Abstract
Introduction
Penile cancer (PeCa) is an orphan disease in European countries. The current guidelines are predominantly based on retrospective studies with a low level of evidence. In our study, we aimed to identify predictors for guideline-conform treatment and hypothesize that reference centers for PeCa and physicians' experience promote guideline compliance and therefore correct local tumor therapy.
Methods
This study is part of the European PROspective Penile Cancer Study (E-PROPS), an international collaboration group evaluating therapeutic management for PeCa in Central Europe. For this module, a 14-item-survey was developed and sent to 681 urologists in 45 European centers. Three questions focused on therapeutic decisions for PeCa in clinical stage Tis, Ta-T1a, and T1b. Four questions addressed potential personal confounders. Survey results were analyzed by bootstrap-adjusted stepwise multivariate linear regression analysis to identify predictors for EAU guideline-conform local treatment of PeCa.
Results
For local therapy of cTis 80.4% recommended guideline-conform treatment, for cTa-cT1a 87.3% and for cT1b 59.1%. In total, 42.4% chose a correct approach in all tumor stages. The number of PeCa patients treated at the hospital, a higher level of training of the physicians, resource-based answering and the option of penile-sparing surgery offered at the hospital matched with giving guideline-conform recommendations and thus accurate local tumor treatment.
Conclusion
Patients with PeCa are best treated by experienced physicians, in centers with a high number of cases, which also offer a wide range of local tumor therapy. This could be offered in reference centers.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Why carry out this study? |
Penile cancer is an orphan disease, and guidelines are predominantly based on retrospective studies with a low level of evidence. Recent studies have shown low guideline compliance. |
We aimed to identify predictors for guideline-conform treatment recommendations and hypothesize that the establishment of reference centers and physicians' experience promote guideline-conform local tumor therapy. |
What was learned from the study? |
Guideline-conform treatment recommendations were dependent on tumor stage and the number of PeCa patients treated at the hospital, a higher level of training of the physicians, resource-based answering and the option of penile-sparing surgery offered at the hospital. |
This could be offered in reference centers. |
Digital Features
This article is published with digital features, including a summary slide, to facilitate understanding of the article. To view digital features for this article go to https://doi.org/10.6084/m9.figshare.12982370.
Introduction
Penile cancer (PeCa) is an orphan disease with a low incidence rate in European countries of 0.45–1.7 per 100,000 male inhabitants [1]. The European Association of Urology (EAU) guidelines on PeCa represent the current standard treatment recommendations [2]. Due to the low number of cases and therefore lack of treatment experience, high-level evidence to back up these guidelines is scarce [3]. Surgical local therapy for primary lesions depends strictly on tumor stage and ranges from local excision over glansectomy to partial or radical penectomy. Penile-sparing surgery is defined as complete preservation of the corpora cavernosa of the penis and is used as an established proxy for the quality of therapy in local tumor stages up to cT2 [4]. A carefully considered balance of complete tumor removal and maximal tissue preservation is essential for successful and guideline-conform treatment. The extent of resection after radical surgeries has been shown to inversely correlate with the postoperative quality of life, i.e., the more radical the surgery, the less preserved organ function is achieved, resulting in lower quality of life [5]. Former recommendations of wide tumor-negative surgical margins of up to 20 mm have been replaced by organ-sparing strategies, reducing radicality to a minimum of margins as narrow as 1 mm [6]. In summary, treatment of PeCa should be as organ-sparing as possible, while as radical as necessary. Despite higher recurrence rates after organ-preserving treatment, no impact on overall survival was observed [7].
A recently published retrospective multicenter study demonstrated that only 66% of patients received local tumor therapy that complied with the recommendations of the 2009 EAU guidelines on PeCa [8]. In one-third of the patients who did not receive correct local tumor therapy, this was due to surgeons' preference. In the majority of cases, this led to a more aggressive therapeutic approach [8]. This observation coincides with data of the Swedish national PeCa register. The authors showed that guideline adherence is as low as 71% for patients where organ-sparing treatment is indicated [9].
The discrepancy between guideline and real-live treatment recommendations for local tumor treatment is addressed by this study. Through a survey that was distributed between 681 urologists in Central Europe, we aimed to identify variables that predict guideline-compliant local tumor treatment. We assume that further specialization of the clinic and more experience of the physician promote guideline compliance and therefore correct local tumor therapy.
Methods
The European PROspective Penile Cancer Study (E-PROPS) was initiated to evaluate the therapeutic management of PeCa patients. The study consists of three separate modules, which are carried out in consecutive order. This article is part of the first module. Its centerpiece is a standardized survey aiming to assess the current state of treatment. The second module will be a retrospective multicenter study about the treatment PeCa patients received over the last 10 years. The third and final module will represent a prospective multicenter study including a tissue and serum database. The survey of E-PROPS module 1 was sent to 681 urologists working in 45 centers participating in E-PROPS (Germany n = 34, Austria n = 8, Switzerland n = 2, Italy n = 1). The survey was developed by the E-PROPS steering committee. It is written in German, an official language in all participating countries, and was checked for comprehensibility prior to its distribution. It consists of 14 questions assessing (1) the position of the surveyed person in the urological clinic, (2) personal responsibilities in PeCa therapy management, (3) individual knowledge on penile PeCa, (4) information about clinic-specific workflow, (5) the therapeutic management of PeCa patients (primary surgery, lymphadenectomy, chemotherapy) in the participating urological department and (6) the need for additional help to answer the questionnaire. Information about the participating physicians is given in Table 1.
Additionally, the following center-related information was collected: (1) the level of medical care (general hospital vs. advanced care hospital vs. maximum care hospital vs. university hospital) and its academic status (university vs. non-university), (2) the size of the urological department (number of practicing doctors—residents and specialists; number of beds for inpatient care), (3) the exact number of PeCa patients who received surgical treatment in the urological department in 2017, (4) availability and workflow for certain PeCa treatment regimens (radiotherapy is available at the hospital to treat PeCa: yes or no; chemotherapy is administered by urologists or medical oncologists or both), (5) the extent of surgical therapy offered to PeCa patients (laser therapy: yes or no; penile-sparing surgery: yes or no). All information about the participating centers that is of interest for this part of the E-PROPS project is given in Table 2.
The survey, its application and the recruitment letter were submitted to the Institutional Review Board at the University of Regensburg, and the project was granted exempt status. The IRB declared that as a survey study for physicians, obtaining information on treatment recommendations for hypothetical patient cases, no written consent is needed and therefore can be waived. This study was conducted in accordance with the Declaration of Helsinki in its latest version. The survey did not provide any information about the person completing it, assuring the anonymization of the data. The physicians in every participating medical center were informed about the study and its purpose and agreed that their survey data were being used as part of the study. The survey was distributed in the third quarter of 2018.
This article deals with the state of the art of local tumor therapy and its coherence with guideline recommendations. Participants in the survey were asked about the local tumor treatment patients will most likely receive at their institution for PeCa stage cTis (1), cTa and cT1a (2) or cT1b (3) (Table 3). For each tumor stage, several therapeutic regimes were given. However, not all of them complied with the EAU guidelines [2]. Participants also had the opportunity to indicate that they do not know the correct answer. The exact wording of the survey is found in Table 3 (the questions have been translated from German to English; the correct answers are written in bold).
Twelve independent variables with possible influence on treatment decisions were defined in advance. They are listed in Table 4. They are either related to the participant or the participating center. All independent variables were evaluated for their influence on guideline compliance. This was carried out by examining the relationship between the independent variables and the number of correctly answered questions (0–3), which we defined as the composite endpoint. The endpoint represents a scale for guideline adherence, where 0 correct answers corresponds to poor and 3 correct answers to exceptional guideline compliance. Testing was done by multivariate linear regression analysis (stepwise approach). The internal validity of the model was evaluated by bootstrapping with 1000 re-samples. The regression coefficient B and the p value were calculated for all independent variables. Regression coefficients > 0 indicate a positive influence of the independent variable on the number of correctly answered questions.
The type I error was not adjusted for multiple testing. Therefore, the results of inferential statistics are descriptive only. Statistical analysis was performed using the open-source R statistical software package, version 3.5.1 (The R Foundation for Statistical Computing, Vienna, Austria).
Results
Five hundred sixty-six out of 681 urologists returned their completed survey. Nine questionnaires were excluded, as they did not meet the minimum requirement for completeness (13/14 questions answered = 92.0%). In total, we included 557 questionnaires for further statistical investigation [response rate (RR) 85.7%, interquartile range (IQR) 75–94; calculated as the median of the individual response rate of the 45 participating clinics].
The number of guideline-conform treatment recommendations given by the participants for the respective tumor stage is listed in Table 5.
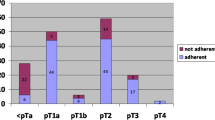
For local therapy of PeCa Tis, 80.4% chose a therapeutic approach recommended by the EAU guidelines (topical therapy 8.4%; laser therapy 49.4%; glans resurfacing 22.6%); 9.4% chose an approach not recommended by the EAU guidelines (partial penectomy 8.6%; radiotherapy 0.8%), and 10.2% declared not to know the correct answer. For local PeCa Ta or T1a therapy, 87.3% chose a therapeutic approach recommended by the EAU guidelines (laser therapy 17.9%; resurfacing of the glans penis 9.8%; glansectomy i.a. partial 59.7%). No participant opted for radiotherapy even though it is a recommended therapeutic approach. Partial penectomy was chosen by 6.8% although it is not indicated in this tumor stage; 5.9% declared not to know the correct answer. For local therapy of PeCa T1b, 59.1% chose a therapeutic approach recommended by the EAU guidelines (glansectomy—i.a. partial 59.1%; radiotherapy 0%). No participant chose radiotherapy, even though it is a feasible choice in this tumor stage; 33.7% chose a therapeutic approach not recommended by the EAU guidelines (laser therapy 0.6%; resurfacing of the glans penis 1.3%; partial penectomy 31.7%) and 7.3% declared not to know the correct answer.
Less than half of all participants (42.4%) decided for a correct therapeutic approach in all tumor stages; 7.6% did not recommend any correct treatment.
Stepwise multivariate linear regression analysis revealed that the variables “level of training of the physician,” “availability of penile-sparing surgery at the hospital,” “number of PeCa patients treated at the hospital” and “resource-based answering” are connected to the number of guideline-conform treatment recommendations given by the participants (Table 6). These findings could be validated with bootstrapping. Physicians with a higher degree of medical training have more often given correct treatment recommendations. The same applies to physicians who were working in a hospital with high numbers of PeCa patients and/or where penile-sparing surgery is offered. Using resources including the EAU guidelines also lead to more correct treatment recommendations. Other variables, such as “performing PeCa surgeries autonomously,” “knowledge of HPV-prevalence in PeCa,” “location” and “size of the urologic department,” “academic status of the hospital” and whether the “hospital offers radiotherapy or laser therapy” are not linked to giving correct treatment recommendations.
Discussion
Keeping updated on important new findings in diagnostics and therapy of the respective disease is essential for all physicians to provide their patients with high standard medical care. The guidelines of international organizations, such as the EAU are an essential tool in this respect. Evidence-based therapy recommendations should reduce personal bias and improve the success of treatment.
However, several studies have shown that adherence to guidelines by physicians in all specialties is still lacking to a significant extent. A recent study from The Netherlands highlighted this problem by comparing treatment regimens recommended by their national oncologic guidelines with treatment regimens patients received for tumor therapy, showing variances in adherence from 40 to 99%, depending on the tumor entity [10]. However, it is difficult to identify a single cause. Instead, the variance in compliance shows that there must be essential disease-specific differences. To our knowledge, only three retrospective studies exist so far comparing guideline recommendations and actual treatment regimens for local tumor treatment in PeCa [8, 9, 11]. Compliance ranged between 66 and 74.8%. In our survey guideline adherence was dependent on the local tumor stage. For PeCa Tis 80.4%, Ta-T1a 87.3% and T1b 59.1% of the participants chose a procedure that was within the guideline recommendations. Despite great adherence for low local tumor stage (Tis-T1a), only 42.4% of all participants were able to choose a correct treatment approach in all tumor stages. Furthermore, 7.6% did not choose any correct therapeutic approach at all. Of course, it should be noted that the survey results may not reflect "real-life scenarios". Choosing a therapeutic approach in a survey is usually handled with less care than if it was for a real patient. Likewise, in daily practice, key decisions on therapeutic regimens are usually made by or are at least evaluated by an experienced physician. Our survey however involved physicians from different countries and different hospitals, with a broad variance in experience and medical education. This gives us a unique opportunity to determine the main factors that lead to higher compliance with the guidelines.
The Hospitals PeCa Caseload Predicts Guideline Compliance
An important predictor for correct local tumor therapy is the number of PeCa patients treated at a hospital per year. Physicians working at a clinic with a higher frequency of PeCa patients suggested a guideline-based therapy more often. Our results further support the conclusions of previous authors who consider the centralization of medical care as the main key for better care of PeCa patients (1214 [12–14]). Bayles et al. compared the surgical results and the therapeutic success of patients at a single hospital before and after it became a regional reference center for PeCa. Bundling of patients resulted in a significantly higher rate of organ-preserving surgery, especially in patients with advanced local tumor stages [12]. However, it remains questionable whether the increase in organ-preserving interventions detected in this study can be solely attributed to the rise in patient frequency. The control group studied by Bayles et al. before the introduction of centralized medical care consists of patients who underwent surgery between 1969 and 1990. At that time, it was common practice to have a safety distance of at least 2 cm when resecting PeCa. Only after the examined hospital became a regional center for PeCa were studies able to prove that safety margins of only a few millimeters result in an equally good local result, making it the new standard of care [6]. Without this knowledge, organ-preserving surgery could never have been established. Thus, it is difficult to differentiate between the contributions to the improvement of local therapy made by the centralization of medical care and the findings on the surgical safety margin. In contrast to the absolute number of PeCa patients, the size of the clinic (assessed by the number of inpatient beds and medical staff) had just as little influence on guideline adherence as its level of care (primary care hospital, secondary care hospital, maximum-care hospital) or its academic status (university hospital: yes or no). These findings further underline that in such a rare disease as PeCa, regular exposure is of utmost importance and cannot be compensated by structural improvements alone.
Availability of Penile-Sparing Surgery Predicts Great Guideline Compliance
In addition to the number of patients with PeCa treated at a clinic per year, the surgical armamentarium offered also has a high predictive value. Physicians working in a hospital providing penile-sparing surgery were more likely to adhere to the guidelines for their treatment decisions. The availability of penile-sparing surgery is particularly important for local tumor stage T1b. While there are various other less invasive therapeutic options for local tumor stages Tis-T1a, such as laser or topical therapy, radiotherapy is the only less invasive therapeutic alternative to tumor stage T1b [2]. However, none of the participating physicians recommended local radiotherapy for tumor stages Ta-T1b. Therefore, it is not surprising that the possibility of being able to carry out local radiotherapy at the same clinic did not influence guideline adherence at all. In our survey, 33.7% recommended a treatment regime for tumor stage T1b that did not comply with the guidelines. In the majority of cases a too radical surgical method—in this case partial penectomy (31.7% of 33.7%)—was chosen. In contrast, only 1.9% chose a too superficial procedure, laser therapy (0.6%) or resurfacing of the glans 1.3%. This is in line with the findings of Bada et al. and Cindolo et al. who also showed that physicians are more likely to choose a too radical rather than a too superficial surgical approach, a problem that is aggravated in less experienced centers [11, 15]. On a positive note, > 90% of the physicians that participated in our survey stated that penile-sparing surgery is common practice in their department.
The Physicians' Skills Predict Guideline Compliance
Not only differences between the hospitals but also differences among the treating physicians have a great influence on correct tumor treatment. The treating physicians' level of medical education is an essential predictor for correct local tumor treatment. Thus, specialists are more likely to recommend a treatment approach that complies with the guidelines than residents. Curiously, this does not apply to the physicians' surgical skills as the ability to perform surgery on the penis autonomously was not a predictor for correct local tumor treatment. Why the latter does not influence the correct tumor therapy is difficult to explain, because it must be assumed that the group of specialists and the group of experienced surgeons are largely similar. However, this result underlines the importance of clinical experience in the management of oncologic patients in a surgical discipline like urology.
Resource-Based Answering
Nonetheless, it is not only clinical experience but also the use of supporting materials in the decision-making process that helps physicians to choose the correct treatment, and this is therefore an essential predictor for guideline compliance; 23.3% of the participants stated that they had used any additional source of reference to answer the questionnaire. Which kind of resource had been used was not specified. However, it is very likely that national or international guidelines, or at least the hospitals' standardized treatment plans, were used to answer the questions. As this has led to an improvement in therapy recommendations, it may be concluded that they are easy to understand and practical to implement. Moreover, a low level of evidence in the guidelines' recommendations, as is the case for penile cancer, does not deter physicians from following them. This indicates that physicians acknowledge that guidelines represent the best evidence available and are willing to accept their recommendations regardless of the significance of the data they are based on. This shows impressively that it is only possible to improve patient care by proving the effectiveness of therapy concepts with high-quality studies. Hence, these kinds of studies are missing for penile cancer, and their initiation has to be further promoted.
This study has several limitations. First, it does not reflect real-life data. In clinical practice treatment decisions are not made based on guideline recommendations alone; they are made depending on the state of health of the patient, his therapy wishes and the treating physicians' personal experience. Of course, they represent the best evidence available, but "guidelines are not mandates and do not purport to be a legal standard of care" [2]. However, due to the small number of cases, it is particularly difficult to develop great expertise in dealing with PeCa patients. The median number of patients treated for PeCa in the participating centers in 2017 was as low as 5 (IQR 3–8). Consequently, the guidelines are of particular importance in the management of these patients. As we know from previous retrospective studies, the contrary position of the treating physician is one of the main reasons that treatment regimens do not follow the guidelines [8]. This in turn explains the strength of our study. It deals exclusively with the physicians’ treatment decisions. Other confounders also influencing treatment decisions in everyday life are faded out. In this way, we were able to identify four parameters that predict the physicians’ guideline compliance for local treatment of PeCa. It is hoped that observance of these principles (1: treatment of patients in high volume centers; 2: penile-sparing surgery is offered by the treating hospital; 3: experienced physicians are involved in the primary therapy decision; 4: in case of any doubt, a source of reference is used) in everyday life will lead to a better rate of guideline-based therapy recommendations and therefore will promote the therapeutic outcome of PeCa patients, especially for patients with a local tumor stage cT1b, who require a less invasive therapy, such as penile-sparing surgery, for the best possible functional result.
Conclusion
Our survey-based data lead us to the conclusion that patients with PeCa are best treated by experienced physicians, in centers with a high number of cases, which also offer a wide range of local tumor therapies. In our opinion, this is only possible in specialized centers. This in turn leads to a repetition of the E-PROPS groups’ demand that a European or at least national network for second opinions for PeCa patients should be established [16, 17]. Until then, the best way to improve patient care for PeCa is to promote the use of auxiliary materials, such as the EAU guidelines, as this is the easiest way to ensure that inexperienced physicians know how to treat PeCa, too.
References
Christodoulidou M, Sahdev V, Houssein S, Muneer A. Epidemiology of penile cancer. Curr Probl Cancer. 2015;39(3):126–36.
Hakenberg OW, Compérat EM, Minhas S, Necchi A, Protzel C, Watkin N. EAU guidelines on penile cancer: 2014 update. Eur Urol. 2015;67(1):142–50.
Hakenberg OW, Drager DL, Erbersdobler A, Naumann CM, Junemann KP, Protzel C. The diagnosis and treatment of penile cancer. Deutsches Arzteblatt International. 2018;115(39):646–52.
Hegarty PK, Eardley I, Heidenreich A, McDougal WS, Minhas S, Spiess PE, et al. Penile cancer: organ-sparing techniques. BJU Int. 2014;114(6):799–805.
Sosnowski R, Wolski JK, Kulpa M, Zietalewicz U, Kosowicz M, Kalinowski T, et al. Assessment of quality of life in patients surgically treated for penile cancer: impact of aggressiveness in surgery. Eur J Oncol Nurs. 2017;31:1–5.
Minhas S, Kayes O, Hegarty P, Kumar P, Freeman A, Ralph D. What surgical resection margins are required to achieve oncological control in men with primary penile cancer? BJU Int. 2005;96(7):1040–3.
Djajadiningrat RS, van Werkhoven E, Meinhardt W, van Rhijn BW, Bex A, van der Poel HG, et al. Penile sparing surgery for penile cancer-does it affect survival? J Urol. 2014;192(1):120–5.
Bada M, Berardinelli F, Nyirady P, Varga J, Ditonno P, Battaglia M, et al. Adherence to the EAU guidelines on Penile Cancer Treatment: European, multicentre, retrospective study. J Cancer Res Clin Oncol. 2019;145(4):921–6.
Kirrander P, Sherif A, Friedrich B, Lambe M, Hakansson U. Swedish National Penile Cancer Register: incidence, tumour characteristics, management and survival. BJU Int. 2016;117(2):287–92.
Heins MJ, de Jong JD, Spronk I, Ho VKY, Brink M, Korevaar JC. Adherence to cancer treatment guidelines: influence of general and cancer-specific guideline characteristics. Eur J Public Health. 2017;27(4):616–20.
Cindolo L, Spiess PE, Bada M, Chipollini JJ, Nyirády P, Chiodini P, et al. Adherence to EAU guidelines on penile cancer translates into better outcomes: a multicenter international study. World J Urol. 2019;37(8):1649–57.
Bayles AC, Sethia KK. The impact of Improving Outcomes Guidance on the management and outcomes of patients with carcinoma of the penis. Ann R Coll Surg Engl. 2010;92(1):44–5.
Vanthoor J, Thomas A, Tsaur I, Albersen M, (eUROGEN) aicwtERNfrudacc. Making surgery safer by centralization of care: impact of case load in penile cancer. World J Urol. 2019;38:1385–90.
Matulewicz RS, Flum AS, Helenowski I, Jovanovic B, Palis B, Bilimoria KY, et al. Centralization of penile cancer management in the United States: a combined analysis of the American Board of Urology and National Cancer Data Base. Urology. 2016;90:82–8.
Bada M, Berardinelli F, Nyiràdy P, Varga J, Ditonno P, Battaglia M, et al. Adherence to the EAU guidelines on Penile Cancer Treatment: European, multicentre, retrospective study. J Cancer Res Clin Oncol. 2019;145(4):921–6.
Distler FA, Pahernik S, Gakis G, Hutterer G, Lebentrau S, Rink M, et al. Adherence to the EAU guideline recommendations for systemic chemotherapy in penile cancer: results of the E-PROPS study group survey. World J Urol. 2019;38:2523–30.
Suarez-Ibarrola R, Zengerling F, Haccius M, Lebentrau S, Schmid HP, Bier M, et al. Adherence to European association of urology and national comprehensive cancer network guidelines criteria for inguinal and pelvic lymph node dissection in penile cancer patients-a survey assessment in German-speaking Countries on Behalf of the European Prospective Penile Cancer Study Group. Eur Urol Focus. 2020;S2405-4569(20)30061-4. https://doi.org/10.1016/j.euf.2020.02.005.
Acknowledgements
We thank the participants of the study.
Funding
No funding or sponsorship was received for this independent and investigator-initiated study. No Rapid Service or Open Access Fees were received by the journal for the publication of this article.
Authorship
All named authors meet the International Committee of Medical Journal Editors (ICMJE) criteria for authorship for this article, take responsibility for the integrity of the work as a whole, and have given their approval for this version to be published.
Disclosures
The authors Maximilian Pallauf, Marie C. Hempel, Marie C. Hupe, Matthias May, Marlene Haccius, Dorothea Weckermann, Steffen Lebentrau, Bernd Hoschke, Ulrike Necknig, Jesco Pfitzenmaier, Lukas Manka, Philipp Nuhn, Peter Törzsök and Lukas Lusuardi have nothing to disclose. Axel S. Merseburger is an Editorial Board Member of Advances in Therapy.
Compliance with Ethics Guidelines
This study was conducted in accordance with the Declaration of Helsinki in its latest version. The survey, its application, and the recruitment letter were submitted to the Institutional Review Board at the University of Regensburg and the project was granted exempt status. The IRB declared that as a survey study for physicians, obtaining information on treatment recommendations for hypothetical patient cases, no written consent is needed and therefore can be waived. The survey did not provide any information about the person completing it, assuring the anonymization of the data. The physicians in every participating medical center were informed about the study and its purpose and agreed that their survey data was being used as part of the study.
Data Availability
The datasets generated during and/or analyzed during the current study are available from the corresponding author on reasonable request.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License, which permits any non-commercial use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc/4.0/.
About this article
Cite this article
Pallauf, M., Hempel, M.C., Hupe, M.C. et al. Adherence to the EAU Guideline Recommendations for Local Tumor Treatment in Penile Cancer: Results of the European PROspective Penile Cancer Study Group Survey (E-PROPS). Adv Ther 37, 4969–4980 (2020). https://doi.org/10.1007/s12325-020-01514-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12325-020-01514-8