Abstract
Objectives
This study aimed to investigate the association between different forms of sedentary behavior and cognitive function in Chinese community-dwelling older adults.
Design
A longitudinal study with a 2-year follow-up.
Setting and Participants
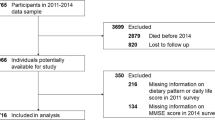
Data from 5356 participants at baseline and 956 participants at the follow-up of the Anhui Healthy Longevity Survey (AHLS) were analysed.
Measurements
Cognitive function was evaluated by the Mini-Mental State Examination (MMSE), and mild cognitive impairment (MCI) was classified according to education-specific criteria. Self-report questionnaires were used to assess the sedentary behavior of the participants.
Results
The participants who reported longer screen-watching sedentary duration had higher MMSE scores (1–2 hours: β=0.758, 95% CI: 0.450, 1.066; > 2 hours: β=1.240, 95% CI: 0.917, 1.562) and lower likelihoods of MCI (1–2 hours: OR= 0.787, 95% CI: 0.677, 0.914; >2 hours: OR=0.617, 95% CI: 0.524, 0.726). The participants who had played cards (or mahjong) sedentary had higher MMSE scores (β= 1.132, 95% CI: 0.788, 1.476) and lower likelihoods of MCI (OR=0.572, 95% CI: 0.476, 0.687). However, the participants who reported longer other forms of sedentary duration had lower MMSE scores (1–2 hours: β=−0.409, 95% CI: −0.735, −0.082; > 2 hours: β=−1.391, 95% CI: −1.696, −1.087) and higher likelihoods of MCI (1–2 hours: OR=1.271, 95% CI: 1.081, 1.496; > 2 hours: OR=1.632, 95% CI: 1.409, 1.889). No significant association was detected between sedentary duration and MCI incidence.
Conclusion
Variations in the impact of diverse sedentary behaviors on the cognitive function were detected in Chinese older adults. However, such associations were cross-sectional and longitudinal associations were not found in the current study.


Similar content being viewed by others
References
Mattson MP. Pathways towards and away from Alzheimer’s disease. Nature 2004; 430(7000): 631–9. doi: https://doi.org/10.1038/nature02621.
Breijyeh Z, Karaman R. Comprehensive Review on Alzheimer’s Disease: Causes and Treatment. Molecules 2020; 25(24). doi: https://doi.org/10.3390/molecules25245789.
Ton TGN, DeLeire T, May SG, Hou N, Tebeka MG, Chen E, Chodosh J. The financial burden and health care utilization patterns associated with amnestic mild cognitive impairment. Alzheimers Dement 2017; 13(3): 217–224. doi: https://doi.org/10.1016/j.jalz.2016.08.009.
Livingston G, Huntley J, Sommerlad A, Ames D, Ballard C, Banerjee S, Brayne C, Burns A, Cohen-Mansfield J, Cooper C, Costafreda SG, Dias A, Fox N, Gitlin LN, Howard R, Kales H C, Kivimäki M, Larson EB, Ogunniyi A, Orgeta V, Ritchie K, Rockwood K, Sampson EL, Samus Q, Schneider LS, Selbæk G, Teri L, Mukadam N. Dementia prevention, intervention, and care: 2020 report of the Lancet Commission. Lancet 2020; 396(10248): 413–446. doi: https://doi.org/10.1016/s0140-6736(20)30367-6.
Chan D, Shafto M, Kievit R, Matthews F, Spink M, Valenzuela M, Henson RN. Lifestyle activities in mid-life contribute to cognitive reserve in late-life, independent of education, occupation, and late-life activities. Neurobiol Aging 2018; 70: 180–183. doi: https://doi.org/10.1016/j.neurobiolaging.2018.06.012.
Fangfang H, Xiao H, Qiong W, Shuai Z, Jingya Z, Guodong S, Yan Z. Cross-Sectional Associations between Living and Built Environments and Depression Symptoms among Chinese Older Adults. Int J Environ Res Public Health 2022; 19(10). doi: https://doi.org/10.3390/ijerph19105819.
Szlejf C, Suemoto CK, Lotufo PA, Benseñor IM. Association of Sarcopenia With Performance on Multiple Cognitive Domains: Results From the ELSA-Brasil Study. J Gerontol A Biol Sci Med Sci 2019; 74(11): 1805–1811. doi: https://doi.org/10.1093/gerona/glz118.
Ravichandran S, Sukumar S, Chandrasekaran B, Kadavigere R, Palaniswamy HP, Uppoor R, Ravichandran K, Almeshari M, Alzamil Y, Abanomy A. Influence of Sedentary Behaviour Interventions on Vascular Functions and Cognitive Functions in Hypertensive Adults-A Scoping Review on Potential Mechanisms and Recommendations. Int J Environ Res Public Health 2022; 19(22). doi: https://doi.org/10.3390/ijerph192215120.
Panahi S, Tremblay A. Sedentariness and Health: Is Sedentary Behavior More Than Just Physical Inactivity? Front Public Health 2018; 6: 258. doi: https://doi.org/10.3389/fpubh.2018.00258.
Ekelund U, Steene-Johannessen J, Brown WJ, Fagerland MW, Owen N, Powell KE, Bauman A, Lee IM. Does physical activity attenuate, or even eliminate, the detrimental association of sitting time with mortality? A harmonised meta-analysis of data from more than 1 million men and women. Lancet 2016; 388(10051): 1302–10. doi: https://doi.org/10.1016/s0140-6736(16)30370-1.
Ross R, Chaput JP, Giangregorio LM, Janssen I, Saunders TJ, Kho ME, Poitras VJ, Tomasone JR, El-Kotob R, McLaughlin EC, Duggan M, Carrier J, Carson V, Chastin SF, Latimer-Cheung AE, Chulak-Bozzer T, Faulkner G, Flood SM, Gazendam MK, Healy GN, Katzmarzyk PT, Kennedy W, Lane KN, Lorbergs A, Maclaren K, Marr S, Powell KE, Rhodes RE, Ross-White A, Welsh F, Willumsen J, Tremblay MS. Canadian 24-Hour Movement Guidelines for Adults aged 18–64 years and Adults aged 65 years or older: an integration of physical activity, sedentary behaviour, and sleep. Appl Physiol Nutr Metab 2020; 45(10 (Suppl. 2)): S57–S102. doi: https://doi.org/10.1139/apnm-2020-0467.
de Rezende LF, Rey-López JP, Matsudo VK, do Carmo Luiz O. Sedentary behavior and health outcomes among older adults: a systematic review. BMC Public Health 2014; 14: 333. doi: https://doi.org/10.1186/1471-2458-14-333.
Lautenschlager NT, Cox KL, Flicker L, Foster JK, van Bockxmeer FM, Xiao J, Greenop KR, Almeida OP. Effect of physical activity on cognitive function in older adults at risk for Alzheimer disease: a randomized trial. Jama 2008; 300(9): 1027–37. doi: https://doi.org/10.1001/jama.300.9.1027.
Olanrewaju O, Stockwell S, Stubbs B, Smith L. Sedentary behaviours, cognitive function, and possible mechanisms in older adults: a systematic review. Aging Clin Exp Res 2020; 32(6): 969–984. doi: https://doi.org/10.1007/s40520-019-01457-3.
Takeuchi H, Kawashima R. A Prospective Study on the Relationship Between Driving and Non-occupational Computer Use With Risk of Dementia. Front Aging Neurosci 2022; 14: 854177. doi: https://doi.org/10.3389/fnagi.2022.854177.
Bakrania K, Edwardson CL, Khunti K, Bandelow S, Davies MJ, Yates T. Associations Between Sedentary Behaviors and Cognitive Function: Cross-Sectional and Prospective Findings From the UK Biobank. Am J Epidemiol 2018; 187(3): 441–454. doi: https://doi.org/10.1093/aje/kwx273.
Almeida-Meza P, Steptoe A, Cadar D. Is Engagement in Intellectual and Social Leisure Activities Protective Against Dementia Risk? Evidence from the English Longitudinal Study of Ageing. J Alzheimers Dis 2021; 80(2): 555–565. doi: https://doi.org/10.3233/jad-200952.
Lu Z, Harris TB, Shiroma EJ, Leung J, Kwok T. Patterns of Physical Activity and Sedentary Behavior for Older Adults with Alzheimer’s Disease, Mild Cognitive Impairment, and Cognitively Normal in Hong Kong. J Alzheimers Dis 2018; 66(4): 1453–1462. doi: https://doi.org/10.3233/jad-180805.
Carter SE, Draijer R, Holder SM, Brown L, Thijssen D, Hopkins ND. Regular walking breaks prevent the decline in cerebral blood flow associated with prolonged sitting. J Appl Physiol (1985) 2018; 125(3): 790–798. doi: https://doi.org/10.1152/japplphysiol.00310.2018.
Fangfang H, Xiao H, Shuai Z, Qiong W, Jingya Z, Guodong S, Yan Z. Living Environment, Built Environment and Cognitive Function among Older Chinese Adults: Results from a Cross-Sectional Study. J Prev Alzheimers Dis 2022; 9(1): 126–135. doi: https://doi.org/10.14283/jpad.2021.59.
Huo Z, Lin J, Bat B, Chan J, Tsoi K, Yip B. Diagnostic accuracy of dementia screening tools in the Chinese population: a systematic review and meta-analysis of 167 diagnostic studies. Age Ageing 2021; 50(4): 1093–1101. doi: https://doi.org/10.1093/ageing/afab005.
Mitchell AJ. A meta-analysis of the accuracy of the mini-mental state examination in the detection of dementia and mild cognitive impairment. J Psychiatr Res 2009; 43(4): 411–31. doi: https://doi.org/10.1016/j.jpsychires.2008.04.014.
Katzman R, Zhang MY, Ouang Q, Wang ZY, Liu WT, Yu E, Wong SC, Salmon DP, Grant I. A Chinese version of the Mini-Mental State Examination; impact of illiteracy in a Shanghai dementia survey. J Clin Epidemiol 1988; 41(10): 971–8. doi: https://doi.org/10.1016/0895-4356(88)90034-0.
Teh JKL, Tey NP. Effects of selected leisure activities on preventing loneliness among older Chinese. SSM Popul Health 2019; 9: 100479. doi: https://doi.org/10.1016/j.ssmph.2019.100479.
Yun W, Xiaofang J, Feifei H, Xiaofan Z, Bing Z, Zhihong W, Huijun W. Analysis of the association between television sedentary time and cognitive function among middle-aged and elderly people in four Chinese provinces. Chinese Journal of Health Education 2020; 36(12): 1067–1072. doi: https://doi.org/10.16168/j.cnki.issn.1002-9982.2020.12.001.
Accuracy of Patient Health Questionnaire-9 (PHQ-9) for screening to detect major depression: individual participant data meta-analysis. Bmj 2019; 365: 11781. doi: https://doi.org/10.1136/bmj.l1781.
Tun PA, Lachman ME. The association between computer use and cognition across adulthood: use it so you won’t lose it? Psychol Aging 2010; 25(3): 560–568. doi: https://doi.org/10.1037/a0019543.
Jia J, Zhao T, Liu Z, Liang Y, Li F, Li Y, Liu W, Li F, Shi S, Zhou C, Yang H, Liao Z, Li Y, Zhao H, Zhang J, Zhang K, Kan M, Yang S, Li H, Liu Z, Ma R, Lv J, Wang Y, Yan X, Liang F, Yuan X, Zhang J, Gauthier S, Cummings J. Association between healthy lifestyle and memory decline in older adults: 10 year, population based, prospective cohort study. Bmj 2023; 380: e072691. doi: https://doi.org/10.1136/bmj-2022-072691.
Almeida OP, Yeap BB, Alfonso H, Hankey GJ, Flicker L, Norman PE. Older men who use computers have lower risk of dementia. PLoS One 2012; 7(8): e44239. doi: https://doi.org/10.1371/journal.pone.0044239.
Boot WR, Moxley JH, Roque NA, Andringa R, Charness N, Czaja SJ, Sharit J, Mitzner T, Lee CC, Rogers WA. Exploring Older Adults’ Video Game Use in the PRISM Computer System. Innov Aging 2018; 2(1): igy009. doi: https://doi.org/10.1093/geroni/igy009.
Kamin ST, Lang FR. Internet Use and Cognitive Functioning in Late Adulthood: Longitudinal Findings from the Survey of Health, Ageing and Retirement in Europe (SHARE). J Gerontol B Psychol Sci Soc Sci 2020; 75(3): 534–539. doi: https://doi.org/10.1093/geronb/gby123.
Zhao X, Yu J, Liu N. Relationship between specific leisure activities and successful aging among older adults. J Exerc Sci Fit 2023; 21(1): 111–118. doi: https://doi.org/10.1016/j.jesf.2022.11.006.
Sun S, Zhang S, Fan X. Media Use, Cognitive Performance, and Life Satisfaction of the Chinese Elderly. Health Commun 2016; 31(10): 1223–34. doi: https://doi.org/10.1080/10410236.2015.1049730.
Small GW, Moody TD, Siddarth P, Bookheimer SY. Your brain on Google: patterns of cerebral activation during internet searching. Am J Geriatr Psychiatry 2009; 17(2): 116–26. doi: https://doi.org/10.1097/JGP.0b013e3181953a02.
Verghese J, Lipton RB, Katz MJ, Hall CB, Derby CA, Kuslansky G, Ambrose AF, Sliwinski M, Buschke H. Leisure activities and the risk of dementia in the elderly. N Engl J Med 2003; 348(25): 2508–16. doi: https://doi.org/10.1056/NEJMoa022252.
Estrada-Plana V, Montanera R, Ibarz-Estruga A, March-Llanes J, Vita-Barrull N, Guzmán N, Ros-Morente A, Ayesa Arriola R, and Moya-Higueras J. Cognitive training with modern board and card games in healthy older adults: two randomized controlled trials. Int J Geriatr Psychiatry 2021; 36(6): 839–850. doi: https://doi.org/10.1002/gps.5484.
Decety J, Jackson PL, Sommerville JA, Chaminade T, Meltzoff AN. The neural bases of cooperation and competition: an fMRI investigation. Neuroimage 2004; 23(2): 744–51. doi: https://doi.org/10.1016/j.neuroimage.2004.05.025.
Coelho L, Hauck K, McKenzie K, Copeland JL, Kan IP, Gibb RL, Gonzalez CLR. The association between sedentary behavior and cognitive ability in older adults. Aging Clin Exp Res 2020; 32(11): 2339–2347. doi: https://doi.org/10.1007/s40520-019-01460-8.
Williamson J, Yabluchanskiy A, Mukli P, Wu DH, Sonntag W, Ciro C, Yang Y. Sex differences in brain functional connectivity of hippocampus in mild cognitive impairment. Front Aging Neurosci 2022; 14: 959394. doi: https://doi.org/10.3389/fnagi.2022.959394.
Sohn D, Shpanskaya K, Lucas JE, Petrella JR, Saykin AJ, Tanzi RE, Samatova NF, Doraiswamy PM. Sex Differences in Cognitive Decline in Subjects with High Likelihood of Mild Cognitive Impairment due to Alzheimer’s disease. Sci Rep 2018; 8(1): 7490. doi: https://doi.org/10.1038/s41598-018-25377-w.
Patterson F, Lozano A, Huang L, Perkett M, Beeson J, Hanlon A. Towards a demographic risk profile for sedentary behaviours in middle-aged British adults: a cross-sectional population study. BMJ Open 2018; 8(7): e019639. doi: https://doi.org/10.1136/bmjopen-2017-019639.
Jia J, Wang F, Wei C, Zhou A, Jia X, Li F, Tang M, Chu L, Zhou Y, Zhou C, Cui Y, Wang Q, Wang W, Yin P, Hu N, Zuo X, Song H, Qin W, Wu L, Li D, Jia L, Song J, Han Y, Xing Y, Yang P, Li Y, Qiao Y, Tang Y, Lv J, Dong X. The prevalence of dementia in urban and rural areas of China. Alzheimers Dement 2014; 10(1): 1–9. doi: https://doi.org/10.1016/j.jalz.2013.01.012.
Zhang X, Lu J, Wu C, Cui J, Wu Y, Hu A, Li J, Li X. Healthy lifestyle behaviours and all-cause and cardiovascular mortality among 0.9 million Chinese adults. Int J Behav Nutr Phys Act 2021; 18(1): 162. doi: https://doi.org/10.1186/s12966-021-01234-4.
Li H, Zeng Y, Gan L, Tuersun Y, Yang J, Liu J, Chen J. Urban-rural disparities in the healthy ageing trajectory in China: a population-based study. BMC Public Health 2022; 22(1): 1406. doi: https://doi.org/10.1186/s12889-022-13757-x.
Lövdén M, Fratiglioni L, Glymour MM, Lindenberger U, Tucker-Drob EM. Education and Cognitive Functioning Across the Life Span. Psychol Sci Public Interest 2020; 21(1): 6–41. doi: https://doi.org/10.1177/1529100620920576.
Zhu X, Qiu C, Zeng Y, Li J. Leisure activities, education, and cognitive impairment in Chinese older adults: a population-based longitudinal study. Int Psychogeriatr 2017; 29(5): 727–739. doi: https://doi.org/10.1017/s1041610216001769.
Edwards MK, Loprinzi PD. The Association Between Sedentary Behavior and Cognitive Function Among Older Adults May Be Attenuated With Adequate Physical Activity. J Phys Act Health 2017; 14(1): 52–58. doi: https://doi.org/10.1123/jpah.2016-0313.
Troiano RP, Berrigan D, Dodd KW, Mâsse LC, Tilert T, McDowell M. Physical activity in the United States measured by accelerometer. Med Sci Sports Exerc 2008; 40(1): 181–8. doi: https://doi.org/10.1249/mss.0b013e31815a51b3.
Prince SA, Adamo KB, Hamel ME, Hardt J, Connor Gorber S, Tremblay M. A comparison of direct versus self-report measures for assessing physical activity in adults: a systematic review. Int J Behav Nutr Phys Act 2008; 5: 56. doi: https://doi.org/10.1186/1479-5868-5-56.
Falck RS, Davis JC, Liu-Ambrose T. What is the association between sedentary behaviour and cognitive function? A systematic review. Br J Sports Med 2017; 51(10): 800–811. doi: https://doi.org/10.1136/bjsports-2015-095551.
Chandrasekaran B, Pesola AJ, Rao CR, Arumugam A. Does breaking up prolonged sitting improve cognitive functions in sedentary adults? A mapping review and hypothesis formulation on the potential physiological mechanisms. BMC Musculoskelet Disord 2021; 22(1): 274. doi: https://doi.org/10.1186/s12891-021-04136-5.
Johnson PR. The effects of medication on cognition in long-term care. Semin Speech Lang 2013; 34(1): 18–27. doi: https://doi.org/10.1055/s-0033-1337391.
Vaz Fragoso CA, McAvay GJ. Antihypertensive medications and physical function in older persons. Exp Gerontol 2020; 138: 111009. doi: https://doi.org/10.1016/j.exger.2020.111009.
Acknowledgements
The authors thank all participants in the AHLS for their cooperation and data sharing. We also thank all the colleagues for their time and efforts on data collection and project management.
Funding
Funding: This research was funded by the National Natural Science Foundation of China, Grant Number 72004003 to YZ, the Key Project of Science and Technology of Anhui Province, Grant Number 202004b11020019 to GS, and the Hefei Municipal Natural Science Foundation, Grant Number 2021005 to GS.
Author information
Authors and Affiliations
Contributions
Author Contributions: SZ drafted the manuscript. GS and YZ framed the concept and designed the study. Data collection and material preparation were conducted by SZ, JZ, QinW, and QioW, and data analysis was performed by WZ and CD. All authors meet the criteria for authorship according to their contributions to the manuscript. All authors contributed to the article and approved the submitted version.
Corresponding authors
Ethics declarations
Ethics approval and consent to participate: The study protocol was approved by the Ethics Review Committee of Anhui Medical University, Hefei, China (No. 2020H011). Informed consent was obtained from all participants included in the study.
Conflict of Interest: None declared. The research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Electronic supplementary material
Rights and permissions
About this article
Cite this article
Shuai, Z., Jingya, Z., Qing, W. et al. Associations between Sedentary Duration and Cognitive Function in Older Adults: A Longitudinal Study with 2-Year Follow-Up. J Nutr Health Aging 27, 656–662 (2023). https://doi.org/10.1007/s12603-023-1963-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12603-023-1963-4