Abstract
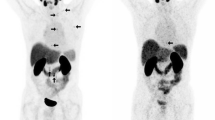
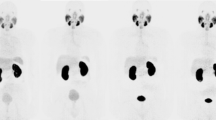
To compare the radiation dose delivered by Positron Emission Tomography (PET) due to Gallium-68 (68Ga) and Fluorine-18(18F) performed for patients with prostate cancer. The greatest importance is to understand how the extremely strong sources in use can be managed effectively and doses to persons and unwanted doses to patients can be minimized. Thus, Radiation safety measurements are necessary to achieve the lowest exposure with reasonable cost and effort. We prospectively analyzed studies from 70 patients who underwent PET-CT using 68Ga or 18F for diagnosis of prostate cancer between January 2017 and December 2017 at the American University of Beirut Medical Center. The dose rates were measured during the uptake period at patient body surface (abdomen) and at 1 m distance; these two points were measured after one hour of radionuclide uptake with background of 0.018 μSv. Then, the equivalent dose is calculated. Patients were selected consecutively until 70 cases were selected for each type of radionuclide. Data on 140 patients are presented. The maximum dose given to 68Ga PSMA (prostate-specific membrane antigen) patients was 5.80 mCi while doses to 18F-Choline patients reached 8.87 mCi. Cronbach’s Alpha values for the correlation between the masses and the dose rates was 0.530.Thus there is a small positive relationship between the body masses and the dose rates. This relationship is not statistically significant. Furthermore, the equivalent dose for both radionuclides was constant whatever the mass of the patient is. There is no effect of the body mass with respect to the dose rate, and equivalent dose due to both radionuclides 68Ga and 18F, which coincides with the principles of radiation protection. This leads to the suggestion that PET/CT equivalent doses with 68Ga-labelled PSMA ligand or 18F-Choline are similar and safe in the diagnosis of prostate cancer. However, 68Ga PSMA coincides more with radiation protection principles since the maximum equivalent dose due to 68Ga after 1 h at 1 m was 17.71 μSv while the maximum equivalent dose due to 18F after 1 h at 1 m was 39.51 μSv.


Similar content being viewed by others
Abbreviations
- PET:
-
Positron Emission Tomography
- CT:
-
Computed Tomography
- PC:
-
Prostate Cancer
- PSMA:
-
Prostate-Specific Membrane Antigen
- Inj:
-
Injection
References
International Commission on Radiological Protection. Radiological protection in medicine. ICRP Publication 105. Ann ICRP. 2007;37:1–63.
Menzel F et al. Using of BEPU methodology in a final safety analysis report. 2015.
ICRP. What is radiation dose? http://www.icrp.org/icrpaedia/dose.asp
Jemal A, Bray F, Center MM, Ferlay J, Ward E, Forman D. Global cancer statistics. CA: CA Cancer J Clin. 2011;61:69–90.
Shamseddine A, Saleh A, Charafeddine M, Seoud M, Mukherji D, Temraz S, et al. Cancer trends in Lebanon: a review of incidence rates for the period of 2003–2008 and projections until 2018. Popul Health Metr. 2014;12:4.
Grant FD et al. Skeletal PET with^ 1^ 8F-Fluoride: applying new technology to an old tracer. J Nuclear Med. 2008: 68.
Pagani M, Stone-Elander S, Larsson SA. Alternative positron emission tomography with non-conventional positron emitters: effects of their physical properties on image quality and potential clinical applications. Eur J Nucl Med. 1997:1301–27.
Production challenges of Gallium-68 labeled radiopharmaceuticals. https://www.comecer.com/nl/gallium-68-radiopharmaceuticals-production-challenges/.
Dwivedi DK et al. Radiation exposure to nuclear medicine personnel handling positron emitters from Ge-68/Ga-68 generator. Indian J Nucl Med: IJNM: Off J Soc Nucl Med, India. 2011: 86.
International Commission on Radiological Protection. Committee IV on Protection Against Electromagnetic Radiation Above 3 MeV and Electrons, Neutrons, and Protons. Radiation protection; recommendations of the International Commission on Radiological Protection: Report of Committee IV (1953–1959) on Protection against Electromagnetic Radiation above 3 MeV and Electrons, Neutrons and Protons. Adopted 1962, with revisions adopted in 1963. Vol. 4. Published for the International Commission on Radiological Protection [by] MacMillan, 1964.
Kendall GM, Smith TJ. Doses to organs and tissues from radon and its decay products. J Radiol Prot. 2002:389.
Valentin J. Basic anatomical and physiological data for use in radiological protection: reference values: ICRP publication 89.Ann ICRP. 2002: 1–277.
Martin CJ. Effective dose: how should it be applied to medical exposures?. The British J Radiol. 2007: 639–647.
Salame-Alfie A. Assessing dose of the representative person for the purpose of radiation protection of the public and the optimization of radiological protection: broadening the process. Health Phys. 2008: 373–374.
Ferrari A, Pelliccioni M, Pillon M. Fluence to effective dose and effective dose equivalent conversion coefficients for photons from 50 keV to 10 GeV. Radiat Prot Dosim. 1996: 245–251.
Pant GS, Senthamizhchelvan S. Radiation exposure to staff in a PET/CT facility. Indian J Nucl Med. 2006: 100–3.
Demir M et al. Radiation protection for accompanying person and radiation workers in PET/CT. Radiation Protect Dosimet. 2010: 528–532.
Benatar NA, Cronin BF, O'doherty M. Radiation doses received by staff and carers/escorts following contact with IsF-FDG PET patients. 1999: 462.
Author information
Authors and Affiliations
Contributions
Zeinab Khansa: contributed data collection and manuscript preparation.
Mohamad B. Haidar: contributed to data collection, study design and manuscript editing.
Nemer Neaimeh: contributed to data collection.
Mahmoud Korek: contributed to study design.
All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Consent for publication
Not applicable.
Availability of data and materials
All relevant data and materials are available upon request.
Conflict of interest
None to declare.
Rights and permissions
About this article
Cite this article
Khansa, Z., Haidar, M.B., Neaimeh, N. et al. Comparison of PET imaging with a 68Ga-labelled PSMA ligand versus 18F-choline PET/CT for the diagnosis of Prostate Cancer & Radioprotection for involved personnel. Health Technol. 9, 607–613 (2019). https://doi.org/10.1007/s12553-018-00281-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12553-018-00281-5