Abstract
Objectives
Evidence on the effectiveness of cooking activities as a well-being promotion intervention for older adults with subjective cognitive decline (SCD) and their caregivers is scarce. In view of this, a randomized controlled trial was conducted to examine whether a dyadic cooking-based intervention can improve the subjective health and well-being of older adults with SCD and their caregivers, as well as the cooking competence of the former group.
Design
Randomized controlled trial.
Setting
Community.
Participants
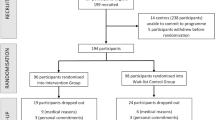
Sixty pairs of community-dwelling older adults aged 60 years or above with SCD (mean age = 78.4 years) and their caregivers (mean age = 65.3 years) were randomly assigned to the intervention group (N = 30 pairs) and the wait-list control group (N = 30 pairs).
Intervention
The intervention was an innovative 5-week (two hours per week) dyadic cooking-based intervention employing procedural learning methods specifically adapted for older adults with SCD.
Measurements
The outcome measures included 1) a well-being index composed by four indicators: life satisfaction, feeling of happiness, sense of purpose and meaning in life, and perceived health, and 2) cooking competence.
Results
For both older adults with SCD and their caregivers, the increases in the well-being index were significantly greater in the intervention group than in the control group (β = 0.508, 95% CI [0.036, 0.980]). For older adults with SCD, the increases in the cooking competence score were significantly greater in the intervention group than in the control group (β = 1.629, 95% CI [0.165, 3.071]).
Conclusion
The dyadic cooking-based intervention resulted in improvements in the cooking competence and well-being of older adults with SCD, as well as the well-being of caregivers.
Access this article
We’re sorry, something doesn't seem to be working properly.
Please try refreshing the page. If that doesn't work, please contact support so we can address the problem.
Similar content being viewed by others
References
Division of Population Health, National Center for Chronic Disease Prevention and Health Promotion. Healthy Brain Initiative. Centers for Disease Control and Prevention. Accessed 24 Feb, 2023. https://www.cdc.gov/aging/healthybrain/
Jessen F, Amariglio RE, van Boxtel M, Breteler M, Ceccaldi M, Chételat G. Subjective Cognitive Decline Initiative (SCD-I) Working Group. A conceptual framework for research on subjective cognitive decline in preclinical Alzheimer’s disease. Alzheimers Dement 2014;10(6):844–852. doi: https://doi.org/10.1016/j.jalz.2014.01.001.
Mitchell AJ, Beaumont H, Ferguson D, Yadegarfar M, Stubbs B. Risk of dementia and mild cognitive impairment in older people with subjective memory complaints: meta-analysis. Acta Psychiatr Scand 2014;130(6):439–451. doi: https://doi.org/10.1111/acps.12336.
Slot RER, Sikkes SAM, Berkhof J, et al. Subjective cognitive decline and rates of incident Alzheimer’s disease and non-Alzheimer’s disease dementia. Alzheimers Dement 2019;15(3):465–476. doi: https://doi.org/10.1016/j.jalz.2018.10.003.
Wilson RS, Boyle PA, Segawa E, et al. The influence of cognitive decline on well-being in old age. Psychol Aging 2013;28(2):304. doi: https://doi.org/10.1037/a0031196.
Hill NL, Mogle J, Wion R, et al. Subjective cognitive impairment and affective symptoms: a systematic review. Gerontologist 2016;56(6):e109–e127. doi: https://doi.org/10.1093/geront/gnw091.
Parikh PK, Troyer AK, Maione AM, Murphy KJ. The impact of memory change on daily life in normal aging and mild cognitive impairment. Gerontologist 2016;56(5):877–885. doi: https://doi.org/10.1093/geront/gnv030.
Cohen-Mansfield J, Cohen R, Buettner L, et al. Interventions for older persons reporting memory difficulties: a randomized controlled pilot study. Int J Geriatr Psychiatry 2015;30(5):478–486. doi: https://doi.org/10.1002/gps.4164.
Valentijn SAM, van Hooren SAH, Bosma H, et al. The effect of two types of memory training on subjective and objective memory performance in healthy individuals aged 55 years and older: a randomized controlled trial. Patient Educ Couns 2005;57(1):106–114. doi: https://doi.org/10.1016/j.pec.2004.05.002.
Pereira-Morales AJ, Cruz-Salinas AF, Aponte J, Pereira-Manrique F. Efficacy of a computer-based cognitive training program in older people with subjective memory complaints: a randomized study. Int J Neurosci 2018;128(1):1–9. doi: https://doi.org/10.1080/00207454.2017.1308930.
Helliwell JF, Putnam RD. The social context of well-being. Philos Trans R Soc B 2004;359(1449):1435–1446. doi: https://doi.org/10.1098/rstb.2004.1522.
Han B, Haley WE. Family caregiving for patients with stroke: review and analysis. Stroke 1999;30(7):1478–1485. doi: https://doi.org/10.1161/01.STR.30.7.1478.
Moon H, Adams KB. The effectiveness of dyadic interventions for people with dementia and their caregivers. Dementia 2013;12(6):821–839. doi: https://doi.org/10.1177/1471301212447026.
Paller KA, Creery JD, Florczak SM, et al. Benefits of mindfulness training for patients with progressive cognitive decline and their caregivers. Am J Alzheimer’s Dis Other Dement 2015;30(3):257–267. doi: https://doi.org/10.1177/1533317514545377.
Bourne P, Camic PM, Crutch SJ. Psychosocial outcomes of dyadic arts interventions for people with a dementia and their informal caregivers: a systematic review. Health Soc Care Community 2021;29(6):1632–1649. doi: https://doi.org/10.1111/hsc.13267.
Gitlin LN, Winter L, Corcoran M, Dennis MP, Schinfeld S, Hauck WW. Effects of the home environmental skill-building program on the caregiver-care recipient dyad: 6-month outcomes from the Philadelphia REACH initiative. Gerontologist 2003;43(4):532–546. doi: https://doi.org/10.1093/geront/43.4.532.
Gitlin LN, Winter L, Dennis MP, Hodgson N, Hauck WW. A biobehavioral home-based intervention and the well-being of patients with dementia and their caregivers: the COPE randomized trial. JAMA 2010;304(9):983–991. doi: https://doi.org/10.1001/jama.2010.1253.
Teri L, Gibbons LE, McCurry SM, et al. Exercise plus behavioral management in patients with Alzheimer disease: a randomized controlled trial. JAMA 2003;290(15):2015–2022. doi: https://doi.org/10.1001/jama.290.15.2015.
Farmer N, Touchton-Leonard K, Ross A. Psychosocial benefits of cooking interventions: a systematic review. Health Educ Behav 2018;45(2):167–180. doi: https://doi.org/10.1177/1090198117736352.
Firpo-Cappiello R. Why patients with dementia could benefit from cooking. American Academy of Neurology. Accessed 24 Feb, 2023. https://www.brainandlife.org/articles/after-a-diagnosis-of-alzheimers-disease-a-renowned-cookbook-author
Daniels S, Glorieux I, Minnen J, van Tienoven TP. More than preparing a meal? Concerning the meanings of home cooking. Appetite 2012;58(3):1050–1056. doi: https://doi.org/10.1016/j.appet.2012.02.040.
Wong A, Xiong YY, Kwan PWL, et al. The validity, reliability and clinical utility of the Hong Kong Montreal Cognitive Assessment (HK-MoCA) in patients with cerebral small vessel disease. Dement Geriatr Cogn Disord 2009;28(1):81–87. doi: https://doi.org/10.1159/000232589.
Keller HH, Gibbs A, Wong S, Vanderkooy P, Hedley M. Men can cook! Development, implementation, and evaluation of a senior men’s cooking group. J Nutr Elder 2004;24(1):71–87. doi: https://doi.org/10.1300/J052v24n01_06.
Alghamdi MM, Burrows T, Barclay B, Baines S, Chojenta C. Culinary Nutrition Education Programs in Community-Dwelling Older Adults: A Scoping Review. J Nutr Health Aging 2023;27(2):142–158. doi: https://doi.org/10.1007/s12603-022-1876-7.
Nijs KAND, De Graaf C, Siebelink E, et al. Effect of family-style meals on energy intake and risk of malnutrition in Dutch nursing home residents: a randomized controlled trial. J Gerontol A Biol Sci Med Sci 2006;61(9):935–942. doi: https://doi.org/10.1093/gerona/61.9.935.
Björnwall A, Mattsson Sydner Y, Koochek A, Neuman N. Eating alone or together among community-living older people—A scoping review. Int J Environ Res Public Health 2021;18(7):3495. doi: https://doi.org/10.3390/ijerph18073495.
Berg CA, Meegan SP, Deviney FP. A social-contextual model of coping with everyday problems across the lifespan. Int J Behav Dev 1998;22(2):239–261. doi: https://doi.org/10.1080/016502598384360.
Acknowledgements
We would like to express our gratitude to the Social Welfare Department (Partnership Fund for the Disadvantaged) for funding the study. We would also like to thank our project partners, including, in alphabetical order, Judy Chan and Lillian Lai from The Hong Kong and China Gas Company Limited (Towngas), and Ester Wong, Jojo Ng, Kit-Ying Law, Sammi Chun, Suki Chan, Tommy Wong, Twiggy Wong, and Wilson Lo from the Hong Kong Sheng Kung Hui Welfare Council Limited. Finally, we would like to thank the participants for their valuable support and participation.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest: None declared.
Ethical standards: Ethical approval was obtained from the Survey and Behavioural Research Ethics Committee of The Chinese University of Hong Kong. All participants provided their informed consent before participation.
Electronic supplementary material
Rights and permissions
About this article
Cite this article
Yu, R., Lai, D., Leung, G. et al. A Dyadic Cooking-Based Intervention for Improving Subjective Health and Well-Being of Older Adults with Subjective Cognitive Decline and Their Caregivers: A Randomized Controlled Trial. J Nutr Health Aging 27, 824–832 (2023). https://doi.org/10.1007/s12603-023-1990-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12603-023-1990-1