Abstract
Objective
Caloric restriction (CR) is proven to be effective in increasing life span and it is well known that, nutritional habits, sleeping pattern and meal frequency have profound effects on human health. In Ramadan some Muslims fast during the day-light hours for a month, providing us a unique model of intermittent fasting (IF) in humans. In the present study, we have investigated the effects of IF versus CR on the same non-diabetic obese subjects who were followed for two years according to the growth hormone (GH)/Insulin like growth factor (IGF)-1 axis and insulin resistance.
Design
Single-arm Interventional Human Study.
Participants
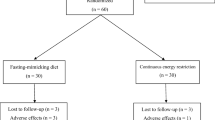
23 female subjects (Body Mass Index (BMI) 29-39, aged between 28-42years).
Setting
Follow-up is designed as 12 months of CR, after which there was a month of IF and 11 months of CR again, to be totally 24 months. Subjects’ daily diets were aligned as low calorie diet during CR and during the IF period, the same subjects fasted for 15 hours in a day for a month and there was no daily calorie restriction. Nutritional pattern was changed as 1 meal in the evening and a late supper before sleeping and no eating and drinking during the day light hours in the IF model. Subjects made brisk walking twice a day during the whole follow-up including both CR and IF periods. BMI, Blood glucose, insulin, TSH, GH, HbA1c, IGF-1, Homa-IR and urinary acetoacetate levels were monitored once in three months and twice in the fasting month.
Measurements and Results
While subjects lost 1250 ± 372g monthly during the CR, in the IF period, weight loss was decreased to 473 ±146 g. BMI of all subjects decreased gradually and as the BMI decreased, glucose, HbA1c, insulin, Homa-IR and TSH levels were decreased. GH levels were at baseline at the beginning, increased in the first six months and stayed steady during the CR and IF period than began decreasing after the IF period, while IGF-I increased gradually during the CR period and beginning with the 7th day of IF period, it decreased and kept on decreasing till the end of the follow-up. Urinary acetoacetate levels were higher during the IF period suggesting a constant lipid catabolism.
Conclusion
Our results suggest that, CR affects metabolic parameters positively which will help especially pre-diabetic and insulin resistant patients without any pharmacological approach. In addition IF without calorie restriction can enhance health and cellular resistance to disease without losing weight and those effects may be attributed to different signalling pathways and circulating ketones during IF. Changes observed during IF are probably due to the changes in eating and sleeping pattern and thus changes in metabolic rhythm.
Similar content being viewed by others
References
Fontana L, Patridge L, Longo V. Dietary restriction, growth factors and aging. From yeast to humans. Science April 2010;16; 328(5976):321–326
Lopez-Otin C, Blasco MA, Partridge L, Serrano M, Kroemer G. The hallmarks of aging. Cell 2013;53: 1194–1217
Colman RJ, Anderson RM, Johnson SC, Kastman EK, Kosmatka KJ, Beasly TM, et al. Caloric restriction delays disease onset and mortality in rhesus monkeys. Science 2009;10;325 (5937):201–204
Anson RM, Guo Z, Cabo R, Lyun T, Rios M, Hagepanos A, et al. Intermittent fasting dissociates beneficial effects of dietary restriction on glucose metabolism and neuronal resistance to injury from calorie intake. PNAS 2003;100: 6216–6220
Martin B, Mattson M, Maudsley S. Caloric restriction and intermittent fasting: two potential diets for successful brain aging. Aging Research Reviews 2006;58(3): 332–353
Ascaso JF, Pardo S, Real JT, Lorente RI, Priego A, et al. Diagnosing Insulin Resistance by Simple Quantitative Methods in Subjects With Normal Glucose Metabolism. Diabetes Care 2003;26: 3320–3325.
Aksungar FB, Topkaya AE, Akyildiz M. Interleukin-6, C-reactive protein and biochemical parameters during prolonged intermittent fasting. Ann Nutr Metab 2007;51: 88–95
Bogdan A, Bouchareb B, Touitou Y. Ramadan fasting alters endocrine and neuroendocrine circadian patterns. Meal-time as a synchronizer in humans? Life Sci 2001;68: 1607–1615
Beavers KM, Gordon MM, Easter L, Beavers DP, Hairston KG, Nicklas BJ, Vitolins MZ. Effect of protein source during weight loss on body composition, cardiometabolic risk and physical performance in abdominally obese, older adults: a pilot feeding study. J Nutr Health Aging. Jan;2015;19(1): 87–95. doi: 10.1007/s12603-015-0438-7.
Normandin E, Senecal M, Prudhomme R, Rabasa-Lhorat R, Brochu M. Effects of Caloric Restriction with or without Resistance Training in Dynapenic-Overweight and Obese Menopausal Women: A Monet Study. J Frailty Aging 2015;4(3): 155–162
Vottero A, Guzetti C, Loche S. New Aspects of The Physiology of The GH-IGF-I Axis. Endocr Dev 2013;24: 96–105
Rajpathak SN, Gunter MJ, Wylie-Rosett J, Ho GYF, Kaplan RC, Muzumdar R, et al. The role of insulin-like growth factor-I and its binding proteins in glucose homeostasis and type 2 diabetes. Diabetes Metab Res Rev 2009;25: 3–12
Underwood LE, Thissen JP, Lemozy S, Ketelslegers JM, Clemmons DR. Hormonal and nutritional regulation of IGF-I and its binding proteins. Horm Res 2004,42: 145–151.
Thissen JP, Ketelslegers JM, Underwood LE. Nutritional regulation of the insulinlike growth factors. Endocr Rev 1994,15: 80–101.
Kaushal K, Heald AH, Siddals KW, et al. The impact of abnormalities in IGF and inflammatory systems on the metabolic syndrome. Diabetes Care 2004,27: 2682–2688.
Woods KA, Camacho-Hubner C, Bergman RN, Barter D, Clark AJ, Savage MO. Effects of insulin-like growth factor I (IGF-I) therapy on body composition and insulin resistance in IGF-I gene deletion. J Clin Endocrinol Metab 2000,85:1407–1411.
Moses AC, Young SC, Morrow LA, O’Brien M, Clemmons DR. Recombinant human insulin-like growth factor I increases insulin sensitivity and improves glycemic control in type II diabetes. Diabetes 1996;45: 91–100.
Yamanaka Y, Fowlkes JL, Wilson EM, Rosenfeld RG, Oh Y. Characterization of insulin-like growth factor binding protein-3 (IGFBP-3) binding to human breast cancer cells: kinetics of IGFBP-3 binding and identification of receptor binding domain on the IGFBP-3 molecule. Endocrinology 1999;140: 1319–1328.
Schedlich LJ, Le Page SL, Firth SM, Briggs LJ, Jans DA, Baxter RC. Nuclear import of insulin-like growth factor-binding protein-3 and -5 is mediated by the importin beta subunit. J Biol Chem 2000;275: 23462–23470.
Muzumdar RH, Ma X, Fishman S, et al. Central and opposing effects of IGF-I and IGF-binding protein-3 on systemic insulin action. Diabetes 2006;55: 2788–2796.
Silha JV, Gui Y, Murphy LJ. Impaired glucose home2006;ostasis in insulin-like growth factor-binding protein-3-transgenic mice. Am J Physiol Endocrinol Metab 2002;283: E937–E945.
Poplawski MM, Mastaitis JW, Yang XJ, Mobbs CV. Hypothalamic responses to fasting indicate metabolic reprogramming away from glycolysis toward lipid oxidation. Endocrinol 2008;295: 101–105.
Bough KJ, Valiyil R, Han FT, Eagles DA. Seizure resistance is dependent upon age and calorie restriction in rats fed a ketogenic diet. Epilepsy Res 1999;35: 21–28
Kashiwaya Y, Takeshima T, Mori N, Nakashima K, Clarke K, Veech R. D-betahydroxybutyrate protects neurons in models of Alzheimer’s and Parkinson’s disease. Proc. Natl. Acad. Sci. 2000;97: 5440–5444.
Rajpathak SN, McGinn AP, Strickler HD, et al. Insulin-like growth factor (IGF)-axis, inflammation, and glucose intolerance among older adults. Growth Horm IGF Res 2008;18(2): 166–173.
Wang Z, Al-Regaiey KA, Masternak MM, Bartke A. Adipocytokines and lipid levels in Ames dwarf and caloric restricted mice. J Gerontol A Biol Sci Med Sci 2006;61A: 323–331
Brown-Borg HM, Bartke A. GH and IGF1: Roles in energy metabolism of longliving GH mutant mice. J Gerontol A Biol Sci Med Sci. June; 2012;67A(6): 652–660
Cheng, B. & Mattson, M.P. IGF-I and IGF-II protect cultured hippocampal and septal neurons against calcium-mediated hypoglycemic damage. J. Neurosci 1992;12: 1558–1566.
Hsieh, C.C., DeFord, J.H., Flurkey, K., Harrison, D.E., Papaconstantinou, J. Implications for the insulin signaling pathway in Snell dwarf mouse longevity: a similarity with the C. elegans longevity paradigm. Mech. Ageing Dev 2002;123: 1229–1244.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Aksungar, F.B., Sarikaya, M., Coskun, A. et al. Comparison of intermittent fasting versus caloric restriction in obese subjects: A two year follow-up. J Nutr Health Aging 21, 681–685 (2017). https://doi.org/10.1007/s12603-016-0786-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12603-016-0786-y