Abstract
The aim was to investigate the concentrations of some per- and polyfluoroalkyl substances (PFAS) in patients with pancreatic cancer from New York, and to compare them with a group of controls from the general population of the United States. We selected 50 cases of pancreatic cancer from donors to the New York University Pancreatic Biorepository. Controls were selected from the 2017–18 National Health and Examination Survey sample (n = 167), matched to cases on age, sex, and race and ethnicity. Six PFAS were analyzed in serum samples using high performance liquid chromatography in conjunction with mass spectrometry. PFAS concentrations were categorized into tertiles to explore non-linear associations, and odds ratios (OR) were estimated using conditional logistic regression, adjusting by BMI. Most PFAS were not associated with pancreatic cancer risk. Serum perfluorohexane sulfonic acid (PFHxS) was associated with a decreased risk (OR for upper tertile = 0.24, 95% CI: 0.09, 0.67). In contrast, participants with the highest tertile of perfluoroundecanoic acid (PFUnDA) had a higher risk (OR = 2.60, 95% CI: 1.11, 6.09). Adjusting for BMI did not materially change the results. Study limitations include: in pancreatic cancer patients, blood used to measure PFAS was collected around the time of diagnosis; cases and controls could not be sampled from the same geographic location; slightly different laboratory methods were used to analyze PFAS in cases and controls. Most PFAS studied were not significantly associated with pancreatic cancer, except for PFHxS and PFUnDA, which exhibited opposite trends. Findings and limitations of the present study warrant further investigation with improved study designs and data on complex PFAS mixtures.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Increases in pancreatic cancer incidence can only partly be explained by changes in diagnostic and screening procedures, and have occurred over a timespan in which genetics cannot be invoked. This leaves environmental contributors as a promising opportunity for prevention. Yet, few studies have examined plausible, common exposures, particularly synthetic chemicals (Fernandez et al. 1994, Ilic and Ilic M 2022, Gasull et al. 2019, Porta et al. 2022, Amaral et al. 2012, Antwi et al. 2015, Barone et al. 2016, Djordjevic et al. 2019, Eriksen et al 2009).
Per- and polyfluoroalkyl compounds (PFAS) were first widely used in the late 1940s, mostly because of their high repellency to both water and oil, as well as thermal and chemical stability. Human exposure is nearly ubiquitous, with more than 100 million Americans drinking water at levels above safety thresholds suggested by laboratory research (Ackerman Grunfeld et al. 2024; Erdenesanaa 2024). Such studies reveal oxidative stress in the pancreas, dose-dependent, and associated with focal ductal hyperplasia and inflammation (National Toxicology Program, 2022). Contamination of food through contact materials and packaging is well-known (Muncke et al. 2014; Mustieles et al. 2023), and human exposure also occurs through house dust, cleaning agents, electronic devices, and other goods (Sunderland et al. 2019, Schulz et al. 2020, Lim 2023, Kannan et al. 2004, Schneider 2019, Geueke 2016, Gore et al. 2015, Cousins et al. 2022, Evich et al. 2022, Geueke et al. 2022, Scheringer 2023, ECHA (European Chemicals Agency), 2023, Berg et al. 2021).
However, studies on human cancer using PFAS biomarkers are scant (Eriksen et al. 2009, Sunderland et al. 2019, Gore et al. 2015, Bonefeld et al. 2014, Feng et al. 2022, Winquist et al. 2023). An occupational study in Minnesota revealed some positive trends for prostate cancer, but was limited in sample size (Lundin et al. 2009). In a large-scale industrial contamination area, the C8 study failed to reveal increases in pancreatic cancer, though it did for renal and testicular cancers (Barry et al. 2013). The Danish National Birth Cohort revealed positive associations with pancreatic cancer and breast cancer (Eriksen et al. 2009, Bonefeld et al. 2014). A case–cohort study in the American Cancer Society’s Cancer Prevention Study II LifeLink Cohort, suggested an inverse association between PFOA and pancreatic cancer among men (Winquist et al. 2023). These studies have methodological limitations (Winquist et al. 2023), and levels of long-chain PFAS have tended to decline with the emergence of replacement PFAS that may be as carcinogenic.
We therefore leveraged a more recent sample (2017–2021) of patients with pancreatic cancer to investigate the concentrations of some per- and polyfluoroalkyl substances (PFAS) in patients with pancreatic cancer and to compare them with a group of controls from the general population of the United States.
Methods
Study Population
Patients with pancreatic cancer (n = 50) diagnosed between 2017 and 2021 with available serum samples in the NYU Pancreatic Biorepository were selected as cases. Serum was collected before, at the time of, or as soon as possible after diagnosis (Supplemental Fig. 1). Selected cases were either stage I or II; other stages were excluded. The majority of cases had no family history of PDA (Supplemental Table 1). Mutations of the KRAS, CDKN2A, and P53 were noted in 42%, 18%, and 32% of participants, respectively. Cases with neuroendocrine pancreatic tumors (n = 5) were excluded from the primary analyses due to their pathophysiology differing from exocrine pancreatic tumors. Demographic characteristics and social and medical history were collected from clinical records. The study was approved by the NYU Grossman School of Medicine Institutional Review Board.
Forest plot of unadjusted associations of PFAS and pancreatic cancer (N = 212). *Continuous exposures are natural log transformed with units of ng/Ml except for the sum of orders of PFAS. * P-values are derived from Wald’s test. * Test for linear trend. Abbreviations: T1–tertile 1 (<34th percentile), T2-tertile2 (34th-66th percentile), T3(>66th percentile)
Controls were selected from the 2017–18 National Health and Nutrition Examination Survey (NHANES) study sample. NHANES is conducted by the Centers for Disease Control and Prevention (CDC) and aims to collect health and demographic data via interviews, physical examinations and biospecimen collections, on a nationally representative sample of approximately 5000 non-institutionalized US adults and children each year (Centers for Disease Control and Prevention (CDC) 2024a). Additional details on study design are provided elsewhere (Centers for Disease Control and Prevention 2024b). To meet inclusion criteria, controls had to be 20 years or older, have serum PFAS measurements, and no history of cancer. Controls who met criteria (n = 1459) were matched with cases on age (five year increments from 20 to 80 + years), sex, and race and ethnicity (i.e., Hispanic, Non-Hispanic White, Non-Hispanic Black, Other or Unknown). Four controls were matched to each case; two cases had three controls, four cases had two controls, and one case had one control.
After matching cases and controls on sex, age, and race and ethnicity, the study sample had a total of 212 adults (Table 1). Participants ranged from mid-30s to over 80 years of age; 55% were female; 15% were Hispanic, 15% were non-Hispanic Black, 61% were non-Hispanic White, and 9% were Other or Unknown. Smoking status and the proportion of participants with diabetes were similar between cases and controls. The median BMI was higher in controls.
PFAS
Six PFAS were measured in the serum of cases and controls and were detected in greater than 70% of participants: perfluorodecanoic acid (PFDA), perfluorohexane sulfonic acid (PFHxS), perfluorononanoic acid (PFNA), perfluorooctanoic acid (PFOA), perfluorooctane sulfonic acid (PFOS), and perfluoroundecanoic acid (PFUnDA).
Briefly, among cases PFAS were measured in the laboratory of Dr. K. Kannan, then at NYU. They were quantified using an AB SCIEX™ 5500 electrospray quadrupole tandem mass spectrometer (ESI–MS/MS: SCIEX, Framingham, MA, USA), interfaced with a Nexera X2 LC-30AD series high performance liquid chromatograpy (Shimadzu, Kyoto, Japan). The analytes were separated using an UPLC BEH C18 column (2.1 × 50 mm, 1.7 µm, Waters, Milford, MA, USA). MeOH and 0.1% w/v ammonium acetate in water were used as mobile phases. Target analytes were determined by selected reaction monitoring in negative ionization mode. Further details have been described elsewhere (Honda et al. 2018). Please see also Supplemental Methods. Measurement techniques used to detect PFAS in cases had a method limit of detection (LOD) of 0.02 ng/mL.
Among controls, PFDA, PFHxS, PFNA, linear and branched PFOA, linear and branched PFOS, and PFUnDA were measured in the National Center for Environmental Health, Organic Analytical Toxicology Branch, as part of NHANES (see section 2.1 above). They were quantified using online solid phase extraction in conjunction with high performance liquid chromatography-negative-ion TurboIonSpray ionization-tandem mass spectrometry. PFAS measurement techniques used for controls had a method LOD of 0.10 ng/mL. Further information on laboratory methods used to analyze serum samples of controls has been previously published (Center and for Environmental Health (NCHS), 2024c). See also Supplemental Methods.
To harmonize the PFAS measurement techniques of cases and controls, all cases with PFAS values below 0.10 ng/mL were considered below the LOD. PFAS values of cases below the LOD were imputed with LOD/√2 and rounded to the second decimal place to align with the handling of below LOD values in the controls dataset (National Center for Health Statistics (NCHS) 2024d). PFAS values of cases that were above the LOD were rounded to the first decimal place to match the precision of the control data. Finally, due to the low detection of branched PFOS and PFOA isomers, when adding the linear and branched isomers of the controls to obtain the total serum concentrations of PFOS and PFOA, values below the LOD were imputed with a random value between 0.1 and 0 so as to not add a static value (e.g., LOD/√2). The total PFOS and PFOA summations were then rounded to the first decimal place to match the precision of the other PFAS measurements.
PFAS concentrations were converted into tertiles based on the distribution of the analytic sample to explore possible non-linear trends. To estimate total PFAS exposure, the sum of all six PFAS concentrations (sum of PFAS) and the sum of all six PFAS tertile rankings (sum of orders) were calculated. Sum of PFAS and the sum of orders of PFAS were additionally converted into tertiles. Continuous individual PFAS and sum of PFAS concentrations were natural log-tranformed to account for right-skew in the data.
Statistical Analyses
Statistical comparisons between characteristics of cases and controls were conducted, including Chi-squared tests for categorical covariates and Mann–Whitney’s U tests for continuous covariates. For variables with categories containing less than five participants, Fisher’s exact test was used. Both the distributions of PFAS concentrations including their geometric means and percent detection and the Spearman’s rank correlation coefficients between each PFAS concentration were calculated for cases and controls to explore possible differences in PFAS exposure between the groups.
We used conditional logistic regression models to estimate the association between pancreatic cancer and the natural log-transformed individual PFAS concentrations and sum of PFAS, as well as the sum of orders of PFAS. PFAS exposures were modeled as tertiles and continuously. As BMI has been associated with PFAS concentrations in some studies and is a risk factor for pancreatic cancer (Jacobs et al. 2020; Qi et al. 2020), we additionally conducted the analyses controlling for continuous BMI collected at time of blood draw. For associations between PFAS tertiles and pancreatic cancer that appeared to have a linear trend, a test for linear trend was performed. For those with no apparent trend, the total effect of the categorized PFAS on the regression model was tested. P-values were estimated with Wald’s test. Statistical tests were two-tailed and we used a threshold of 0.05 to evaluate statistical significance. All analyses were conducted using SAS version 9.4 (Cary, NC).
Results
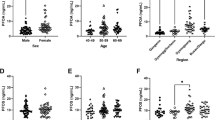
PFAS concentrations and the percent of samples with detectable PFAS quantities were similar between cases and controls (Table 2). PFOS and PFOA were detected in all samples, while PFUnDA, the least detected, was found in approximately 70% of cases and controls. Spearman’s rank correlation coefficients between PFAS were similar among cases and controls, with PFDA and PFUnDA having the highest coefficients, and PFHxS and PFDA having the lowest among cases and second lowest among controls (Supplementary Tables 2A and 2B).
PFHxS exposure was inversely associated with pancreatic cancer, with one unit increase in natural log-transformed PFHxS decreasing the odds of pancreatic cancer by 41% (Odds Ratio [OR] = 0.59, 95% Confidence Interval [CI]: 0.37, 0.92). Similarly, the results of the regression using categorized PFHxS showed that participants in the highest tertile (67th-100th percentile) had significantly lower odds of pancreatic cancer (OR = 0.24, 95% CI: 0.09, 0.67) compared to the lowest tertile (0th-33rd percentile) of PFHxS exposure (Fig. 1). In contrast, participants in the highest tertile of PFUnDA concentration had 2.60 (95% CI: 1.11, 6.09) times the odds of the lowest tertile of being diagnosed with pancreatic cancer.
There were no associations between pancreatic cancer and the continuous or categorized concentrations of PFDA, PFNA, PFOA, PFOS, and summary measures of PFAS. Associations were similar after adjustment for BMI except for the association of PFOA with pancreatic cancer (Fig. 2). Participants in the second tertile (34th-66th percentile) of PFOA exposure had a 60% (OR = 0.40, 95% CI: 0.17, 0.99) lower odds of being diagnosed with pancreatic cancer compared to the first tertile of exposure after adjusting for BMI.
Forest plot of associations of PFAS and pancreatic cancer adjusted for BMI (N = 207). *Continuous exposures are natural log transformed with units of ng/Ml except for the sum of orders of PFAS. *P-values are derived from Wald’s test. *Test for linear trend. Abbreviations: T1–tertile 1 (34th percentile), T2-tertile 2 (34th-66th percentile), T3-tertile 3 (66th percentile)
Discussion
In this new case–control study of long-chain PFAS and pancreatic cancer we found that most PFAS were not associated with pancreatic cancer risk. While PFHxS was associated with a decreased risk, participants with the highest tertile of PFUnDA had a higher risk. Results are unlikely to be confounded by BMI.
As mentioned above, the C8 study reported no associations between PFAS and pancreatic cancer,(Barry et al. 2013), while the Danish National Birth Cohort did (Eriksen et al. 2009, Bonefeld et al. 2014). The LifeLink Cohort suggested an inverse association between PFOA and pancreatic cancer among men (Winquist et al. 2023) A decreased risk associated to PFHxS concentrations was previously observed for breast cancer in the Danish cohort-nested case–control study: for the 4th versus 1st quintiles the RR was 0.38 (95% CI: 0.20–0.70)] (Bonefeld et al. 2014).
In the present study, the shortest-chain sulfonate was associated with a decreased risk, and the longest-chain carboxylate was potentially associated with an increased risk. Obviously, we are not reporting on an in vitro laboratory experiment, not on an experiment with animals, but on pancreatic cancer in real human beings who live under usual conditions; e.g., exposed to a large variety of PFAS mixtures. Therefore, we must be cautious before we speculate on possible biological mechanisms of just two PFAS, beyond what was written in previous publications. We think that in this study the functional groups or the chain lengths do not particularly suggest pathways for their impact on biological mechanisms in humans with pancreatic cancer.
The study has five limitations:
-
1.
In pancreatic cancer patients, blood used to measure PFAS was collected around the time of diagnosis, thus raising the possibility of disease progression bias, a form of reverse causation (Gasull et al. 2019).
-
2.
Cases and controls could not be sampled from the same geographic location (although NHANES has geographic data on its participants, the information is restricted); as both the incidence of pancreatic cancer and exposure to PFAS, particularly via groundwater, vary by region, (Sunderland et al. 2019, National Cancer Institute, State cancer profiles 2016, Cavalier et al. 2023) confounding, from risk factors that are location specific may remain in our analyses, and matching by geographic area might unveil differences in PFAS levels between cases and controls that are not apparent in our data set.
-
3.
Slightly different laboratory methods were used to analyze PFAS in cases and controls.
-
4.
While a large number of PFAS may contaminate humans, the study analyzed only long-chain PFAS; and
-
5.
Some comparisons suffered from low precision due to the small number of participants.
While pondering these limitations we should also keep in mind that: (1) we were measuring serum concentrations, which integrate all sources of exposure; and (2) our study did not aim to analyze such sources.
Therefore, methods of subsequent studies should be improved in the areas mentioned above (Gasull et al. 2019, Porta el al. 2022). For instance, studies should be based on pancreatic cancer cases whose blood samples were drawn as many years as possible before diagnosis (e.g., in a case–control study nested in a prospective cohort that established a biobank at baseline). The extended follow-up from blood draw that such cases would have, would also allow to estimate risk during the corresponding, long period. International consortia should also be able to analyze larger samples from diverse populations, and to assess the effects of mixtures of prevalent PFAS and other contaminants (Gasull et al. 2019, Cavalier et al. 2023, Porta el al. 2001).
Concentrations of PFHxS and PFCAs with 9–14 carbons in human serum have not decreased concomitantly with PFOS, PFOA and their precursors. No change and some increases in exposures to these compounds have been observed across populations. For example, significant increases in PFNA, PFDA, and PFUnDA and no change in PFHxS was observed in Swedish and Danish women (Sunderland el al. 2019, Glynn et al. 2015, Bjerregaard-Olesen et al. 2016). Similarly, no changes in PFDA and PFUnDA concentrations were observed in NHANES participants (National Center for Health Statistics (NCHS) 2024a, b). Despite the decline of long-chain PFAS concentrations observed in some populations, we detected PFOS and PFOA in all our study participants, and they showed the highest concentrations.
As long-chain PFAS have been increasingly subjected to regulatory actions in some areas worldwide, their concentrations are decreasing in some populations (Olsen et al. 2017; Göckener et al. 2020). Furthermore, short chain (less than 7 perfluorinated C atoms), ultra-short chain (less than 4 C perfluorinated atoms), and novel organofluorine chemicals, such as perfluoroalkyl ether carboxylic acids (PFECAs), are being increasingly used as replacements. These chemicals, along with precursors like fluorotelomers alcohols and polyfluoroalkyl phosphate esters, should be considered in future etiologic and biomonitoring studies to ensure a more comprehensive assessment of human exposure to PFAS.
Conclusions
Some of our findings provide tentative reassurance that PFAS may not increase pancreatic cancer risk; yet others raise concerns that PFAS may increase such risk. Therefore, findings and limitations of the present study warrant conducting further studies with improved designs.
Data availability
Data will be made available upon reasonable request.
Abbreviations
- BMI:
-
Body mass index
- CI:
-
Confidence interval
- LOD:
-
Limit of detection
- LOQ:
-
Limit of quantification
- OR:
-
Odds ratio
- PFAS:
-
Per- and polyfluoroalkyl substances
- PFOA:
-
Perfluorooctanoic acid
- PFDA:
-
Perfluorodecanoic acid
- PFHxS:
-
Perfluorohexane sulfonate
- PFNA:
-
Perfluorononanoic acid
- PFOS:
-
Perfluorooctane sulfonate
- PFUnDA:
-
Perfluoroundecanoic acid
References
Ackerman Grunfeld D, Gilbert D, Hou J et al (2024) Underestimated burden of per-and polyfluoroalkyl substances in global surface waters and groundwaters. Nat Geosci. https://doi.org/10.1038/s41561-024-01402-8
Amaral AFS, Porta M, Silverman DT et al (2012) Pancreatic cancer risk and levels of trace elements. Gut 61:1583–1588
Antwi SO, Eckert EC, Sabaque CV et al (2015) Exposure to environmental chemicals and heavy metals, and risk of pancreatic cancer. Cancer Causes Control 26:1583–1591
Barone E, Corrado A, Gemignani F, Landi S (2016) Environmental risk factors for pancreatic cancer: an update. Arch Toxicol 90:2617–2642
Barry V, Winquist A, Steenland K (2013) Perfluorooctanoic acid (PFOA) exposures and incident cancers among adults living near a chemical plant. Environ Health Perspect 121(11–12):1313–1318. https://doi.org/10.1289/ehp.1306615
Berg V, Sandanger TM, Hanssen L, Rylander C, Nøst TH (2021) Time trends of perfluoroalkyl substances in blood in 30-year old Norwegian men and women in the period 1986–2007. Environ Sci Pollut Res Int 28:43897–43907
Bjerregaard-Olesen C, Bach CC, Long M, Ghisari M, Bossi R, Bech BH et al (2016) Time trends of perfluorinated alkyl acids in serum from danish pregnant women 2008–2013. Environ Int 91:14–21
Bonefeld-Jorgensen EC, Long M, Fredslund SO, Bossi R, Olsen J (2014) Breast cancer risk after exposure to perfluorinated compounds in danish women: a case-control study nested in the danish national birth cohort. Cancer Causes Control 25:1439–1448
Cavalier H, Trasande L, Porta M (2023) Exposures to pesticides and risk of cancer: evaluation of recent epidemiological evidence in humans, and paths forward. Int J Cancer 152:879–912. https://doi.org/10.1002/ijc.34300
Cousins IT, Johansson JH, Salter ME, Sha B, Scheringer M (2022) Outside the safe operating space of a new planetary boundary for per- and polyfluoroalkyl substances (PFAS). Environ Sci Technol 56:11172–11179. https://doi.org/10.1021/acs.est.2c02765
Djordjevic VR, Wallace DR, Schweitzer A et al (2019) Environmental cadmium exposure and pancreatic cancer: evidence from case control, animal and in vitro studies. Environ Int 128:353–361
ECHA (european chemicals agency), 2023.ECHA publishes PFAS restriction proposal. ECHA/NR/23/04. https://echa.europa.eu/-/echa-publishes-pfas-restriction-proposal.
Erdenesanaa D. PFAS ‘Forever chemicals’ are pervasive in water worldwide, study finds. New York Times 2024, April 9, Section A, page 5. https://www.nytimes.com/2024/04/08/climate/pfas-forever-chemicals-water.html
Eriksen KT, Sørensen M, McLaughlin JK et al (2009) Perfluorooctanoate and perfluorooctanesulfonate plasma levels and risk of cancer in the general Danish population. J Natl Cancer Inst 101:605–609
Evich MG, Davis MJB, McCord JP et al (2022) Per- and polyfluoroalkyl substances in the environment. Science 375(6580):9065. https://doi.org/10.1126/science.abg9065
Feng Y, Bai Y, Lu Y et al (2022) Plasma perfluoroalkyl substance exposure and incidence risk of breast cancer: a case-cohort study in the Dongfeng-Tongji cohort. Environ Pollut 306:119345. https://doi.org/10.1016/j.envpol.2022.119345
Fernandez E, La Vecchia C, Porta M, Negri E, Lucchini F, Levi F (1994) Trends in pancreatic cancer mortality in Europe, 1955–1989. Int J Cancer 57:786–792
Gasull M, Pumarega J, Kiviranta H et al (2019) Methodological issues in a prospective study on plasma concentrations of persistent organic pollutants and pancreatic cancer risk within the EPIC cohort. Environ Res 169:417–433
Geueke B (2016) Dossier: Per- and polyfluoroalkyl substances (PFASs). Zürich: food packaging forum. https://www.foodpackagingforum.org/fpf-2016/wp-content/uploads/2016/07/FPF_Dossier10_PFASs.pdf.
Geueke B, Groh KJ, Maffini MV et al (2022) Systematic evidence on migrating and extractable food contact chemicals: most chemicals detected in food contact materials are not listed for use. Critical Rev Food Sci Nutr 63(28):9425–9435.https://doi.org/10.1080/10408398.2022.2067828
Glynn A, Benskin J, Lignell S et al. (2015) Temporal trends of perfluoroalkyl substances in pooled serum samples from first-time mothers in Uppsala 1997–2014. Report to the Swedish EPA, 2015.
Göckener B, Weber T, Rüdel H et al (2020) Human biomonitoring of per-and polyfluoroalkyl substances in German blood plasma samples from 1982 to 2019. Environ Int 145:106123. https://doi.org/10.1016/j.envint.2020.106123
Gore AC, Chappell VA, Fenton SE et al (2015) EDC-2: The endocrine society’s second scientific statement on endocrine-disrupting chemicals. Endocr Rev 36:E1–E150. https://doi.org/10.1210/er.2015-1010
Honda M, Robinson M, Kannan K (2018) A rapid method for the analysis of perfluorinated alkyl substances in serum by hybrid solid-phase extraction. Environ Chem (online) 15(1):92–99
Ilic I, Ilic M (2022) International patterns in incidence and mortality trends of pancreatic cancer in the last three decades: a joinpoint regression analysis. World J Gastroenterol 28:4698–4715
Jacobs EJ, Newton CC, Patel AV et al (2020) The association between body mass index and pancreatic cancer: variation by age at body mass index assessment. Am J Epidemiol; 189: 108–115. https://academic.oup.com/aje/article/189/2/108/5584410.
Kannan K, Corsolini S, Falandysz J et al (2004) Perfluorooctanesulfonate and related fluorochemicals in human blood from several countries. Environ Sci Technol 38:4489–4495. https://doi.org/10.1021/es0493446
Lim X (2023) Could the world go PFAS-free? Proposal to ban ‘forever chemicals’ fuels debate. Nature 620:24–27. https://doi.org/10.1038/d41586-023-02444-5
Lundin JI, Alexander BH, Olsen GW, Church TR (2009) Ammonium perfluorooctanoate production and occupational mortality. Epidemiology 20:921–928
Muncke J, Myers JP, Scheringer M, Porta M (2014) Food packaging and migration of food contact materials: will epidemiologists rise to the neotoxic challenge? J Epidemiol Community Health 68:592–594. https://doi.org/10.1136/JECH-2013-202593
Mustieles V, Arrebola JP, Porta M (2023) From old pollutants to the regulation of bisphenol A: Lessons learned for health promotion and disease prevention. Prev Med 169:107460. https://doi.org/10.1016/j.ypmed.2023.107460
National Cancer Institute. State cancer profiles. Incidence rates by State. Pancreas cancer, 2016–2020. https://statecancerprofiles.cancer.gov/map/map.withimage.php?00&state&001&040&00&0&01&0&1&5&0#results
National Center for Environmental Health Statistics (NCHS) (2024c). Laboratory procedure manual. analytes: perfluoroalkyl and polyfluoroalkyl substances. NHANES 2017-2018. https://wwwn.cdc.gov/nchs/data/nhanes/2017-2018/labmethods/PFAS-J-MET-508.pdf
National Center for Environmental Health Statistics (NCHS), Centers for Disease Control and Prevention (CDC) (2024a). National Health and Nutrition Examination Survey (NHANES). https://www.cdc.gov/nchs/nhanes/about_nhanes.htm.
National Center for Health Statistics (NCHS) 2024d. Centers for Disease Control and Prevention (CDC). NHANES 2017–2018 Laboratory Data Overview. https://wwwn.cdc.gov/nchs/nhanes/continuousnhanes/overviewlab.aspx?BeginYear=2017
National Center for Health Statistics (NCHS), Centers for Disease Control and Prevention (CDC) (2024b). NHANES 2017–2018 overzview. https://wwwn.cdc.gov/nchs/nhanes/continuousnhanes/overview.aspx?BeginYear=2017, https://www.cdc.gov/exposurereport/data_tables.html.
National Toxicology Program, Department of Health and Human Services. Per- and Polyfluoroalkyl Substances (PFAS). TOX-97. Toxicity studies of perfluoroalkyl carboxylates administered by gavage to Hsd: Sprague Dawley SD rats (Revised). July 2022. https://ntp.niehs.nih.gov/publications/reports/tox/000s/tox097, https://ntp.niehs.nih.gov/whatwestudy/topics/pfas#:~:text=Completed-,Findings%3A,male%20rats%20with%20lifetime%20exposure.
Olsen GW, Mair DC, Lange CC, Harrington LM, Church TR, Goldberg CL et al (2017) Per- and polyfluoroalkyl substances (PFAS) in American Red Cross adult blood donors, 2000–2015. Environ Res 157:87–95. https://doi.org/10.1016/j.envres.2017.05.013
Porta M (2001) Role of organochlorine compounds in the etiology of pancreatic cancer: a proposal to develop methodological standards. Epidemiology 12:272–276
Porta M, Gasull M, Pumarega J et al (2022) Plasma concentrations of persistent organic pollutants and pancreatic cancer risk. Int J Epidemiol 51:479–490. https://doi.org/10.1093/ije/dyab115
Qi W, Clark JM, Timme-Laragy AR, Park Y (2020) Per- and Polyfluoroalkyl Substances and obesity, Type 2 diabetes and non-alcoholic fatty liver disease: a review of epidemiologic findings. Toxicol Environ Chem 102 (1–4): 1–36. https://doi.org/10.1080/02772248.2020.1763997. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7723340/
Scheringer M (2023) Innovate beyond PFAS. Science 381:251–251. https://doi.org/10.1126/science.adj7475
Schneider J. PFAS – the ‘forever chemicals’. Invisible threats from persistent chemicals. CHEM Trust, 2019. https://chemtrust.org/pfasbrief/.
Schulz K, Silva MR, Klaper R (2020) Distribution and effects of branched versus linear isomers of PFOA, PFOS, and PFHxS: A review of recent literature. Sci Total Environ 733:139186
Sunderland EM, Hu XC, Dassuncao C, et al (2019) A review of the pathways of human exposure to poly-and perfluoroalkyl substances (PFASs) and present understanding of health effects. J Expo Sci Environ Epidemiol 29:131–147. https://doi.org/10.1038/s41370-018-0094-1
Winquist A, Hodge JM, Diver WR, et al (2023) Case-cohort study of the association between PFAS and selected cancers among participants in the American cancer society’s cancer prevention study ii lifelink cohort. Environ Health Perspect 131(12):127007. https://doi.org/10.1289/EHP13174
Acknowledgements
The authors gratefully acknowledge statistical assistance provided by Yuyan Wang. They also thank Kurunthachalam Kannan, Morgan Robinson, Sunmi Lee, José Pumarega, Laura Campi, and Vittorio Albergamo for scientific and technical assistance.
Funding
Open Access Funding provided by Universitat Autonoma de Barcelona. The work was supported in part by research pilot funds from NYU Langone Center for the Investigation of Environmental Hazards.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no known competing financial interests or personal relationships that could have appeared to influence the work reported in this paper.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Long, S., Porta, M., Yang, J. et al. Concentrations of Per-and Polyfluoroalkyl Substances (PFAS) and Pancreatic Cancer: A Case–Control Study in New York. Expo Health (2024). https://doi.org/10.1007/s12403-024-00661-5
Received:
Revised:
Accepted:
Published:
DOI: https://doi.org/10.1007/s12403-024-00661-5