Abstract
Introduction
Chronic pain is an important yet overlooked non-motor symptom of Parkinson’s disease (PD), caused by an imbalance of the dopaminergic and glutamatergic systems. Safinamide has a multimodal mechanism of action, dopaminergic (reversible MAO-B inhibition) and non-dopaminergic (modulation of the abnormal glutamate release), that might be beneficial for both motor and non-motor symptoms.
Objectives
To investigate the long-term (2-year) efficacy of safinamide on PD chronic pain and to confirm the positive effects observed after 6 months of treatment.
Methods
This is a post hoc analysis of the data from the 2-year study 018, focused on the reduction of concomitant pain treatments and on the scores of pain-related items of the Parkinson’s disease quality of life questionnaire (PDQ-39).
Results
Safinamide, compared with placebo, significantly improved the PDQ-39 items 37 (“painful cramps or spasm,” p = 0.0074) and 39 (“unpleasantly hot or cold,” p = 0.0209) and significantly reduced the number of concomitant pain treatments by 26.2% (p = 0.005). A significantly greater proportion of patients in the safinamide group was not using pain drugs after 2 years of treatment (p = 0.0478).
Conclusions
The positive effects of safinamide on PD chronic pain were maintained in the long term. Further investigations are desirable to confirm their clinical relevance.
Funding
Zambon SpA.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Parkinson’s disease (PD) is a progressive neurologic condition, characterized by the loss of the neurons in the substantia nigra, where the typical motor symptoms include bradykinesia (slowness of the movements), rigidity (stiffness), resting tremor and balance problems. The disease is also associated with some non-motor symptoms such as depression, cognitive deterioration, apathy and chronic pain. Even if pain is not a cardinal feature of PD, nevertheless it is an important complication that has a substantial negative impact on patients’ quality of life. Several studies showed that pain may represent a significant comorbidity in up to 85% of PD patients and may precede and overshadow the motor symptoms of the disease [1].
Despite its relevance, the pathophysiologic mechanisms underlying pain in PD are not fully understood. Abnormal nociceptive inputs may be the consequence of decreased basal ganglia dopaminergic neurotransmission: pain occurs more frequently in patients during their “OFF” periods, which correlates with low dopaminergic activity in the striatum. Furthermore, a neurodegeneration involving non-dopaminergic systems, such as gamma-aminobutyric acid and glutamate, which modulate pain processing in other regions of the brain, may also play a relevant role [2].
No drugs are specifically indicated for PD pain, and about 50% of the patients do not receive any treatment because of the inefficacy of common analgesics [3].
Safinamide has a multimodal mechanism of action completely different from those of any other PD treatments. Beyond the reversible monoamine oxidase-B (MAO-B) inhibition, safinamide is endowed with non-dopaminergic properties such as the modulation of the abnormal glutamate release through the sodium channels blockade (Fig. 1). A first post hoc analysis of two 24-week pivotal trials showed positive effects on pain management [4]: the aim of this new post hoc analysis of the data from the 2-year study 018 was to investigate the long-term efficacy of safinamide on PD chronic pain and confirm the previous results.
Methods
Trial 018 (NCT01286935) [5] was a multicenter, multinational, double-blind, placebo-controlled extension of the phase III, 24-week, pivotal study 016 [6] in mid- to late-stage fluctuating PD patients on a stable dose of levodopa (alone or with other PD drugs).
Patients were included in study 018 if they had completed trial 016, were treatment compliant and willing to continue, and were further treated with safinamide or placebo as add-on to their optimized standard therapy for up to 2 years. The doses of levodopa and additional PD therapies should remain stable, whenever possible, during the treatment period. However, the doses could be changed in case of motor symptom deterioration or occurrence of adverse events.
Treatments with tri-tetracyclics, MAO-B inhibitors, serotonin-norepinephrine reuptake inhibitors (SNRIs), opioids, neuroleptics, barbiturates and phenothiazines were not permitted. Selective serotonin reuptake inhibitors (SSRIs) were allowed at study entry at the lowest therapeutic dose and had to remain stable throughout the trial.
Both the protocol and patient materials were approved by Independent Ethics Committees and Health Authorities in all the participating countries. All procedures performed were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards. Informed consent was obtained from all individual participants included in the study.
The primary endpoint was the change from baseline (study 016 start) to study end (week 102) in the total dyskinesia rating scale (DRS) score, and the main secondary endpoints were the change in the total daily ON and OFF time and in the quality of life. Even if the primary endpoint was not met, despite a substantial decrease in DRS scores with safinamide 100 mg/day compared with placebo (27% vs. 3%, respectively), safinamide significantly improved the daily ON time and significantly reduced the OFF time without increasing troublesome dyskinesia, maintaining its efficacy for up to 2 years. All the scales/questionnaires administered during the study were performed during the “ON” phase. The incidence of adverse events and serious adverse events was similar in the safinamide and placebo groups, and no significant abnormalities were detected in cardiovascular and laboratory examinations [5].
Outcome Measures
This is a post hoc analysis of the data from study 018, evaluating the long-term effects of safinamide 100 mg/day oral tablets versus placebo on chronic pain in fluctuating PD patients.
The variables assessed were:
-
The proportion of patients not using concomitant pain treatments during the study period and the number of pain treatments used in each group. Pain treatments included analgesics, anti-inflammatory, anti-rheumatic drugs and topical products for joint and muscular pain.
-
The changes from baseline to study end in the scores for the pain-related items 37–39 of the PDQ-39 “Bodily discomfort” domain. The PDQ-39 scale was administered during the “ON” phase.
Statistical Methods
The methods reported here are the same as those of the previous post hoc analysis of the data after 6 months' treatment [4], but are also reported here for clarity. This report expands on the previous study by long-term data up to 2 years.
The intention-to-treat (ITT) populations were used for all the analyses, while the last observation carried forward (LOCF) approach was applied to account for missing data at study termination.
The comparison of the percentage of patients not using concomitant pain drugs after 2 years of treatment was performed using conventional Pearson’s chi square. The reduction in the number of pain treatments was estimated by means of a negative binomial regression model obtained with a generalized linear model parameterized with a logarithmic link function and negative binomial distribution and with “treatment” (safinamide 100 mg/day or placebo) and “study indicator” (study 018) as fixed effects. The analysis was performed using the GENMOD procedure of SAS software version 9.4.
The analyses of PDQ-39 domain “Bodily discomfort” and PDQ-39 individual items related to pain were performed using an ANCOVA model with changes from baseline scores as dependent variable, “Treatment” (safinamide 100 mg/day or placebo) and “Study indicator” (study 018) as fixed effects and with baseline values as covariate.
Results
A previous post hoc analysis on the data after 6 months of treatment showed that the percentage of patients with no pain treatments was significantly higher in the safinamide group compared with the placebo group (76.1% vs. 70%), with a reduction of concomitant pain drugs of about 24% [4].
These results were confirmed in the long term: after 2 years, the proportion of patients not using concomitant pain treatments was significantly greater in the group receiving safinamide than in the placebo group (respectively 61.1% vs. 50.9%, p = 0.0478) (Fig. 2).
Safinamide, compared with placebo, significantly reduced the individual number of concomitant pain treatments on average by 26.2% compared with placebo [95% confidence interval (CI): 8.9%, 40.3%; p = 0.005].
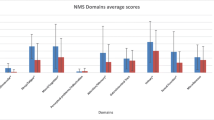
The long-term treatment with safinamide was also associated with a statistically significant improvement compared with placebo in two of the three items of the PDQ-39 related to pain, confirming the benefits seen after 6 months: item 37 “Had painful muscle cramps or spasm,” least squares (LS) mean difference vs. placebo for the changes from baseline – 0.23 (95% CI: − 0.40, − 0–06; p = 0.0074) after 2 years (− 0.19, p = 0.0009 after 6 months); item 39 “Felt unpleasantly hot or cold,” LS mean difference vs. placebo for the changes from baseline − 0.14 (95% CI: − 0.33, − 0.03; p = 0.0209) after 2 years (− 0.15, p = 0.0060 after 6 months) (Fig. 3). Item 38 (“Had aches and pains in your joints or body?”) was not improved in either the short or long term. The joint pain in PD patients is related to the lack of mobility and stiffness of limb movements and is generally treated with nonsteroidal anti-inflammatory drugs, analgesics or opioids in tandem with physical activity [7]. Safinamide is devoid of analgesic properties; therefore, this lack of efficacy is not unexpected.
The overall “Bodily discomfort” domain score was also significantly improved with safinamide compared with placebo: LS mean difference vs. placebo for the changes from baseline − 3.66 (95% CI: − 6.71, − 0.60; p = 0.0190) after 2 years (− 3.69, p = 0.0007 after 6 months).
Discussion
The correlation between pain and PD was first described by James Parkinson as “rheumatic pain extending from the arms to the fingers" [8].
Chronic pain is one the most important non-motor symptoms of PD, present in the majority of the subjects, and occurs two to three times more frequently in PD patients than in the age-matched healthy population [9]. It is classically classified into nociceptive pain (musculoskeletal, dystonic and visceral) and neuropathic pain (radicular-peripheral and central), and musculoskeletal and central neuropathic pains are the prevalent syndromes [10].
Chronic pain is associated with a worsening of the quality of life greater than motor symptom deterioration and affects patients’ daily activities more than memory problems and depression, with a consequent considerable economic burden [11]. Chronic analgesic prescription is significantly higher in PD patients (33%) than in the general population (20%) and diabetic patients (26%) with an abuse of non-steroidal anti-inflammatory drugs [12].
The basal ganglia are involved not only in motor functions, but also in the processing of nociceptive inputs through two main dopaminergic pathways: the nigrostriatal pathway, which is directly involved in the deterioration of motor symptoms, and the mesolimbic pathway, which is related to the reward system and central modulation of pain. Therefore, there is a substantial overlap between the dopaminergic system and the brain regions implicated in pain processing, and perturbations in dopaminergic tonus in these areas could lead to motor and sensory abnormalities [13]. Moreover, a small fiber pathology occurs in the early stage of PD and may contribute to some non-motor symptoms including pain [14]. Pain in PD is often associated with motor fluctuations and wearing-off, and its intensity may also fluctuate during the day [15].
Although the involvement of dopamine in the central modulation of pain is well established, other neurotransmitters, including glutamate, play an important role in pain signals, as suggested by the poor response of non-dystonic pain to levodopa [16]. Elevated glutamatergic neurotransmission is observed during neuropathic pain, and an imbalance between dopaminergic and non-dopaminergic systems might contribute to chronic pain in PD [17]. Moreover, deep brain stimulation targeted to the subthalamic nucleus was shown to reduce the glutamatergic overstimulation of the globus pallidus and improve the musculoskeletal and central neuropathic pain [18].
The results of this post hoc analysis showed that the positive effects of safinamide on pain observed after 6 months were maintained over 2 years.
The add-on of safinamide 100 mg/day to a stable dose of levodopa (alone or in combination with other dopaminergic treatments) was associated with a reduction of the number of concomitant pain treatments of about 26% and a significant improvement in the PDQ-39 “Bodily discomfort” domain and in the two items related to musculoskeletal and neuropathic pain.
These results may be explained by both the dopaminergic and non-dopaminergic mechanism of action of safinamide. Safinamide, in fact, is not just another MAO-B inhibitor, but also modulates the glutamatergic hyperactivity through the state-dependent inhibition of sodium channels [19].
The improvements in motor fluctuations due to the MAO-B inhibition could certainly contribute to the benefits observed. There is, in fact, a significant correlation between pain and motor complications (fluctuations and dyskinesia), and they may share the same pathophysiologic mechanisms; in particular, the non-dopaminergic neurotransmitter systems (including glutamate) may contribute to both motor complications and chronic pain [15].
It is also known that sodium channel blockers have great efficacy against neuropathic pain [20], and drugs that modulate glutamate release, including NMDA antagonists, decrease nociceptive transmission [21]. Moreover, rotigotine, which is solely a dopamine receptor agonist, has been recently found to have no clinically significant effects on chronic pain in PD patients [22].
Some limitations must be considered in this post hoc analysis: the original trials were not designed to investigate pain as a primary endpoint. For this reason, it was not possible to differentiate between the different types of pain, and some therapies commonly used in routine clinical practice for the treatment of pain were not allowed. These findings should therefore be considered as exploratory and must be confirmed in larger clinical trials.
Conclusion
Chronic pain is one of the most frequent and bothersome non-motor symptoms in PD, present since the early stages of the disease in a large proportion of patients [23].
There is growing evidence of the involvement of the basal ganglia in somatosensory and pain modulation, and motor complications and pain may share common pathophysiologic mechanisms that include not only dopaminergic but also non-dopaminergic systems dysfunction, such as glutamatergic hyperactivity. Therefore, glutamatergic neurotransmission is considered a potential focus for pharmacotherapy in PD, and drugs that modulate glutamate release may be a promising option for the treatment of PD chronic pain [24].
Despite some limitations, the results of these analyses suggest that safinamide 100 mg/day may have positive effects on chronic pain, maintained in the long term, which might be explained by the improvement of motor fluctuations due to MAO-B inhibition and by the modulation of glutamatergic hyperactivity. Further investigation with a large-scale confirmatory study is needed to fully evaluate the efficacy of safinamide on PD chronic pain.
References
Martinez-Martin P, Rodriguez-Blazquez C, Kurtis MM, Chaudhuri KR. The impact of non-motor symptoms on health-related quality of life of patients with Parkinson’s disease. Mov Disord. 2011;26:399–406.
Wasner G, Deuschl G. Pains in Parkinson’s disease: many syndromes under one umbrella. Nat Rev Neurol. 2012;8:284–94.
Beiske AG, Loge JH, Rønningen A, Svennsson E. Pain in Parkinson’s disease: prevalence and characteristics. Pain. 2009;141:173–7.
Cattaneo C, Barone P, Bonizzoni E, Sardina M. Effects of safinamide on pain in fluctuating Parkinson’s disease patients: a post hoc analysis. J Parkinsons Dis. 2017;7(1):95–101.
Borgohain R, Szasz J, Stanzione P, Meshram C, et al. Two-year, randomized, controlled study of safinamide as add-on to levodopa in mid to late Parkinson’s disease. Mov Disord. 2014;29(10):1273–80.
Borgohain R, Szasz J, Stanzione P, Meshram C, et al. Randomized trial of safinamide add-on to levodopa in Parkinson’s disease with motor fluctuations. Mov Disord. 2014;29(2):229–37.
Munazza S, Ford B. Management of pain in Parkinson’s disease. CNS Drugs. 2012;26:937–48.
Parkinson J. An essay on the shaking palsy. London: Whittingham and Rowland; 1817.
Nègre-Pagès L, Regragui W, Bouhassira D, Grandjean H, Rascol O. DoPaMiP Study Group. Chronic pain in Parkinson’s disease: the cross-sectional French DoPaMiP survey. Mov Disord. 2008;23:1361–9.
Truini A, Frontoni M, Cruccu G. Parkinson’s disease related pain: a review of recent findings. J Neurol. 2013;260:330–4.
Shearer J, Green C, Counsell CE, Zajicek JP. The impact of motor and non motor symptoms on health state values in newly diagnosed idiopathic Parkinson’s disease. J Neurol. 2012;259:462–8.
Brefel-Courbon C, Grolleau S, Thalams C, Bourrel L, et al. Comparison of chronic analgesic drugs prevalence in Parkinson’s disease, other chronic diseases and the general population. Pain. 2009;141:14–8.
Cury RG, Galhardoni R, Fonoff ET, Perez Lloret S, et al. Sensory abnormalities and pain in Parkinson disease and its modulation by treatment of motor symptoms. Eur J Pain. 2016;20:151–65.
Nolano M, Provitera V, Manganelli F, Iodice R, et al. Loss of cutaneous large and small fibers in naïve and L-dopa treated PD patients. Neurology. 2017;89:776–84.
Tinazzi M, Del Vesco C, Fincati E, Ottaviani S, Smania N, et al. Pain and motor complications in Parkinson’s disease. J Neurol Neurosurg Psychiatry. 2006;77:822–5.
Defazio G, Berardelli A, Fabbrini G, Martino D, et al. Pain as a nonmotor symptom of Parkinson disease: evidence from a case-control study. Arch Neurol. 2008;65:1191–4.
Chudler EH, Dong WK. The role of the basal ganglia in nociception and pain. Pain. 1995;60:3–38.
Kim HJ, Paek SH, Kim JY, Lee JY, et al. Chronic subthalamic deep brain stimulation improves pain in Parkinson disease. J Neurol. 2008;255(12):1889–94.
Salvati P, Maj R, Caccia C, Cervini MA, Fornaretto MG, et al. Biochemical and electrophysiological studies on the mechanism of action of PNU-151774E, a novel antiepileptic compound. J Pharmacol Exp Ther. 1999;288:1151–9.
Miladinovic T, Nashed MG, Sungh G. Overview of glutamatergic dysregulation in central pathologies. Biomolecules. 2015;5:3122–41.
Bleakman D, Alt A, Nisenbaum ES. Glutamate receptors and pain. Semin Cell Dev Biol. 2006;17(5):592–604.
Rascol O, Zesiewicz T, Chaudhuri KR, Ashgarnejad M, et al. A randomized controlled exploratory pilot study to evaluate the effect of rotigotine transdermal patch on Parkinson’s disease-associated chronic pain. J Clin Pharm. 2016;56(7):852–61.
Chaudhuri KR, Shapira AH. Non-motor symptoms of Parkinson’s disease: dopaminergic pathophysiology and treatment. Lancet Neurol. 2009;8(5):464–74.
Fox SH. Non-dopaminergic treatments for motor control in Parkinson’s disease. Drugs. 2013;73:1405–15.
Acknowldgements
We thank the participants in the study.
Funding
The sponsor (Zambon SpA) funded the study, article processing charges and Open Access fee.
Authorship
All authors had full access to all of the data in this study and take complete responsibility for the integrity of the data and accuracy of the data analysis. All named authors meet the International Committee of Medical Journal Editors (ICMJE) criteria for authorship for this article, take responsibility for the integrity of the work as a whole, and have given their approval for this version to be published.
Disclosures
Jaime Kulisevsky is member of the Scientific Advisory Board of Zambon SpA. Carlo Cattaneo is an employee at Zambon SpA, the pharmaceutical company marketing safinamide in Europe. Viviana Tubazio is an employee at Zambon SpA, the pharmaceutical company marketing safinamide in Europe. Paola Castellani is an employee at Zambon SpA, the pharmaceutical company marketing safinamide in Europe.
Compliance with Ethics Guidelines
All procedures performed were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards. Informed consent was obtained from all individual participants included in the study.
Data Availability
The data sets during and/or analyzed during the current study are available from the corresponding author on reasonable request.
Open Access
This article is distributed under the terms of the Creative Commons Attribution-NonCommercial 4.0 International License (http://creativecommons.org/licenses/by-nc/4.0/), which permits any noncommercial use, distribution, and reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made.
Author information
Authors and Affiliations
Corresponding author
Additional information
Enhanced content
To view enhanced content for this article go to https://doi.org/10.6084/m9.figshare.5938972.
Rights and permissions
Open Access This article is distributed under the terms of the Creative Commons Attribution 4.0 International License (https://creativecommons.org/licenses/by/4.0), which permits use, duplication, adaptation, distribution, and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made.
About this article
Cite this article
Cattaneo, C., Kulisevsky, J., Tubazio, V. et al. Long-term Efficacy of Safinamide on Parkinson’s Disease Chronic Pain. Adv Ther 35, 515–522 (2018). https://doi.org/10.1007/s12325-018-0687-z
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12325-018-0687-z