Abstract
Introduction
About 50% of patients do not take their long-term therapy for chronic conditions as prescribed. Many studies have centered on patients’ adherence to a specific treatment or single conditions, but few have taken all chronic conditions into consideration from a patient’s perspective. This study aims to explore factors that impact on drug compliance and to identify strategies to improve this from the perspective of patients with at least one chronic condition.
Methods
Patients were recruited by healthcare professionals from a hospital pharmacy, four community pharmacies, patient associations, and a primary care center in Barcelona. Five focus groups were conducted (N = 36). Conversations were audiotaped and transcribed verbatim to allow qualitative analysis.
Results
Study subjects were aged 39–90 years (mean 65 years) and the mean number of comorbidities per patient was 2.3 (range 1–7). The main modifiers of therapeutic conduct were: patients’ health beliefs, patient–prescriber relationships, and patients’ motivation and perception of illness control. Study participants wanted greater participation in decision-making concerning their health and increased education about their illness and medication. They also wanted individualized healthcare that took their preferences and personal and emotional issues into account.
Conclusion
Our results highlight how the patient–prescriber’s relationship and factors such as health beliefs, motivation and perception of illness control impact on medication adherence in chronic patients. Future interventions to optimize adherence to treatment should focus on shared decision-making and more extensive health education.
Funding
Celgene Corporation.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Background
Medication adherence is a complex and dynamic behavior that has been linked to many aspects, such as socio-economic status, the healthcare team and the healthcare system, condition-related factors, therapy-related factors, and patient-related factors [1–3]. It has been estimated that about 50% of patients do not take their long-term therapy for chronic conditions as prescribed [1, 2, 4]. Such non-adherence to medication is a major public health problem. It has significant negative consequences on both patients and providers, such as loss of treatment effectiveness and increases in healthcare costs [5]. Consequently, in view of the increasing prevalence of chronic diseases, there is a clear need to tackle medication non-adherence. In Catalonia, as in many other regions in developed countries, the prevalence of chronic conditions is growing rapidly. Updated demographic data shows that 38% of its population has at least one chronic condition and this percentage reaches 82.8% of people over 75 years old [6].
The topic of medication adherence has been largely reviewed through qualitative and quantitative studies meaning a large number of risk factors that play a role as barriers or facilitators for medication adherence have been identified. However, many studies have centered on patients’ adherence to a specific treatment or single conditions [7–13], but few have taken all chronic conditions into consideration from a patient’s perspective [14, 15]. Due to the increasing burden of chronic illness and prevalence of patients with comorbidities, it is important to study medication adherence not only in patients with single conditions, but also with coexisting chronic diseases.
To better understand medication adherence and design interventions to improve it, it can be useful to examine health behaviors. No single theory can explain medication non-adherence adequately since each one has its own advantages and disadvantages. A conceptual framework developed by combining aspects from various theories can provide a better understanding of this topic. Communicative theories consider that an equal relationship between patient and physician can improve adherence. However, a change in adherence behavior is not guaranteed since these theories do not take into consideration patients’ attitudes and beliefs [16]. From the cognitive perspective, there are some theories such as the health belief model and the theory of reasoned action that focus on behavior change and consider that patients’ attitudes, beliefs, and expectancies of outcomes are major determinants of health behaviors including medication adherence [17, 18]. Furthermore, these theories suggest that patients act in the way most likely to achieve positive health outcomes according to their beliefs. The common sense self-regulatory model proposes that individuals form cognitive representations of “illness representation” through five dimensions: causality, consequences, controllability, identity, and timeline [19]. According to this theory, medication adherence is based on a patient’s cognitive factors and planning. This theory assumes that people are active, self-regulating problem solvers.
To gain insight into what factors act as a barriers or facilitators of medication adherence from a holistic approach and what interventions may enhance patients’ health behaviors to adherence conducts, it may be useful to perform qualitative research.
Objective
As part of a larger project on medication adherence, we conducted a qualitative study to explore factors that impact on drug compliance and to identify strategies to improve it from the perspective of patients with at least one chronic condition in the city of Barcelona.
Methods
Setting
The study took place in within a regional health area at a tertiary hospital in the city of Barcelona (Catalonia, Spain). Through a literature review, we identified the most interesting key informants for a first approach to the study subject and to help in the design of the discussion guide to conduct focus groups. Consequently, we conducted eight semi-structured interviews to a primary care physician, a primary care nurse, a community pharmacist, a member of the Spanish Adherence Observatory, and four patients with varying levels of medication adherence. They helped identify the dimensions to be discussed during focus group development. We chose focus group methodology because this technique enables discovering variety within a population, in other words, obtaining a broad range of views on a specific topic over a relatively short period of time as opposed to in-depth interviews [20]. Furthermore, group interaction allows participants to clarify and explore common perspectives.
The study protocol was approved by the ethics committee of Hospital de la Santa Creu i Sant Pau and was in accordance with the 1964 Helsinki declaration and its later amendments. Informed consent was obtained from all individual participants included in the study.
Patient Recruitment and Conduction of Focus Groups
The inclusion criteria for participating in the focus groups were patients receiving medication for one or more chronic diseases. We excluded patients <18 years old, patients with cognitive impairment, patients with uncontrolled mental conditions, and patients with no chronic disease. We used a purposive and theoretical sampling strategy and applied the purposeful selection as an initial starting point, to study examples that represent the phenomenon of interest and, ultimately, to facilitate comparison of emerging conceptual categories and theory. Patients fulfilling eligibility criteria were recruited by healthcare professionals (co-investigators and collaborators of the study) from a hospital pharmacy, four community pharmacies, patient associations, and a primary care center in Barcelona. Study subjects did not receive any economic compensation for their participation.
The objective was to have 6–12 participants for each focus group. We divided the groups as much as possible into gender and level of comorbidity. Further to this, there were two participants that turned up in the focus group with their partner that also had the role of caregiver. As they also met inclusion criteria, the members of the investigation team considered that their point of view could be useful and could enrich the discussion as they were both patient and caregiver. The reason to split up groups into these two variables was to determine if a comparative assessment into a wider spectrum of pathologies could help determine the impact of gender factors and complex comorbidity towards adherence. As well as this, we also conducted a mixed group to determine whether there were speech divergences between male and female participants.
Focus group sessions were conducted by two members of the research team and lasted for about 2 h or until saturation of responses was reached. One member acted as a moderator and asked open-ended questions (see Appendix 1 in the supplementary material) while the other member took detailed notes during each group discussion. All focus group sessions were audiotaped and transcribed verbatim.
Study Analysis
The research team fragmented the texts of the audiotapes, coded passages and performed inductive categorization. Recurring themes and discourse divergences were identified. When the investigators had a complete study overview, they met for discussion to reach a consensus on emerging themes and made a thematic content analysis.
Patients’ quotations were translated from Catalan or Spanish into English by a native speaker.
Results
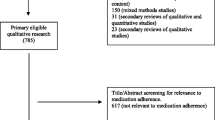
Sixty-three people were contacted to participate in the study. Sixteen declined to take part in the study and 13 were not located when organizing focus groups. Finally, 36 people took part in five focus groups (19 females, 17 males) between December 2014 and February 2015. Study subjects were aged 39–90 years (mean 65 years) and the mean number of comorbidities per patient was 2.3 (range 1–7). Participants’ conditions are shown in Table 1.
Below, we present a brief review that offers some insight into what life with chronic conditions involves, and how patients’ adherence perception is affected by its constructs. We structured the results of the focus groups into three major topics: patients’ health beliefs, patients’ health experiences, and patients’ health behaviors related to medication adherence and therapeutic attitudes. Table 2 lists a summary of the factors identified in our study that impact on medication adherence with representative quotations of study participants.
Patients’ Health Beliefs
Patients with multimorbidity had the perception of a main disease (that which most affects their quality of life or threatens survival) and the rate of medication adherence to treat it was usually higher. On some occasions, patients made decisions based on their own perceived effect of the drug. The beliefs that affected medication adherence and were expressed by study participants were concerning drugs, drug prescription, expectancies of treatment effectiveness, and relative to non-pharmacologic therapies.
Some study patients expressed beliefs that led them to non-adherent conducts such as considering drugs as chemicals or toxic products and that they create a vicious cycle, and a confidence in spontaneous organic recovery without treatment.
Study participants showed a clear preference not to take any medication, but they accepted it with a certain feeling of defeat and resignation. They considered that medication was often prescribed routinely and that health professionals did not contemplate possible changes in health status so as to reduce drug dose. They felt that in some way, a drug prescription was a consequence of a lack of time or resources for other types of treatments. Some of them identified the pill burden as a trend imposed by the health system as an alternative to tailoring treatment. Polymedicated patients wanted to prioritize drugs regarded as essential for survival and to maintain a good quality of life. From their point of view, doctors should review their medications regularly to see whether they are still necessary. Patients also disagreed with the responsibility transfer currently occurring in healthcare; they felt disease was attributed as their fault due to a lack of preventive measures and self-care activities. Adherence behavior was also influenced by patient’ expectancies of treatment outcomes. Although, many study subjects were conscious their illness could not be cured, they expected an improvement in their quality of life. Consequently, despite initial skepticism and reluctance, if their perception of their health status was good, their trust in treatment was solid.
Although this was not a general opinion, some participants commented on the possible use of non-pharmacologic therapies. They called these therapies complementary or alternative depending on their confidence in drugs. In some cases, the use of these therapies was due to the subjective perception of drug ineffectiveness and worsening of patient’s quality of life.
Patients’ Health Experiences
The vast majority of study patients highlighted the importance of the prescriber–patient relationship. Patients’ trust in treatment could vary depending on how they perceived the prescriber’s attitude, especially in the initial phases. Once mistrust was established, patients were more likely to adopt skeptical attitudes and non-adherent behaviors. Study participants also pointed out the persistence of a paternalistic model in the doctor–patient relationship, known to be one of the main barriers for patients to acquire responsibility for their medication. They considered that specialists had excellent clinical skills, but lacked empathy towards patients. They also felt a lack of therapeutic negotiation during medical visits. In other words, patients wanted to take some responsibility for their medication under guidance of their physicians so some of them considered therapeutic alliance a good strategy to empower them.
Study patients especially appreciated a treatment that could increase their autonomy. They stated that when suffering from a chronic illness the conciliation between medication and their daily life influences therapeutic adherence, especially in patients with low comorbidity because of constant journeys to healthcare centers. Patients also worried about the impact of treatment on their professional careers and family life.
In our study population, patients’ perception of disease control appeared to motivate medication adherence especially in patients with high comorbidity. Body-listening, related to the response of symptoms, was an important part of this process, the ‘guiding light’ through which it is possible to determine if the patient’s treatment experience is good or must be changed. Each participant faced multiple and diverse challenges in order to balance the prescribed regimen with physical and psychosocial wellbeing whilst trying to maintain quality of life. If treatment duration was long and if patients did not perceive therapeutic effectiveness their motivation could decrease and thus their adherence to treatment. This was especially significant in those patients suffering from several comorbidities. Furthermore, treatment characteristics such as dosage form, pill burden and presence of adverse effects could modify therapeutic conduct. Those treatments that affect physical appearance (for instance, increasing body weight) were reported by some female participants to be causes of non-adherence. Therapeutic complexity was also identified as a cause of non-intentional non-adherence by patients with polypharmacy and high level of comorbidity.
Study participants also stressed the importance of patient’s education and claimed that more complete information would improve therapeutic adherence. Most patients said that a lack of knowledge about how drugs work and their adverse effects increased their fear of the nature of the drugs and their distrust in medicine. As a result, information was identified as a central element that allows patients to deal better with their illness. Patients took great value from explanations given by health professionals as to how their drugs worked as this helped to increase their confidence in the treatment. Generally speaking, patients showed a clear interest in being involved in decision-making throughout the therapeutic process if they received adequate information.
Family and social support were very important for many patients because they helped in illness control. This support was expressed in terms of accompaniment and not helping in the administration of drugs. Sometimes this support came from patients in similar situations. Contrary to the majority, one participant reported that today’s society expected chronic patients to lead a normal life even if their body did not allow them to.
Patient’ Health Behaviors
In this study, we identified three attitudes to therapy: responsibility, prevention, and defeat. The attitude of responsibility was expressed by some female patients and by a need to have a more proactive role in the management of their health status. We also observed that when a patient is also a caregiver, this attitude is dominated by surveillance of the other person’s medication adherence rather than that of self. Many other patients showed a prevention attitude that was strongly linked to a desire to prevent future complications and to maintain a good health status. This was more common in women, and also in men with polypharmacy or with high functional impairment. Patients with this attitude also tended to have a more active role in their own care. Only few patients (those with AIDS and epilepsy) had a defeatist attitude and this was determined by the high level of social stigmatization associated with these diseases that led to not accepting the disease. This attitude might account for the lack of adaptation to therapeutic routine and the commitment and the self-sacrifice needed for following a treatment. Consequently, it could lead to a suboptimal adherence.
In our study, collaborating actively to achieve a better health status appeared to generate greater security among patients. Participants with healthy lifestyles and habits tended to have adequate conduct towards medication. Therefore, patients’ motivation could enhance medication adherence.
Suggestions for Improving Medication Adherence
Participants were also asked what helped them to follow a treatment or improve medication adherence (Table 3). Most of the suggestions were centered on improving patients’ education and the relationship or the attention they received from their prescriber. Participants also complained about the little attention given to mental health status in medical visits. They sought greater clinical support concerning emotional aspects and would like a holistic approach, taking their preferences and family context into account.
Discussion
This study was motivated by the need to understand chronic patients’ perspectives about medication adherence. Knowing why patients do not adhere to their treatments is important for promoting adherence and modifying the therapeutic regimen according to their needs. Living with a chronic disease encompasses multiple and complex behaviors that patients must incorporate in their daily routine and are determined by multiple factors and modifiers. From this perspective, the individual experience of adherence can be understood as a continual evaluation by the patient in terms of assessing the effectiveness of the prescribed treatments in recovering their normal daily life after disease onset. Treatment process was related by participants as continuous in time but a dynamic experience. In other words, a personal experience that varies according to the individual’s disease and therapeutic process experience. Long-term treatment is sometimes perceived by chronic patients as a burden and loss, but on other occasions as an opportunity to recover health status and improve quality of life.
In our study, separating some focus groups by gender and level of comorbidities meant investigators were able to find some differences. Until now, some research linked female gender to a better adherence conduct [21–26], whereas other studies suggested the opposite [27, 28] and some other studies found no relationship between gender and therapeutic adherence [29, 30]. Our results showed that some female patients took both a responsible and preventative attitude, whereas this was absent in men with the exception of those with polypharmacy or high functional impairment. For a patient with multiple comorbidities, treatment over a longer duration was perceived as worse, if it was not accompanied by good clinical outcomes, than in a patient with few conditions. This could lead to non-adherence behavior. In contrast, patients with few comorbidities were more concerned about the conciliation of personal life than with the duration of the treatment due to the constant follow-up at healthcare centers.
Our research allowed us to identify several modifiers of therapeutic conduct. The most important modifiers for our patients were: their health beliefs, the patient–prescriber relationship, their motivation, and their perception of illness control. However, there were other factors involved in medication adherence identified such as: patients’ fears, patients’ education about treatment, family and social support and patients’ personality (or attitudes).
Patients’ beliefs about treatment are the starting point of adherence and non-adherence conduct. Beliefs and misbeliefs influence both intentional and unintentional adherence. On many occasions, the pattern of therapeutic non-compliance in our participants responded to health beliefs of overmedication, pharmacological dependence, or disease non-acceptance. Several participants also recognized that certain situations triggered a non-compliant conduct towards treatment: a perceived lack of satisfactory results following initial expectations, a fear of side effects, and emotional tiredness from high pill burden. Cognitive theories such as health belief model and the theory of planned behavior assume that if patients are provided with the logical understanding of the benefits and risks of taking medications, they will be better adherent with the medications. Consequently, health professionals need to engage with chronic patients and communicate with them regarding their health beliefs and provide them with the adequate information about their illness and treatment in order to increase positive health results.
Subjects also sought a therapeutic balance between the impossibility to cure their illness, the dosage schedule, and their quality of life. Due to this, treatment effectiveness has been expressed as a search for the best match between the right dosage and patient’s expectations. Managing patients’ fears and tailoring drug treatment to patients’ needs and preferences during medical visits might improve adherence to medication as some patients reported.
Other factors involved in medication adherence that emerged from this study and coincide with numerous other studies were confidence towards prescribers and the patient–prescriber relationship [31, 32]. The greater the confidence in the prescriber, the greater the confidence in treatment. Many patients wanted more complete information and education from healthcare professionals so as to be more involved in their own treatment. They would like to change the paternalistic model in healthcare assistance for a model where they could negotiate their treatment and the goals to achieve with their prescriber. This topic of therapeutic alliance has been largely studied in the field of psychotherapy and many studies indicate that it plays a major role as a good predictor of clinical outcome [33]. It helps both healthcare professionals and patients to work together effectively. The literature has also described the relationship between good medication adherence and therapeutic alliance. However, most studies to date have been mainly performed in psychiatric conditions like schizophrenia and bipolar disorder [34, 35].
Many participants also stressed their dislike of drugs being prescribed routinely and stated a lack of emotional support during medical visits in our healthcare system. For this reason, they expressed the need for a holistic approach to achieve health attention more centered to person. This aspect is related to patient–prescriber communication and this relationship could explain why the number of people who trust in complementary and alternative medicines is increasing [36].
Patients with high comorbidities aimed not to cure their disorder but to improve their quality of life. When patients had a greater perception of control of their disease, quality of life and side effects, there was a greater tendency to follow a correct therapeutic conduct. Some patients complained of the discipline required to follow a treatment. This can lead to a non-adherent conduct if they do not perceive positive outcomes.
Limitations
The main limitation of this study is its qualitative nature that does not allow the results to be generalized. However, this was not a purpose of the study since we wanted to explore and to obtain rich and detailed information about modifiers of medication adherence in our health area. With this information, we want to later design and conduct a survey to determine the impact of the factors identified in this qualitative research in a wider and representative sample of chronic patients.
Although this was a relatively adherent population, as this was a qualitative study it can be an advantage that study participants had a common reality to avoid a polarization during discussion that would have prevented from advancing the discussion. Furthermore, many participants expressed a good adherence conduct when it referred to following a drug treatment, but not when they had to change their diet or exercise habits. And we know that for reaching positive health outcomes in some conditions, it is as important to engage in drug treatment as it is a change in a patient’s lifestyle.
In addition, all participants lived in an urban area and none of them were immigrants, which possibly influenced beliefs and opinions related to therapeutic adherence.
Conclusions
Patients’ health beliefs, patient–prescriber relationships, and patient’s motivation and perception of illness control are important modifiers of therapeutic adherence in our study population from a regional health area in Barcelona. Therapeutic alliance, shared decision-making and better education about their illness and treatments appear to be the main strategies to improve medication adherence in patients with chronic diseases.
Practical Implications
This study helps to understand patients’ attitudes and feelings towards their chronic medication and illustrate that future interventions to improve medication adherence should focus on therapeutic alliance and reinforcement of patient education. The factors identified in this study will be the basis to design a survey about what factors impact on medication adherence in a wider sample of patients affected by chronic conditions in the same regional health area using a quantitative approach.
References
Sabaté E. Adherence to long-term therapies: evidence for action. Geneva: World Health Organization; 2003. http://www.who.int/chp/knowledge/publications/adherence_introduction.pdf. Accessed 9 March 2016.
Osterberg L, Blaschke T. Adherence to medication. N Engl J Med. 2005;353(5):487–97. doi:10.1056/NEJMra050100.
Kardas P, Lewek P, Matyjaszczyk M. Determinants of patient adherence: a review of systematic reviews. Front Pharmacol. 2013;4(July):1–16. doi:10.3389/fphar.2013.00091.
Brown MT, Bussell JK. Medication adherence: WHO cares? Mayo Clinic Proc. 2011;86(4):304–14. doi:10.4065/mcp.2010.0575.
Simpson SH. A meta-analysis of the association between adherence to drug therapy and mortality. BMJ. 2006;333(7557):15. doi:10.1136/bmj.38875.675486.55.
Constante C. Enquesta de salut de Catalunya 2014. Informe dels principals resultats. [Catalan Health Survey 2014]. http://salutweb.gencat.cat/web/.content/home/el_departament/estadistiques_sanitaries/enquestes/onada09/esca2014_resultats.pdf. Accessed 9 March 2016.
Gascón JJ, Sánchez-Ortuño M, Llor B, Skidmore D, Saturno PJ. Why hypertensive patients do not comply with the treatment: results from a qualitative study. Fam Pract. 2004;21(2):125–30. doi:10.1093/fampra/cmh202.
Jones RCM, Hyland ME, Hanney K, Erwin J. A qualitative study of compliance with medication and lifestyle modification in chronic obstructive pulmonary disease (COPD). Prim Care Respir J. 2004;13(3):149–54. doi:10.1016/j.pcrj.2004.05.006.
Raynor DK, Savage I, Knapp P, Henley J. We are the experts: people with asthma talk about their medicine information needs. Patient Educ Couns. 2004;53(2):167–74. doi:10.1016/S0738-3991(03)00126-5.
Fung V, Sinclair F, Wang H, Dailey D, Hsu J, Shaber R. Patients’ perspectives on nonadherence to statin therapy: a focus-group study. Perm J. 2010;14(1):4–10.
Iversen MD, Vora RR, Servi A. Factors affecting adherence to osteoporosis medications: a focus group approach examining viewpoints of patients and providers. J Geriatr Phys Ther. 2011;34(2):72–81. doi:10.1097/JPT.0b013e3181ff03b4.
Monroe AK, Rowe TL, Moore RD, Chander G. Medication adherence in HIV-positive patients with diabetes or hypertension: a focus group study. BMC Heal Serv Res. 2013;13:488. doi:10.1186/1472-6963-13-488.
White S, Bissell P, Anderson C. A qualitative study of cardiac rehabilitation patients’ perspectives on making dietary changes. J Hum Nutr Diet [Internet]. BMC Health Serv Res 2011;24(2):122–7. doi:10.1111/j.1365-277X.2010.01136.x.
Mishra SI, Gioia D, Childress S, Barnet B, Webster RL. Adherence to medication regimens among low-income patients with multiple comorbid chronic conditions. Health Soc Work. 2011;36(4):249–58.
Laba T-L, Lehnbom E, Brien J-A, Jan S. Understanding if, how and why non-adherent decisions are made in an Australian community sample: a key to sustaining medication adherence in chronic disease? Res Soc Adm Pharm. 2015;11(2):154–62. doi:10.1016/j.sapharm.2014.06.006.
Leventhal H, Cameron L. Behavioral theories and the problem of compliance. Patient Educ Couns. 1987;10(2):117–38.
Rosenstock IM, et al. A National Study of Health Attitudes and Behavior. Ann Arbor: The University of Michigan, School of Public Health; 1965.
Fishbein MAI. Belief, attitude intention and behaviour: an introduction to theory and research. Menlo Park: Addison-Wesley; 1975.
Leventhal H, Benyamini Y, Brownlee S, et al. Illness representations: theoretical foundations. In: Petrie KJ, Weinman JA, editors. Perceptions of health and illness. Amsterdam: Harwood Academic; 1997. p. 19–45.
Mack N, Woodsong C, MacQueen KM, Guest G, Namey E. Qualitative research methods: a data collector’s field guide. Family Health International (FHI). North Carolina, USA; 2005. p. 51–2.
Balbay O, Annakkaya AN, Arbak P, Bilgin C, Erbas M. Which patients are able to adhere to tuberculosis treatment? A study in a rural area in the northwest part of Turkey. Jpn J Infect Dis. 2005;58(3):152–8.
Choi-Kwon S, Kwon SUKJ. Compliance with risk factor modification: early-onset versus late-onset stroke patients. Eur Neurol. 2005;54(4):204–11. doi:10.1159/000090710.
Fodor GJ, Kotrec M, Bacskai K, Dorner T, Lietava J, Sonkodi S, et al. Is interview a reliable method to verify the compliance with antihypertensive therapy? An international central-European study. J Hypertens. 2005;23(6):1261–6.
Kiortsis DN, Giral P, Bruckert ETG. Factors associated with low compliance with lipid-lowering drugs in hyperlipidemic patients. J Clin Pharm Ther. 2000;25(6):445–51.
Lertmaharit S, Kamol-Ratankul P, Sawert H, Jittimanee S, Wangmanee S. Factors associated with compliance among tuberculosis patients in Thailand. J Med Assoc Thai. 2005;88(Suppl 4):S149–56.
Lindberg M, Ekström T, Möller MAJ. Asthma care and factors affecting medication compliance: the patient’s point of view. Int J Qual Heal Care. 2001;13(5):375–83.
Frazier PA, Davis-Ali SH, Dahl KE. Correlates of noncompliance among renal transplant recipients. Clin Transplant. 1994;8(6):550–7.
Sung JC, Nichol MB, Venturini F, Bailey KL, McCombs JSCM. Factors affecting patient compliance with antihyperlipidemic medications in an HMO population. Am J Manag Care. 1998;4(10):1421–30.
Ghods AJND. Noncompliance with immunnosuppressive medications after renal transplantation. Exp Clin Transpl. 2003;1(1):39–47.
Senior V, Marteau TM, Weinman J, Genetic Risk Assessment for FH Trial (GRAFT) Study Group. Self-reported adherence to cholesterol-lowering medication in patients with familial hypercholesterolaemia: the role of illness perceptions. Cardiovasc Drugs Ther. 2004;18(6):475–81. doi:10.1007/s10557-004-6225-z.
Chambers JA, O’Carroll RE, Hamilton B, Whittaker J, Johnston M, Sudlow C, et al. Adherence to medication in stroke survivors: a qualitative comparison of low and high adherers. Br J Health Psychol. 2011;16(3):592–609. doi:10.1348/2044-8287.002000.
Gordon K, Smith F, Dhillon S. Effective chronic disease management: patients’ perspectives on medication-related problems. Patient Educ Couns. 2007;65(3):407–15.
Ardito RB, Rabellino D. Therapeutic alliance and outcome of psychotherapy: historical excursus, measurements, and prospects for research. Front Psychol. 2011;2:270. doi:10.3389/fpsyg.2011.00270.
Sylvia LG, Hay A, Ostacher MJ, Miklowitz DJ, Nierenberg AA, Thase ME, et al. Association between therapeutic alliance, care satisfaction, and pharmacological adherence in bipolar disorder. J Clin Psychopharmacol. 2013;33(3):343–50. doi:10.1097/JCP.0b013e3182900c6f.
Zeber JE, Copeland LA, Good CB, Fine MJ, Bauer MS, Kilbourne AM. Therapeutic alliance perceptions and medication adherence in patients with bipolar disorder. J Affect Disord. 2008;107(1–3):53–62. doi:10.1016/j.jad.2007.07.026.
Nilsson J, Kallman M, Ostlund U, Holgersson G, Bergqvist M, Bergstrom S. The use of complementary and alternative medicine in Scandinavia. Anticancer Res Greece. 2016;36(7):3243–51.
Acknowledgments
This study was funded by Celgene Corporation. The sponsor had no involvement in data collection, analysis, interpretation of the study or writing of the report. All named authors meet the International Committee of Medical Journal Editors (ICMJE) criteria for authorship for this manuscript, take responsibility for the integrity of the work as a whole, and have given final approval to the version to be published. The authors thank Carolyn Newey for English assistance.
Disclosure
Neus Pagès-Puigdemont, Maria Antònia Mangues, Montserrat Masip, Giovanna Gabriele, Laura Fernández-Maldonado, Sergi Blancafort, and Laura Tuneu declare that they have no conflict of interest.
Compliance with Ethics Guidelines
All procedures followed were in accordance with the ethical standards of the responsible committee on human experimentation (institutional and national) and with the Helsinki Declaration of 1964, as revised in 2013. Informed consent was obtained from all patients for being included in the study.
Open Access
This article is distributed under the terms of the Creative Commons Attribution-NonCommercial 4.0 International License (http://creativecommons.org/licenses/by-nc/4.0/), which permits any noncommercial use, distribution, and reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made.
Author information
Authors and Affiliations
Corresponding author
Additional information
Enhanced content
To view enhanced content for this article go to http://www.medengine.com/Redeem/0AE4F06044A472AD.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is distributed under the terms of the Creative Commons Attribution 4.0 International License (https://creativecommons.org/licenses/by/4.0), which permits use, duplication, adaptation, distribution, and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made.
About this article
Cite this article
Pagès-Puigdemont, N., Mangues, M.A., Masip, M. et al. Patients’ Perspective of Medication Adherence in Chronic Conditions: A Qualitative Study. Adv Ther 33, 1740–1754 (2016). https://doi.org/10.1007/s12325-016-0394-6
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12325-016-0394-6