Abstract
Objective
This study aims to appraise and summarize consistent recommendations from clinical practice guidelines (CPGs) for identification and management of frailty to maintain and improve functional independence of elderly population.
Methods
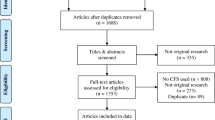
A systematic search of Ovid MEDLINE, Embase, PubMed, PsycINFO, and CINAHL electronic databases using database-specific search terms in two broad areas “guidelines” and “frailty”, and a manual search of websites with the key phrase “frailty guideline” was performed. The inclusion criteria included CPGs focusing on identifying and managing frailty in population >65 years old, published in English since January 2010. Three reviewers independently assessed guideline quality using the AGREE II instrument. Data extraction was performed, followed by compilation and comparison of all recommendations to identify the key consistent recommendations.
Results
Six CPGs met the inclusion criteria; however, only three CPGs had high methodological quality in accordance with AGREE II appraisal. The average AGREE II scores of all six CPGs were: 84.5%, 68%, 46.5%, 81.5%, 56.3%, and 60.2% for domains 1–6 (scope and purpose, stakeholder involvement, rigour of development, clarity of presentation, applicability, and editorial independence) respectively. A total of 54 recommendations were identified, with 12 key recommendations suggested frequently by the CPGs.
Conclusion
The AGREE II instrument identified strengths and weaknesses of the CPGs, but failed to assess clinical implications and feasibility of the guidelines. Further research is needed to improve clinical relevance of CPGs in the identification and management of frailty. The feasibility in implementing these guidelines with regards to cost-effectiveness of frailty screening warrants further investigation.


Similar content being viewed by others
References
Dent E, Morley JE, Cruz-Jentoft AJ, Woodhouse L, Rodriguez-Manas L, Fried LP, et al. Physical frailty: ICFSR international clinical practice guidelines for identification and management. J Nutr Health Aging. 2019;23(9):771–787.
Dent E, Lien C, Lim WS, Wong WC, Wong CH, Ng TP, et al. The Asia-Pacific clinical practice guidelines for the management of frailty. J Am Med Dir Assoc. 2017; 18(7):564–575.
Ministry of Health. BCGuidelines.ca: Frailty in older adults- early identification and management [Internet]. Victoria BC: Ministry of Health; 2017 [cited 2020 Apr 30]. Available from: https://www2.gov.be.ca/assets/gov/health/practitioner-pro/bc-guidelines/frailty-full_guideline.pdf
British Geriatrics Society. Fit for frailty: consensus best practice guidance for the care of older people living in community and outpatient settings [Internet]. London: British Geriatrics Society; 2014 [cited 2020 Apr 30]. Available from: https://www.bgs.org.uk/sites/default/files/content/resources/files/2018-05-23/fff_full.pdf
Fried LP, Tangen CM, Walston J, Newman AB, Hirsch C, Gottdiener J, et al. Frailty in older adults: evidence for a phenotype. Journal of Gerontology, Medical Sciences. 2001;56(3):M146–M156.
O’Caoimh R, Galluzzo L, Rodriguez-Laso A, Van der Heyden J, Ranhoff AH, Lamprini-Koula M, et al. Prevalence of frailty at population level in European ADVANTAGE Joint Action Member States: a systematic review and meta-analysis. Ann 1st Super Sanita. 2018;54(3):226–238.
Collard RM, Boter H, Schoevers RA, Oude Voshaar RC. Prevalence of frailty in community-dwelling older persons: a systematic review. J Am Geriatr Soc. 2012;60(8): 1487–1492.
Biritwum R, Minicuci N, Yawson A, Theou O, Mensah G, Naidoo N, et al. Prevalence of and factors associated with frailty and disability in older adults from China, Ghana, India, Mexico, Russia and South Africa. Maturitas. 2016;91:8–18.
Hyde Z, Flicker L, Smith K, Atkinson D, Fenner S, Skeaf L, et al. Prevalence and incidence of frailty in Aboriginal Australians, and associations with mortality and disability. Maturitas. 2016;87:89–94.
Hoogendijk EO, Rockwood K, Theou O, Armstrong JJ, Onwuteaka-Philipsen BD, Deeg DJH, et al. Tracking changes in frailty throughout later life: results from a 17-year longitudinal study in the Netherlands. Age and Ageing. 2018;47(5):727–733.
Clegg A, Young J, Hiffe S, Rikkert MO, Rockwood K. Frailty in elderly people. The Lancet. 2013;381(9868):752–762.
Sieliwonczyk E, Perkisas S, Vandewoude M. Frailty indexes, screening instruments and their application in Belgian primary care. Acta Clin Belg. 2014;69(4):233–239.
Morley JE, Vellas B, van Kan GA, Anker S, Bauer J, Bernabei R, et al. Frailty consensus: a call to action. J Am Med Dir Assoc. 2013; 14(6):392–397.
Dent E, Kowal P, Hoogendijk EO. Frailty measurement in research and clinical practice: areview. Eur J Intern Med. 2016;31:3–10.
Lu Y, Tan CT, Nyunt MS, Mok E, Camous X, Kared H, et al. Inflammatory and immune markers associated with physical frailty syndrome: findings from Singapore longitudinal aging studies. Oncotarget. 2016;7(20):28783–28795.
Woolf S, Schünemann H, Eccles M, Grimshaw J, Shekelle P. Developing clinical practice guidelines: types of evidence and outcomes; values and economics, synthesis, grading, and presentation and deriving recommendations. Implementation Science. 2012;7(1):1–12.
Field M, Lohr K. Clinical practice guidelines: directions for a new program. Institute of Medicine. Washington, DC: National Academy Press; 1990.
Murad MH. Clinical practice guidelines: a primer on development and dissemination. Mayo Clinic Proceedings. 2017 Mar l;92(3):423–433.
AGREE Next Steps Consortium. AGREE H instrument [Internet]. 2010 [cited 2020 Apr 30]. Available from: https://www.agreetrust.org/wp-content/uploads/2017/12/AGREE-II-Users-Manual-and-23-item-Instrument-2009-Update-2017.pdf
Brouwers M, Kho M, Browman G, Burgers J, Cluzeau F, Feder G, et al. Development of the AGREE II, part 1: performance, usefulness and areas for improvement. Can Med Assoc J. 2010; 182(10): 1045–52.
Brouwers M, Kho M, Browman G, Burgers J, Cluzeau F, Feder G, et al. Development of the AGREE II, part 2: assessment of validity of items and tools to support application. CMAJ. 2010;182(10):E472–8.
Simon A, Pratt M, Hutton B, Skidmore B, Fakhraei R, Rybak N, et al. Guidelines for the management of pregnant women with obesity: a systematic review. Obesity Reviews. 2020;21(3):e12972.
Zhang P, Lu Q, Li H, Wang W, Li G, Si L, et al. The quality of guidelines for diabetic foot ulcers: a critical appraisal using the AGREE II instrument. PLoS ONE. 2019;14(9):e0217555.
Choi T, Choi J, Lee J, Jun J, Park B, Lee M. The quality of clinical practice guidelines in traditional medicine in Korea: appraisal using the AGREE II instrument. Implementation Science. 2015;10(1):1–10.
Yao L, Chen Y, Wang X, Shi X, Wang Y, Guo T, et al. Appraising the quality of clinical practice guidelines in traditional Chinese medicine using AGREE II instrument: a systematic review. Int J Clin Pract. 2017;71(5):e12931.
Lin I, Wiles L, Waller R, Goucke R, Nagree Y, Gibberd M, et al. What does best practice care for musculoskeletal pain look like? Eleven consistent recommendations from high-quality clinical practice guidelines: systematic review. British Journal of Sports Medicine. 2020;54(2):79–86.
Health Quality and Safety Commission NZ. Frailty care guides [Internet]. Wellington: Health Quality and Safety Commission NZ; 2019 [cited 2020 May 1]. Available from: https://www.hqsc.govt.nz/assets/ARC/PR/Frailty_care_guides/Frailty-care-guide-master.pdf
Bavazzano A, Badiani E, Bandinelli S, Benvenuti F, Berni G, Biagini CA, et al. SNLG-Regions: frailty in elderly people [Internet]. Italy: Regione Toscana; 2013 [cited 2020 May 4]. Available from: https://www.regione.toscana.it/documents/10180/320308/Frailty+in+elderly+people/327bb85-6d3c-4elb-a398-669e76ce5b01?version=1.0
Bock J, König H, Brenner H, Haefeli W, Quinzler R, Matschinger H, et al. Associations of frailty with health care costs- results of the ESTHER cohort study. BMC Health Serv Res. 2016; 16(1): 128.
Cornwall J, Davey JA. Impact of population ageing in New Zealand on the demand for health and disability support services, and workforce implications [Internet]. Wellington, New Zealand: Ministry of Health; 2004 [cited 2020 Aug 30]. Available from: https://www.health.govt.nz/system/files/documents/publications/cornwallanddavey.pdf
Lehnert T, Heider D, Leicht H, Heinrich S, Corrieri S, Luppa M, et al. Health care utilization and costs of elderly persons with multiple chronic conditions. Medical Care Research and Review. 2011;68(4):387–420.
Ritchie H, Roser M. Age structure. Our World in Data [Internet]. 2019 Sep [cited 2020 May 11]. Available from: https://ourworldindata.org/age-structure
Commonwealth of Australia. Geriatric medicine 2016 factsheet [Internet]. Australia: Australia Government Department of Health; 2017 Oct [cited 2020 May 11]. Available from: https://hwd.health.gov.au/webapi/customer/documents/factsheets/2016/Geriatric%20medicine.pdf
Commonwealth of Australia. Paediatrics & child health 2016 factsheet [Internet]. Australia: Australia Government Department of Health; 2017 Oct [cited 2020 May 11]. Available from: https://hwd.health.gov.au/webapi/customer/documents/factsheets/2016/Paediatrics%20&%20child%20health%20data.pdf
World Health Organisation. Ageing and health [Internet]. Geneva: WHO; 2018 [cited 2020 May 11]. Available from: https://www.who.int/news-room/fact-sheets/detail/ageing-and-health
World Health Organisation. 10 facts on aging and the life course [Internet]. Geneva: WHO; 2011 [cited 2020 May 11]. Available from: https://www.who.int/features/factfiles/ageing/ageing_facts/en/
Bleijenberg N, Drubbel I, Neslo RE, Schuurmans MJ, Ten Dam VH, Numans ME, et al. Cost-effectiveness of a proactive primary care program for frail older people: a cluster-randomized controlled trial. J Am Med Dir Assoc. 2017; 18(12): 1029–36.e3
Blom JW, Van den Hout WB, Den Elzen WBJ, Drewes YM, Bleijenberg N, Fabbricotti IN, et al. Effectiveness and cost-effectiveness of proactive and multidisciplinary integrated care for older people with complex problems in general practice: an individual participant data meta-analysis. Age and Ageing. 2018;47(5):705–714.
Woo J, Yu R, Wong M, Yeung F, Wong M, Lum C. Frailty screening in the community using the FRAIL scale. J Am Med Dir Assoc. 2015; 16(5):412–419.
Acknowledgements
The authors would like to thank subject librarian Ms. Thelma Fisher (University of Otago) for her expertise and guidance in performing electronic database searches for the systematic review.
Funding
Funding: None.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethics: Not applicable.
Conflicts of interest: None declared.
Electronic Supplementary Material
Rights and permissions
About this article
Cite this article
Mehta, P., Lemon, G., Hight, L. et al. A Systematic Review of Clinical Practice Guidelines for Identification and Management of Frailty. J Nutr Health Aging 25, 382–391 (2021). https://doi.org/10.1007/s12603-020-1549-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12603-020-1549-3