Abstract
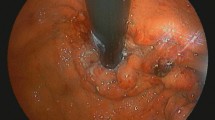
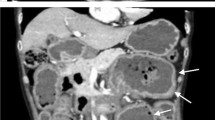
Most adult intussusceptions are secondary to various pathological conditions that serve as a lead point. Because of their serious nature, intussusceptions often require emergency surgery. We report a surgical case of amyloidosis associated with intussusception, probably due to polypoid protrusions and bleeding tendencies. An 80-year-old man with abdominal pain was suspected of having jejunal intussusception on computed tomography. He had been prescribed warfarin for atrial fibrillation, and excessive anticoagulation was observed with a prolonged prothrombin time/international normalized ratio of 5.44 at presentation. After the excessive anticoagulation was resolved, emergency surgery was performed. The intussuscepted jejunum was resected, and a 7 cm long dark-red pedunculated polyp was identified as the lead point, which was accompanied by multiple small pedunculated polyps. Histopathological examination showed that these were all hemorrhagic polyps. Amyloid depositions were observed in the muscularis mucosae, submucosa, and the walls of the blood vessels. Immunohistochemical analysis revealed immunoglobulin light chain amyloidosis. This case is informative to discuss the clinical sequelae of gastrointestinal amyloid deposition.




Similar content being viewed by others
References
Weilbaecher D, Bolin JA, Hearn D, et al. Intussusception in adults. Review of 160 cases. Am J Surg. 1971;121:531–5.
Stubenbord WT, Thorbjarnarson B. Intussusception in adults. Ann Surg. 1970;172:306–10.
Akçay MN, Polat M, Cadirci M, et al. Tumor-induced ileo-ileal invagination in adults. Am Surg. 1994;60:980–1.
Marinis A, Yiallourou A, Samanides L, et al. Intussusception of the bowel in adults: a review. World J Gastroenterol. 2009;15:407–11.
Felix EL, Cohen MH, Bernstein AD, et al. Adult intussusception; case report of recurrent intussusception and review of the literature. Am J Surg. 1976;131:758–61.
Wechalekar AD, Gillmore JD, Hawkins PN. Systemic amyloidosis. Lancet. 2016;387:2641–54.
Scott PP, Scott WW Jr, Siegelman SS. Amyloidosis: an overview. Semin Roentgenol. 1986;21:103–12.
Gilat T, Revach M, Sohar E. Deposition of amyloid in the gastrointestinal tract. Gut. 1969;10:98–104.
Tada S, Iida M, Yao T, et al. Gastrointestinal amyloidosis: radiologic features by chemical types. Radiology. 1994;190:37–42.
Cui XH, Liu H, Fu L, et al. Henoch-Schonlein purpura with intussusception and hematochezia in an adult: A case report. Medicine. 2019;98:e16981.
Diaz MC, Ramundo ML, Christopher NC. Spontaneous reduction of a small bowel intussusception in a patient with Henoch Schonlein purpura. Am J Emerg Med. 2004;22:323–5.
LeBlanc KE. Jejuno-jejunal intussusception in a hemophiliac: a case report. Ann Emerg Med. 1982;11:149–51.
Nakayama Y, Fukushima M, Sakai M, et al. Intramural hematoma of the cecum as the lead point of intussusception in an elderly patient with hemophilia a: report of a case. Surg Today. 2006;36:563–5.
Tan HL, Chok AY, Li Y, et al. Systemic Amyloid Light-chain amyloidosis with colonic involvement complicated by colo-colic intussusception. ANZ J Surg. 2020;90:1162–3.
Haralabopoulos T, Soo M, Levingston R. An unusual case of gastrointestinal immunoglobulin light chain amyloidosis causing small bowel intussusception. Pathology. 2022;54:S46.
Matsumoto Y, Masuda T, Nishimura A, et al. A case of AL amyloidosis associated with follicular lymphoma with plasmacytic differentiation. Int J Hematol. 2020;111:317–23.
Kitahara T, Washiro M, Yoda A, et al. Gastrointestinal AL amyloidosis associated with intussusception–a case report. J Jpn Surg Assoc. 2022;83:1470–4.
Hokama A, Kishimoto K, Nakamoto M, et al. Endoscopic and histopathological features of gastrointestinal amyloidosis. World J Gastrointest Endosc. 2011;3:157–61.
Koop AH, Mousa OY, Wang MH. Clinical and endoscopic manifestations of gastrointestinal amyloidosis: a case series. Clujul Med. 2018;91:469–73.
Hemmer PR, Topazian MD, Gertz MA, et al. Globular amyloid doposits isolated to the small bowel. Am J Surg Pathol. 2007;31:141–5.
Mumford AD, O’Donnell J, Gillmore JD, et al. Bleeding symptoms and coagulation abnormalities in 337 patients with AL-amyloidosis. Br J Haematol. 2000;110:454–60.
James DG, Zuckerman GR, Sayuk GS, et al. Clinical recognition of Al type amyloidosis of the luminal gastrointestinal tract. Clin Gastroenterol Hepatol. 2007;5:582–8.
Greipp PR, Kyle RA, Bowie EJ. Factor-X deficiency in amyloidosis: a critical review. Am J Hematol. 1981;11:443–50.
Choufani EB, Sanchorawala V, Ernst T, et al. Acquired factor X deficiency in patients with amyloid light-chain amyloidosis: incidence, bleeding manifestations, and response to high-dose chemotherapy. Blood. 2001;97:1885–7.
Furie B, Voo L, McAdam KP, et al. Mechanism of factor X deficiency in systemic amyloidosis. N Engl J Med. 1981;304:827–30.
Acknowledgements
The authors would like to thank the Amyloidosis Research Group of the Ministry of Health, Labour and Welfare (Hironobu Naiki, Team Leader) for classifying the type of amyloidosis.
Author information
Authors and Affiliations
Contributions
The first draft of the manuscript was written by RH. SM and HK commented on previous versions of the manuscript and edited. GS, YI, AT, MM, and HF had discussion with the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Hayashi, R., Sawada, G., Ichikawa, Y. et al. A case of intestinal intussusception with unique hemorrhagic polyps due to AL amyloidosis and excessive anticoagulation. Clin J Gastroenterol 17, 258–262 (2024). https://doi.org/10.1007/s12328-023-01915-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12328-023-01915-6