Abstract
Background
The glucagon-like peptide-1 analog liraglutide increases heart rate and may be associated with more cardiac events in chronic heart failure (CHF) patients. We studied whether this could be ascribed to effects on myocardial glucose uptake (MGU), myocardial blood flow (MBF) and MBF reserve (MFR).
Methods and Results
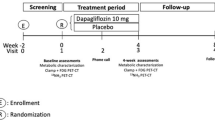
CHF patients with left ventricular ejection fraction ≤45% and without type 2 diabetes were randomized to liraglutide (N = 18) 1.8 mg once daily or placebo (N = 18) for 24 weeks in a double-blinded design. Changes in MGU during an oral glucose tolerance test (OGTT) and changes in MBF and MFR from baseline to follow-up were measured quantitatively by 18F-FDG and 15O-H2O positron emission tomography. Compared with placebo, liraglutide reduced weight (P = 0.03), HbA1c (P = 0.03) and the 2-hour glucose value during the OGTT (P = 0.004). Despite this, changes in MGU (P = 0.98), MBF (P = 0.76) and MFR (P = 0.89) from baseline to follow-up did not differ between groups. Furthermore, there was no association between the level of insulin resistance at baseline and changes in MGU in patients treated with liraglutide.
Conclusion
Liraglutide did not affect MGU, MBF, or MFR in non-diabetic CHF patients. Any potential increase in cardiac events in these patients seems not to involve changes in MGU, MBF, or MFR.
Trial Registration
Trial registry: http://www.ClinicalTrials.org. Identifier: NCT01472640. Url: https://clinicaltrials.gov/ct2/show/NCT01472640?term=NCT01472640&rank=1




Similar content being viewed by others
Abbreviations
- CHF:
-
Chronic heart failure
- HEC:
-
Hyperinsulinemic-euglycemic clamp
- LVEF:
-
Left ventricular ejection fraction
- MGU:
-
Myocardial glucose uptake
- MBF:
-
Myocardial blood flow
- MFR:
-
Myocardial flow reserve
- OGTT:
-
Oral glucose tolerance test
- PTI:
-
Perfusable tissue index
- WMS:
-
Wall motion score
References
Egan JM, Meneilly GS, Habener JF, Elahi D. Glucagon-like peptide-1 augments insulin-mediated glucose uptake in the obese state. J Clin Endocrinol Metab. 2002;87:3768-73.
Bhashyam S, Fields AV, Patterson B, Testani JM, Chen L, Shen YT, et al. Glucagon-like peptide-1 increases myocardial glucose uptake via p38 MAP kinase mediated, nitric oxide dependent mechanisms in conscious dogs with dilated cardiomyopathy/clinical perspective,Circulation. Heart Fail. 2010;3:512-21.
Dokken BB, Hilwig WR, Teachey MK, Panchal RA, Hubner K, Allen D, et al. Glucagon-like peptide-1 (GLP-1) attenuates post-resuscitation myocardial microcirculatory dysfunction. Resuscitation. 2010;81:755-60.
Zhao T, Parikh P, Bhashyam S, Bolukoglu H, Poornima I, Shen YT, et al. Direct effects of glucagon-like peptide-1 on myocardial contractility and glucose uptake in normal and postischemic isolated rat hearts. J Pharmacol Exp Ther. 2006;317:1106-13.
Gejl M, Lerche S, Mengel A, Møller N, Bibby BM, Smidt K, et al. Influence of GLP-1 on myocardial glucose metabolism in healthy men during normo- or hypoglycemia. PLoS ONE. 2014;9:e83758.
Gejl M, Søndergaard HM, Stecher C, Bibby BM, Møller N, Bøtker HE, et al. Exenatide alters myocardial glucose transport and uptake depending on insulin resistance and increases myocardial blood flow in patients with type 2 diabetes. J Clin Endocrinol Metab. 2012;97(7):E1165-9.
Lepore JJ, Olson E, Demopoulos L, Haws T, Fang Z, Barbour AM, et al. Effects of the novel long-acting GLP-1 agonist, albiglutide, on cardiac function, cardiac metabolism, and exercise capacity in patients with chronic heart failure and reduced ejection fraction. JACC. 2016;4(7):559-66.
Subaran SC, Sauder MA, Chai W, Jahn LA, Fowler DE, Aylor KW, et al. GLP-1 at physiological concentrations recruits skeletal and cardiac muscle microvasculature in healthy humans. Clin Sci (Lond). 2014;127(3):163-70.
Moberly SP, Mather KJ, Berwick ZC, Owen MK, Goodwill AG, Casalini ED, et al. Impaired cardiometabolic responses to glucagon-like peptide 1 in obesity and type 2 diabetes mellitus. Basic Res Cardiol. 2013;108(4):1-15.
Faber R, Zander M, Pena A, Michelsen MM, Mygind ND, Prescott E. Effect of the glucagon-like peptide-1 analogue liraglutide on coronary microvascular function in patients with type 2 diabetes - a randomized, single-blinded, cross-over pilot study. Cardiovasc Diabetol. 2015;14:41.
Jorsal A, Kistorp C, Holmager P, Tougaard RS, Nielsen R, Hänselmann A, et al. Effect of liraglutide, a glucagon-like peptide-1 analogue, on left ventricular function in stable chronic heart failure patients with and without diabetes (LIVE) - a multicentre, double-blind, randomised, placebo-controlled trial. Eur J Heart Fail. 2016;19(1):69-77.
Margulies KB, Hernandez AF, Redfield MM. Effects of liraglutide on clinical stability among patients with advanced heart failure and reduced ejection fraction: A randomized clinical trial. JAMA. 2016;316:500-8.
Marso SP, Daniels GH, Brown-Frandsen K, Kristensen P, Mann JFE, Nauck MA, et al. Liraglutide and cardiovascular outcomes in type 2 diabetes. N Engl J Med. 2016;375:311-22.
Kofoed K, Carstensen S, Hove J, Freiberg J, Bangsgaard R, Holm S, et al. Low whole-body insulin sensitivity in patients with ischaemic heart disease is associated with impaired myocardial glucose uptake predictive of poor outcome after revascularisation. Eur J Nucl Med. 2002;29(8):991-8.
Majmudar MD, Murthy VL, Shah RV, Kolli S, Mousavi N, Foster C, et al. Quantification of coronary flow reserve in patients with ischaemic and non-ischaemic cardiomyopathy and its association with clinical outcomes. Eur Heart J. 2015;16(8):900-9.
Jorsal A, Wiggers H, Holmager P, Nilsson B, Nielsen R, Boesgaard TW, et al. A protocol for a randomised, double-blind, placebo-controlled study of the effect of LIraglutide on left VEntricular function in chronic heart failure patients with and without type 2 diabetes (The LIVE Study). BMJ Open. 2014;4:e004885.
Nielsen R, Nørrelund H, Kampmann U, Kim WY, Ringgaard S, Schär M, et al. Failing heart of patients with type 2 diabetes mellitus can adapt to extreme short-term increases in circulating lipids and does not display features of acute myocardial lipotoxicity. Circulation. 2013;6:845-52.
Wiggers H, Bøttcher M, Nielsen TT, Gjedde A, Bøtker HE. Measurement of myocardial glucose uptake in patients with ischemic cardiomyopathy: Application of a new quantitative method using regional tracer kinetic information. J Nucl Med. 1999;40:1292-300.
Harms H, Knaapen P, de Haan S, Halbmeijer R, Lammertsma A, Lubberink M. Automatic generation of absolute myocardial blood flow images using [15O]H2O and a clinical PET/CT scanner. Eur J Nucl Med Mol Imaging. 2011;38(5):930-9.
Rischpler C, Langwieser N, Souvatzoglou M, Batrice A, van Marwick S, Snajberk J, et al. PET/MRI early after myocardial infarction: Evaluation of viability with late gadolinium enhancement transmurality vs. 18F-FDG uptake. Eur Heart J. 2015;16:661-9.
Nielsen R, Jorsal A, Iversen P, Tolbod L, Bouchelouche K, Sørensen J, et al. Heart failure patients with prediabetes and newly diagnosed diabetes display abnormalities in myocardial metabolism. J Nucl Cardiol. 2016;. doi:10.1007/s12350-016-0622-0.
Knaapen P, Boellaard R, Götte MJW, Dijkmans PA, van Campen LMC, de Cock CC, et al. Perfusable tissue index as a potential marker of fibrosis in patients with idiopathic dilated cardiomyopathy. J Nucl Med. 2004;45(8):1299-304.
Marinho NVS, Keogh BE, Costa DC, Lammerstma AA, Ell PJ, Camici PG. Pathophysiology of chronic left ventricular dysfunction: New insights from the measurement of absolute myocardial blood flow and glucose utilization. Circulation. 1996;93:737-44.
Kaufmann PA, Gnecchi-Ruscone T, Yap JT, Rimoldi O, Camici PG. Assessment of the reproducibility of baseline and hyperemic myocardial blood flow measurements with 15O-labeled water and PET. J Nucl Med. 1999;40(11):1848-56.
Boudina S, Abel ED. Mitochondrial uncoupling: A key contributor to reduced cardiac efficiency in diabetes. Physiology. 2006;21:250-8.
Nikolaidis LA, Elahi D, Shen YT, Shannon RP. Active metabolite of GLP-1 mediates myocardial glucose uptake and improves left ventricular performance in conscious dogs with dilated cardiomyopathy. Am J Physiol. 2005;289:H2401-8.
Vyas AK, Yang KC, Woo D, Tzekov A, Kovacs A, Jay PY, et al. Exenatide improves glucose homeostasis and prolongs survival in a murine model of dilated cardiomyopathy. PLoS ONE. 2011;6(2):e17178.
Aravindhan K, Bao W, Harpel MR, Willette RN, Lepore JJ, Jucker BM. Cardioprotection resulting from glucagon-like peptide-1 administration involves shifting metabolic substrate utilization to increase energy efficiency in the rat heart. PLoS ONE. 2015;10(6):e0130894.
Egstrup M, Schou M, Gustafsson I, Kistorp CN, Hildebrandt PR, Tuxen CD. Oral glucose tolerance testing in an outpatient heart failure clinic reveals a high proportion of undiagnosed diabetic patients with an adverse prognosis. Eur J Heart Fail. 2011;13(3):319-26.
Lautamäki R, Airaksinen KEJ, Seppänen M, Toikka J, Luotolahti M, Ball E, et al. Rosiglitazone improves myocardial glucose uptake in patients with type 2 diabetes and coronary artery disease. Diabetes. 2005;54:2787-94.
Marathe CS, Rayner CK, Jones KL, Horowitz M. Relationships between gastric emptying, postprandial glycemia, and incretin hormones. Diabetes Care. 2013;36(5):1396-405.
Ban K, Noyan-Ashraf MH, Hoefer J, Bolz SS, Drucker DJ, Husain M. Cardioprotective and vasodilatory actions of glucagon-like peptide 1 receptor are mediated through both glucagon-like peptide 1 receptor dependent and independent pathways. Circulation. 2008;117:2340-50.
Wang D, Luo P, Wang Y, Li W, Wang C, Sun D, et al. Glucagon-like peptide-1 protects against cardiac microvascular injury in diabetes via a cAMP/PKA/Rho-dependent mechanism. Diabetes. 2013;62:1697.
Ke J, Liu Y, Yang J, Lu R, Tian Q, Hou W, et al. Synergistic effects of metformin with liraglutide against endothelial dysfunction through GLP-1 receptor and PKA signalling pathway. Sci Rep. 2017;7:41085.
Bøttcher M, Refsgaard J, Gøtzsche O, Andreasen F, Toftegaard NT. Effect of carvedilol on microcirculatory and glucose metabolic regulation in patients with congestive heart failure secondary to ischemic cardiomyopathy. Am J Cardiol. 2002;89(12):1388-93.
Disclosures
Anders Jorsal and Lise Tarnow hold shares in Novo Nordisk A/S. Caroline Kistorp has been a principal or sub-investigator for the following companies: MSD, Novo Nordisk, Novartis, GSK and Astra Zeneca, and has participated in advisory boards for MSD and Astra Zeneca and Novo Nordisk. Henrik Wiggers has been a principal or sub-investigator in studies involving the following pharmaceutical companies: MSD, Bayer, Daiichi-Sankyo, Novartis, Novo Nordisk, Sanofi-Aventis and Pfizer. Ida Gustafsson has been principal or sub-investigator in studies involving the following pharmaceutical companies: Novartis, Janssen, GSK, MSD and Astra-Zeneca and has participated in an advisory board meeting at Boehringer-Ingelheim and Novo Nordisk. Lise Tarnow has conducted studies with, served as a consultant for and is a member of advisory boards for Novo Nordisk. The authors declare no other conflicts of interests.
Author information
Authors and Affiliations
Corresponding author
Additional information
Funding
The study was investigator-initiated and investigator-designed. The investigators received an unrestricted grant from Novo Nordisk A/S for the LIVE study, but the company was not involved in data collection, study management, analysis, or interpretation of data; nor in preparation, approval and the decision to submit the present manuscript.
All editorial decisions for this article, including selection of reviewers and the final decision, were made by guest editor Robert Gropler, MD
Rights and permissions
About this article
Cite this article
Nielsen, R., Jorsal, A., Iversen, P. et al. Effect of liraglutide on myocardial glucose uptake and blood flow in stable chronic heart failure patients: A double-blind, randomized, placebo-controlled LIVE sub-study. J. Nucl. Cardiol. 26, 585–597 (2019). https://doi.org/10.1007/s12350-017-1000-2
Received:
Revised:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12350-017-1000-2