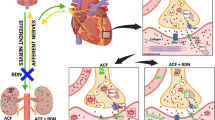
Abstract
Percutaneous transluminal renal angioplasty (PTRA) may improve cardiac function in renovascular hypertension (RVH), but its effect on the biological mechanisms implicated in cardiac damage remains unknown. We hypothesized that restoration of kidney function by PTRA ameliorates myocardial mitochondrial damage and preserves cardiac function in pigs with metabolic syndrome (MetS) and RVH. Pigs were studied after 16 weeks of MetS+RVH, MetS+RVH treated 4 weeks earlier with PTRA, and Lean and MetS Sham controls (n=6 each). Cardiac function was assessed by multi-detector CT, whereas cardiac mitochondrial morphology and function, microvascular remodeling, and injury pathways were assessed ex vivo. PTRA attenuated myocardial mitochondrial damage, improved capillary and microvascular maturity, and ameliorated oxidative stress and fibrosis, in association with attenuation of left ventricular remodeling and diastolic dysfunction. Myocardial mitochondrial damage correlated with myocardial injury and renal dysfunction. Preservation of myocardial mitochondria with PTRA can enhance cardiac recovery, underscoring its therapeutic potential in experimental MetS+RVH.






Similar content being viewed by others
Abbreviations
- RVH:
-
Renovascular hypertension
- MetS:
-
Metabolic syndrome
- PTRA:
-
Percutaneous transluminal renal angioplasty
- ATP:
-
Adenosine triphosphate
- ROS:
-
Reactive oxygen species
- LV:
-
Left ventricular
- PRA:
-
Plasma renin activity
- MCP:
-
Monocyte chemoattractant protein
- IL:
-
Interleukin
- NT-proBNP:
-
N-terminal pro-brain natriuretic peptide
- MDCT:
-
Multi-detector computed tomography
- LVMM:
-
LV muscle mass
- LA:
-
Left atrium
- RBF:
-
Renal blood flow
- GFR:
-
Glomerular filtration rate
- H202 :
-
Hydrogen peroxide
- COX-IV:
-
Cytochrome-c oxidase
- DHE:
-
Dihydroethidium
- WGA:
-
Wheat germ agglutinin
- EDV:
-
End-diastolic volume
References
Herrmann, S. M., & Textor, S. C. (2019). Renovascular hypertension. Endocrinol Metab Clin N Am, 48(4), 765–778.
Green, D., Kalra, P. A., & The heart in atherosclerotic renovascular disease. (2012). Front Biosci (Elite Ed), 4, 856–864.
Textor, S. C., & Lerman, L. O. (2015). Paradigm shifts in atherosclerotic renovascular disease: Where are we now? J Am Soc Nephrol, 26(9), 2074–2080.
Kane, G. C., et al. (2010). Renal artery revascularization improves heart failure control in patients with atherosclerotic renal artery stenosis. Nephrol Dial Transplant, 25(3), 813–820.
Holmuhamedov, E. L., et al. (2012). Cardiac subsarcolemmal and interfibrillar mitochondria display distinct responsiveness to protection by diazoxide. PLoS One, 7(9), e44667.
Duchen, M. R. (2004). Mitochondria in health and disease: Perspectives on a new mitochondrial biology. Mol Asp Med, 25(4), 365–451.
Yuan, F., et al. (2018). Mitochondrial targeted peptides preserve mitochondrial organization and decrease reversible myocardial changes in early swine metabolic syndrome. Cardiovasc Res, 114(3), 431–442.
Yuan, F., et al. (2018). Mitoprotection attenuates myocardial vascular impairment in porcine metabolic syndrome. Am J Physiol Heart Circ Physiol, 314(3), H669–H680.
Eirin, A., et al. (2016). Restoration of mitochondrial cardiolipin attenuates cardiac damage in swine renovascular hypertension. J Am Heart Assoc, 5(6).
Aghajani Nargesi, A., et al. (2020). Renovascular hypertension induces myocardial mitochondrial damage, contributing to cardiac injury and dysfunction in pigs with metabolic syndrome. Am J Hypertens.
Eirin, A., et al. (2018). Mesenchymal stem cell-derived extracellular vesicles improve the renal microvasculature in metabolic renovascular disease in swine. Cell Transplant, 27(7), 1080–1095.
Eirin, A., et al. (2017). Mesenchymal stem cell-derived extracellular vesicles attenuate kidney inflammation. Kidney Int, 92(1), 114–124.
Nargesi, A. A., et al. (2019). Coexisting renal artery stenosis and metabolic syndrome magnifies mitochondrial damage, aggravating poststenotic kidney injury in pigs. J Hypertens, 37(10), 2061–2073.
Farahani, R. A., et al. (2020). Percutaneous transluminal renal angioplasty attenuates poststenotic kidney mitochondrial damage in pigs with renal artery stenosis and metabolic syndrome. J Cell Physiol.
Pawar, A. S., et al. (2015). Adipose tissue remodeling in a novel domestic porcine model of diet-induced obesity. Obesity (Silver Spring), 23(2), 399–407.
Lerman, L. O., et al. (1999). Noninvasive evaluation of a novel swine model of renal artery stenosis. J Am Soc Nephrol, 10(7), 1455–1465.
Eirin, A., et al. (2012). A mitochondrial permeability transition pore inhibitor improves renal outcomes after revascularization in experimental atherosclerotic renal artery stenosis. Hypertension, 60(5), 1242–1249.
Eirin, A., et al. (2011). Persistent kidney dysfunction in swine renal artery stenosis correlates with outer cortical microvascular remodeling. Am J Physiol Ren Physiol, 300(6), F1394–F1401.
Eirin, A., et al. (2012). Adipose tissue-derived mesenchymal stem cells improve revascularization outcomes to restore renal function in swine atherosclerotic renal artery stenosis. Stem Cells, 30(5), 1030–1041.
Eirin, A., et al. (2012). Changes in glomerular filtration rate after renal revascularization correlate with microvascular hemodynamics and inflammation in Swine renal artery stenosis. Circ Cardiovasc Interv, 5(5), 720–728.
Eirin, A., et al. (2015). Intra-renal delivery of mesenchymal stem cells attenuates myocardial injury after reversal of hypertension in porcine renovascular disease. Stem Cell Res Ther, 6, 7.
Rodriguez-Porcel, M., et al. (2004). Long-term antioxidant intervention improves myocardial microvascular function in experimental hypertension. Hypertension, 43(2), 493–498.
Zhu, X. Y., et al. (2007). Simvastatin prevents coronary microvascular remodeling in renovascular hypertensive pigs. J Am Soc Nephrol, 18(4), 1209–1217.
Krier, J. D., et al. (2001). Noninvasive measurement of concurrent single-kidney perfusion, glomerular filtration, and tubular function. Am J Physiol Ren Physiol, 281(4), F630–F638.
Eirin, A., et al. (2016). Urinary mitochondrial DNA copy number identifies chronic renal injury in hypertensive patients. Hypertension, 68(2), 401–410.
Pi, J., et al. (2007). Reactive oxygen species as a signal in glucose-stimulated insulin secretion. Diabetes, 56(7), 1783–1791.
Eirin, A., et al. (2014). Mitochondrial targeted peptides attenuate residual myocardial damage after reversal of experimental renovascular hypertension. J Hypertens, 32(1), 154–165.
Conlon, P. J., et al. (2001). Severity of renal vascular disease predicts mortality in patients undergoing coronary angiography. Kidney Int, 60(4), 1490–1497.
Wright, J. R., et al. (2005). Left ventricular morphology and function in patients with atherosclerotic renovascular disease. J Am Soc Nephrol, 16(9), 2746–2753.
Cooper, C. J., et al. (2014). Stenting and medical therapy for atherosclerotic renal-artery stenosis. N Engl J Med, 370(1), 13–22.
Ritchie, J., et al. (2014). High-risk clinical presentations in atherosclerotic renovascular disease: Prognosis and response to renal artery revascularization. Am J Kidney Dis, 63(2), 186–197.
Hollander, J. M., Thapa, D., & Shepherd, D. L. (2014). Physiological and structural differences in spatially distinct subpopulations of cardiac mitochondria: influence of cardiac pathologies. Am J Physiol Heart Circ Physiol, 307(1), H1–H14.
Wong, H. S., et al. (2017). Production of superoxide and hydrogen peroxide from specific mitochondrial sites under different bioenergetic conditions. J Biol Chem, 292(41), 16804–16809.
Li, Y., et al. (2006). Cytochrome c oxidase subunit IV is essential for assembly and respiratory function of the enzyme complex. J Bioenerg Biomembr, 38(5-6), 283–291.
Bao, L., et al. (2009). Mitochondria are the source of hydrogen peroxide for dynamic brain-cell signaling. J Neurosci, 29(28), 9002–9010.
Kluge, M. A., Fetterman, J. L., & Vita, J. A. (2013). Mitochondria and endothelial function. Circ Res, 112(8), 1171–1188.
Ahmad, A., et al. (2020). Coronary microvascular dysfunction is associated with exertional haemodynamic abnormalities in patients with heart failure with preserved ejection fraction. Eur J Heart Fail.
Zhao, W., et al. (2008). Oxidative stress mediates cardiac fibrosis by enhancing transforming growth factor-beta1 in hypertensive rats. Mol Cell Biochem, 317(1-2), 43–50.
Eirin, A., et al. (2013). Endothelial outgrowth cells shift macrophage phenotype and improve kidney viability in swine renal artery stenosis. Arterioscler Thromb Vasc Biol, 33(5), 1006–1013.
Lerman, L. O., et al. (2001). Increased oxidative stress in experimental renovascular hypertension. Hypertension, 37(2 Pt 2), 541–546.
Wilson, S. H., et al. (1999). Enhanced coronary vasoconstriction to oxidative stress product, 8-epi-prostaglandinF2 alpha, in experimental hypercholesterolemia. Cardiovasc Res, 44(3), 601–607.
Zhang, L., et al. (2020). Selective intrarenal delivery of mesenchymal stem cell-derived extracellular vesicles attenuates myocardial injury in experimental metabolic renovascular disease. Basic Res Cardiol, 115(2), 16.
Eirin, A., et al. (2013). Inflammatory and injury signals released from the post-stenotic human kidney. Eur Heart J, 34(7), 540–548a.
Urbieta-Caceres, V. H., et al. (2012). Selective improvement in renal function preserved remote myocardial microvascular integrity and architecture in experimental renovascular disease. Atherosclerosis, 221(2), 350–358.
Tapuria, N., et al. (2008). Remote ischemic preconditioning: A novel protective method from ischemia reperfusion injury--a review. J Surg Res, 150(2), 304–330.
Mangalat, D., et al. (2009). Value of cardiac CT in patients with heart failure. Curr Cardiovasc Imaging Rep, 2(6), 410–417.
Pipinos, I. I., et al. (1998). Response to angiotensin inhibition in rats with sustained renovascular hypertension correlates with response to removing renal artery stenosis. J Vasc Surg, 28(1), 167–177.
Safian, R. D., & Madder, R. D. (2009). Refining the approach to renal artery revascularization. JACC Cardiovasc Interv, 2(3), 161–174.
Funding
This work was supported by the NIH grants: DK122137, DK104273, DK120292, HL095638, DK118120, and DK102325.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethics Approval
This article does not contain any studies with human participants. All animal studies were approved by the Mayo Clinic Animal Care and Use Committee.
Conflict of Interest
The authors declare no competing interests.
Additional information
Associate Editor Nicola Smart oversaw the review of this article
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
ESM 1
(PDF 1090 kb)
Rights and permissions
About this article
Cite this article
Farahani, R.A., Yu, S., Ferguson, C.M. et al. Renal Revascularization Attenuates Myocardial Mitochondrial Damage and Improves Diastolic Function in Pigs with Metabolic Syndrome and Renovascular Hypertension. J. of Cardiovasc. Trans. Res. 15, 15–26 (2022). https://doi.org/10.1007/s12265-021-10155-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12265-021-10155-3