Abstract
Background and Purpose
As a very common risk of adverse outcomes of the ischemic stroke patients, sarcopenia is associated with infectious complications and higher mortality. The goal of this retrospective study is to explore the predictive value of serum Cr/CysC ratio in acute ischemic stroke patients receiving nutritional intervention.
Methods
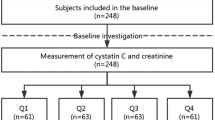
We reviewed adult patients with AIS from December 2019 to February 2020. Patients with acute kidney injury were excluded and all patients received nutritional intervention during a 3-month follow-up period. We collected baseline data at admission including creatinine and cystatin C. The primary poor outcome was major disability (modified Rankin Scale score ≥ 4) at 3 months after AIS.
Results
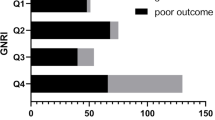
A total of 217 patients with AIS were identified for this study. Serum Cr/CysC ratio was significantly correlated with NIHSS at discharge, 1-month modified Rankin Scale score, and 3-month modified Rankin Scale score. During 3 months, 34 (15.70%) patients had a poor outcome after AIS and 11 (5.10%) patients died within 30 days. In multivariable logistic regression analyses, serum Cr/CysC ratio at admission was independently associated with 3-month poor outcomes (OR: 0.953, 95% CI: 0.921–0.986, p =.006) and 30-day mortality (OR: 0.953, 95% CI: 0.921–0.986, p =.006).
Conclusion
As a blood biochemical indexes reflecting the muscle mass and aiding in risk stratification, Cr/CysC ratio at admission could be used as a predictor of 30-day mortality and long-term poor prognosis in AIS patients.

Similar content being viewed by others
Availability of data and materials: Original data of the present study are available from the corresponding author upon reasonable request.
References
Announcement: World Stroke Day — October 29, 2016. MMWR Morb Mortal Wkly Rep. 2016;65(42):1176.
Zhang Y, Sun L. Cystatin C in Cerebrovascular Disorders. Curr Neurovasc Res. 2017;14(4):406–14.
Hatem SM, Saussez G, Delia Faille M, Prist V, Zhang X, Dispa D, et al. Rehabilitation of Motor Function after Stroke: A Multiple Systematic Review Focused on Techniques to Stimulate Upper Extremity Recovery. Front Hum Neurosci. 2016;10:442.
Dhand A, Lang CE, Luke DA, Kim A, Li K, McCafferty L, et al. Social Network Mapping and Functional Recovery Within 6 Months of Ischemic Stroke. Neurorehabil Neural Repair. 2019;33(11):922–32.
Nozoe M, Kanai M, Kubo H, Yamamoto M, Shimada S, Mase K. Prestroke sarcopenia and functional outcomes in elderly patients who have had an acute stroke: A prospective cohort study. Nutrition. 2019;66:44–7.
Peterson SJ, Braunschweig CA. Prevalence of Sarcopenia and Associated Outcomes in the Clinical Setting. Nutr Clin Pract. 2016;31(1):40–8.
Papadatou MC. Sarcopenia in Hemiplegia. J Frailty Sarcopenia Falls. 2020;5(2):38–41.
Heymsfield SB, Gonzalez MC, Lu J, Jia G, Zheng J. Skeletal muscle mass and quality: evolution of modern measurement concepts in the context of sarcopenia. Proc Nutr Soc. 2015;74(4):355–66.
Bagshaw SM, Bellomo R. Cystatin C in acute kidney injury. Curr Opin Crit Care. 2010;16(6):533–9.
Kashani KB, Frazee EN, Kukralova L, Sarvottam K, Herasevich V, Young PM, et al. Evaluating Muscle Mass by Using Markers of Kidney Function: Development of the Sarcopenia Index. Crit Care Med. 2017;45(1):e23–e9.
Osaka T, Hamaguchi M, Hashimoto Y, Ushigome E, Tanaka M, Yamazaki M, et al. Decreased the creatinine to cystatin C ratio is a surrogate marker of sarcopenia in patients with type 2 diabetes. Diabetes Res Clin Pract. 2018;139:52–8.
Rabito EI, Marcadenti A, da Silva Fink J, Figueira L, Silva FM. Nutritional Risk Screening 2002, Short Nutritional Assessment Questionnaire, Malnutrition Screening Tool, and Malnutrition Universal Screening Tool Are Good Predictors of Nutrition Risk in an Emergency Service. Nutr Clin Pract. 2017;32(4):S26–32.
Chen PC, Chuang CH, Leong CP, Guo SE, Hsin YJ. Systematic review and metaanalysis of the diagnostic accuracy of the water swallow test for screening aspiration in stroke patients. J Adv Nurs. 2016;72(11):2575–86.
Wendelboe AM, Raskob GE. Global Burden of Thrombosis: Epidemiologic Aspects. CircRes. 2016;118(9):1340–7.
Matsushita T, Nishioka S, Taguchi S, Yamanouchi A. Sarcopenia as a predictor of activities of daily living capability in stroke patients undergoing rehabilitation. Geriatr Gerontol Int. 2019;19(11):1124–8.
Nozoe M, Kanai M, Kubo H, Yamamoto M, Shimada S, Mase K. Prestroke Sarcopenia and Stroke Severity in Elderly Patients with Acute Stroke. J Stroke Cerebrovasc Dis. 2019;28(8):2228–31.
Scherbakov N, Sandek A, Doehner W. Stroke-related sarcopenia: specific characteristics. J Am Med Dir Assoc. 2015;16(4):272–6.
Robinson SM, Reginster JY, Rizzoli R, Shaw SC, Kanis JA, Bautmans I, et al. Does nutrition play a role in the prevention and management of sarcopenia. Clin Nutr. 2018;37(4):1121–32.
Wang S, Xie L, Xu J, Hu Y, Wu Y, Lin Z, et al. Predictive value of serum creatinine/cystatin C in neurocritically ill patients. Brain Behav. 2019;9(12):e01462.
Maeda K, Akagi J. Decreased tongue pressure is associated with sarcopenia and sarcopenic dysphagia in the elderly. Dysphagia. 2015;30(1):80–7.
Shiraishi A, Yoshimura Y, Wakabayashi H, Tsuji Y. Prevalence of stroke-related sarcopenia and its association with poor oral status in post-acute stroke patients: Implications for oral sarcopenia. Clin Nutr. 2018;37(1):204–7.
Chang KV, Hsu TH, Wu WT, Huang KC, Han DS. Association Between Sarcopenia and Cognitive Impairment: A Systematic Review and Meta-Analysis. J Am Med Dir Assoc. 2016;17(12):1164e7–e15.
Maeda K, Akagi J. Sarcopenia is an independent risk factor of dysphagia in hospitalized older people. Geriatr Gerontol Int. 2016;16(4):515–21.
Yoshimura Y, Wakabayashi H, Bise T, Nagano F, Shimazu S, Shiraishi A, et al. Sarcopenia is associated with worse recovery of physical function and dysphagia and a lower rate of home discharge in Japanese hospitalized adults undergoing convalescent rehabilitation. Nutrition. 2019;61:111–8.
Millward DJ. Nutrition and sarcopenia: evidence for an interaction. Proc Nutr Soc. 2012;71(4):566–75.
Arnold M, Liesirova K, Broeg-Morvay A, Meisterernst J, Schlager M, Mono ML, et al. Dysphagia in Acute Stroke: Incidence, Burden and Impact on Clinical Outcome. PLoS One. 2016;11(2):e0148424.
Manabe T, Teramoto S, Tamiya N, Okochi J, Hizawa N. Risk Factors for Aspiration Pneumonia in Older Adults. PLoS One. 2015;10(10):e0140060.
Xu Z, Gu Y, Li J, Wang C, Wang R, Huang Y, et al. Dysphagia and aspiration pneumonia in elderly hospitalization stroke patients: Risk factors, cerebral infarction area comparison. J Back Musculoskelet Rehabil. 2019;32(1):85–91.
Tamura T, Sakurai K, Nambara M, Miki Y, Toyokawa T, Kubo N, et al. Adverse Effects of Preoperative Sarcopenia on Postoperative Complications of Patients With Gastric Cancer. Anticancer Res. 2019;39(2):987–92.
Kou HW, Yeh CH, Tsai HI, Hsu CC, Hsieh YC, Chen WT, et al. Sarcopenia is an effective predictor of difficult-to-wean and mortality among critically ill surgical patients. PLoS One. 2019;14(8):e0220699.
Acknowledgments
We would like to thank Prof. Wanli Dong for valuable comments on this manuscript.
Funding
Funding: This work was supported by the grants from National Key R&D Program of China (2017YFC0110304).
Author information
Authors and Affiliations
Contributions
Authors’ contributions: WL, YY, and JN designed the study. WL, XZ, XT, YW, SD, SH, XZ and YY evaluated the subjects and collected the data. LY and YY analyzed the data. WL wrote the initial draft, with YY and JN participating in revising the manuscript.
Corresponding authors
Ethics declarations
Consent for publication: Not applicable.
Competing interests: On behalf of all authors, the corresponding author states that there is no conflict of interest.
Ethics approval and consent to participate: This study involving human participants were reviewed and approved by the Institutional Review Board of The First Affiliated Hospital of Soochow University. The experiment comply with the current laws of the country in which they were performed. All patients gave informed consent.
Rights and permissions
About this article
Cite this article
Liu, W., Zhu, X., Tan, X. et al. Predictive Value of Serum Creatinine/Cystatin C in Acute Ischemic Stroke Patients under Nutritional Intervention. J Nutr Health Aging 25, 335–339 (2021). https://doi.org/10.1007/s12603-020-1495-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12603-020-1495-0