Abstract
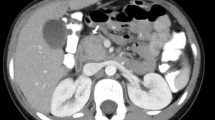
A 70-year-old man with epigastric pain was referred to our hospital. Computed tomography and magnetic resonance imaging showed the diffusely enlarged pancreas compared to his normal pancreas 6 months prior to presentation. Serum levels of IgG4 and amylase were normal, while C-reactive protein was slightly elevated. Endoscopic ultrasound-guided fine-needle biopsy of the pancreas revealed acinar–ductal metaplasia with neutrophil infiltration and without infiltration of IgG4-positive plasma cells. After the clinical diagnosis of type 2 autoimmune pancreatitis (AIP), his symptoms spontaneously improved without steroid therapy. Three months later, radiological findings showed improved pancreas size and serological findings. The pathological diagnosis of type 2 AIP using endoscopic ultrasound-guided fine-needle biopsy is challenging, particularly for proving granulocyte epithelial lesions. This was a valuable type 2 AIP case in which the images before, at the time of onset, and at the time of spontaneous remission were evaluated.




Similar content being viewed by others
Abbreviations
- AIP:
-
Autoimmune pancreatitis
- ICDC:
-
International Consensus Diagnostic Criteria
- LPSP:
-
Lymphoplasmacytic sclerosing pancreatitis
- GELs:
-
Granulocyte epithelial lesions
- IBD:
-
Inflammatory bowel disease
- IPMN:
-
Intraductal papillary mucinous neoplasm
- MRCP:
-
Magnetic resonance cholangiopancreatography
- CeCT:
-
Contrast-enhanced computed tomography
- MRI:
-
Magnetic resonance imaging
- EUS-FNB:
-
Endoscopic ultrasound-guided fine-needle biopsy
- EUS-FNA:
-
Endoscopic ultrasound-guided fine-needle aspiration
- ADM:
-
Acinar–ductal metaplasia
References
Shimosegawa T, Chari ST, Frulloni L, et al. International consensus diagnostic criteria for autoimmune pancreatitis: guidelines of the International Association of Pancreatology. Pancreas. 2011;40:352–8.
Yoshida K, Toki F, Takeuchi T, et al. Chronic pancreatitis caused by an autoimmune abnormality. Proposal of the concept of autoimmune pancreatitis. Dig Dis Sci. 1995;40:1561–8.
Kawaguchi K, Koike M, Tsuruta K, et al. Lymphoplasmacytic sclerosing pancreatitis with cholangitis: a variant of primary sclerosing cholangitis extensively involving pancreas. Hum Pathol. 1991;22:387–95.
Zamboni G, Lüttges J, Capelli P, et al. Histopathological features of diagnostic and clinical relevance in autoimmune pancreatitis: a study on 53 resection specimens and 9 biopsy specimens. Virchows Arch. 2004;445:552–63.
Notohara K, Burgart LJ, Yadav D, et al. Idiopathic chronic pancreatitis with periductal lymphoplasmacytic infiltration: clinicopathologic features of 35 cases. Am J Surg Pathol. 2003;27:1119–27.
Hamano H, Kawa S, Horiuchi A, et al. High serum IgG4 concentrations in patients with sclerosing pancreatitis. N Engl J Med. 2001;344:732–8.
Umehara H, Okazaki K, Masaki Y, et al. A novel clinical entity, IgG4-related disease (IgG4RD): general concept and details. Mod Rheumatol. 2012;22:1–14.
Stone JH, Khosroshahi A, Deshpande V, et al. Recommendations for the nomenclature of IgG4-related disease and its individual organ system manifestations. Arthr Rheum. 2012;64:3061–7.
Deshpande V, Zen Y, Chan JK, et al. Consensus statement on the pathology of IgG4-related disease. Mod Pathol. 2012;25:1181–92.
Chari ST, Kloeppel G, Zhang L, et al. Histopathologic and clinical subtypes of autoimmune pancreatitis: the Honolulu consensus document. Pancreas. 2010;39:549–54.
Levy MJ, Reddy RP, Wiersema MJ, et al. EUS-guided trucut biopsy in establishing autoimmune pancreatitis as the cause of obstructive jaundice. Gastrointest Endosc. 2005;61:467–72.
Mizuno N, Bhatia V, Hosoda W, et al. Histological diagnosis of autoimmune pancreatitis using EUS-guided trucut biopsy: a comparison study with EUS-FNA. J Gastroenterol. 2009;44:742–50.
Banks PA, Bollen TL, Dervenis C, et al. Classification of acute pancreatitis–2012: revision of the Atlanta classification and definitions by international consensus. Gut. 2013;62:102–11.
Imai K, Matsubayashi H, Fukutomi A, et al. Endoscopic ultrasonography-guided fine needle aspiration biopsy using 22-gauge needle in diagnosis of autoimmune pancreatitis. Dig Liver Dis. 2011;43:869–74.
Sah RP, Chari ST, Pannala R, et al. Differences in clinical profile and relapse rate of type 1 versus type 2 autoimmune pancreatitis. Gastroenterology. 2010;139:140–8 (quiz e12-3).
Kurita A, Yasukawa S, Zen Y, et al. Comparison of a 22-gauge Franseen-tip needle with a 20-gauge forward-bevel needle for the diagnosis of type 1 autoimmune pancreatitis: a prospective, randomized, controlled, multicenter study (COMPAS study). Gastrointest Endosc. 2020;91:373-81.e2.
Ishikawa T, Kawashima H, Ohno E, et al. Usefulness of endoscopic ultrasound-guided fine-needle biopsy for the diagnosis of autoimmune pancreatitis using a 22-gauge Franseen needle: a prospective multicenter study. Endoscopy. 2020;52:978–85.
Notohara K, Kamisawa T, Fukushima N, et al. Guidance for diagnosing autoimmune pancreatitis with biopsy tissues. Pathol Int. 2020;70:699–711.
Detlefsen S, Joergensen MT, Mortensen MB. Microscopic findings in EUS-guided fine needle (SharkCore) biopsies with type 1 and type 2 autoimmune pancreatitis. Pathol Int. 2017;67:514–20.
Matsumoto Y, Shimizu A, Ogawa K, et al. Late-onset type-2 autoimmune pancreatitis with two mass lesions diagnosed by endoscopic ultrasound-guided fine-needle aspiration. Clin J Gastroenterol. 2021;14:899–904.
Ollo D, Terraz S, Arnoux G, et al. Biliary involvement in type 2 autoimmune pancreatitis. Case Rep Gastroenterol. 2019;13:200–6.
Yoon SB, Moon SH, Song TJ, et al. Endoscopic ultrasound-guided fine needle aspiration versus biopsy for diagnosis of autoimmune pancreatitis: systematic review and comparative meta-analysis. Dig Endosc. 2021;33:1024–33.
Hayashi H, Miura S, Fujishima F, et al. Utility of endoscopic ultrasound-guided fine-needle aspiration and biopsy for histological diagnosis of type 2 autoimmune pancreatitis. Diagnostics. 2022;12:2464.
Hart PA, Levy MJ, Smyrk TC, et al. Clinical profiles and outcomes in idiopathic duct-centric chronic pancreatitis (type 2 autoimmune pancreatitis): the Mayo Clinic experience. Gut. 2016;65:1702–9.
Maire F, Le Baleur Y, Rebours V, et al. Outcome of patients with type 1 or 2 autoimmune pancreatitis. Am J Gastroenterol. 2011;106:151–6.
Notohara K. Histological features of autoimmune pancreatitis and IgG4-related sclerosing cholangitis with a correlation with imaging findings. J Med Ultrason. 2001;2021(48):581–94.
Hart PA, Kamisawa T, Brugge WR, et al. Long-term outcomes of autoimmune pancreatitis: a multicentre, international analysis. Gut. 2013;62:1771–6.
Kamisawa T, Chari ST, Giday SA, et al. Clinical profile of autoimmune pancreatitis and its histological subtypes: an international multicenter survey. Pancreas. 2011;40:809–14.
Iwamoto Y, Tatsumi F, Kohara K, et al. Dramatic recovery without steroid therapy and withdrawal from insulin therapy in a subject with hyperglycemic and hyperosmolar syndrome and depletion of insulin secretory capacity induced by type 2 autoimmune pancreatitis: a case report. Medicine (Baltimore). 2022;101: e28609.
Funding
None.
Author information
Authors and Affiliations
Contributions
All authors contributed to this case report. The first draft of the manuscript was written by Takashi Ito and all authors commented on previous versions of the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
Takashi Ito, Tsukasa Ikeura, Kenji Notohara, Masataka Masuda, Koh Nakamaru, Shinji Nakayama, Masaaki Shimatani, Makoto Takaoka, Kazuichi Okazaki, and Makoto Naganuma declare that they have no conflict of interest.
Human/animal rights
Not applicable.
Informed Consent
Informed consent was obtained from the patient to publised this report.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Ito, T., Ikeura, T., Notohara, K. et al. A case of type 2 autoimmune pancreatitis with spontaneous remission. Clin J Gastroenterol 16, 297–302 (2023). https://doi.org/10.1007/s12328-022-01753-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12328-022-01753-y