Abstract
Objectives
The aim of the present study was to verify the associations between dysphagia as screened by the Eating Assessment Tool-10 (EAT-10) and indicators in the 100-mL water swallowing test (WST) or medical history among community-dwelling older people.
Study design
A cross-sectional study.
Setting and Participants
The study participants were 202 community-dwelling older Japanese adults aged ≥65 years.
Measurements
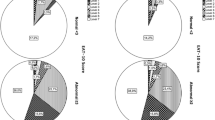
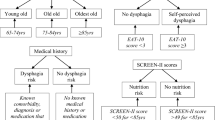
We investigated the participants’ basic attributes, including age, sex, body mass index, medical history (cerebrovascular disease, respiratory disease: chronic obstructive pulmonary disease [COPD], and history of pneumonia within the previous year), and number of prescribed medications. Dysphagia assessment was performed using the EAT-10 and the 100-mL WST as subjective and objective examinations, respectively. The 100-mL WST used four indicators (SC: swallowing capacity, VS: volume per swallow, TS: time per swallow, and choking signs). Patients with and without dysphagia according to the EAT-10 were divided into two groups according to a cutoff score of 3, and the two groups were then compared in terms of their characteristics including medical history and 100-mL WST indicators. A multiple logistic regression model was used to determine whether the indicators of the 100-mL WST or medical history were independently associated with dysphagia in the EAT-10.
Results
The multiple logistic regression analysis revealed that dysphagia in the EAT-10 was independently associated with male sex (odds ratio [OR] = 2.78; 95% confidence interval [CI] = 0.98–7.90), COPD (OR = 14.68; 95% CI = 3.14–68.85), and VS and TS in the 100-mL WST (OR = 0.85; 95% CI = 0.80–0.90 and OR = 3.03; 95% CI = 1.78–5.16, respectively).
Conclusions
Our results revealed that the EAT-10 was independently associated with the 100-mL WST and respiratory disease. We propose that swallowing rehabilitation incorporating respiratory training could be effective for older people screened using the EAT-10.
Similar content being viewed by others
References
Makizako H, Shimada H, Doi T, Tsutsumimoto K, Suzuki T. Impact of physical frailty on disability in community-dwelling older adults: a prospective cohort study. BMJ Open. 2015;5(9):e008462. doi: https://doi.org/10.1136/bmjopen-2015-008462.
Yamada M, Arai H, Sonoda T, Aoyama T. Community-based exercise program is cost-effective by preventing care and disability in Japanese frail older adults. J Am Med Dir Assoc. 2012;13(6):507–511.
Gobbens RJ, van Assen MA, Luijkx KG, Schols JM. Testing an integral conceptual model of frailty. J Adv Nurs. 2012;68(9):2047–2060.
de Andrade FB, Lebrão ML, Santos JL, Duarte YA. Relationship between oral health and frailty in community-dwelling elderly individuals in Brazil. J Am Geriatr Soc. 2013;61(5):809–814.
Tanaka T, Takahashi K, Hirano H, Kikutani T, Watanabe Y, Ohara Y, et al. Oral Frailty as a Risk Factor for Physical Frailty and Mortality in Community-Dwelling Elderly. J Gerontol A Biol Sci Med Sci.2017 Nov 17. doi: https://doi.org/10.1093/gerona/glx225. [Epub ahead of print]
Ortega O, Sakwinska O, Combremont S, Berger B, Sauser J, Parra C, et al. High prevalence of colonization of oral cavity by respiratory pathogens in frail older patients with oropharyngeal dysphagia. Neurogastroenterol Motil. 2015;27(12):1804–1816.
Serra-Prat M, Palomera M, Gomez C, Sar-Shalom D, Saiz A, Montoya JG, et al. Oropharyngeal dysphagia as a risk factor for malnutrition and lower respiratory tract infection in independently living older persons: a population-based prospective study. Age Ageing. 2012;41(3):376–381.
Minakuchi S, Tsuga K, Ikebe K, Ueda T, Tamura F, Nagao K, et al. Oral hypofunction in the older population: Position paper of the Japanese Society of Gerodontology in 2016. Gerodontology. 2018;35(4):317–324.
Nishida T, Yamabe K, Honda S. Dysphagia is associated with oral, physical, cognitive, and psychological frailty in Japanese community-dwelling elderly persons. Gerodontology. 2019;(in press).
Nimmons D, Michou E, Jones M, Pendleton N, Horan M, Hamdy S. A Longitudinal Study of Symptoms of Oropharyngeal Dysphagia in an Elderly Community-Dwelling Population. Dysphagia. 2016;31(4):560–566.
Kawashima K, Motohashi Y, Fujishima. Prevalence of dysphagia among community-dwelling elderly individuals as estimated using a questionnaire for dysphagia screening. Dysphagia. 2004;19(4):266–271.
Belafsky PC, Mouadeb DA, Rees CJ, Pryor JC, Postma GN, Allen J, et al. Validity and reliability of the Eating Assessment Tool (EAT-10). Ann Otol Rhinol Laryngol. 2008;117(12):919–924.
Wakabayashi H, Kayashita J. Translation, reliability, and validity of the Japanese version of the 10-item eating assessment tool (EAT-10) for the screening of dysphagia. Annals of Nutrition and Metabolism. 2014;29(3):75–80.(in Japanese)
Mañas-Martínez AB, Bucar-Barjud M, Campos-Fernández J, Gimeno-Orna JA, Pérez-Calvo J, Ocón-Bretón J. Association of positive screening for dysphagia with nutritional status and long-term mortality in hospitalized elderly patients. Endocrinol Diabetes Nutr. 2018;65(7):402–408.
Osawa A, Maeshima S, Tanahashi N. Water-swallowing test: Screening for aspiration in stroke patients. Cerebrovasc Dis. 2013;(35):276–281.
Wu MC, Chang YC, Wang TG, Lin LC. Evaluating swallowing dysfunction using a 100-ml water swallowing test. Dysphagia. 2004;19(1):43–47.
Patterson JM, Hildreth A, McColl E, Carding PN, Hamilton D, Wilson JA. The clinical application of the 100mL water swallow test in head and neck cancer. Oral Oncol. 2011;47(3):180–184.
Palacios-Ceña D, Hernández-Barrera V, López-de-Andrés A, Fernández-de-Las-Peñas C, Palacios-Ceña M, de Miguel-Díez J, et al. Time trends in incidence and outcomes of hospitalizations for aspiration pneumonia among elderly people in Spain (2003–2013). Eur J Intern Med. 2017;38:61–67.
Gonzalez Lindh M, Blom Johansson M, Jennische M, Koyi H. Prevalence of swallowing dysfunction screened in Swedish cohort of COPD patients. Int J Chron Obstruct Pulmon Dis. 2017;12:331–337.
Hughes TA, Wiles CM. Clinical measurement of swallowing in health and in neurogenic dysphagia. QJM. 1996;89(2):109–116.
Shaker R, Li Q, Ren J, Townsend WF, Dodds WJ, Martin BJ, et al. Coordination of deglutition and phases of respiration: effect of aging, tachypnea, bolus volume, and chronic obstructive pulmonary disease. Am J Physiol. 1992;263(5 Pt 1):G750–755.
Steidl E, Ribeiro CS, Gonçalves BF, Fernandes N, Antunes V, Mancopes R. Relationship between Dysphagia and Exacerbations in Chronic Obstructive Pulmonary Disease: A Literature Review. Int Arch Otorhinolaryngol. 2015;19(1):74–79.
Ebihara S, Sekiya H, Miyagi M, Ebihara T, Okazaki T. Dysphagia, dystussia, and aspiration pneumonia in elderly people. J Thorac Dis. 2016;8(3):632–639.
Takeuchi K, Aida J, Ito K, Furuta M, Yamashita Y, Osaka K. Nutritional status and dysphagia risk among community-dwelling frail older adults. J Nutr Health Aging. 2014;18(4):352–357.
Stoschus B, Allescher HD. Drug-induced dysphagia. Dysphagia. 1993;8(2):154–159.
Acknowledgments
We are grateful to all the participants for their valuable contributions to this study. We also thank Ms. Fumiko Iwai from Yamabe Dental Clinic and Ms. Chinatu Rokutanzono from Sasebo-Chuo Hospital for their support with the data collection.
Funding
Funding: None.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Declaration of interest: none
Competing interests: None declared.
Ethical Approval: All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards. The study protocol was reviewed and approved by the ethics committee of Sasebo-Chuo Hospital before the survey was conducted. Written informed consent was obtained from all participants.
Rights and permissions
About this article
Cite this article
Nishida, T., Yamabe, K., Ide, Y. et al. Utility of the Eating Assessment Tool-10 (EAT-10) in Evaluating Self-Reported Dysphagia Associated with Oral Frailty in Japanese Community-Dwelling Older People. J Nutr Health Aging 24, 3–8 (2020). https://doi.org/10.1007/s12603-019-1256-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12603-019-1256-0