Abstract
Background
Frailty-related characteristics, such as sarcopenia, malnutrition and cognitive impairment, are often overlooked, both in clinical practice and research, as potential contributors to functional recovery during geriatric rehabilitation.
Objective
The aim of the study was to identify frailty-related characteristics associated with functional recovery in a cohort of post-orthopedic surgery and post-stroke older adults.
Design
Multi-centric cohort study.
Participanst and Settings
Patients over 65 years, admitted to three geriatric rehabilitation units, in Spain and Italy, after an orthopedic event or a stroke, from December 2014 to May 2016.
Measurements
The Absolute Functional Gain (AFG) defined as the difference between Barthel Index score at discharge and at admission, and the Relative Functional Gain (RFG) that represents the percentage of recovery of the function lost due to the event, were selected as outcomes. Both outcomes were analyzed as continuous and dichotomous variables. Analyses were also stratified as diagnostic at admission.
Results
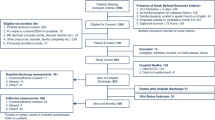
We enrolled 459 patients (mean age±SD=80.75±8.21 years), 66.2% women, 69.5% with orthopedic conditions and with a length of stay of 28.8±9.1 days. Admission after a stroke (Odds Ratio=0.36, 95% Confidence Interval=0.22-0.59]) and a better functional status at admission (OR=0.96, 95% CI=0.94-0.97), were associated with a lower likelihood of AFG, while a better pre-event Barthel index (OR=1.03 for each point in score, 95% CI=1.01-1.04), being able to walk (OR=2.07, 95% CI=1.16-3.70), and a better cognitive status at admission (OR=1.05, 95% CI=1.01-1.09), were associated with a higher chance of AFG. Post-stroke patients with delirium at admission had a re-duced chance of AFG (OR=0.25, 95% CI=0.07-0.91]). Patients admitted after an orthopedic event with better pre-event functional status (OR=1.04, 95% CI=1.02-1.06) and able to walk at admission (OR=2.79, 95% CI=1.29-6.03]) had an increased chance of AFG. Additionally, in both diagnostics groups, a better handgrip strength increased the chance of RFG.
Conclusions
Among frailty-related variables, physical, cognitive and muscular function at admission could be relevant for functional improvement during geriatric reha-bilitation. If confirmed, this data might orient targeted interventions.







Similar content being viewed by others
References
Morley JE, Vellas B, Abellan Van Kan G, et al. Frailty consensus: a call to action. J Am Med Dir Assoc 2013; 14:392–7.
Clegg A, Young J, Iliffe S et al. Frailty in elderly people. Lancet 2013; 381:752–62.
Theou O, Brothers TD, Mitnitski A, Rockwood K. Operationalization of frailty using eight commonly used scales and comparison of their ability to predict all-cause mortali-ty. J Am Geriatr Soc 2013; 61:1537–51.
Fried LP, Tangen CN, Walston J, et al. Frailty in older adults: evidence for a phenotype. J Gerontol A Biol Sci Med Sci 2001; 56:146–56.
Whitson HE, Purser JL, Cohen HJ. Frailty thy name is᾿Phrailty? J Gerontol A Biol Sci Med Sci 2007; 62:728–30.
Bachmann S, Finger C, Huss A, et al. Inpatient rehabilitation specifically designed for geriatric patients: systematic review and meta-analysis of randomised controlled trials. BMJ 2010; 340:c1718.
Onder G, Penninx BW, Ferrucci L, et al. Measures of physical performance and risk for progressive and catastrophic disability: results from the women’s health and aging study. J Gerontol A Biol Sci Med Sci 2005; 60:74–79.
Buntin MB, Colla CH, Deb P, et al. Medicare spending and outcomes after postacute care for stroke and hip fracture. Med Care 2010; 48:776–84.
Bellelli G, Mazzola P, Morandi A, et al. Duration of postoperative delirium is an independent predictor of 6-month mortality in older adults after hip fracture. J Am Geriatr Soc. 2014; 62:1335–40
Formiga F, Navarro M, Duaso E et al. Factors associated with hip fracture-related falls among patients with a history of recurrent falling. Bone 2008; 43: 941–44
Krishnan M, Beck S, Havelock W, et al. Predicting outcome after hip fracture: using a frailty index to integrate comprehensive geriatric assessment results. Age Ageing. 2014; 43:122–26
Landi F, Onder G, Cesari M, et al. Functional decline in frail community-dwelling stroke patients. Eur J Neurol 2006; 13:17–23.
Amblàs-Novellas J, Espaulella-Panicot J, Inzitari M, et al. En busca de respuestas al reto de la complejidad clínica en el siglo XXI: A propósito de los índices de fragilidad. Rev Esp Geriatr Gerontol. 2016; https://doi.org/10.1016/j.regg.2016.07.005, pii:S0211-139X (16)30104-4.
Scherbakov N, Sandek A, Doehner W. Stroke-related sarcopenia: specific characteristics. J Am Med Dir Assoc 2015; 16:272–6.
Ricci E, Guerini F, Bellelli G, Trabucchi M. Rehabilitation of older adults with hip frac-ture: cognitive function and walking abilities. J Am Geriatr Soc 2011; 59:1497᾿02.
Gotor P, Queipo R, Velasco R, et al. Prevalence of sarcopenia in acute hip fracture patients and its influence on short-term clinical outcome. Geriatr Gerontol Int 2016; 16:1021᾿7.
Charlson ME, Pompei P, Ales KL, MacKenzie CR. A new method of classifying prognostic comorbidity in longitudinal studies: development and validation. J Chronic Dis 1987; 40: 373᾿3.
Rubenstein LZ, Harker JO, Salvà A, et al. Screening for under nutrition in geriatric practice: developing the Short- Form Mini-Nutritional Assessment (MNA-SF). J Gerontol A Biol Sci Med Sci 2001; 56: M366᾿2.
Folstein MF, Folstein SE, McHugh PR. MiniMental State. A practical method for grading the cognitive state of patients for the clinician. J Psychiatr Res. 1975; 12:189᾿8.
Inouye SK, Van Dyck CH, Alessi CA, et al. Clarifying confusion: The Confusion As-sessment Method. A new method for detection of delirium. Ann Intern Med 1990; 113:941᾿8.
Cruz-Jentoft AJ, Baeyens JP, Bauer JM, et al. Sarcopenia: European consensus on definition and diagnosis. Age Ageing 2010; 39: 412᾿3.
Bosaeus I, Wilcox G, Rothenberg E, Strauss BJ. Skeletal muscle mass in hospital-ized elderly patients: comparison of measurements by single-frequency BIA and DXA. Clin Nutr 2014; 33: 426᾿1.
Janssen I, Heymsfield SB, Baumgartner RN, Ross R. Estimation of skeletal muscle mass by bioelectrical impedance analysis. J Appl Physiol 2000; 89:465᾿1.
Mahoney FI, Barthel DW. Funtional evaluation: The Barthel index. Md State Med J 1965; 14: 61᾿5.
Koh GC-H, Chen CH, Petrella R, Thind A. Rehabilitation impact indices and their independent predictors: a systematic review. BMJ Open 2013; 3: e003483.
Heinemann AW, Roth EJ, Cichowski K, et al. Multivariate analysis of improvement and outcome following stroke rehabilitation. Arch Neurol 1987; 44:1167–72.
Pérez LM, Inzitari M, Quinn TJ, et al. Rehabilitation Profiles of Older Adult Stroke Survivors Admitted to Intermediate Care Units: A Multi-Centre Study. PLoS One 2016 Nov 9; 11(11):e0166304.
Miralles R, Muniesa JM, Mojal S, et al. Three measures of physical rehabilitation effectiveness in elderly patients: a prospective, longitudinal, comparative analysis. BMC Geriatr 2015 Oct 29; 15:142.
Baztán JJ, Gálvez CP, Socorro A. Recovery of functional impairment after acute illness and mortality: One-Year follow-up study. Gerontology 2009; 55:269–74.
Pérez LM, Inzitari M, Roqué M, et al. Change in cognitive performance is associated with functional recovery during post-acute stroke rehabilitation: a multi-centric study from intermediate care geriatric rehabilitation units of Catalonia. Neurol Sci. 2015; 36: 1875–80.
Morghen S, Morandi A, Guccione AA, et al. The association between patient participation and functional gain following inpatient rehabilitation. Aging Clin Exp Res 2017; 29:729–36.
Morghen S, Gentile S, Ricci E, et al. Rehabilitation of older adults with hip fracture: Cognitive function and walking abilities. J Am Geriatr Soc 2011;59:1497–502.
Inouye M, Kishi K, Ikeda Y et al. Prediction of functional outcome after stroke rehabilitation. Am J Phys Med Rehabil. 2000;79:513–18.
Peel NM, Navanathan S, Hubbard RE. Gait speed as a predictor of outcomes in postacute transitional care for older people. Geriatr Gerontol Int 2014; 14:906–10
Fritz S, Lusardi M. White paper:“walking speed: the sixth vital sign᾿J Geriatr Phys Ther 2009; 32:2–5
Abellan Van Kan G, Rolland Y, Andrieu S et al. Gait speed at usual pace as a predic-tor of adverse outcomes in community-dwelling older people an International Academy on Nutrition and Aging (IANA) Task Force. J Nutr Health Aging 2009; 13: 881–9.
Sánchez-Rodríguez D, Marco E, Miralles R, et al. Sarcopenia, physical rehabilitation and functional outcomes of patients in a subacute geriatric care unit. Arch Gerontol Ge-riatr 2014; 59:39–43.
Bianchi L, Abete P, Bellelli G, et al. GLISTEN Group Investigators. Prevalence and Clinical Correlates of Sarcopenia, Identified According to the EWGSOP Definition and Diagnostic Algorithm, in Hospitalized Older People: The GLISTEN Study. J Gerontol A Biol Sci Med Sci 2017 Jan 21. doi: 10.1093/gerona/glw343
Morandi A, Onder G, Fodri L, et al. The association between the probability of sar-copenia and functional outcomes in older patients undergoing in-hospital rehabilitation. J Am Med Dir Assoc 2015; 16:951–56.
Di Monaco M, Castiglioni C, De Toma E, et al. Handgrip strength is an independent predictor of functional outcome in hip-fracture women: a prospective study with 6-month follow-up. Medicine (Baltimore) 2015; 94: e542.
Inouye M, Kishi K, Ikeda Y et al. Prediction of functional outcome after stroke rehabilitation. Am J Phys Med Rehabil. 2000; 79:513–18.
Reeves MJ, Bushnell CD, Howard G, et al. Sex differences in stroke: epidemiolo-gy, clinical presentation, medical care, and outcomes. Lancet Neurol 2008; 7: 915–26.
Arber S, Cooper S. Gender differences in later life: the new paradox. Soc Sci Med 1999; 48:61–76.
Cary MP, Jr, Merwin EI, Oliver MN, Williams IC. Inpatient rehabilitation outcomes in a national sample of Medicare beneficiaries with hip fracture. J Appl Gerontol 2014
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Calle, A., Onder, G., Morandi, A. et al. Frailty Related Factors as Predictors of Functional Recovery in Geriatric Rehabilitation: The Sarcopenia and Function in Aging Rehabilitation (SAFARI) Multi-Centric Study. J Nutr Health Aging 22, 1099–1106 (2018). https://doi.org/10.1007/s12603-018-1060-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12603-018-1060-2