Abstract
Rosacea is a common, chronic inflammatory skin disease that can present with a variety of signs and symptoms. The potentially simultaneous occurrence of different signs and symptoms is due to different underlying inflammatory pathways, emphasizing the need for complementary treatment approaches. Topical ivermectin cream (10 mg/g) and systemic, oral anti-inflammatory doxycycline (40 mg modified-release) are both approved for the treatment of papulopustular rosacea (PPR). Whether or not a combined therapeutic approach may be more beneficial than monotherapy for patients with PPR remains to be tested. Here, we summarize underlying inflammatory pathways implicated in rosacea and clarify the impact of these two agents on selective pathways during inflammation, due to specific characteristics of their individual mechanisms of action (MoA). Based on the complementary MoA of doxycycline modified-release and ivermectin, a scientific rationale for a combined therapy targeting inflammatory lesions in rosacea is given. We propose that topical ivermectin cream is a promising new candidate as first-line treatment to target the inflammatory lesions of rosacea, which can be used in combination with systemic doxycycline modified-release to provide an optimal treatment approach considering all inflammatory pathways involved in PPR.
Funding Galderma.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Rosacea is a chronic inflammatory disease characterized by the presence of various signs and symptoms including flushing (transient erythema), persistent erythema, inflammatory papules and pustules (inflammatory lesions), telangiectasia, skin irritation (burning and stinging), etc. These signs and symptoms can occur in isolation or combination [1, 2]. Recommendations for the classification of rosacea into four subtypes based on clinical presentation were proposed in 2002, as follows: erythematotelangiectatic rosacea (ETR); papulopustular rosacea (PPR); phymatous rosacea (PYR); and ocular rosacea (OR). However, patients usually present with a spectrum of symptoms overlapping these subtypes [1, 2]. For example, although PPR is characterized by the presence of lesions (papules, pustules), patients may also additionally present with persistent erythema [2], and if the papules/pustules are cured, the erythema still remains. Furthermore, PYR is observed after or at the same time as PPR and erythema (either transient or persistent) [3, 4]. Symptoms may vary from one week to the next, making the disease unpredictable, which can affect the patient’s quality of life [2, 5]. Finally, scientific evidence indicates that the erythema observed in ETR is an inflammatory process and the underlying cause demands anti-inflammatory therapy [6–10].
Signs and symptoms of rosacea often appear to be triggered by environmental factors, including sun exposure, temperature change, stress, spicy foods, and heavy exercise [11, 12]. Recent epidemiological studies have indicated that rosacea also has a genetic component [6, 13]. Affected rosacea skin exhibits increased sensitivity to these triggers [14]; for example, compared with people with non-lesional skin, individuals with PPR have a significantly lower threshold for temperature-induced pain, resulting in facial hypersensitivity [15]. This is thought to be due to a hyper-responsive immune system and increased levels of proteins involved in inflammatory pathways [14]. Neurovascular and neuro-immune dysregulation may contribute to erythematous changes (flushing, erythema) in rosacea patients, which can impact innate and adaptive immune defense mechanisms [6–9]; whether the autonomic or sensory nervous system (or both) is crucial for the mediation of flushing or erythema is still under debate [16, 17]. A link has also been established between the presence of high levels of Demodex mites (such as D. folliculorum and D. brevis) and rosacea, with signs and symptoms of rosacea potentially resulting from heightened pro-inflammatory skin response [18–24]. Whether the impact of Demodex mites is more quantitative or qualitative, and whether or not Demodex mites play a role in erythema as well as in the development of papules/pustules, is still under investigation.
Despite our current knowledge of trigger factors and potential role of genetics, the etiology of rosacea is yet to be fully elucidated [12]. An important interplay exists between the key mechanisms that are responsible for underlying pathophysiology of the disease, namely innate and adaptive immunity as well as neurovascular dysregulation [4, 14, 25, 26]. These altered pathophysiological inflammatory processes correlate well with the clinical signs/symptoms of the disease. Although they are only partly understood, the correlation between innate and adaptive immunity, in which the infiltrate leads to the development of papules and pustules, has been demonstrated. Because the inflammatory infiltrate in PPR consists of innate immune cells (papules: macrophages, mast cells; pustules: neutrophils) and adaptive immune cells (T helper [Th] 1 and Th17 cells, as well as plasma cells) [6–10], a combination of different drugs that optimally block the various inflammatory pathways may be necessary. This may also be true for the optimal treatment of neurovascular dysregulation, namely flushing (transient erythema) and persistent erythema, for which the underlying mechanisms are still poorly understood. For example, recent data indicate that angiogenesis may not play an important role in the context of erythema [7, 10]. The glandular hyperplasia and fibrotic changes, as observed in PYR, are now seen as a result of chronic inflammatory stimuli, although the pathophysiology of this development on the molecular level is poorly understood [12, 25, 26]. Overall, the various inflammatory cells and pathways involved in the pathophysiology of these overlapping yet distinct signs of rosacea highlight the necessity to implement optimized combination therapies for greater benefit to the patient. This fact is also supported by evidence in other dermatological diseases such as acne or psoriasis, where consensus guidelines recommend the use of a combination of different therapies with complementary mechanisms of action to target multiple pathogenic factors simultaneously [27, 28].
The aim of this review is to discuss the complementary and distinct mechanisms of action (MoA) of topical ivermectin 10 mg/g cream and systemic doxycycline 40 mg modified-release, which could be used in combination to optimize efficacy in the treatment of PPR. From this current evidence, we propose that ivermectin 10 mg/g cream is a promising new candidate as the first-line agent in the treatment of the inflammatory lesions of rosacea which, when used in combination with doxycycline modified-release, could potentially provide an even more effective, faster, and longer-acting treatment approach. This article is based on previously conducted studies and does not involve any new studies of human or animal subjects performed by any of the authors.
Potential Role of the Innate and Adaptive Immune Systems in the Development of Inflammatory Lesions of Rosacea
Innate Immune System Response
The facial skin of people with rosacea-prone skin expresses anomalous levels of certain proteins with an ability to trigger pro-inflammatory pathways and modulate vascular changes (Fig. 1) [16, 29–34]. Histological examination of papulopustular inflammatory lesions has demonstrated both superficial and deep inflammation, consisting of a mixed inflammatory infiltrate containing macrophages, mast cells, Th1/Th17 cells and eosinophils [8], as well as the presence of Demodex mites [12]. Neutrophils are only found in pustules and plasma cells are occasionally present [7, 8, 12].

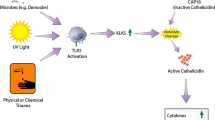
Modified from Yamasaki et al. [29, 30, 34], Two et al. [31], Muto et al. [32], Reinholz et al. [33], and Steinhoff et al. [16]
Innate immune dysfunction in rosacea. Overview of innate immune-mediated inflammatory responses in rosacea. UV light activates the vitamin D pathway, leading to increased levels of cathelicidin. Activation of TLR2 leads to increased levels and activity of KLKs (e.g., KLK5), resulting in increased cleavage of cathelicidin to form LL-37, causing release of pro-inflammatory cytokines; mast cell activation, and macrophage and neutrophil chemotaxis. In response to trigger factors (e.g., stress, spices, exercise, noxious cold, and heat), TRPV1 and/or TRPA1 channels become activated, inducing neuropeptide responses, which activate/amplify the inflammatory response leading to the signs and symptoms of rosacea. KLKs kallikreins, MMPs matrix metalloproteinases, TLR2 toll-like receptor 2, ROS reactive oxygen species, UV ultraviolet.
During the inflammatory process in rosacea, chronic inflammation results in prolonged vasodilation, allowing fluid to leak out. This, in turn, causes edema, infiltration of leukocytes and production of pro-inflammatory cytokines, such as tumor necrosis factor alpha (TNF-α), interleukin (IL)-1, and IL-6, which eventually leak into the dermis [35]. This vascular leakage attracts additional neutrophils, which are recruited by chemotactic factors released from inflamed dermal structures [35]. Leukocytes release nitric oxide (NO), matrix metalloproteinases (MMPs), and reactive oxygen species (ROS), which contribute to chronic vasodilation and dermal matrix degradation [35, 36]. Significantly elevated levels of ROS are responsible for the initiation of several pro-inflammatory processes in the skin, including expression of leukocyte-attracting chemokines, C–C motif chemokine ligand 2 (CCL2), and C-X-C motif chemokine 8 (CXCL8) [37]. During this process, pro-inflammatory cytokines such as TNF-α and IL-1 become upregulated, promoting leukocyte chemotaxis [37]. In addition, the leakage of pro-inflammatory cytokines such as TNF-α and IL-1 into the dermis triggers production of secondary chemokines (including CXCL1, CXCL8, CCL20, and CCL27) in keratinocytes, leading to T cell recruitment into the perifollicular space, contributing to disease progression [37].
Rosacea skin may be more sensitive to specific triggers due to irregular expression of certain proteins, such as toll-like receptor-2 (TLR2), serine protease kallikrein (KLK), and abnormal forms of cathelicidin [2, 29]. Signaling via TLRs upregulates the vitamin D receptor, causing induction of the cathelicidin pathway [34, 38] and increased expression of TLR2, which in turn induces a calcium-dependent increase KLK5 levels in keratinocytes and subsequent increase in serine protease activity by KLK5 [29, 33]. KLK5 activity and post-translational processing cleaves the C-terminal cathelin domain of the inactive precursor of cathelicidin, hCAP18, to give rise to the active peptide LL-37 [36]. Increased cathelicidin expression in rosacea skin promotes leukocyte infiltration and stimulates angiogenesis [30]. MMP cleavage/activation of KLK5 indirectly catalyzes the proteolytic activation of hCAP18 to LL-37; therefore, MMP activation of KLK5 can increase the levels of LL-37, leading to increased inflammation [36]. Inhibition of KLK5 has been linked with a reduction in the occurrence of papules and erythema severity, providing further evidence of this pathway in the pathogenesis of rosacea [39]. This has recently been demonstrated in a clinical setting, with patients with PPR treated with doxycycline 40 mg modified-release showing a decrease in both gene expression and protein levels of MMPs, KLK, and cathelicidin, which resulted in a reduction in inflammatory lesion count and consequently improved clinical outcomes [40].
Mast cells have also been implicated in the pathophysiology of rosacea, with the number of mast cells shown to be elevated in the dermis of rosacea patients presenting with different subtypes [7, 32]. When mast cells in the skin are activated, they secrete proteases such as chymase, tryptase, KLK5, and MMPs, which induce dermal inflammation and increase the production of enzymes in the epidermal layer that generate LL-37, thereby creating a pro-inflammatory loop [32, 41]. In the skin, mast cells are primarily found in the epidermis and dermis in close proximity to keratinocytes and sensory nerves endings; the secretion of proteases, histamine, and pro-inflammatory cytokines by mast cells contributes to the amplification of the skin inflammation, tissue remodeling, and angiogenesis [32].
Increased stratum corneum permeability has been linked to an aggravated innate immune response [26], with barrier impairment causing skin sensitivity in patients with rosacea [42]. Elevated levels of serine proteases can contribute to stratum corneum permeability barrier dysfunction [14]. The innate immune system may be activated as a homeostatic counter-regulatory response to impaired stratum corneum barrier, resulting in increased trans-epidermal water loss (TEWL), and increased expression and secretion of cathelicidin (LL-37) [14]. Compared with control subjects, patients with both PPR and ETR have increased TEWL and heightened reactivity to skin irritation using lactic acid [43]. Individuals with PPR have also been found to have reduced epidermal hydration and a more alkaline centro-facial region compared with controls [44].
Adaptive Immune System Response
The adaptive immune system has been shown to contribute to inflammation in several inflammatory dermatoses including acne [45], psoriasis [46], atopic dermatitis [47], and rosacea [8]. In a recent study, it was demonstrated that expression of CD4+ T cells in the three facial subtypes (PPR, ETR, and PYR) was significantly increased compared with normal skin at all stages of rosacea; the highest levels of CD4+ cells, primarily localized to the hair follicles, were recorded in patients with PPR [8]. In addition, of the three subtypes investigated, individuals with PPR demonstrated the highest gene expression levels for T cell activation and proliferation-associated genes (e.g., Lck, Vav1), costimulatory molecules for T cell activation (including Cd80, Cd86, and Tnfsf14) and pro-inflammatory cytokines such as Il-1β [8]. Transcriptome analysis of induced T cell response genes isolated from rosacea infiltrate found that gene expression levels of the Th1-signature cytokines interferon-gamma (Ifn-γ) and Tnf-α and Th1-immune response-associated cellular receptors (including Il12rb1 and Ccr5) were significantly elevated in PPR, indicating a Th1-polarized immune response in rosacea [8].
Elevated levels of antibody-producing B cells can be found in patients with PPR or PYR [8]; however, the role of B cells in the pathogenesis of rosacea has yet to be fully elucidated. Evidence from other disease models indicate a potential role of B cells in disease development, with B cell activation having been shown to contribute to downstream inflammatory infiltration of other immune cells via TLR signaling in a model of skin fibrosis [48]. In addition, CD19 expression in B cells was found to play a key role in antigen-specific CD4+ T cell proliferation and Th2 and Th17 responses in a murine model of atopic dermatitis [49].
Treatment of Inflammatory Lesions of Rosacea
Ivermectin
In patients with PPR, the aims of treatment are to alleviate signs and symptoms such as inflammatory lesions, lesional redness, and subsequently the inflammatory background erythema; to delay progression of disease; to facilitate remission; and to avoid exacerbations [50]. Before 2014, there were a limited number of treatments indicated for use on the inflammatory lesions of rosacea [51]: topical azelaic acid gel (FINACEA® 150 mg/g, Bayer plc.) [52]; topical metronidazole gel, cream, and lotion (METROGEL® 7.5 mg/g and 10 mg/g, METROCREAM® 7.5 mg/g, and METROLOTION® 7.5 mg/mL, Galderma Ltd.) [53]; and oral doxycycline 40 mg modified-release (EFRACEA/ORACEA/ORAYCEA®, Galderma Ltd.) [54].
Ivermectin 10 mg/g (1%) cream (SOOLANTRA®, Galderma Ltd.) received Food and Drug Administration (FDA) approval for the treatment of the inflammatory lesions of rosacea in December 2014 [55], and first European approval in March 2015 [56]. Ivermectin has a similar structure to macrolide antibiotics [57, 58]; however, its use is not associated with the development of antibiotic resistance [59, 60]. As a semi-synthetic derivative of avermectin (macrocyclic lactones) [57, 58], oral ivermectin has been used as an anti-parasitic since the 1970 s [61–63], and is associated with reduction of levels of mites, such as Demodex mites, on the skin [55, 64]. In vitro and in vivo studies have also demonstrated that oral ivermectin strongly reduces the priming of specific effector T cells (Ventre et al., submitted), and accumulation of neutrophils and monocytes [65].
Oral ivermectin also acts further downstream in inflammatory pathways, having previously been shown to inhibit lipopolysaccharide (LPS)-induced production of pro-inflammatory cytokines, including TNF-α, IL-1, and IL-6 [66], through the inhibition of the nuclear factor kappa B (NF-κB) pathway [66]. Ivermectin is able to suppress production of the inflammatory mediators NO and prostaglandin E2 (PGE2), and reduce inducible NO synthase (iNOS) and cyclooxygenase-2 (COX2) mRNA expression levels by inhibiting phosphorylation of the mitogen-activated protein kinases (MAPK) p38, extracellular-signal-regulated kinase (ERK) 1/2, and c-Jun N-terminal kinase (JNK) [67]. NO can generate or modify intracellular signals, thereby affecting the function of immune cells [67]. The modulation of NO, iNOS, COX2, and PGE2 release are major contributing factors during the inflammatory process. Inhibition of NO and PGE2 production by ivermectin results from the inhibition of iNOS and COX2 gene expression [67]. The MoA of ivermectin is yet to be fully elucidated, but a proposed MoA has been derived from the current preclinical evidence (Fig. 2). Further studies will be needed to confirm this proposed MoA.

Adapted from Casas et al. [19], Yamasaki et al. [29, 30], Muto et al. [32], and Zhang et al. [66, 67]
Proposed targets of ivermectin in the inflammatory pathways in rosacea. Overview of molecular and cellular targets of ivermectin (green triangle). Ivermectin is an anti-parasitic, which is known to target Demodex mites, which can be found at increased levels in patients with rosacea. Ivermectin also inhibits multiple pro-inflammatory cytokines, including IL-1β, IL-6, and TNF-α; and inflammatory mediators such as NO, COX2, and PGE2. COX2 cyclooxygenase-2, IL interleukin, KLK kallikreins, MMP matrix metalloproteinases, NO nitric oxide, PGE2 prostaglandin E2, ROS reactive oxygen species, TLR2 toll-like receptor 2, TNF tumor necrosis factor, VEGF vascular endothelial growth factor.
Recently, the anti-inflammatory effects of topical ivermectin have been demonstrated in clinical trials, as shown by decreased counts of inflammatory lesions [59, 68], although further studies will be required to confirm the exact anti-inflammatory effects of topical ivermectin in PPR.
Phase III clinical trials have been conducted, investigating the efficacy and safety of ivermectin 10 mg/g cream in the treatment of inflammatory lesions of rosacea. In two studies, Stein Gold et al. [59] assessed the efficacy and safety of ivermectin 10 mg/g cream (ivermectin cream) once daily versus vehicle applied once daily to their entire face for 12 weeks in patients with PPR. Ivermectin cream was significantly superior to vehicle in reducing the inflammatory lesions count from baseline; this was observed as early as Week 2 [59]. The median reduction from baseline in inflammatory lesion counts for both studies with ivermectin cream was 76.0% and 75.0%, respectively, versus 50.0% in both vehicle groups at Week 12 (P < 0.001) [59]. At Week 12, for Studies 1 and 2, 38.4% and 40.1% of patients treated with ivermectin 10 mg/g cream, respectively, had an Investigator’s Global Assessment (IGA) of 0 or 1 (‘clear’ or ‘almost clear’), compared with 11.6% and 18.8% of those treated with vehicle (both P < 0.001) [59]. Ivermectin cream was well tolerated and shown to be safe over the 12-week study period, with a lower incidence of treatment-related dermatological adverse events (AEs) compared with vehicle (3.5% and 1.5% versus 6.9% and 5.7%, respectively) [59]. Based on the results observed in the vehicle group in terms of reduction in inflammatory lesion counts, the vehicle formulation of ivermectin cream is also thought to play a role in reducing inflammation in rosacea, although further studies will be needed to support this initial observation.
As an extension to these studies, two 40-week investigator-blinded active controlled studies were conducted with ivermectin cream once daily and with azelaic acid 150 mg/g gel twice daily (azelaic acid gel) [69]. Azelaic acid is also known to act as an anti-inflammatory agent by inhibiting ROS formation and release by neutrophils [70]; and by reducing signaling via the CD36/NADPH oxidase, MAPK/NFκB, and KLK5/cathelicidin pathways, which indirectly inhibits production of pro-inflammatory cytokines [70–72]. Investigation of the long-term safety of ivermectin cream compared with azelaic acid gel revealed that ivermectin cream was safe and well tolerated in this long-term comparator study, with a lower incidence of treatment-related dermatological AEs compared with azelaic acid gel [69].
Metronidazole is also indicated for use against inflammatory lesions of rosacea and is known to target inflammation by decreasing ROS levels through scavenging and inactivation, and inhibiting production of these free oxygen radicals, which helps to protect the skin from damage [73]. An investigator-blinded, randomized, parallel-group study was conducted to demonstrate the superiority of ivermectin cream versus metronidazole 7.5 mg/g cream twice daily (metronidazole cream) in patients with moderate or severe inflammatory lesions of rosacea [68]. Ivermectin cream was found to be significantly superior to metronidazole cream in reducing inflammatory lesion counts from 3 weeks of treatment initiation, with a good safety profile [68]. Following this superiority study, patients who were initially successfully treated with ivermectin cream or metronidazole cream (i.e., ‘clear’ or ‘almost clear’, IGA 0 or 1) were enrolled to an extension study, in which the study treatment was discontinued [74]. Length of remission was monitored and patients were only re-treated with the initial agent if they presented with an IGA ≥2 during the 36-week extension [74]. Overall, ivermectin cream significantly extended remission of disease compared with initial treatment with metronidazole cream following treatment cessation [74]. Evidence from clinical studies demonstrates that ivermectin cream rapidly and effectively reduces inflammatory lesions, even in severe cases of rosacea.
Doxycycline
Despite rosacea being an inflammatory disease, the use of antibiotics is a common practice in dermatology [75]; and oral antibiotics have been used in the treatment of rosacea since the 1950 s [76]. Due to the chronicity of rosacea, antibiotic use is often over the long term, which can result in side effects such as candidal vulvovaginitis, gastrointestinal (GI) distress, dose-dependent photosensitivity, lupus-like syndrome, vertigo, hypersensitivity, and blue dyspigmentation [76–79].
Tetracyclines are a class of antibiotics that includes the second-generation derivatives doxycycline, minocycline, and lymecycline [76, 80–83], which have broad-spectrum activity [76]. Antibiotics were first widely prescribed by dermatologists in the 1950s, when it was discovered that they were effective in the treatment of acne [82]. Doxycycline and minocycline were approved in 1966 and 1973, respectively [76]; and have an improved bioavailability, longer elimination half-life and can be administered with food, which minimizes GI side effects [82]. Tetracyclines have been demonstrated to: downregulate the production of the pro-inflammatory cytokines IL-1 and TNF-α; inhibit neutrophil chemotaxis; inhibit the production of NO, ROS, and MMPs [76, 80]; increase epidermal hydration (following TEWL), and reduce erythema on the cheeks and centro-facial regions (determined by erythema index and melanin index of the skin) [44].
Although antibiotics have been a mainstay treatment for the inflammatory lesions of rosacea, there is increasing concern regarding the development of antibiotic resistance with prolonged use of these agents, which could potentially result in adverse global health consequences [76]. There has been a call to minimize or discontinue routine and regular use of antibiotics in the treatment of skin diseases such as acne and rosacea [84]. Tetracyclines are the most commonly prescribed type of oral antibiotic, with doxycycline accounting for approximately one-third of prescriptions, and over the past three decades, bacterial resistance to tetracycline has increased [75]. Traditional doses of immediate-release doxycycline (≥ 50 mg) can exert selection pressure, increasing the risk of bacterial resistance [80]. They can also alter the balance of commensal microflora, which can predispose patients to side effects such as vaginal candidiasis [80]. Doxycycline 50–200 mg is commonly prescribed off-label for rosacea based on its anti-inflammatory properties [76, 85], which unnecessarily exposes patients to antibiotics [76, 84]. A prospective, placebo-controlled, randomized, double-blind trial in 29 healthy volunteers demonstrated that daily administration of oral doxycycline 100 mg was associated with a significant increase in doxycycline-resistant nasopharyngeal flora measured at Days 7 and 14, which continued for more than 2 weeks after cessation of therapy [86]. Daily treatment with doxycycline 100 mg has also been shown to induce microbial resistance as early as 7 days after the start of treatment [86].
Doxycycline 40 mg Modified-Release (Anti-Inflammatory Dose)
In 2006, doxycycline 40 mg modified-release became the first FDA-approved oral treatment for PPR and the only FDA-approved tetracycline indicated for long-term use for up to 9 months [87]. The once-daily capsule formulation of doxycycline monohydrate contains 30 mg immediate-release and 10 mg delayed-release doxycycline [88].
Doxycycline 40 mg modified-release achieves plasma concentrations of doxycycline (~500 ng/mL) that fall below the minimum inhibitory concentration (MIC) of doxycycline-susceptible bacteria (1000 ng/mL) in comparison to doxycycline 50 mg (1200 ng/mL), while delivering a strong anti-inflammatory response (Fig. 3) [80]. Consequently, the modified-release formulation does not induce antimicrobial resistance or affect commensal microflora [80].
Doxycycline 40 mg modified-release plasma concentration remains below the antimicrobial threshold [80]. Graph showing plasma concentration of doxycycline 50 mg once daily (gray) and doxycycline 40 mg/g modified-release (orange) compared with the antimicrobial threshold (red dotted line)
Preclinical studies using doxycycline 40 mg modified-release demonstrated its ability to inhibit generation of active cathelicidin peptides via the direct inhibition of MMP activity (and repression of MMP gene expression) and indirect inhibition of KLK5 serine protease activity (Fig. 4) [36]. Doxycycline 40 mg modified-release has also been shown to have anti-angiogenic effects, through its inhibition of MMPs, which are essential for the coordinated degradation of matrix during angiogenesis [89]. Inhibition of MMPs indirectly inhibits vascular endothelial growth factor (VEGF)-induced angiogenesis (evidence suggests that neutrophils express VEGF, VEGF receptor [VEGFR]-1, and VEGFR-2 in rosacea, and VEGF is known to be a potent stimulator of angiogenesis) [80, 90]. In addition, doxycycline 40 mg modified-release is a more potent inhibitor of MMPs than minocycline or tetracycline, acting as a non-competitive inhibitor of these enzymes [80].

Adapted from Del Rosso et al. [14], Kanada et al. [36], Di Nardo et al. [40], Baldwin [76], Fowler [80], and Cazalis et al. [94]
Proposed targets of doxycycline 40 mg modified-release on inflammatory pathways in rosacea based on current evidence [14, 36, 76, 80, 94]. Overview of molecular and cellular targets of doxycycline 40 mg modified-release (orange circle). Doxycycline 40 mg modified-release acts on several targets in the cathelicidin pathway, including MMPs, KLKs (e.g., KLK5), and cathelicidin. It also acts on pro-inflammatory cytokines, including IL-1β, IL-8, and TNF-α; and inflammatory mediators such as ROS. IL interleukin, KLK kallikreins, MMPs matrix metalloproteinases, NO nitric oxide, PGE2 prostaglandin E2, ROS reactive oxygen species, TLR2 toll-like receptor 2, TNF tumor necrosis factor, VEGF vascular endothelial growth factor.
A recent study indicates that patients with rosacea may be at a higher risk of developing cardiovascular disease (CVD) [91]. MMPs have been shown to be influential in the pathology of both rosacea and CVD [92], triggering an inflammatory pathway via production of KLK5 and cathelicidin and subsequent production of LL-37 [36]. Based on the fact that doxycycline 40 mg modified-release inhibits MMP activity, this agent could potentially also be beneficial in the prevention or reduction of CVD risk, as doxycycline has previously been shown to: defend capillary wall and connective tissue integrity; reduce hypersensitivity to vasodilatory stimuli; prevent leakage of capillaries: and inhibit cytokines involved in inflammation [92]. Furthermore, it has been observed that sub-antimicrobial-dose doxycycline (20 mg twice daily) lowers the levels of the inflammatory biomarker serum C-reactive protein (CRP), with elevated CRP levels being a known CVD risk factor [93]. By inhibiting the production and activity of MMPs, doxycycline 40 mg modified-release blocks multiple inflammatory pathways, which inhibits the production of proteins contributing to the pathophysiology of PPR inflammation. This ultimately reduces the inflammation associated with inflammatory lesions of rosacea [36, 94].
Although doxycycline 40 mg modified-release acts as an anti-inflammatory agent [76, 80], it does not have antimicrobial activity [80, 95], and does not exert selective pressure on microorganisms or encourage the development of bacterial resistance [76]. In a 9-month, multicenter, randomized, double-blind, placebo-controlled trial, subgingival samples were collected from adult patients with periodontitis at baseline and after 9 months of doxycycline 40 mg modified-release once-daily (n = 34) or placebo therapy (n = 36) [80, 96]. Treatment with either doxycycline 40 mg modified-release or placebo did not result in the development of antibiotic resistance, and only a minor comparable increase in doxycycline-resistant bacteria was observed in both study arms after 9 months (5.09% vs. 5.38%, respectively; P = 0.965) [80, 96].
In patients with rosacea, the efficacy and safety of doxycycline 40 mg modified-release (anti-inflammatory dose) has been investigated versus placebo [95] and doxycycline 100 mg [97]. In two trials, adult patients with inflammatory lesions (moderate to severe disease) were randomized to receive either doxycycline 40 mg modified-release (n = 269) or placebo (n = 268) once daily [95]. The mean total inflammatory lesion count of patients was 19.9 in Study 1 and 20.8 in Study 2 [95]. At Week 16, the mean change from baseline in inflammatory lesion counts in the active treatment groups was −11.8 in Study 1 and −9.5 in Study 2, compared with −5.9 and −4.3 in the placebo groups, respectively (P < 0.001 for both comparisons) [95]. In addition, doxycycline 40 mg modified-release was well tolerated, with a similar number of AEs experienced by patients in both groups [95]. In a separate 16-week study, the efficacy and safety of doxycycline 40 mg modified-release was compared with those of doxycycline 100 mg, showing that reduction in inflammatory lesion counts from baseline was similar in the two groups; at Week 16, the mean change in inflammatory lesion counts from baseline was −14.3 with doxycycline 40 mg modified-release compared with −13.0 with doxycycline 100 mg [97]. Overall, doxycycline 40 mg modified-release was shown to have similar efficacy to doxycycline 100 mg, with approximately five times fewer gastrointestinal AEs [97]. In studies with healthy volunteers administered doxycycline 40 mg modified-release (n = 16) or doxycycline 50 mg (n = 16), doxycycline 40 mg modified-release reached steady-state plasma concentrations that remained below the MIC of common doxycycline-susceptible microorganisms throughout a 24-hour dosing period [80]. In contrast, with conventional immediate-release doxycycline 50 mg, steady-state plasma concentrations do not remain below MICs [80].
Rationale for a Combinatorial Treatment of Inflammatory Lesions of Rosacea with Ivermectin 10 mg/g and Doxycycline 40 mg Modified-Release
Ivermectin and doxycycline 40 mg modified-release have different targets in the inflammatory pathways of rosacea, with each agent providing add-on effects summarized in Table 1 and presented in Fig. 5 [36, 55, 64, 66, 80, 94]. Treatment efficacy could be increased if these two agents were used in combination, through a targeting of multiple steps of different inflammatory pathways. Doxycycline 40 mg modified-release targets MMPs and ROS, indirectly blocking production of inflammatory mediators [36, 80, 89]. Oral ivermectin has been shown to inhibit T cell activation, release of pro-inflammatory mediators, macrophage and neutrophil recruitment, as well as reducing levels of Demodex mites on the skin, which prevents the subsequent amplification of the inflammatory response [64–66]. In addition, these agents also act on several common targets, which further reduce the intensity of the inflammatory response. In a recent preclinical study, the synergistic activity of doxycycline and ivermectin was demonstrated to be effective in the complete eradication of body lice [98]. The hypothesis is that combining treatments which act on different targets within inflammatory pathways could provide improved results for patients with inflammatory lesions of rosacea.

Adapted from Del Rosso et al. [14], Casas et al. [19], Yamasaki et al. [29, 30], Muto et al. [32], Kanada et al. [36], Di Nardo et al. [40], Zhang et al. [66, 67], Baldwin [76], Fowler [80], Cazalis et al. [94]
Proposed complementary targets of ivermectin and doxycycline 40 mg modified-release in the inflammatory pathways in rosacea based on current evidence. IL interleukin, KLK kallikreins, MMPs matrix metalloproteinases, NO nitric oxide, PGE2 prostaglandin E2, ROS reactive oxygen species, TLR2 toll-like receptor 2, TNF tumor necrosis factor, VEGF vascular endothelial growth factor.
Results from combination studies provide a rationale for the combinatorial use of agents in the treatment of inflammatory lesions of rosacea. In a 16-week, randomized, double-blind, placebo-controlled study, adult patients with inflammatory lesions of rosacea (8–40 inflammatory lesions) and moderate to severe erythema were randomized to oral doxycycline 40 mg modified-release and topical metronidazole 10 mg/g gel once daily (Group 1) or placebo and topical metronidazole 10 mg/g gel once daily (Group 2) for 12 weeks; double-blind administration of doxycycline 40 mg modified-release or placebo was continued up to Week 16 [99]. Combination therapy significantly reduced inflammatory lesion counts from Week 4, i.e., with a faster onset of action than metronidazole monotherapy, and continued to Week 12 compared with metronidazole 10 mg/g gel monotherapy [99]. Total inflammatory lesion count at baseline was 21.3 in Group 1 and 18.7 in Group 2 [99]. From baseline to Week 4, the mean change in inflammatory lesions count was −9.69 in Group 1 compared with Group 2 (P = 0.008); and at Week 12 was −13.86 versus −8.7, respectively (P = 0.002) [99].
Discussion
The combination of augmented immune responses (inflammation), neurovascular dysregulation, and physiochemical and structural changes contributes to the pathogenesis of rosacea [12, 25, 26]. Increased expression of specific proteins such as MMPs, KLK5, cathelicidin, and LL-37, as well as cytokines such as IL-1, TNF-α, and IFN-γ contribute to a heightened and constitutively active inflammatory response, leading to the development of inflammatory lesions [29, 35–37]. Oral ivermectin has been shown to inhibit the activation of T cells (Ventre et al., submitted) and the production of pro-inflammatory cytokines [66], and to reduce levels of Demodex mites on the skin [41, 55, 64]. Doxycycline 40 mg modified-release, a tetracycline derivative with anti-inflammatory and sub-antimicrobial activity, has been shown to inhibit MMPs and suppress the production of KLK5, the cathelicidin peptide LL-37, as well as inhibit the production of certain pro-inflammatory cytokines [36, 94]. Both ivermectin 10 mg/g cream and doxycycline 40 mg modified-release have been shown to be clinically effective in reducing the number of inflammatory lesions in patients with PPR; in addition, both agents have a good safety profile [59, 68, 69, 95, 97].
Based on the initial evidence of the efficacy of combinatorial therapies, both in rosacea [99] and in the treatment of other dermatological diseases such as acne [27], the combination of topical ivermectin 10 mg/g cream with oral doxycycline 40 mg modified-release could provide an intensive initial regimen, especially for those patients with more involved disease or when a fast onset of action is required. Onset of treatment effect can be seen as early as 2 weeks after treatment initiation with ivermectin 10 mg/g cream monotherapy [59] and 3 weeks with doxycycline 40 mg modified-release monotherapy [95]; onset of action could potentially be faster, with a potentially larger reduction in inflammatory lesions, if these agents were to be used in combination.
Summary and Conclusions
Given the chronic nature of rosacea, the need for continuous therapy often leads to reduced adherence in patients with this disease [76]. A fast onset of action means that patients would see the benefits of treatment immediately, and be more likely to continue treatment as prescribed. Clinical evidence seems to support that a combination of these two agents as an intensive initial treatment would be effective in patients with severe disease, i.e., disease with a high inflammatory component, or when a fast onset of results is sought. Both ivermectin and doxycycline 40 mg modified-release act on inflammatory pathways, which results in modulation of the production of downstream inflammatory mediators. This could potentially also help patients see results early on in their treatment, which in turn could improve long-term adherence.
Further research is needed to correlate clinical manifestations in patients with rosacea with predominance of certain inflammatory cascades. This will allow clinicians to identify which patients will most benefit from monotherapy versus combination therapy and enable treatments to be tailored to individual patients, depending on their symptoms. The use of combination therapies in rosacea has yet to be thoroughly evaluated and validated, and clinical studies that investigate the efficacy of combination regimens are needed. Availability of such data would provide a clear message regarding optimal, individualized treatment options. However, current evidence suggests that the combinatorial treatment of topical ivermectin 10 mg/g cream and oral doxycycline 40 mg modified-release should be used as the first-line treatment for inflammatory lesions of rosacea for optimal efficacy.
References
Feldman SR, Huang WW, Huynh TT. Current drug therapies for rosacea: a chronic vascular and inflammatory skin disease. J Manag Care Spec Pharm. 2014;20(6):623–9.
Baldwin HE. Diagnosis and treatment of rosacea: state of the art. J Drugs Dermatol. 2012;11(6):725–30.
Wilkin J, Dahl M, Detmar M, Drake L, Feinstein A, Odom R, et al. Standard classification of rosacea: Report of the National Rosacea Society Expert Committee on the Classification and Staging of Rosacea. J Am Acad Dermatol. 2002;46(4):584–7.
Holmes AD, Steinhoff M. Integrative concepts of rosacea pathophysiology, presentation, and therapeutics. Exp Dermatol. 2016. doi:10.1111/exd.13143
Dirschka T, Micali G, Papadopoulos L, Tan J, Layton A, Moore S. Perceptions on the Psychological Impact of Facial Erythema Associated with Rosacea: results of International Survey. Dermatol Ther (Heidelb). 2015;5(2):117–27. doi:10.1007/s13555-015-0077-2.
Steinhoff M, Buddenkotte J, Aubert J, Sulk M, Novak P, Schwab VD, et al. Clinical, cellular, and molecular aspects in the pathophysiology of rosacea. J Investig Dermatol Symp Proc. 2011;15(1):2–11. doi:10.1038/jidsymp.2011.7.
Schwab VD, Sulk M, Seeliger S, Nowak P, Aubert J, Mess C, et al. Neurovascular and neuroimmune aspects in the pathophysiology of rosacea. J Investig Dermatol Symp Proc. 2011;15(1):53–62. doi:10.1038/jidsymp.2011.6.
Buhl T, Sulk M, Nowak P, Buddenkotte J, McDonald I, Aubert J, et al. Molecular and morphological characterization of inflammatory infiltrate in rosacea reveals activation of Th1/Th17 pathways. J Invest Dermatol. 2015;135(9):2198–208. doi:10.1038/jid.2015.141.
Sulk M, Seeliger S, Aubert J, Schwab VD, Cevikbas F, Rivier M, et al. Distribution and expression of non-neuronal transient receptor potential (TRPV) ion channels in rosacea. J Invest Dermatol. 2012;132(4):1253–62. doi:10.1038/jid.2011.424.
Helfrich YR, Maier LE, Cui Y, Fisher GJ, Chubb H, Fligiel S, et al. Clinical, histologic, and molecular analysis of differences between erythematotelangiectatic rosacea and telangiectatic photoaging. JAMA Dermatol. 2015;151(8):825–36. doi:10.1001/jamadermatol.2014.4728.
Odom R, Dahl M, Dover J, Draelos Z, Drake L, Macsai M, et al. Standard management options for rosacea, part 1: overview and broad spectrum of care. Cutis. 2009;84(1):43–7.
Cribier B. Rosacea under the microscope: characteristic histological findings. J Eur Acad Dermatol Venereol. 2013;27(11):1336–43. doi:10.1111/jdv.12121.
Chang AL, Raber I, Xu J, Li R, Spitale R, Chen J, et al. Assessment of the genetic basis of rosacea by genome-wide association study. J Invest Dermatol. 2015;135(6):1548–55. doi:10.1038/jid.2015.53.
Del Rosso JQ, Gallo RL, Kircik L, Thiboutot D, Baldwin HE, Cohen D. Why is rosacea considered to be an inflammatory disorder? The primary role, clinical relevance, and therapeutic correlations of abnormal innate immune response in rosacea-prone skin. J Drugs Dermatol. 2012;11(6):694–700.
Guzman-Sanchez DA, Ishiuji Y, Patel T, Fountain J, Chan YH, Yosipovitch G. Enhanced skin blood flow and sensitivity to noxious heat stimuli in papulopustular rosacea. J Am Acad Dermatol. 2007;57(5):800–5. doi:10.1016/j.jaad.2007.06.009.
Steinhoff M, Schmelz M, Schauber J. Facial erythema of rosacea— aetiology, different pathophysiologies and treatment options. Acta Derm Venereol. 2016;96(5):579–86. doi:10.2340/00015555-2335
Metzler-Wilson K, Toma K, Sammons DL, Mann S, Jurovcik AJ, Demidova O, et al. Augmented supraorbital skin sympathetic nerve activity responses to symptom trigger events in rosacea patients. J Neurophysiol. 2015;114(3):1530–7. doi:10.1152/jn.00458.2015.
Zhao YE, Peng Y, Wang XL, Wu LP, Wang M, Yan HL, et al. Facial dermatosis associated with Demodex: a case-control study. J Zhejiang Univ Sci B. 2011;12(12):1008–15. doi:10.1631/jzus.B1100179.
Casas C, Paul C, Lahfa M, Livideanu B, Lejeune O, Alvarez-Georges S, et al. Quantification of Demodex folliculorum by PCR in rosacea and its relationship to skin innate immune activation. Exp Dermatol. 2012;21(12):906–10. doi:10.1111/exd.12030.
Forton F, Seys B. Density of Demodex folliculorum in rosacea: a case-control study using standardized skin-surface biopsy. Br J Dermatol. 1993;128(6):650–9.
Liang H, Randon M, Michee S, Tahiri R, Labbe A, Baudouin C. In vivo confocal microscopy evaluation of ocular and cutaneous alterations in patients with rosacea. Br J Ophthalmol. 2016. doi:10.1136/bjophthalmol-2015-308110.
Turgut Erdemir A, Gurel MS, Koku Aksu AE, Falay T, Inan Yuksel E, Sarikaya E. Demodex mites in acne rosacea: reflectance confocal microscopic study. Australas J Dermatol. 2016. doi:10.1111/ajd.12452.
Sattler EC, Hoffmann VS, Ruzicka T, Braunmuhl TV, Berking C. Reflectance confocal microscopy for monitoring the density of Demodex mites in patients with rosacea before and after treatment. Br J Dermatol. 2015;173(1):69–75. doi:10.1111/bjd.13783.
Chen W, Plewig G. Are Demodex mites principal, conspirator, accomplice, witness or bystander in the cause of rosacea? Am J Clin Dermatol. 2015;16(2):67–72. doi:10.1007/s40257-015-0115-y.
Del Rosso JQ. Management of facial erythema of rosacea: what is the role of topical alpha-adrenergic receptor agonist therapy? J Am Acad Dermatol. 2013;69(6 Suppl 1):S44–56. doi:10.1016/j.jaad.2013.06.009.
Del Rosso JQ. Advances in understanding and managing rosacea: part 2: the central role, evaluation, and medical management of diffuse and persistent facial erythema of rosacea. J Clin Aesthet Dermatol. 2012;5(3):26–36.
Nast A, Dréno B, Bettoli V, Degitz K, Erdmann R, Finlay AY, et al. European evidence-based (S3) guidelines for the treatment of acne. J Eur Acad Dermatol Venereol. 2012;26(Suppl 1):1–29. doi:10.1111/j.1468-3083.2011.04374.x.
American Academy of Dermatology Work G, Menter A, Korman NJ, Elmets CA, Feldman SR, Gelfand JM, et al. Guidelines of care for the management of psoriasis and psoriatic arthritis: section 6. Guidelines of care for the treatment of psoriasis and psoriatic arthritis: case-based presentations and evidence-based conclusions. J Am Acad Dermatol. 2011;65(1):137–74. doi:10.1016/j.jaad.2010.11.055.
Yamasaki K, Kanada K, Macleod DT, Borkowski AW, Morizane S, Nakatsuji T, et al. TLR2 expression is increased in rosacea and stimulates enhanced serine protease production by keratinocytes. J Invest Dermatol. 2011;131(3):688–97. doi:10.1038/jid.2010.351.
Yamasaki K, Di Nardo A, Bardan A, Murakami M, Ohtake T, Coda A, et al. Increased serine protease activity and cathelicidin promotes skin inflammation in rosacea. Nat Med. 2007;13(8):975–80. doi:10.1038/nm1616.
Two AM, Wu W, Gallo RL, Hata TR. Rosacea: part I. Introduction, categorization, histology, pathogenesis, and risk factors. J Am Acad Dermatol. 2015;72(5):749–58. doi:10.1016/j.jaad.2014.08.028 (quiz 59–60).
Muto Y, Wang Z, Vanderberghe M, Two A, Gallo RL, Di Nardo A. Mast cells are key mediators of cathelicidin-initiated skin inflammation in rosacea. J Invest Dermatol. 2014;134(11):2728–36. doi:10.1038/jid.2014.222.
Reinholz M, Ruzicka T, Schauber J. Cathelicidin LL-37: an antimicrobial peptide with a role in inflammatory skin disease. Ann Dermatol. 2012;24(2):126–35. doi:10.5021/ad.2012.24.2.126.
Yamasaki K, Gallo RL. Rosacea as a disease of cathelicidins and skin innate immunity. J Investig Dermatol Symp Proc. 2011;15(1):12–5. doi:10.1038/jidsymp.2011.4.
Wise RD. Submicrobial doxycycline and rosacea. Compr Ther. 2007;33(2):78–81.
Kanada KN, Nakatsuji T, Gallo RL. Doxycycline indirectly inhibits proteolytic activation of tryptic kallikrein-related peptidases and activation of cathelicidin. J Invest Dermatol. 2012;132(5):1435–42. doi:10.1038/jid.2012.14.
Gerber PA, Buhren BA, Steinhoff M, Homey B. Rosacea: the cytokine and chemokine network. J Investig Dermatol Symp Proc. 2011;15(1):40–7. doi:10.1038/jidsymp.2011.9.
Liu PT, Stenger S, Li H, Wenzel L, Tan BH, Krutzik SR, et al. Toll-like receptor triggering of a vitamin D-mediated human antimicrobial response. Science. 2006;311(5768):1770–3. doi:10.1126/science.1123933.
Two AM, Hata TR, Nakatsuji T, Coda AB, Kotol PF, Wu W, et al. Reduction in serine protease activity correlates with improved rosacea severity in a small, randomized pilot study of a topical serine protease inhibitor. J Invest Dermatol. 2014;134(4):1143–5. doi:10.1038/jid.2013.472.
Di Nardo A, Holmes AD, Muto Y, Huang EY, Preston N, Winkelman WJ, et al. Improved clinical outcome and biomarkers in adults with papulopustular rosacea treated with doxycycline modified-release capsules in a randomized trial. J Am Acad Dermatol. 2016;. doi:10.1016/j.jaad.2016.01.023.
Di Nardo A, Vitiello A, Gallo RL. Cutting edge: mast cell antimicrobial activity is mediated by expression of cathelicidin antimicrobial peptide. J Immunol. 2003;170(5):2274–8.
Del Rosso JQ, Levin J. The clinical relevance of maintaining the functional integrity of the stratum corneum in both healthy and disease-affected skin. J Clin Aesthet Dermatol. 2011;4(9):22–42.
Dirschka T, Tronnier H, Folster-Holst R. Epithelial barrier function and atopic diathesis in rosacea and perioral dermatitis. Br J Dermatol. 2004;150(6):1136–41. doi:10.1111/j.1365-2133.2004.05985.x.
Ní Raghallaigh S, Powell FC. Epidermal hydration levels in patients with rosacea improve after minocycline therapy. Br J Dermatol. 2014;171(2):259–66. doi:10.1111/bjd.12770.
Kelhälä HL, Palatsi R, Fyhrquist N, Lehtimaki S, Vayrynen JP, Kallioinen M, et al. IL-17/Th17 pathway is activated in acne lesions. PLoS ONE. 2014;9(8):e105238. doi:10.1371/journal.pone.0105238.
Palau N, Julia A, Ferrandiz C, Puig L, Fonseca E, Fernandez E, et al. Genome-wide transcriptional analysis of T cell activation reveals differential gene expression associated with psoriasis. BMC Genom. 2013;14:825. doi:10.1186/1471-2164-14-825.
Suárez-Fariiñas M, Dhingra N, Gittler J, Shemer A, Cardinale I, de Guzman Strong C, et al. Intrinsic atopic dermatitis shows similar TH2 and higher TH17 immune activation compared with extrinsic atopic dermatitis. J Allergy Clin Immunol. 2013;132(2):361–70. doi:10.1016/j.jaci.2013.04.046.
Yoshizaki A, Iwata Y, Komura K, Ogawa F, Hara T, Muroi E, et al. CD19 regulates skin and lung fibrosis via Toll-like receptor signaling in a model of bleomycin-induced scleroderma. Am J Pathol. 2008;172(6):1650–63. doi:10.2353/ajpath.2008.071049.
Yanaba K, Kamata M, Asano Y, Tada Y, Sugaya M, Kadono T, et al. CD19 expression in B cells regulates atopic dermatitis in a mouse model. Am J Pathol. 2013;182(6):2214–22. doi:10.1016/j.ajpath.2013.02.042.
Elewski BE, Draelos Z, Dreno B, Jansen T, Layton A, Picardo M. Rosacea— global diversity and optimized outcome: proposed international consensus from the Rosacea International Expert Group. J Eur Acad Dermatol Venereol. 2011;25(2):188–200. doi:10.1111/j.1468-3083.2010.03751.x.
van Zuuren EJ, Kramer SF, Carter BR, Graber MA, Fedorowicz Z. Effective and evidence-based management strategies for rosacea: summary of a Cochrane systematic review. Br J Dermatol. 2011;165(4):760–81. doi:10.1111/j.1365-2133.2011.10473.x.
European Medicines Agency. FINACEA®—summary of product characteristics. June 2014.
Galderma Ltd. METROGEL®, METROCREAM®, METROLOTION™—product monograph. January 2014.
European Medicines Agency. EFRACEA/ORACEA/ORAYCEA® 40 mg modified-release hard capsules—summary of product characteristics. February 2014.
European Medicines Agency. SOOLANTRA®—summary of product characteristics. April 2015.
Galderma Ltd. Galderma Announces Positive Outcome of European Decentralised Procedure for Approval of SOOLANTRA® (Ivermectin) Cream 10 mg/g for Rosacea Patients. In: Galderma News. 2015. http://www.galderma.com/News/articleType/ArticleView/articleId/79/Galderma-Announces-Positive-Outcome-of-European-Decentralised-Procedure-for-Approval-of-SOOLANTRA-ivermectin-Cream-10mgg-for-Rosacea-Patients. Accessed May 17, 2015.
Crump A, Omura S. Ivermectin, ‘wonder drug’ from Japan: the human use perspective. Proc Jpn Acad Ser B Phys Biol Sci. 2011;87(2):13–28.
Lynagh T, Lynch JW. Ivermectin binding sites in human and invertebrate Cys-loop receptors. Trends Pharmacol Sci. 2012;33(8):432–41. doi:10.1016/j.tips.2012.05.002.
Stein Gold L, Kircik L, Fowler J, Tan J, Draelos Z, Fleischer A, et al. Efficacy and safety of ivermectin 1% cream in treatment of papulopustular rosacea: results of two randomized, double-blind, vehicle-controlled pivotal studies. J Drugs Dermatol. 2014;13(3):316–23.
Raedler LA. Soolantra (Ivermectin) 1% cream: a novel, antibiotic-free agent approved for the treatment of patients with rosacea. Am Health Drug Benefits. 2015;8(Spec Feature):122–5.
Burg RW, Miller BM, Baker EE, Birnbaum J, Currie SA, Hartman R, et al. Avermectins, new family of potent anthelmintic agents: producing organism and fermentation. Antimicrob Agents Chemother. 1979;15(3):361–7.
Fox LM. Ivermectin: uses and impact 20 years on. Curr Opin Infect Dis. 2006;19(6):588–93. doi:10.1097/QCO.0b013e328010774c.
Geary TG. Ivermectin 20 years on: maturation of a wonder drug. Trends Parasitol. 2005;21(11):530–2. doi:10.1016/j.pt.2005.08.014.
Salem DA, El-Shazly A, Nabih N, El-Bayoumy Y, Saleh S. Evaluation of the efficacy of oral ivermectin in comparison with ivermectin-metronidazole combined therapy in the treatment of ocular and skin lesions of Demodex folliculorum. Int J Infect Dis. 2013;17(5):e343–7. doi:10.1016/j.ijid.2012.11.022.
Yan S, Ci X, Chen N, Chen C, Li X, Chu X, et al. Anti-inflammatory effects of ivermectin in mouse model of allergic asthma. Inflamm Res. 2011;60(6):589–96. doi:10.1007/s00011-011-0307-8.
Zhang X, Song Y, Ci X, An N, Ju Y, Li H, et al. Ivermectin inhibits LPS-induced production of inflammatory cytokines and improves LPS-induced survival in mice. Inflamm Res. 2008;57(11):524–9. doi:10.1007/s00011-008-8007-8.
Zhang X, Song Y, Xiong H, Ci X, Li H, Yu L, et al. Inhibitory effects of ivermectin on nitric oxide and prostaglandin E2 production in LPS-stimulated RAW 264.7 macrophages. Int Immunopharmacol. 2009;9(3):354–9. doi:10.1016/j.intimp.2008.12.016.
Taieb A, Ortonne JP, Ruzicka T, Roszkiewicz J, Berth-Jones J, Peirone MH, et al. Superiority of ivermectin 1% cream over metronidazole 0.75% cream in treating inflammatory lesions of rosacea: a randomized, investigator-blinded trial. Br J Dermatol. 2015;172(4):1103–10. doi:10.1111/bjd.13408.
Stein Gold L, Kircik L, Fowler J, Jackson JM, Tan J, Draelos Z, et al. Long-term safety of ivermectin 1% cream vs azelaic acid 15% gel in treating inflammatory lesions of rosacea: results of two 40-week controlled, investigator-blinded trials. J Drugs Dermatol. 2014;13(11):1380–6.
Akamatsu H, Komura J, Asada Y, Miyachi Y, Niwa Y. Inhibitory effect of azelaic acid on neutrophil functions: a possible cause for its efficacy in treating pathogenetically unrelated diseases. Arch Dermatol Res. 1991;283(3):162–6.
Sieber MA, Hegel JK. Azelaic acid: properties and mode of action. Skin Pharmacol Physiol. 2014;27(Suppl 1):9–17. doi:10.1159/000354888.
Mastrofrancesco A, Ottaviani M, Aspite N, Cardinali G, Izzo E, Graupe K, et al. Azelaic acid modulates the inflammatory response in normal human keratinocytes through PPARgamma activation. Exp Dermatol. 2010;19(9):813–20. doi:10.1111/j.1600-0625.2010.01107.x.
Narayanan S, Hunerbein A, Getie M, Jackel A, Neubert RH. Scavenging properties of metronidazole on free oxygen radicals in a skin lipid model system. J Pharm Pharmacol. 2007;59(8):1125–30. doi:10.1211/jpp.59.8.0010.
Taieb A, Khemis A, Ruzicka T, Baranska-Rybak W, Berth-Jones J, Schauber J, et al. Maintenance of remission following successful treatment of papulopustular rosacea with ivermectin 1% cream vs. metronidazole 0.75% cream: 36-week extension of the ATTRACT randomized study. J Eur Acad Dermatol Venereol. 2015;. doi:10.1111/jdv.13537.
Del Rosso JQ, Leyden JJ. Status report on antibiotic resistance: implications for the dermatologist. Dermatol Clin. 2007;25(2):127–32. doi:10.1016/j.det.2007.01.001.
Baldwin HE. Systemic therapy for rosacea. Skin Therapy Lett. 2007;12(2):1–5, 9.
Del Rosso JQ. Systemic therapy for rosacea: focus on oral antibiotic therapy and safety. Cutis. 2000;66(4 Suppl):7–13.
Bikowski JB. Rosacea: a tiered approach to therapy. Cutis. 2000;66(4 Suppl):3–6.
Rebora A. The management of rosacea. Am J Clin Dermatol. 2002;3(7):489–96.
Fowler JF Jr. Anti-inflammatory dose doxycycline for the treatment of rosacea. Expert Rev Dermatol. 2007;6:523–31.
Sloan B, Scheinfeld N. The use and safety of doxycycline hyclate and other second-generation tetracyclines. Expert Opin Drug Saf. 2008;7(5):571–7. doi:10.1517/14740338.7.5.571.
Korting HC, Schollmann C. Current topical and systemic approaches to treatment of rosacea. J Eur Acad Dermatol Venereol. 2009;23(8):876–82. doi:10.1111/j.1468-3083.2009.03167.x.
Goulden V. Guidelines for the management of acne vulgaris in adolescents. Paediatr Drugs. 2003;5(5):301–13.
Muhammad M, Rosen T. A controversial proposal: no more antibiotics for acne! Skin Therapy Lett. 2013;18(5):1–4.
Culp B, Scheinfeld N. Rosacea: a review. P T. 2009;34(1):38–45.
Walker C, Bradshaw M, editors. The effect of oral doxycycline 100 mg once-daily for 14 days on the nasopharyngeal flora of healthy volunteers: a preliminary analysis. Poster presentation. 26th Anniversary Fall Clinical Dermatology Conference: Las Vegas, NV, USA; 2007 18–27 October 2007.
Preshaw PM, Novak MJ, Mellonig J, Magnusson I, Polson A, Giannobile WV, et al. Modified-release subantimicrobial dose doxycycline enhances scaling and root planing in subjects with periodontal disease. J Periodontol. 2008;79(3):440–52. doi:10.1902/jop.2008.070375.
European Medicines Agency. ORACEA®—summary of product characteristics. February 2014.
Kim MH. Flavonoids inhibit VEGF/bFGF-induced angiogenesis in vitro by inhibiting the matrix-degrading proteases. J Cell Biochem. 2003;89(3):529–38. doi:10.1002/jcb.10543.
Smith JR, Lanier VB, Braziel RM, Falkenhagen KM, White C, Rosenbaum JT. Expression of vascular endothelial growth factor and its receptors in rosacea. Br J Ophthalmol. 2007;91(2):226–9. doi:10.1136/bjo.2006.101121.
Hua TC, Chung PI, Chen YJ, Wu LC, Chen YD, Hwang CY, et al. Cardiovascular comorbidities in patients with rosacea: a nationwide case-control study from Taiwan. J Am Acad Dermatol. 2015;73(2):249–54. doi:10.1016/j.jaad.2015.04.028.
Dosal J, Keri J. Rosacea and cardiovascular disease: is there an association? J Am Acad Dermatol. 2015;73(2):308–9. doi:10.1016/j.jaad.2015.03.031.
Koppikar RS, Agrawal SV. The effect of sub-antimicrobial dose-doxycycline periodontal therapy on serum inflammatory biomarker C-reactive protein levels in post-menopausal women: a 2-year, double-blinded, randomized clinical trial. Contemp Clin Dent. 2013;4(1):71–3. doi:10.4103/0976-237X.111628.
Cazalis J, Bodet C, Gagnon G, Grenier D. Doxycycline reduces lipopolysaccharide-induced inflammatory mediator secretion in macrophage and ex vivo human whole blood models. J Periodontol. 2008;79(9):1762–8. doi:10.1902/jop.2008.080051.
Del Rosso JQ, Webster GF, Jackson M, Rendon M, Rich P, Torok H, et al. Two randomized phase III clinical trials evaluating anti-inflammatory dose doxycycline (40-mg doxycycline, USP capsules) administered once daily for treatment of rosacea. J Am Acad Dermatol. 2007;56(5):791–802. doi:10.1016/j.jaad.2006.11.021.
Walker C, Webster GF, editors. A multicenter, double-blind randomized trial to evaluate long-term anti-inflammatory dose doxycycline (40 mg) therapy: results of the lack of the effect of bacterial flora. Full Clinical Dermatology Conference: Las Vegas, NV, USA; 2006 7–11 October 2006.
Del Rosso JQ, Schlessinger J, Werschler P. Comparison of anti-inflammatory dose doxycycline versus doxycycline 100 mg in the treatment of rosacea. J Drugs Dermatol. 2008;7(6):573–6.
Sangaré AK, Rolain JM, Gaudart J, Weber P, Raoult D. Synergistic activity of antibiotics combined with ivermectin to kill body lice. Int J Antimicrob Agents. 2016. doi:10.1016/j.ijantimicag.2016.01.001.
Fowler JF Jr. Combined effect of anti-inflammatory dose doxycycline (40-mg doxycycline, usp monohydrate controlled-release capsules) and metronidazole topical gel 1% in the treatment of rosacea. J Drugs Dermatol. 2007;6(6):641–5.
Acknowledgments
Editorial assistance in the preparation of the manuscript was provided by Dr. Raffaella Facchini and Dr. Carole Mongin-Bulewski of Havas Life Medicom. The authors would like to thank Dr Anna Holmes for her scientific advice. Support for editorial assistance was funded by Galderma. The work was also supported by grants from Science foundation Ireland (SFI IvP award to MS). The article processing charges and open access fee for this publication were funded by Galderma. All named authors meet the International Committee of Medical Journal Editors (ICMJE) criteria for authorship for this manuscript, take responsibility for the integrity of the work as a whole, and have given final approval for the version to be published.
Disclosures
Martin Steinhoff has received research support and/or honoraria from Almirall, Avon, Bayer, BMS, Galderma, GSK, L’Oreal, LaRoche Posay, Leo Pharm, Pfizer, Pierre-Fabre, Regeneron, Tigercat and Vertex. Marc Vocanson has no conflicts of interest. Johannes J Voegel, Feriel Hacini-Rachinel, and Gregor Schäfer are employees of Galderma.
Compliance with Ethics Guidelines
This article is based on previously conducted studies and does not involve any new studies of human or animal subjects performed by any of the authors.
Open Access
This article is distributed under the terms of the Creative Commons Attribution-NonCommercial 4.0 International License (http://creativecommons.org/licenses/by-nc/4.0/), which permits any noncommercial use, distribution, and reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made.
Author information
Authors and Affiliations
Corresponding author
Additional information
Enhanced content
To view enhanced content for this article go to www.medengine.com/Redeem/31E4F0600FDF1ED6.
Rights and permissions
Open Access This article is distributed under the terms of the Creative Commons Attribution 4.0 International License (https://creativecommons.org/licenses/by/4.0), which permits use, duplication, adaptation, distribution, and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made.
About this article
Cite this article
Steinhoff, M., Vocanson, M., Voegel, J.J. et al. Topical Ivermectin 10 mg/g and Oral Doxycycline 40 mg Modified-Release: Current Evidence on the Complementary Use of Anti-Inflammatory Rosacea Treatments. Adv Ther 33, 1481–1501 (2016). https://doi.org/10.1007/s12325-016-0380-z
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12325-016-0380-z