Abstract
Hematologic complete remission (CR) is achievable for most adults with B cell precursor acute lymphoblastic leukemia (BCP-ALL). However, minimal residual disease (MRD) in patients with hematologic CR is associated with increased risk of relapse, shorter survival, and poorer transplantation outcomes. This study explored the concept of cure in adults with Philadelphia chromosome-negative (Ph−) BCP-ALL by MRD status at first hematologic CR (CR1) to inform evaluation of the clinical and economic benefits of new agents, where the concept of cure is important but long-term data are not available. The study used modified Delphi methodology involving clinicians experienced in the treatment of adult ALL. Participants completed a questionnaire, which was followed by country-specific panel discussions to discuss results and identify consensus on concepts and definitions. Clinicians from France (n = 4), Germany (n = 4), and the UK (n = 5) took part. Participants described cure in terms of the probability of future relapse. Relapse-free survival (RFS) was the preferred outcome measure to describe cure for the three patient groups considered (patients with MRD at CR1; patients who become negative for MRD after further treatment; patients who continue to have MRD). Consensus was reached on definitions of cure: that cure would begin to be considered at 3 years’ RFS and/or would be highly likely at 5 years’ RFS. Participants agreed that patients with MRD should usually undergo hematopoietic stem cell transplantation to have the best chance of survival; consensus was reached that alternatives are required when transplantation is not an option. Panels agreed that patients who achieve cure have a higher mortality rate and lower health-related quality of life than the general population. This study provides quantitative and qualitative information on the concept of cure in Ph− BCP-ALL in CR by MRD status applicable to interpreting the value of new therapies.
Funding: Amgen.
Plain Language Summary: Plain language summary available for this article.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Plain Language Summary
Acute lymphoblastic leukemia (ALL) is a blood cancer caused by abnormal white blood cells in the bone marrow. Patients with ALL are given chemotherapy to destroy the abnormal cells, but in some patients a small number of abnormal cells remain that cannot be detected by conventional methods. The risk of disease returning is greater for these patients than for patients without residual abnormal cells.
New therapies are being introduced for ALL that may help patients to achieve cure, but there is no clear agreement on how cure should be defined. To find out, we asked the opinions of specialists to see if they could reach a consensus. As the presence of residual abnormal cells increases the likelihood that ALL will return, we asked these specialists to consider groups of patients with and without these cells. The specialists agreed that:
-
The length of time that patients continued without their disease returning was important in deciding whether the disease was likely to be cured.
-
Patients (with and without residual abnormal cells) are considered likely to be cured after 3–5 years of their disease not returning.
-
Patients with residual abnormal cells should usually undergo stem cell transplantation to have the best chance of survival.
-
Patients who are cured have poorer health and a higher risk of dying than people who have not had ALL.
The information gained from this study will help interpret evidence from clinical trials by suggesting which long-term outcomes of patients treated with new therapies are most meaningful.
Introduction
Acute lymphoblastic leukemia (ALL) is a rare hematologic malignancy that shows bimodal incidence, with most cases occurring in children (80%), followed by a gradual increase in incidence after 50 years of age [1, 2]. Approximately three-quarters of adult ALL cases are of B cell lineage, the majority originating from B lymphocyte precursors (BCP-ALL) [3].
For most adults with ALL, front-line chemotherapy will result in hematologic complete remission (CR) (based on morphologic assessment), which is a prerequisite, but by itself not sufficient, for cure. Patients who achieve hematologic CR can potentially harbor leukemic cells in the bone marrow. The presence of leukemic cells that are below the threshold of detection by conventional morphologic methods is referred to as minimal residual disease (MRD).
Large-scale analyses have shown a strong association between the presence of MRD after front-line chemotherapy and poor long-term outcomes, including increased risk of relapse and shorter relapse-free and disease-free survival [4,5,6,7,8]. European clinical guidelines therefore recommend testing patients in first hematologic complete remission (CR1) for MRD for the purpose of risk stratification [9], and this is reflected in national protocols for the treatment of adult ALL. This risk stratification dictates whether immediate (allogeneic) hematopoietic stem cell transplant (HSCT) is indicated for a given patient, because of a higher risk of relapse, or whether that patient should receive additional chemotherapy, because the lower risk of relapse would outweigh the mortality and morbidity associated with HSCT. Nevertheless, the current European guidelines lack deep clarity on the most appropriate use of MRD status and other prognostic factors for clinical decision-making in adults. In addition, the designated MRD status of an individual patient may be influenced by the detection technology and the time point of measurement. Decisions about treatment are further complicated by the recent approvals of immunotherapies for the treatment of adults with ALL (including blinatumomab, inotuzumab ozogamicin, and chimeric antigen receptor T cell therapy), as it is not yet clear how HSCT should be used in future treatment pathways incorporating these agents.
The concept of cure has been highlighted as particularly important when assessing the value of immunotherapies, for which treatment outcomes suggest that cure may be an increasingly achievable goal [10,11,12]. The long-term survival of patients who have received a new treatment versus the standard of care (SOC) is frequently critical to quantify potential clinical and economic benefits; however, data over longer time frames are rarely available, necessitating estimation of long-term outcomes using assumptions informed by expert opinion. Specifically, this includes understanding after what time point it may be assumed that patients will continue to survive in the long term, and what will be their long-term health status. This study was initiated to provide such estimates for patients in first hematologic CR in a transparent and methodologically sound manner, in the absence of previously published findings for this patient population.
Given the demonstrable prognostic implications of MRD in patients with BCP-ALL, this study aimed to use MRD status as the basis to explore concepts of cure, with the focus on adults with Philadelphia chromosome-negative (Ph−) BCP-ALL. Patients with Ph+ BCP-ALL were not considered in this study, as this group represents a minority with its own specific treatment pathways (including the use of tyrosine kinase inhibitors) and a distinctly different prognosis. This study also aimed to understand clinicians’ perspectives on the relationship between HSCT and cure, specifically whether HSCT is required for a patient to be considered “cured” in current clinical practice. Further, the study aimed to elicit estimates of the proportion of patients who meet specialists’ own definitions of cure in current clinical practice, and to garner understanding of the long-term prognoses of these patients (in terms of mortality and health-related quality of life, HRQL).
Several of these questions were deemed to be best answered through exploration of expert opinion from clinicians currently treating patients with ALL. Therefore, a consensus approach widely applied in health service research—Delphi methodology—was used for this study.
Representatives from five countries were included in this study: France, Germany, Italy, the UK, and Australia. It was considered valuable to gather country-specific insights into these various concepts, particularly given the differences between national protocols for adult ALL and differences in actual clinical practice. The clinical community treating adults with ALL is small and specialist in nature, such that a panel size of four or five experienced clinicians per country was considered pragmatic and appropriate. The findings based on data collected in France, Germany, and the UK are presented here, as the panels in these countries described similar patterns of practice in treating BCP-ALL and were aligned on definitions of cure. The findings from Italy and Australia were distinct in their definition of cure and will be described in a separate publication.
This report therefore describes the findings of this study for three European countries. In summary, the study aimed to better understand how cure can be defined in adult BCP-ALL for patients in first complete hematological remission and in the context of clinical practice in each country, to inform evaluation of the clinical and economic benefits of emerging agents, specifically immunotherapies.
Methods
Design
The study used a modified Delphi methodology, which is designed to reach consensus between individuals using questionnaire-based surveys [13]. The study had two phases: phase 1 involved the completion of a Word-based questionnaire; phase 2 involved participation in country-specific virtual panel discussions (including response gathering and voting). For categorical questions about which consensus for a given country could be evaluated (i.e., non-descriptive questions), consensus was defined by at least 80% of participants being in agreement if five participants were involved (i.e., four out of five participants). When panels involved four participants, consensus was defined as 75% agreement (i.e., three out of four participants). Ethical approval for the study was received from the Human Research Ethics Committee of the University of Technology, Sydney, Australia, and all participants provided informed consent.
Recruitment of Participants
The study aimed to recruit five participants from each of the countries. However, as a result of the limited availability of suitable participants, only four clinicians were recruited in both France and Germany.
Participants were recruited if they met the following inclusion criteria: board-certified or specialized in hematology or hemato-oncology; at least 5 years’ experience in this role after completion of training; treats adults with ALL; has seen at least two adults with ALL in the last 12 months, or at least five in the past 5 years; regularly tests patients with ALL for MRD in clinical practice; is able and willing to participate in the Delphi study; and is able to speak and write English as assessed by the research team during recruitment.
The identities of participants were kept confidential during the study, including from the study sponsor, to avoid potential bias.
Data Collection
In phase 1, participants completed Word-based questionnaires sent via email. The questionnaire consisted of categorical, numerical, and open-ended questions and included questions related to background information about the participants and their clinics; definition of cure; cure rates and survival outcomes; and the roles of allogeneic HSCT in achieving cure.
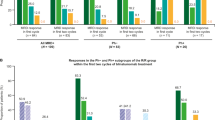
To understand the role of MRD status in the concept of cure, participants were initially asked to consider patients with Ph− BCP-ALL who were MRD-positive at the first MRD test (defined as the test after country-specific SOC induction therapy, typically used to determine risk of relapse and to establish the treatment plan for a given patient) (population A; Fig. 1). Participants were then asked to consider the concept of cure in two further patient populations: those who are initially MRD-positive at CR1 but who achieve MRD-negative status after subsequent treatment, and those who are MRD-positive at CR1 and remain so after subsequent treatment (populations B and C, respectively; Fig. 1). Participants were asked to define cure based on the general concepts of cure in oncology outlined by Johnson et al. [12], which were made specific to ALL: absence of disease (interpreted as MRD-negative status for patients with ALL at CR1), relapse-free survival (RFS), and overall survival (OS), with stratification for different MRD scenarios as described above. Questions were then asked about mortality risk and HRQL in patients with Ph− BCP-ALL who subsequently are considered to have achieved cure according to the clinician’s previously elicited specific definition.
Phase 2 consisted of a series of country-specific panel meetings conducted virtually (through a web conference platform, with audio and screen share capabilities). A summary of the country-specific phase 1 results was provided as input for the panel meetings. For questions about which consensus was reached in phase 1, no further discussion was facilitated in phase 2. When there was no consensus in phase 1, facilitated discussion of the phase 1 results took place, and when appropriate, additional participant responses were collected using an interactive voting system; on occasion, data were recorded manually. The voting involved presenting participants with statements on a topic, derived from phase 1 responses (either repeating questions already asked in the questionnaire after discussion had been completed or new statements based on responses received). The findings of the first panel meeting conducted (in the UK) informed refinement of the statements presented to subsequent panels. Participants were then asked to indicate with which statements they agreed. In some cases, participants could choose more than one statement, while in other cases only one answer was permitted. In France, one clinician was unable to attend the panel discussion at the last minute. Therefore, in this case, a one-to-one interview was conducted at a later time: the points raised in the panel were discussed, and the participant was asked to vote on the same statements, without knowledge of the responses from the other participants.
Data Analysis
Data from phases 1 and 2 of the study were entered into Microsoft Excel, anonymized, and analyzed to generate country-specific results. The analyses involved determining frequencies for categorical responses, using standard summary statistics for numerical responses, and identifying common themes from open-ended questions.
Results
Demographics of Panel
A total of 13 clinicians from France (n = 4), Germany (n = 4), and the UK (n = 5) took part in the study. Nine participants were hematologists and four were hemato-oncologists. The majority of the participants worked in a university hospital (n = 10), two were from a designated cancer hospital or specialist oncology center, and one was from a general (urban or community) hospital. All participants were working on clinical teams that conduct HSCT. Overall, participants had a median of 20 years’ experience (range 10–30 years) in treating ALL and treated a median of 14 patients (range 8–50) with Ph− BCP-ALL per year.
Definition of Cure
Participants described the potential for cure in terms of probability of relapse, rather than providing a definitive definition (see “Box 1”). They considered this to be a more appropriate way to discuss treatment goals and outcomes in patients with ALL. Importantly, all panels noted that a small minority of patients with ALL experience late relapses, so cure could not be defined with absolute certainty. In patients who are MRD-positive at CR1, participants in all countries described RFS as the preferred outcome measure for cure. MRD-negative status was described by some participants as an early indicator or predictor of cure, and OS was generally not preferred to RFS (or these measures were considered equivalent given the poor prognosis of ALL after relapse). Similarly, participants agreed that cure should be defined on the basis of RFS in the other patient groups (patients who are MRD-positive but subsequently became MRD-negative, population B, and those who remain MRD-positive, population C).
Discussion
The concept of cure has become an important element in healthcare decision-making in recent years. Critically, in this disease area, the lack of clarity regarding the definition of cure for adult Ph− BCP-ALL makes it challenging to interpret evidence about the long-term efficacy and relative value of emerging agents. This study was conducted using a Delphi approach to analyze the expert opinions of clinicians currently treating patients with ALL. The findings highlight both areas of commonality among experts from the three countries included, as well as areas where consensus could not be reached.
Our research aligns with other studies [16, 17], indicating that clinicians are hesitant to define patients as definitively “cured” because of the risk of late relapse. Despite this, participants were able to frame the concept of cure as being inversely related to the probability of relapse. Consistent with the results of a prior study using a similar methodology that focused specifically on patients with relapsed and refractory ALL [17], long-term leukemia-free (or in this study, “relapse-free”) survival was seen as key to the concept of cure. Our research complements this previous study; the current study has generated findings on the concept of cure for patients in first hematological remission, and in addition considered the impact of MRD status and provided country-specific findings.
The duration of relapse-free survival after which the potential for cure emerges also aligned among this group of expert panelists: in two of the three country-specific panels, there was consensus that cure could begin to be considered at 3 years’ RFS. The concept of a high likelihood of cure for patients at 5 years’ RFS was also agreed, most notably by all panels for patients in population C (patients who are MRD-positive and subsequently remain MRD-positive).
When considering the likelihood of cure, participants found it difficult to estimate cure rates for patients with Ph− BCP-ALL, because treatment options are rapidly evolving, the condition is rare, and outcomes vary with age, health status, and eligibility for HSCT. For patients who are MRD-positive, and critically who are eligible for HSCT, consensus among each panel was that cure rates could be expected in the range 30–50%, with considerably lower rates of cure expected among those ineligible for HSCT.
Reflecting the dependence of the probability of cure on eligibility for HSCT, participants pointed out the integral role of HSCT in current clinical practice for patients who are MRD-positive at CR1; they furthermore agreed that allogeneic HSCT cannot be performed in all patients. For patients who are ineligible for HSCT on the basis of age, comorbidities, or availability of a donor, participants agreed that alternative treatments are needed. A number of participants noted that cure is possible in some patients with Ph− BCP-ALL who are MRD-positive, despite not receiving HSCT. There was some speculation about the future role of immunotherapy in patients who have MRD-positive status at CR1. This was discussed as an important option for achieving MRD-negative status, but there was uncertainty regarding the long-term durability of responses to such therapy.
Notably, participants generally agreed that the concept of cure does not imply that “cured” patients are likely to revert to the mortality risk and HRQL expectations of people who have not suffered this disease. However, mortality rates among those considered to be cured from ALL after HSCT were generally felt by panelists to have improved in recent years (two of the three panels agreed that the mortality risk was not more than four times greater than the age- and gender-matched general population). Moreover, some clinicians opined that the impact of BCP-ALL on HRQL varies between individual patients, depending on whether they have long-term complications of treatment, notably chronic GVHD, and that the detrimental effects of therapy may lessen in subsequent years.
A strength of this study is that the Delphi methodology allows participants to exchange information and discuss their experiences before final responses are captured. Importantly, this method involves collecting both quantitative estimates and qualitative explanations of the rationales behind decisions and opinions. This provides a nuanced understanding of the concepts under consideration and the reasons for agreement or lack thereof.
We also recognize the limitations of this study, particularly with respect to the size of the panels and how representative these are of the country-specific clinician community (i.e., only four or five participants provided their opinions, to represent a country-wide perspective). We do, however, consider these panel sizes to be adequate to provide meaningful results, given the small and specialist nature of the clinical community treating adults with ALL in each country.
Conclusions
This study offers quantitative and qualitative information on the concept of cure in adults with BCP-ALL in hematologic CR with or without MRD—from the points of view of clinicians in three Western European countries—with the aim of informing evaluation of the clinical and economic benefits of emerging novel therapeutic agents for ALL, specifically immunotherapies. Expert clinicians defined the threshold for reasonable probability of cure for this disease and patient population on the basis of 3–5 years’ RFS. The likelihood of cure in patients with MRD was described as dependent on eligibility for HSCT, with clinicians consistently suggesting that alternative therapies are needed for those who are ineligible. Cure was associated with increased mortality risk and negative impacts on HRQL (compared with the general population), critically as a consequence of treatment.
References
Paul S, Kantarjian H, Jabbour EJ. Adult acute lymphoblastic leukemia. Mayo Clin Proc. 2016;91(11):1645–66.
American Cancer Society. Key statistics for acute lymphocytic leukemia (ALL) 2019. https://www.cancer.org/cancer/acute-lymphocytic-leukemia/about/key-statistics.html. Accessed 20 Feb 2019.
Terwilliger T, Abdul-Hay M. Acute lymphoblastic leukemia: a comprehensive review and 2017 update. Blood Cancer J. 2017;7(6):e577.
Bruggemann M, Raff T, Flohr T, et al. Clinical significance of minimal residual disease quantification in adult patients with standard-risk acute lymphoblastic leukemia. Blood. 2006;107(3):1116–23.
Patel B, Rai L, Buck G, et al. Minimal residual disease is a significant predictor of treatment failure in non T-lineage adult acute lymphoblastic leukaemia: final results of the international trial UKALL XII/ECOG2993. Br J Haematol. 2010;148(1):80–9.
Gökbuget N, Kneba M, Raff T, et al. Adult patients with acute lymphoblastic leukemia and molecular failure display a poor prognosis and are candidates for stem cell transplantation and targeted therapies. Blood. 2012;120(9):1868–76.
Ravandi F, Jorgensen JL, O’Brien SM, et al. Minimal residual disease assessed by multi-parameter flow cytometry is highly prognostic in adult patients with acute lymphoblastic leukaemia. Br J Haematol. 2016;172(3):392–400.
Gokbuget N, Dombret H, Giebel S, et al. Minimal residual disease level predicts outcome in adults with Ph-negative B-precursor acute lymphoblastic leukemia. Hematology. 2019;24(1):337–48.
Hoelzer D, Bassan R, Dombret H, Fielding A, Ribera JM, Buske C. Acute lymphoblastic leukaemia in adult patients: ESMO Clinical Practice Guidelines for diagnosis, treatment and follow-up. Ann Oncol. 2016;27(suppl 5):v69–82.
Eggermont AM, Kroemer G, Zitvogel L. Immunotherapy and the concept of a clinical cure. Eur J Cancer. 2013;49(14):2965–7.
Hellmann MD, Kris MG, Rudin CM. Medians and milestones in describing the path to cancer cures: telling “tails”. JAMA Oncol. 2016;2(2):167–8.
Johnson P, Greiner W, Al-Dakkak I, Wagner S. Which metrics are appropriate to describe the value of new cancer therapies? Biomed Res Int. 2015;2015:865101.
Hsu C-C, Sandford B. The Delphi technique: making sense of consensus. Pract Assess Res Eval. 2007;12:1–8.
Berry DA, Zhou S, Higley H, et al. Association of minimal residual disease with clinical outcome in pediatric and adult acute lymphoblastic leukemia: a meta-analysis. JAMA Oncol. 2017;3(7):e170580.
Martin PJ, Counts GW, Jr, Appelbaum FR, et al. Life expectancy in patients surviving more than 5 years after hematopoietic cell transplantation. J Clin Oncol. 2010;28(6):1011–6.
Miller K, Abraham JH, Rhodes L, Roberts R. Use of the word “cure” in oncology. J Oncol Pract. 2013;9(4):e136–40.
Bassan R, Hoelzer D, Thomas X, et al. Clinician concepts of cure in adult relapsed and refractory Philadelphia-negative B cell precursor acute lymphoblastic leukemia: a Delphi study. Adv Ther. 2019;36(4):870–9.
Acknowledgements
The authors thank the participants for their time and engagement with the study.
Funding
Sponsorship for this study, the journal’s rapid service fee, and open access fees were funded by Amgen.
Medical Writing Assistance
Medical writing assistance was provided by members of PRMA Consulting and funded by Amgen.
Authorship
All named authors meet the International Committee of Medical Journal Editors (ICMJE) criteria for authorship for this article, take responsibility for the integrity of the work as a whole, and have given their approval for this version to be published.
Disclosures
Wendy Gidman is a former employee of PRMA Consulting Ltd (current affiliation: Roche Ltd) and does not have any competing interests. Shweta Shah is a current employee and shareholder of Amgen Inc. Lirong Zhang is a former employee of PRMA Consulting Ltd (current affiliation: ICON plc) and does not have any competing interests. Jan McKendrick is a current employee of PRMA Consulting Ltd and does not have any competing interests. Ze Cong is a former employee and shareholder of Amgen Inc. (current affiliation: Global Blood Therapeutics Inc.). David Cohan is a current employee and shareholder of Amgen Inc. Oliver Ottmann is an employee of Cardiff University; he has received research grants from Amgen, Celgene, and Incyte, and consulting fees or other remuneration from Amgen, Celgene, Fusion Pharma, Incyte, Novartis, Pfizer, Roche, and Takeda.
Compliance with Ethics Guidelines
Ethical approval for the study was received from the Human Research Ethics Committee of the University of Technology, Sydney, Australia. All procedures performed in studies involving human participants were in accordance with the ethical standards of the research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards. Informed consent was obtained from all individual participants included in the study.
Data Availability
The datasets generated during and/or analyzed during the current study are available from the corresponding author on reasonable request.
Author information
Authors and Affiliations
Corresponding author
Additional information
Enhanced Digital Features
To view enhanced digital features for this article go to https://doi.org/10.6084/m9.figshare.9816290.
Rights and permissions
Open Access This article is distributed under the terms of the Creative Commons Attribution-NonCommercial 4.0 International License (http://creativecommons.org/licenses/by-nc/4.0/), which permits any noncommercial use, distribution, and reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made.
About this article
Cite this article
Gidman, W., Shah, S., Zhang, L. et al. Clinicians’ Perspectives on Cure in Adult Patients with Acute Lymphoblastic Leukemia with Minimal Residual Disease: A Delphi Study. Adv Ther 36, 3017–3029 (2019). https://doi.org/10.1007/s12325-019-01099-x
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12325-019-01099-x