Abstract
Background
Ingestion of button batteries occurs in about ten persons per one million persons each year, with most of them children, and one in every 1000 battery ingestions leads to serious injuries. This study aimed to describe the clinical features and outcome of ingestion or inhalation of button batteries in children spanning a decade from January, 2006 to December, 2016 at a tertiary care hospital.
Methods
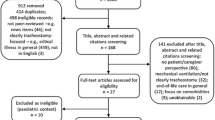
We reviewed the clinical records of children who sought treatment for inhaled or ingested button batteries at our hospital during the study period. Data on gender, age, time from ingestion to treatment, site of impaction, imaging findings, and outcomes were retrieved and analyzed.
Results
We identified 116 pediatric cases of ingestion or inhalation of button batteries. Their mean age was 26 months. The time from ingestion or inhalation of button batteries to treatment was 0.5 hours to 2 weeks. Ninety-seven (83.6%) button batteries were located in the nasal cavity, 13 (11.2%) in the gastrointestinal (GI) tract including 6 in the esophagus, and 7 in the stomach and lower GI tract, and 6 (5.2%) in the auditory tract. Twenty-one (21.6%) children with nasal button batteries had preoperative septal perforations and one (1.0%) had postoperative septal perforation. One child with esophageal button battery developed esophageal stricture and one died of sudden cardiac arrest perioperatively. One child had auditory damages in the right tympanic membrane and ossicles.
Conclusions
Inhalation or ingestion may occur in the nasal cavities, the esophagus and GI tract and the auditory tract. Prompt diagnosis and treatment are required for a satisfactory outcome and ingested or inhaled button batteries require different treatment protocols.




Similar content being viewed by others
References
Litovitz T, Whitaker N, Clark L. Preventing battery ingestions: an analysis of 8648 cases. Pediatrics. 2010;125:1178–83.
Cowan SA, Jacobsen P. Ingestion of button batteries. Epidemiology, clinical signs and therapeutic recommendations. Ugeskr Laeger. 2002;164:1204–7.
Litovitz T, Schmitz BF. Ingestion of cylindrical and button batteries: an analysis of 2382 cases. Pediatrics. 1992;89:747–57.
Centers for Disease control and Prevention. Injuries from batteries among children aged < 13 years—United States, 1995–2010. MMWR Morb Mortal Wkly Rep. 2012;61:661–6.
Buttazzoni E, Gregori D, Paoli B, Soriani N, Baldas S, Rodriguez H, et al. Symptoms associated with button batteries injuries in children: an epidemiological review. Int J Pediatr Otorhinolaryngol. 2015;79:2200–7.
Liao W, Wen G, Zhang X. Button battery intake as foreign body in Chinese children: review of case reports and the literature. Pediatr Emerg Care. 2015;31:412–5.
Leinwand K, Brumbaugh DE, Kramer RE. Button battery ingestion in children: a paradigm for management of severe pediatric foreign body ingestions. Gastrointest Endosc Clin N Am. 2016;26:99–118.
Ettyreddy AR, Georg MW, Chi DH, Gaines BA, Simons JP. Button battery injuries in the pediatric aerodigestive tract. Ear Nose Throat J. 2015;94:486–93.
Suita S, Ohgami H, Yakabe S, Nagasaki A. The fate of swallowed button batteries in children. Z Kinderchir. 1990;45:212–4.
Scholes MA, Jensen EL. Presentation and management of nasal foreign bodies at a tertiary children’s hospital in an American metro area. Int J Pediatr Otorhinolaryngol. 2016;88:190–3.
Loh WS, Leong JL, Tan HK. Hazardous foreign bodies: complications and management of button batteries in nose. Ann Otol Rhinol Laryngol. 2003;112:379–83.
Guidera AK, Stegehuis HR. Button batteries: the worst case scenario in nasal foreign bodies. N Z Med J. 2010;123:68–73.
Brumbaugh DE, Colson SB, Sandoval JA, Karrer FM, Bealer JF, Litovitz T, et al. Management of button battery-induced hemorrhage in children. J Pediatr Gastroenterol Nutr. 2011;52:585–9.
Anfang RR, Jatana KR, Linn RL, Rhoades K, Fry J, Jacobs IN. pH-neutralizing esophageal irrigations as a novel mitigation strategy for button battery injury. Laryngoscope. Laryngoscope. 2018. https://doi.org/10.1002/lary.27312.
Sharpe SJ, Rochette LM, Smith GA. Pediatric battery-related emergency department visits in the United States, 1990–2009. Pediatrics. 2012;129:1111–7.
Funding
No funding was received for this study.
Author information
Authors and Affiliations
Contributions
TH and WQL equally contributed to the conception and design of the research; ZFX contributed to the design of the research; JL contributed to the acquisition and analysis of the data; KCR and EMX contributed to the interpretation of the data; and TH and WQL drafted the manuscript. All authors critically revised the manuscript, agreed to be fully accountable for ensuring the integrity and accuracy of the work, and read and approved the final manuscript.
Corresponding author
Ethics declarations
Ethical approval
The study protocol was approved by the local ethics committee of Wuhan Children’s Hospital.
Conflict of interest
No financial or nonfinancial benefits have been received or will be received from any party related directly or indirectly to the subject of this article.
Electronic supplementary material
Below is the link to the electronic supplementary material.
12519_2018_188_MOESM1_ESM.tif
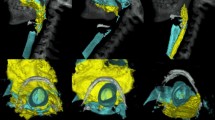
Supplementary Fig. 1 Electron nasopharyngoscope shows brown black scar in the nasal septum at one week post foreign body removal (A and B) and septal perforation at one month post foreign body removal (C) (TIFF 8023 kb)
12519_2018_188_MOESM2_ESM.tif
Supplementary Fig. 2 Chest x-ray shows extensive bilateral lung solidification with pneumothorax in a 14-month old boy (TIFF 3207 kb)
Rights and permissions
About this article
Cite this article
Huang, T., Li, WQ., Xia, ZF. et al. Characteristics and outcome of impacted button batteries among young children less than 7 years of age in China: a retrospective analysis of 116 cases. World J Pediatr 14, 570–575 (2018). https://doi.org/10.1007/s12519-018-0188-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12519-018-0188-9