visibility with or without electronic beam steering due to specular reflection of the incident rays. Consequently, use of a non-echogenic needle is appropriate either with or without beam steering. This concept will apply to superficial blocks such as axillary and interscalene brachial plexus blocks. At a 40° angle of needle insertion, electronic beam steering improved the visibility of the non-echogenic needle from poor to good visibility. In other words, electronic beam steering was an effective modality when the angle of needle insertion was 40° in relation to the ultrasound probe. The type of needle used did not affect needle visibility at this angle of needle insertion. Interestingly, the beam-steered non-echogenic needle was more visible than the echogenic needle with or without beam steering. The lower visibility scores for the echogenic needle at this angle of needle insertion may be due to scattering of the ultrasound beam by the Cornerstone reflector, whereas the smooth surface of the non-echogenic needle may lead to more uniform reflection of ultrasound waves back to the transducer when the angle of incidence of ultrasound waves is perpendicular to the needle. It is also possible that the higher visibility of the beam-steered non-echogenic needle compared with the echogenic needle (at this particular angle) may be a “random high”, and this may require confirmation through replication of the experiment. The electronic beam steering did not improve the visibility of the echogenic needle. This is an important finding, as the non-echogenic needle with the aid of beam steering may be adequate with little role from an echogenic needle if the estimated needle trajectory is expected to be about 40° as assessed during the pre-procedural scan. Nevertheless, if electronic beam steering is not available, the echogenic needle can provide intermediate needle visibility on its own.
At 60° and 70° angles of needle insertion, the visibility of the non-echogenic needle was poor and remained poor even with electronic beam steering. At a 60° angle of insertion, the echogenic needle showed intermediate visibility without beam steering, which improved to good visibility with application of beam steering. At a 70° angle of needle insertion, the echogenic needle showed intermediate needle visibility which showed little improvement with the application of electronic beam steering. Therefore, we can recommend that echogenic needles should be used when the angle of needle insertion is expected to be 60° or 70° (e.g., while performing ultrasound-guided infraclavicular brachial plexus block), particularly in obese patients.19 Electronic beam steering might have little role in such circumstances. The interaction between the angle of needle insertion, beam steering, and needle type is yet to be assessed with the use of a low-frequency curved array probe often used for sciatic blocks.
Cheung and Rohling have described the algorithm and principles of physics used to enhance needle visibility by electronic beam steering.20 The angle of needle insertion in clinical practice is dependent on the needle entry point and the depth of the target structure. The current commercially available ultrasound machines steer the ultrasound beams at three fixed angles (shallow, medium, and steep). This is an important limitation, as the steered ultrasound beam may not be exactly perpendicular to the needle shaft surface, which is required for best needle visibility. In the future, the technology may allow us to steer the ultrasound beam directly perpendicular to the needle, enabling better needle visualization. Until such technology is available that allows the ultrasound beam to be steered exactly perpendicular to the angle of needle insertion, the clinical utility of beam steering may be limited except at particular angles of needle insertion. Nevertheless, if the electronic beam steering is pre-installed in the ultrasound machine, it may be prudent to use it if the needle visibility is poor at certain angles.
Our study has several limitations. The study was not designed to replicate a real patient scenario, as needle visibility is a dynamic process. We used pork meat for the study because previous studies recommend that meat-based models are superior to synthetic models (e.g., gel phantoms or water baths) when comparing needle visibility.21,22 The pork meat also had adequate thickness to allow for needle insertion at a steep angle to the desired length. Secondly, we did not look at needle tip and shaft visibility separately; instead, we requested the scorers to score higher if the tip was seen more clearly. This methodology has been used previously by Guo et al. and allows comparison of the overall visibility of the needles.9 Needle tip visibility is a subject of interest with no established single best method of identification. The overall improvement in needle visibility with the use of a new technology may translate to better needle tip visibility with control of other factors of needle visibility. Thirdly, we did not compare different types of echogenic needles and the effect of beam steering on them. Echogenic needles from different manufactures may show differences with the application of beam steering.10 Finally, we did not evaluate whether or not electronic beam steering caused deterioration of the image quality of target structures.
In conclusion, the PAJUNK echogenic needle was more visible compared with the non-echogenic needle at 60° and 70° angles of insertion with or without beam steering; whereas, at a 40° angle of needle insertion, the non-echogenic needle with beam steering was more visible compared with the echogenic needle.
References
Chin KJ, Perlas A, Chan VW, Brull R. Needle visualization in ultrasound-guided regional anesthesia: challenges and solutions. Reg Anesth Pain Med 2008; 33: 532-44.
Sites BD, Spence BC, Gallagher JD, Wiley CW, Bertrand ML, Blike GT. Characterizing novice behavior associated with learning ultrasound-guided peripheral regional anesthesia. Reg Anesth Pain Med 2007; 32: 107-15.
Schafhalter-Zoppoth I, McCulloch CE, Gray AT. Ultrasound visibility of needles used for regional nerve block: an in vitro study. Reg Anesth Pain Med 2004; 29: 480-8.
Nichols K, Wright LB, Spencer T, Culp WC. Changes in ultrasonographic echogenicity and visibility of needles with changes in angles of insonation. J Vasc Interv Radiol 2003; 14: 1553-7.
Deam RK, Kluger R, Barrington MJ, McCutcheon CA. Investigation of a new echogenic needle for use with ultrasound peripheral nerve blocks. Anaesth Intensive Care 2007; 35: 582-6.
Hopkins RE, Bradley M. In-vitro visualization of biopsy needles with ultrasound: a comparative study of standard and echogenic needles using an ultrasound phantom. Clin Radiol 2001; 56: 499-502.
Barr RG. Improved needle visualization with electronic beam steering: proof of concept. Ultrasound Q 2012; 28: 59-64.
Baker JA, Soo MS, Mengoni P. Sonographically guided percutaneous interventions of the breast using a steerable ultrasound beam. AJR Am J Roentgenol 1999; 172: 157-9.
Guo S, Schwab A, McLeod G, et al. Echogenic regional anaesthesia needles: a comparison study in Thiel cadavers. Ultrasound Med Biol 2012; 38: 702-7.
Sviggum HP, Ahn K, Dilger JA, Smith HM. Needle echogenicity in sonographically guided regional anesthesia: blinded comparison of 4 enhanced needles and validation of visual criteria for evaluation. J Ultrasound Med 2013; 32: 143-8.
Phal PM, Brooks DM, Wolfe R. Sonographically guided biopsy of focal lesions: a comparison of freehand and probe-guided techniques using a phantom. AJR Am J Roentgenol 2005; 184: 1652-6.
Tsui BC. Facilitating needle alignment in-plane to an ultrasound beam using a portable laser unit. Reg Anesth Pain Med 2007; 32: 84-8.
Armstrong G, Cardon L, Vilkomerson D, et al. Localization of needle tip with color doppler during pericardiocentesis: in vitro validation and initial clinical application. J Am Soc Echocardiogr 2001; 14: 29-37.
Cockburn JF, Cosgrove DO. Device to enhance visibility of needle or catheter tip at color Doppler US. Radiology 1995; 195: 570-2.
Wiesmann T, Borntrager A, Zoremba M, Neff M, Wulf H, Steinfeldt T. Compound Imaging Technology and Echogenic Needle Design: Effects on Needle Visibility and Tissue Imaging. Reg Anesth Pain Med 2013; 38: 452-5.
Tsui BC, Kropelin B, Ganapathy S, Finucane B. Dextrose 5% in water: fluid medium for maintaining electrical stimulation of peripheral nerves during stimulating catheter placement. Acta Anaesthesiol Scand 2005; 49: 1562-5.
Dhir S, Ganapathy S. Use of ultrasound guidance and contrast enhancement: a study of continuous infraclavicular brachial plexus approach. Acta Anaesthesiol Scand 2008; 52: 338-42.
Sondekoppam RV, Brookes J, Terlecki M, Uppal V, Ganapathy S. Intracatheter air in continuous thoracic paravertebral block: distraction or assistance? Can J Anesth 2013; 60: 824-5.
Uppal V, Kalagara HK, McKinlay S, Macfarlane A, Anderson K. Higher body mass index is associated with greater angle of needle insertion and more difficult needle visualization during lateral sagittal infraclavicular brachial plexus blocks. Reg Anesth Pain Med 2012; 37 (Suppl), E294 (abstract).
Cheung S, Rohling R. Enhancement of needle visibility in ultrasound-guided percutaneous procedures. Ultrasound Med Biol 2004; 30: 617-24.
Hocking G, Hebard S, Mitchell CH. A review of the benefits and pitfalls of phantoms in ultrasound-guided regional anesthesia. Reg Anesth Pain Med 2011; 36: 162-70.
Wiesmann T, Borntrager A, Neff M, Wulf H, Steinfeldt T. Needle visibility in different tissue models for ultrasound-guided regional anaesthesia. Acta Anaesthesiol Scand 2012; 56: 1152-5.
Acknowledgements
We sincerely thank the consultants and fellows from the Department of Anesthesia at the University of Western Ontario who participated in scoring needle visibility for the study. We also thank Mr. Larry Stitt (Department of Biostatistics, Western University) for his input in the statistical interpretation of this study.
Funding
Departmental research funds.
Conflicts of interest
Drs. Uppal and Sondekoppam have no conflict of interest regarding this study. Dr. Ganapathy has received: peer-reviewed funding from Physician Services Incorporated for a study evaluating and comparing the echogenic needle and catheter system with non-echogenic needles; equipment from PAJUNK® MEDIZINTECHNOLOGIE GmbH, Geisingen, Germany for an ongoing study on paravertebral blocks; honoraria from BBraun for taking part in a breakfast panel at the World Congress of Regional Anesthesia and Pain Therapy, Sydney, 2013; equipment support for her workshops (until four years ago) from SonoSite, Zonare, Philips, and GE. Dr. Ganapathy was involved in developing an educational DVD for SonoSite and was in the physician advisory group for SonoSite until six years ago. She has attended one meeting with Arrow Teleflex in May 2013 to discuss recent developments in technology for ultrasound-guided regional anesthesia.
Author information
Authors and Affiliations
Corresponding author
Additional information
This report was awarded 3rd prize for the best e-poster discussion at the 32nd Annual European Society of Regional Anesthesia Congress 2013, Glasgow, UK.
Author contributions
Vishal Uppal and Sugantha Ganapathy made substantial contributions to the conception of the study. Vishal Uppal, Sugantha Ganapathy, and Rakesh V. Sondekoppam were involved in the study design and data collection and helped conduct the study. Vishal Uppal made substantial contributions to the analysis and interpretation of data and wrote the manuscript. Sugantha Ganapathy and Rakesh V. Sondekoppam contributed to the manuscript and critically reviewed and edited the manuscript.
Rights and permissions
About this article
Cite this article
Uppal, V., Sondekoppam, R.V. & Ganapathy, S. Effect of beam steering on the visibility of echogenic and non-echogenic needles: a laboratory study. Can J Anesth/J Can Anesth 61, 909–915 (2014). https://doi.org/10.1007/s12630-014-0207-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12630-014-0207-9