Abstract
Human heart samples from the Sydney Heart Bank have become a de facto standard against which others can be measured. Crucially, the heart bank contains a lot of donor heart material: for most researchers this is the hardest to obtain and yet is necessary since we can only study the pathological human heart in comparison with a control, preferably a normal heart sample. It is not generally realised how important the control is for human heart studies. We review our studies on donor heart samples. We report the results obtained with 17 different donor samples collected from 1994 to 2011 and measured from 2005 to 2015 by our standard methodology for in vitro motility and troponin I phosphorylation measurements. The donor heart sample parameters are consistent between the hearts, over time and with different operators indicating that Sydney Heart Bank donor hearts are a valid baseline control for comparison with pathological heart samples. We also discuss to what extent donor heart samples are representative of the normal heart.
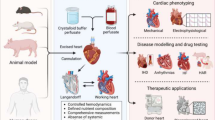
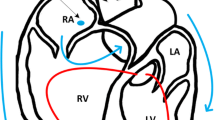
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
It is a great pleasure to contribute to this special issue celebrating the achievements of Cris Dos Remedios and to celebrate his unique creation— the Sydney Heart Bank.
This story starts in Berlin in September 2000. I had known Cris as a biophysicist for as long as I can remember. The European Muscle Congress was held in Berlin for the first time in 2000—an age when PowerPoint was a new and risky mode of presentation. After the meeting finished, we found ourselves at a loose end waiting for evening flights and trains and went for a late lunch at the Potsdamer Platz. During our conversation, Cris revealed that he had been collecting human hearts from transplant operations in Sydney.
This was a great surprise to me and a pleasant one as well. A couple of years prior, I had started a project to apply our in vitro motility assay to the contractile proteins from human hearts. Ian Purcell, then an MD student, had been able to obtain a small amount of fresh heart tissue from transplant operations at the Freeman Hospital in Newcastle. We had a few end-stage failing samples and one donor sample. Cris said that he had dozens of samples, including donor hearts already and was continuously adding to the collection; moreover, he was willing to supply such samples to anyone who could make good use of them.
We immediately came to an agreement to work on these heart samples with our in vitro assays, and a month later, Cris sent us 5 1-g vials each of 5 donor hearts and 5 end-stage failing hearts. These were the basis of Andrew Messer’s thesis and many publications since.
The samples that Cris provided then and later were essential for the work we did for the next 15 years. The key merits of the Sydney Heart Bank are that the material is abundant, both in quantity per heart and number of hearts, that the collection regime is of the highest quality with very prompt freezing and storing in liquid nitrogen and that it is shared with the scientific community worldwide. This last point is crucial: there are a significant number of reports on human heart tissue, but they mainly use ‘private’ tissue collections; consequently, there is no way of independently checking whether such results are valid—a fundamental requirement in any scientific investigation.
Cris’ generosity in sharing his samples is outstanding, such that his samples have become a sort of de facto standard against which others can be measured. This has been well documented in recent publications (dos Remedios et al. 2017; Lal et al. 2015; Li et al. 2019) Crucially, his heart bank contains a lot of donor heart material: for most researchers, this is the hardest to obtain and yet is necessary since we can only study the pathological human heart in comparison with a control, preferably a normal heart sample. Cris’ donor hearts are such a control, and this review will be devoted to the studies on donor heart samples since it is not generally realised how important the control is for human heart studies.
We report the results obtained with 17 different donor samples collected from 1994 to 2011 and measured from 2005 to 2015 by our standard methodology for in vitro motility and troponin I phosphorylation measurements. The donor heart sample parameters are consistent between the hearts, over time and with different operators indicating that Sydney Heart Bank donor hearts are a valid baseline control for comparison with pathological heart samples.
Materials and methods
Tissue samples were supplied by Prof. C Dos Remedios, University of Sydney, Australia. The protocols for tissue collection are well established (Lal et al. 2015), and the methods introduced at the Sydney Heart Bank—rapid freezing and storage in liquid nitrogen—have been followed by most other laboratories. Samples from the Sydney Heart Bank were shipped in liquid nitrogen and stored in liquid nitrogen for up to 11 years before use. Ethical approval was obtained from The Royal Brompton and Harefield NHS Trust, London, and St Vincent’s Hospital, Sydney. The investigation conformed with the principles outlined in the Declaration of Helsinki.
Donor myocardium was obtained from patients with brain stem death from a variety of causes who were assessed as potential heart donors, but their organs were subsequently rejected on technical grounds or because no suitable transplant recipient was found. The donors had no history of cardiac disease, a normal cardiac examination, a normal ECG and normal cardiac function on transthoracic echocardiography performed within 24 h of heart explantation. Myocardial samples were snap frozen in liquid nitrogen and stored for later analysis.
Proteins extracted from human heart donor samples were investigated in two assays. Troponin was isolated from 100 mg of human heart tissue by crushing the frozen tissue in a liquid nitrogen-cooled percussion mortar and rapidly extracting washed myofibrils. Myofibrils were dissolved in sample buffer, and the phosphospecies of troponin I were separated by phosphate affinity SDS-PAGE and identified by western blotting with an anti-cTnI monoclonal antibody as describe by Messer et al. (2009). Pure troponin was extracted from the myofibrils using an anti-cTnI antibody affinity column as described by Messer et al. (2007). Thin filaments were reconstituted with the human troponin, recombinant alpha-tropomyosin and skeletal muscle actin. The movement of thin filaments over a bed of immobilised skeletal muscle HMM and its regulation by Ca2+was visualised by the in vitro motility assay (Fraser and Marston 1995; Marston 2003; Marston et al. 1996). Ca2+-control of fraction motile and sliding speed was measured. Ca2+-sensitivity was determined by a curve fit of the data to the Hill equation. These methods were standard throughout the 12 years of this investigation.
Historic values from these assays were obtained from the PhD theses of Adam Jacques, Andrew Messer, Emma Dyer, Christopher Bayliss, Massimiliano Memo and Mary Papadaki, since these contained full details not present in their published papers, plus recent papers by Messer et al. (Bayliss 2011; Dyer 2008; Jacques 2012; Memo 2012; Messer 2007; Papadaki 2015).
Results
I found 88 measurements of Ca2+-sensitivity from 17 donor samples with accompanying measurements of troponin I phosphorylation for each sample, measured over a period of 12 years. The results are shown in Supplementary Table 1. Many samples were measured multiple times (e.g. 2.149, 7 values; 4.104, 8 values; 5.089, 9 values; 5.090, 12 values; 5.126, 8 values; 6.008, 10 values; 7.08, 8 values).
Although the cause of brain death in these patients varied, time on life support varied from 20 to 135 h and times in cardioplegia also varied, non-failing donor heart muscle samples showed very similar motility parameters and phosphorylation levels.
The variabilities between reported values do not correlate with the sample nor does it correlate with the operator. A statistical analysis of Messer’s data (Messer et al. 2007) shows that there was as much variability between 5 separate troponin preparations made from one muscle sample as between troponin made from six different muscle samples. This applies to both Ca2+-sensitivity of fraction motile and the level of TnI phosphorylation (although the latter had a smaller range of variation) as illustrated in Fig. 1. We also note that most of these samples have been used as control by other research groups measuring different properties of heart muscle as listed in Supplementary Table 1.
a Box and whisker plot of EC50 for Ca2+-activation of fraction of filaments motile measured in different donor samples by in vitro motility assay. Only the samples with 5 or more replicates are shown here (see Supplementary Table 1). The mean of all values is 0.137 μM ± .007 (SEM), 82 points. b Level of troponin I phosphorylation measured in 14 donor samples by phosphate affinity SDS-PAGE. The mean of these values is 1.59 molPi/molTnI ± 0.051 (SEM)
At the bottom of the table, we show results obtained with donor samples from other sources that were also rapidly frozen in liquid nitrogen: Ian Purcell’s sample from 1999 (Knott et al. 2002; Purcell et al. 1999) and recent samples collected by Ken Campbell, Kentucky University (Messer et al. 2016; Vikhorev et al. 2017). It is clear that these samples are similar to the Sydney Heart Bank samples when assayed in the same way.
Discussion
Donor samples have been used as controls for studies on human heart for many years on the assumption that they are uniform without objective evidence that this was so. Operationally, all researchers have found that pathological material, be it failing heart, or familial heart diseases (hypertrophic cardiomyopathy, dilated cardiomyopathy) with known mutations, have clear and reproducible differences from donor heart, implicitly indicating that the donor heart is an acceptable control.
Our extensive measurements of myofilament Ca2+-sensitivity using the same techniques with many samples over many years clearly demonstrates that donor samples from the Sydney Heart Bank do indeed have uniform properties. Therefore, it is valid to use these samples as controls for comparative experiments (Messer et al. 2007), and it is also worth noting that other laboratories have collected donor heart tissue following the protocols established by the Sydney Heart Bank and come up with similar results.
Of course, it is entirely possible that when other properties of the samples are measured, variable results might be obtained from different sample donor samples. However, most studies have used several donor samples, and no such variability has been reported. Supplementary Table 1 lists other papers that use the samples we studied, and dos Remedios et al. list many more (dos Remedios et al. 2017). There are a few objective tests of whether preservation is adequate. RNA and protein degradation is an obvious way to detect a ‘bad’ sample. A particularly sensitive test is the level of protein phosphorylation, since, counter-intuitively, if tissue is not frozen soon enough or thaws out later, the level of TnI phosphorylation increases (Cai et al. 2018).
Despite the uniformity of donor samples, the question of whether such samples are normal remains to be addressed. The definition of a normal heart is itself difficult since the heart is such a dynamic organ. The resting heart (50–70 bpm) is the nearest to a standard state as could be defined. Applying such a criterion to the Sydney Heart Bank samples would suggest they are unlikely to be normal. The cause of brain death in these patients varied, time on life support varied from 20 to 135 h and times in cardioplegia also varied (Smith 2004). The argument could be made that all these samples are abnormal and that the uniformity of properties represents a common abnormality. The subject was much debated a few years ago, but not resolved, and it seems the two sides in the argument have agreed to differ (Jweied et al. 2007; Marston and deTombe 2008): I have not found any further studies that address this question since the work of Jweid in 2007.
It is well known that subarachnoid haemorrhage, stroke and trauma all cause markedly elevated catecholamine levels, and this may be increased again at the time of organ harvest (Fitzgerald et al. 1995); therefore, our samples may have abnormally high PKA phosphorylation levels. Protocols for organ harvesting are not available for Sydney Heart Bank samples and may have varied over the years anyway. Explanted hearts are usually maintained with inotropes which would tend towards a high level of phosphorylation of TnI and MyBP-C.
The ‘normality’ of Sydney Heart Bank samples is essentially unknowable. Nevertheless, several experiments indicate that abnormal phosphorylation levels may not be an issue for Sydney Heart Bank samples. Notably, the levels of troponin I and troponin T phosphorylation we found in mouse and guinea pig heart that had been rapidly frozen immediately after schedule 1 euthanasia without stimulation are the same as in donor heart muscle samples. In all three cases, only about 60% of the PKA sites on troponin I are phosphorylated which means that adrenergic activation is not maximal. In the mice, isoprenaline was shown to initiate an inotropic response with further phosphorylation (Pi et al. 2003; Pi et al. 2002), and further PKA phosphorylation decreased Ca2+-sensitivity in both human donor samples and mouse (Hamdani et al. 2009; van der Velden et al. 2003.; Wolff et al. 1996). Thus, on the basis of these rather limited criteria, Sydney Heart Bank samples may be representative of the normal heart muscle at rest.
References
Bayliss C (2011) Dysfunction of contractile proteins in hypertrophic cardiomyopathy. Imperial College London, London
Cai W et al (2018) Temperature-sensitive sarcomeric protein post-translational modifications revealed by top-down proteomics. J Mol Cell Cardiol 122:11–22. https://doi.org/10.1016/j.yjmcc.2018.07.247
dos Remedios CG et al (2017) The Sydney Heart Bank: improving translational research while eliminating or reducing the use of animal models of human heart disease. Biophys Rev 89:1065–1011. https://doi.org/10.1007/s12551-017-0305-3
Dyer E (2008) A functional investigation of mutations associated with hypertrophic and dilated cardiomyopathy doctoral thesis. Imperial College London, London
Fitzgerald RD, Dechtyar I, Templ E, Fridrich P, Lackner FX (1995) Cardiovascular and catecholamine response to surgery in brain-dead organ donors. Anaesthesia 50:388–392. https://doi.org/10.1111/j.1365-2044.1995.tb05989.x
Fraser IDC, Marston SB (1995) In vitro motility analysis of actin-tropomyosin regulation by troponin and Ca2+: the thin filament is switched as a single cooperative unit. J Biol Chem 270:7836–7841
Hamdani N et al (2009) Myofilament dysfunction in cardiac disease from mice to men. J Muscle Res Cell Motil 29:189–201. https://doi.org/10.1007/s10974-008-9160-y
Jacques A (2012) Hypertrophic and dilated cardiomyopathies, the relationship of phenotype to genotype. Imperial College London, London
Jweied E, deTombe P, Buttrick PM (2007) The use of human cardiac tissue in biophysical research: the risks of translation. J Mol Cell Cardiol 42:722–726. https://doi.org/10.1016/j.yjmcc.2007.02.002
Knott A, Purcell IF, Marston S (2002) In vitro motility analysis of thin filaments from failing and non-failing human hearts induces slower filament sliding and higher Ca2+−sensitivity. J Mol Cell Cardiol 34:469–482. https://doi.org/10.1006/jmcc.2002.1528
Lal S et al (2015) Best practice BioBanking of human heart tissue. Biophys Rev 7:399–406. https://doi.org/10.1007/s12551-015-0182-6
Li A, Lal S, Remedios CG (2019) A step towards understanding the molecular nature of human heart failure: advances using the Sydney Heart Bank collection. Biophys Rev 11:1–4. https://doi.org/10.1007/s12551-019-00514-5
Marston S (2003) Random walks with thin filaments: application of in vitro motility assay to the study of actomyosin regulation. J Muscle Res Cell Motil 24:149–156. https://doi.org/10.1023/A:1026097313020
Marston S, deTombe P (2008) Point/counterpoint. Troponin phosphorylation and myofilament Ca2+−sensitivity in heart failure: increased or decreased? J Mol Cell Cardiol 45:603–607. https://doi.org/10.1016/j.yjmcc.2008.07.004
Marston SB, Fraser IDC, Wu B, Roper G (1996) A simple method for automatic tracking of actin filaments in the motility assay. J Muscle Res Cell Motil 17:497–506. https://doi.org/10.1007/BF00123365
Memo M (2012) Molecular mechanisms of myopathies. Imperial College London, London
Messer A (2007) Structural and functional polymorphisms of troponin in failing heart. PhD Thesis London
Messer AE, Jacques AM, Marston SB (2007) Troponin phosphorylation and regulatory function in human heart muscle: dephosphorylation of Ser23/24 on troponin I could account for the contractile defect in end-stage heart failure. J Mol Cell Cardiol 42:247–259. https://doi.org/10.1016/j.yjmcc.2006.08.017
Messer A, Gallon C, McKenna W, Elliott P, Dos Remedios C, Marston S (2009) The use of phosphate-affinity SDS-PAGE to measure the troponin I phosphorylation site distribution in human heart muscle. Proteomics Clin Appl 3:1371–1382. https://doi.org/10.1002/prca.200900071
Messer A et al (2016) Mutations in troponin T associated with hypertrophic cardiomyopathy increase Ca2+−sensitivity and suppress the modulation of Ca2+−sensitivity by troponin I phosphorylation. Arch Biochem Biophys 601:113–120. https://doi.org/10.1016/j.abb.2016.03.027
Papadaki M (2015) The importance of uncoupling of troponin I phosphorylation from Ca2+ sensitivity in the pathogenesis of cardiomyopathy. Imperial College London, London
Pi Y-Q, Kemnitz KR, Zhang D, Kranias EG, Walker JW (2002) Phosphorylation of troponin I controls cardiac twitch dynamics. Evidence from phosphorylation site mutants expressed on a troponin I-null background in mice. Circ Res 90:649–656. https://doi.org/10.1161/01.RES.0000014080.82861.5F
Pi Y, Zhang D, Kemnitz KR, Wang H, Walker JW (2003) Protein kinase C and a sites on troponin I regulate Myofilament Ca2+ sensitivity and ATPase rate in mouse myocardium. J Physiol 552:845–857. https://doi.org/10.1113/jphysiol.2003.045260
Purcell IF, Bing W, Marston SB (1999) Functional analysis of human cardiac troponin by the in vitro motility assay: comparison of adult, foetal and failing hearts. Cardiovasc Res 43:884–891. https://doi.org/10.1016/S0008-6363(99)00123-6
Smith M (2004) Physiologic changes during brain stem death—lessons for management of the organ donor. J Heart Lung Transplant 23:S217–S222. https://doi.org/10.1016/j.healun.2004.06.017
van der Velden J et al (2003) Increased Ca2+−sensitivity of the contractile apparatus in end-stage human heart failure results from altered phosphorylation of contractile proteins. Cardiovasc Res 57:37–47. https://doi.org/10.1016/S0008-6363(02)00606-5
Vikhorev PG et al (2017) Abnormal contractility in human heart myofibrils from patients with dilated cardiomyopathy due to mutations in TTN and contractile protein genes. Sci Rep 7:14829. https://doi.org/10.1038/s41598-017-13675-8
Wolff M, Buck S, Stoker S, Greaser M, Mentzer R (1996) Myofibrillar calcium sensitivity of isometric tension is increased in human dilated cardiomyopathies. J Clin Invest 98:167–176. https://doi.org/10.1172/JCI118762
Acknowledgements
We are grateful to Amy Li and Sean Lal for providing clinical and publication data from the Sydney Heart Bank.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
Ethical approval was obtained from The Royal Brompton and Harefield NHS Trust, London, and St Vincent’s Hospital, Sydney. The investigation conformed with the principles outlined in the Declaration of Helsinki.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
ESM 1
(DOCX 28 kb).
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Marston, S., Jacques, A., Bayliss, C. et al. Donor hearts in the Sydney Heart Bank: reliable control but is it ‘normal’ heart?. Biophys Rev 12, 799–803 (2020). https://doi.org/10.1007/s12551-020-00740-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12551-020-00740-2