Abstract
Objectives
To gather available evidence about overtime changes on physical performance in institutionalized elderly.
Design, setting and participants
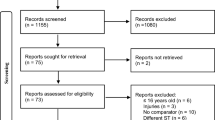
An electronic search was performed on PubMed database on May 2018. We selected articles reporting the evolution of physical performance in older adults living in care institutions. We looked for data from observational longitudinal studies; data from clinical trials were extracted only for subjects who did not receive exercise intervention. All types of performance-based tests, for upper- and/or lower-body, were scrutinized.
Results
Seventeen studies were reviewed; mean age varied from 78.3 to 88 years old. Fourteen studies were randomized controlled trials (RCTs), other three studies were non-randomized trials and a longitudinal observational study. Different tests assessing physical performance were examined: upper limb strength and lower limb strength, static balance, dynamic balance and mobility showed a tendency to decline over time. On average hand grip strength decreased by 2.2% per month, chair stand test by 3.5%, Berg balance scale by 2%, timed up-and-go test by 2.8%, gait speed by 2.1% and short physical performance battery by 2.8%. A minority of studies have shown an improvement in lower limb muscle strength, endurance and gait speed: in these studies, participants did not attend any kind of physical training but took part to social activities or cognitive interventions.
Conclusion
This review shows how physical performance decreases over time in nursing home residents and quantifies their decline. However, in active controls, there was an improvement in some physical performance measures, which indicates that intervention other than exercise might prevent some loss in physical performance.

Similar content being viewed by others
References
Tabue-Teguo M, Dartigues J-F, Simo N, Kuate-Tegueu C, Vellas B, Cesari M. Physical status and frailty index in nursing home residents: Results from the INCUR study. Arch Gerontol Geriatr 2018;74:72–76. doi: https://doi.org/10.1016/j.archger.2017.10.005
Reid N, Keogh JW, Swinton P, Gardiner PA, Henwood TR. The Association of Sitting Time With Sarcopenia Status and Physical Performance at Baseline and 18-Month Follow-Up in the Residential Aged Care Setting. J Aging Phys Act 2018;1–6. doi: https://doi.org/10.1123/japa.2017-0204
Bradley C, Australian Institute of Health and Welfare. Hospitalisations due to falls by older people, Australia, 2009–10. Australian Institute of Health and Welfare, Canberra
Wolinsky FD, Miller DK, Andresen EM, Malmstrom TK, Miller JP, Miller TR. Effect of subclinical status in functional limitation and disability on adverse health outcomes 3 years later. J Gerontol A Biol Sci Med Sci 2007;62:101–106
Wisniowska-Szurlej A, Cwirlej-Sozanska A, Wilmowska-Pietruszynska A, Milewska N, Sozanski B. The influence of 3 months of physical exercises and verbal stimulation on functional efficiency and use of free time in an older population under institutional care: study protocol for a randomized controlled trial. Trials 2017;18:376. doi: https://doi.org/10.1186/s13063-017-2114-1
Williams SW, Williams CS, Zimmerman S, Sloane PD, Preisser JS, Boustani M, Reed PS. Characteristics associated with mobility limitation in long-term care residents with dementia. Gerontologist 2005;45 Spec No 1:62–67
World Alzheimer Report 2013 — Journey of Caring: An analysis of long-term care for dementia. 92
Arrieta H, Rezola-Pardo C, Zarrazquin I, Echeverria I, Yanguas JJ, Iturburu M, Gil SM, Rodriguez-Larrad A, Irazusta J. A multicomponent exercise program improves physical function in long-term nursing home residents: A randomized controlled trial. Exp Gerontol 2018;103:94–100. doi: https://doi.org/10.1016/j.exger.2018.01.008
Binder EF, Miller JP, Ball LJ. Development of a test of physical performance for the nursing home setting. Gerontologist 2001;41:671–679
Guralnik JM, Ferrucci L, Simonsick EM, Salive ME, Wallace RB. Lower-extremity function in persons over the age of 70 years as a predictor of subsequent disability. N Engl J Med 1995;332:556–561. doi: https://doi.org/10.1056/NEJM199503023320902
Ferrucci L, Guralnik JM, Salive ME, Fried LP, Bandeen-Roche K, Brock DB, Simonsick EM, Corti MC, Zeger SL. Effect of age and severity of disability on short-term variation in walking speed: the Women’s Health and Aging Study. J Clin Epidemiol 1996;49:1089–1096
Reuben DB, Rubenstein LV, Hirsch SH, Hays RD. Value of functional status as a predictor of mortality: results of a prospective study. Am J Med 1992;93:663–669
Reuben DB, Siu AL, Kimpau S. The predictive validity of self-report and performance-based measures of function and health. J Gerontol 1992;47:M106–110
Applegate WB, Blass JP, Williams TF. Instruments for the functional assessment of older patients. N Engl J Med 1990;322:1207–1214. doi: https://doi.org/10.1056/NEJM199004263221707
Branch LG, Meyers AR. Assessing physical function in the elderly. Clin Geriatr Med 1987;3:29–51
de Souto Barreto P, Cesari M, Denormandie P, Armaingaud D, Vellas B, Rolland Y. Exercise or Social Intervention for Nursing Home Residents with Dementia: A Pilot Randomized, Controlled Trial. J Am Geriatr Soc 2017;65:E123–E129. doi: https://doi.org/10.1111/jgs.14947
Mulrow CD, Gerety MB, Kanten D, Cornell JE, DeNino LA, Chiodo L, Aguilar C, O’Neil MB, Rosenberg J, Solis RM. A randomized trial of physical rehabilitation for very frail nursing home residents. JAMA 1994;271:519–524
Chiu S-C, Yang R-S, Yang R-J, Chang S-F. Effects of resistance training on body composition and functional capacity among sarcopenic obese residents in long-term care facilities: a preliminary study. BMC Geriatr 2018;18:21. doi: https://doi.org/10.1186/s12877-018-0714-6
Frandin K, Gronstedt H, Helbostad JL, Bergland A, Andresen M, Puggaard L, Harms-Ringdahl K, Granbo R, Hellstrom K. Long-Term Effects of Individually Tailored Physical Training and Activity on Physical Function, Well-Being and Cognition in Scandinavian Nursing Home Residents: A Randomized Controlled Trial. Gerontology 2016;62:571–580. doi: https://doi.org/10.1159/000443611
Benavent-Caballer V, Rosado-Calatayud P, Segura-Orti E, Amer-Cuenca JJ, Lison JF. Effects of three different low-intensity exercise interventions on physical performance, muscle CSA and activities of daily living: a randomized controlled trial. Exp Gerontol 2014;58:159–165. doi: https://doi.org/10.1016/j.exger.2014.08.004
Cebria I Iranzo MA, I Bernat MB, Tortosa-Chulia MA, Balasch-Parisi S. Effects of Resistance Training of Peripheral Muscles versus Respiratory Muscles in Institutionalized Older Adults with Sarcopenia: A Randomized Controlled Trial. J Aging Phys Act 2018;1–32. doi: https://doi.org/10.1123/japa.2017-0268
Tak ECPM, van Hespen A, van Dommelen P, Hopman-Rock M. Does improved functional performance help to reduce urinary incontinence in institutionalized older women? A multicenter randomized clinical trial. BMC Geriatr 2012;12:51. doi: https://doi.org/10.1186/1471-2318-12-51
Holmerova I, Machacova K, Vankova H, Veleta P, Juraskova B, Hrnciarikova D, Volicer L, Andel R. Effect of the Exercise Dance for Seniors (EXDASE) program on lower-body functioning among institutionalized older adults. J Aging Health 2010;22:106–119. doi: https://doi.org/10.1177/0898264309351738
Rolland Y, Pillard F, Klapouszczak A, Reynish E, Thomas D, Andrieu S, Riviere D, Vellas B. Exercise program for nursing home residents with Alzheimer’s disease: a 1-year randomized, controlled trial. J Am Geriatr Soc 2007;55:158–165. doi: https://doi.org/10.1111/j.1532-5415.2007.01035.x
Lauze M, Martel DD, Aubertin-Leheudre M. Feasibility and Effects of a Physical Activity Program Using Gerontechnology in Assisted Living Communities for Older Adults. J Am Med Dir Assoc 2017;18:1069–1075. doi: https://doi.org/10.1016/j.jamda.2017.06.030
Baum EE, Jarjoura D, Polen AE, Faur D, Rutecki G. Effectiveness of a group exercise program in a long-term care facility: a randomized pilot trial. J Am Med Dir Assoc 2003;4:74–80. doi: https://doi.org/10.1097/01.JAM.0000053513.24044.6C
Meng G, Wang H, Pei Y, Li Y, Wu H, Song Y, Guo Q, Guo H, Fukushima S, Tatefuji T, Wang J, Du H, Su Q, Zhang W, Shen S, Wang X, Dong R, Han P, Okazaki T, Nagatomi R, Wang J, Huang G, Sun Z, Song K, Niu K. Effects of protease-treated royal jelly on muscle strength in elderly nursing home residents: A randomized, double-blind, placebo-controlled, dose-response study. Sci Rep 2017;7:11416. doi: https://doi.org/10.1038/s41598-017-11415-6
Gronstedt H, Frandin K, Bergland A, Helbostad JL, Granbo R, Puggaard L, Andresen M, Hellstrom K. Effects of individually tailored physical and daily activities in nursing home residents on activities of daily living, physical performance and physical activity level: a randomized controlled trial. Gerontology 2013;59:220–229. doi: https://doi.org/10.1159/000345416
Oesen S, Halper B, Hofmann M, Jandrasits W, Franzke B, Strasser E-M, Graf A, Tschan H, Bachl N, Quittan M, Wagner KH, Wessner B. Effects of elastic band resistance training and nutritional supplementation on physical performance of institutionalised elderly—A randomized controlled trial. Exp Gerontol 2015;72:99–108. doi: https://doi.org/10.1016/j.exger.2015.08.013
Mouton A, Gillet N, Mouton F, Van Kann D, Bruyere O, Cloes M, Buckinx F. Effects of a giant exercising board game intervention on ambulatory physical activity among nursing home residents: a preliminary study. Clin Interv Aging 2017;12:847–858. doi: https://doi.org/10.2147/CIA.S134760
Leavitt MO. Physical Activity Guidelines for Americans. 2008;76
Matthews CE, Chen KY, Freedson PS, Buchowski MS, Beech BM, Pate RR, Troiano RP. Amount of Time Spent in Sedentary Behaviors in the United States, 2003–2004. American Journal of Epidemiology 2008;167:875–881. doi: https://doi.org/10.1093/aje/kwm390
Healy GN, Clark BK, Winkler EAH, Gardiner PA, Brown WJ, Matthews CE. Measurement of Adults’ Sedentary Time in Population-Based Studies. American Journal of Preventive Medicine 2011;41:216–227. doi: https://doi.org/10.1016/j.amepre.2011.05.005
Reid N, Eakin E, Henwood T, Keogh JWL, Senior HE, Gardiner PA, Winkler E, Healy GN. Objectively measured activity patterns among adults in residential aged care. Int J Environ Res Public Health 2013;10:6783–6798. doi: https://doi.org/10.3390/ijerph10126783
Harvey JA, Chastin SFM, Skelton DA. How Sedentary are Older People? A Systematic Review of the Amount of Sedentary Behavior. J Aging Phys Act 2015;23:471–487. doi: https://doi.org/10.1123/japa.2014-0164
Kojima G. Prevalence of Frailty in Nursing Homes: A Systematic Review and Meta-Analysis. J Am Med Dir Assoc 2015;16:940–945. doi: https://doi.org/10.1016/j.jamda.2015.06.025
Collard RM, Boter H, Schoevers RA, Oude Voshaar RC. Prevalence of Frailty in Community-Dwelling Older Persons: A Systematic Review. Journal of the American Geriatrics Society 2012;60:1487–1492. doi: https://doi.org/10.1111/j.1532-5415.2012.04054.x
Smith GI, Atherton P, Villareal DT, Frimel TN, Rankin D, Rennie MJ, Mittendorfer B. Differences in muscle protein synthesis and anabolic signaling in the postabsorptive state and in response to food in 65–80 year old men and women. PLoS One 2008;3:e1875. https://doi.org/10.1371/journal.pone.0001875
Pothier K, Gagnon C, Fraser SA, Lussier M, Desjardins-Crepeau L, Berryman N, Kergoat M-J, Vu TTM, Li KZH, Bosquet L, Bherer L. A comparison of the impact of physical exercise, cognitive training and combined intervention on spontaneous walking speed in older adults. Aging Clin Exp Res 2017. doi: https://doi.org/10.1007/s40520-017-0878-5
Azadian E, Torbati HRT, Kakhki ARS, Farahpour N. The effect of dual task and executive training on pattern of gait in older adults with balance impairment: A Randomized controlled trial. Arch Gerontol Geriatr 2016;62:83–89. doi: https://doi.org/10.1016/j.archger.2015.10.001
Li KZH, Roudaia E, Lussier M, Bherer L, Leroux A, McKinley PA. Benefits of cognitive dual-task training on balance performance in healthy older adults. J Gerontol A Biol Sci Med Sci 2010;65:1344–1352. doi: https://doi.org/10.1093/gerona/glq151
Acknowledgements
I would like to thank Mathieu Maltais and Philipe de Souto Barreto for their help and their work. A special thanks to Professor Yves Rolland and Professor Bruno Vellas for giving me the chance to work on his team.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Masciocchi, E., Maltais, M., Rolland, Y. et al. Time Effects on Physical Performance in Older Adults in Nursing Home: A Narrative Review. J Nutr Health Aging 23, 586–594 (2019). https://doi.org/10.1007/s12603-019-1199-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12603-019-1199-5