Abstract
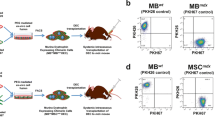
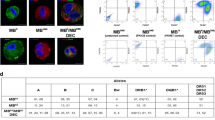
Progressive cardiomyocyte loss in Duchenne muscular dystrophy (DMD) leads to cardiac fibrosis, cardiomyopathy, and eventually heart failure. In the present study, we observed that myogenic progenitor cells (MPC) carry mRNA for the dystrophin gene. We tested whether cardiac function can be improved in DMD by allograft transplantation of MPC-derived exosomes (MPC-Exo) into the heart to restore dystrophin protein expression. Exo from C2C12 cells (an MPC cell line) or vehicle were delivered locally into the hearts of MDX mice. After 2 days of treatment, we observed that MPC-Exo restored dystrophin expression in the hearts of MDX mice, which correlated with improved myocardial function in dystrophin-deficient MDX mouse hearts. In conclusion, this study demonstrated that allogeneic WT-MPC-Exo transplantation transiently restored dystrophin gene expression and improved cardiac function in MDX mice, suggesting that allogenic exosomal delivery may serve as an alternative treatment for cardiomyopathy of DMD.





Similar content being viewed by others
References
Fayssoil, A., Nardi, O., Orlikowski, D., & Annane, D. (2010). Cardiomyopathy in Duchenne muscular dystrophy: pathogenesis and therapeutics. Heart Failure Reviews., 15(1), 103–107.
Gumerson, J. D., & Michele, D. E. (2011). The dystrophin-glycoprotein complex in the prevention of muscle damage. Journal of biomedicine & biotechnology., 2011, 210797.
D’Amario, D., Amodeo, A., Adorisio, R., Tiziano, F. D., Leone, A. M., Perri, G., et al. (2017). A current approach to heart failure in Duchenne muscular dystrophy. Heart (British Cardiac Society)., 103(22), 1770–1779.
Kamdar, F., & Garry, D. J. (2016). Dystrophin-deficient cardiomyopathy. Journal of the American College of Cardiology, 67(21), 2533–2546.
Siemionow, M., Cwykiel, J., Heydemann, A., Garcia-Martinez, J., Siemionow, K., & Szilagyi, E. (2018). Creation of dystrophin expressing chimeric cells of myoblast origin as a novel stem cell based therapy for Duchenne muscular dystrophy. Stem cell reviews., 14(2), 189–199.
Lee Y, El Andaloussi S, Wood MJ. Exosomes and microvesicles: extracellular vesicles for genetic information transfer and gene therapy. Human molecular genetics. 2012;21(R1):R125–R134.
Aminzadeh, M. A., Rogers, R. G., Fournier, M., Tobin, R. E., Guan, X., Childers, M. K., et al. (2018). Exosome-mediated benefits of cell therapy in mouse and human models of Duchenne muscular dystrophy. Stem cell reports., 10(3), 942–955.
Tang, Y. T., Huang, Y. Y., Zheng, L., Qin, S. H., Xu, X. P., An, T. X., et al. (2017). Comparison of isolation methods of exosomes and exosomal RNA from cell culture medium and serum. International Journal of Molecular Medicine, 40(3), 834–844.
Hu, G., Yao, H., Chaudhuri, A. D., Duan, M., Yelamanchili, S. V., Wen, H., et al. (2012). Exosome-mediated shuttling of microRNA-29 regulates HIV Tat and morphine-mediated neuronal dysfunction. Cell Death & Disease, 3, e381.
Ruan, X. F., Li, Y. J., Ju, C. W., Shen, Y., Lei, W., Chen, C., et al. (2018). Exosomes from Suxiao Jiuxin pill-treated cardiac mesenchymal stem cells decrease H3K27 demethylase UTX expression in mouse cardiomyocytes in vitro. Acta Pharmacologica Sinica, 39(4), 579–586.
Ruan, X. F., Ju, C. W., Shen, Y., Liu, Y. T., Kim, I. M., Yu, H., et al. (2018). Suxiao Jiuxin pill promotes exosome secretion from mouse cardiac mesenchymal stem cells in vitro. Acta Pharmacologica Sinica, 39(4), 569–578.
Chen, Z., Li, Y., Yu, H., Shen, Y., Ju, C., Ma, G., et al. (2017). Isolation of extracellular vesicles from stem cells. Methods in molecular biology (Clifton, NJ)., 1660, 389–394.
Wang, Y., Zhang, L., Li, Y., Chen, L., Wang, X., Guo, W., et al. (2015). Exosomes/microvesicles from induced pluripotent stem cells deliver cardioprotective miRNAs and prevent cardiomyocyte apoptosis in the ischemic myocardium. International journal of cardiology., 192, 61–69.
Helwa, I., Cai, J., Drewry, M. D., Zimmerman, A., Dinkins, M. B., Khaled, M. L., et al. (2017). A comparative study of serum exosome isolation using differential ultracentrifugation and three commercial reagents. PLoS One, 12(1), e0170628.
Bayoumi AS, Park KM, Wang Y, Teoh JP, Aonuma T, Tang Y, et al. A carvedilol-responsive microRNA, miR-125b-5p protects the heart from acute myocardial infarction by repressing pro-apoptotic bak1 and klf13 in cardiomyocytes. Journal of molecular and cellular cardiology. 2018;114:72–82.
Liu, N., Williams, A. H., Maxeiner, J. M., Bezprozvannaya, S., Shelton, J. M., Richardson, J. A., et al. (2012). microRNA-206 promotes skeletal muscle regeneration and delays progression of Duchenne muscular dystrophy in mice. The Journal of Clinical Investigation, 122(6), 2054–2065.
Terrill, J. R., Pinniger, G. J., Graves, J. A., Grounds, M. D., & Arthur, P. G. (2016). Increasing taurine intake and taurine synthesis improves skeletal muscle function in the mdx mouse model for Duchenne muscular dystrophy. The Journal of physiology., 594(11), 3095–3110.
Messina, S., Bitto, A., Aguennouz, M., Mazzeo, A., Migliorato, A., Polito, F., et al. (2009). Flavocoxid counteracts muscle necrosis and improves functional properties in mdx mice: a comparison study with methylprednisolone. Experimental neurology., 220(2), 349–358.
McDonald CM, Campbell C, Torricelli RE, Finkel RS, Flanigan KM, Goemans N, et al. Ataluren in patients with nonsense mutation Duchenne muscular dystrophy (ACT DMD): a multicentre, randomised, double-blind, placebo-controlled, phase 3 trial. Lancet (London, England). 2017;390(10101):1489–1498.
Sakamoto, M., Yuasa, K., Yoshimura, M., Yokota, T., Ikemoto, T., Suzuki, M., et al. (2002). Micro-dystrophin cDNA ameliorates dystrophic phenotypes when introduced into mdx mice as a transgene. Biochemical and Biophysical Research Communications, 293(4), 1265–1272.
Mendell, J. R., Sahenk, Z., Malik, V., Gomez, A. M., Flanigan, K. M., Lowes, L. P., et al. (2015). A phase 1/2a follistatin gene therapy trial for Becker muscular dystrophy. Molecular therapy: the journal of the American Society of Gene Therapy., 23(1), 192–201.
Syed, Y. Y. (2016). Eteplirsen: first global approval. Drugs, 76(17), 1699–1704.
Zhang, Y., Long, C., Li, H., McAnally, J. R., Baskin, K. K., Shelton, J. M., et al. (2017). CRISPR-Cpf1 correction of muscular dystrophy mutations in human cardiomyocytes and mice. Science advances., 3(4), e1602814.
Young, C. S., Hicks, M. R., Ermolova, N. V., Nakano, H., Jan, M., Younesi, S., et al. (2016). A single CRISPR-Cas9 deletion strategy that targets the majority of DMD patients restores dystrophin function in hiPSC-derived muscle cells. Cell Stem Cell, 18(4), 533–540.
Gauvreau, M. E., Cote, M. H., Bourgeois-Daigneault, M. C., Rivard, L. D., Xiu, F., Brunet, A., et al. (2009). Sorting of MHC class II molecules into exosomes through a ubiquitin-independent pathway. Traffic (Copenhagen, Denmark)., 10(10), 1518–1527.
Hagan, M., Ashraf, M., Kim, I. M., Weintraub, N. L., & Tang, Y. (2018). Effective regeneration of dystrophic muscle using autologous iPSC-derived progenitors with CRISPR-Cas9 mediated precise correction. Medical hypotheses., 110, 97–100.
Kanelidis, A. J., Premer, C., Lopez, J., Balkan, W., & Hare, J. M. (2017). Route of delivery modulates the efficacy of mesenchymal stem cell therapy for myocardial infarction: a meta-analysis of preclinical studies and clinical trials. Circulation research., 120(7), 1139–1150.
Zhang, L., Hoffman, J. A., & Ruoslahti, E. (2005). Molecular profiling of heart endothelial cells. Circulation, 112(11), 1601–1611.
Kim, H., Yun, N., Mun, D., Kang, J. Y., Lee, S. H., Park, H., et al. (2018). Cardiac-specific delivery by cardiac tissue-targeting peptide-expressing exosomes. Biochemical and biophysical research communications., 499(4), 803–808.
Funding
I. Kim, N.L. Weintraub, and Y. Tang were partially supported by the American Heart Association: GRNT31430008, NIH-AR070029, NIH-HL086555, NIH-HL134354, and NIH -HL12425.
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
This article does not contain any studies with human participants performed by any of the authors.
Animals were handled according to approved protocols and animal welfare regulations of the Institutional Animal Care and Use Committee of the Medical College of Georgia/Augusta University.
Conflict of Interest
The authors declare that they have no conflict of interest.
Additional information
Associate Editor Enrique Lara-Pezzi oversaw the review of this article
Rights and permissions
About this article
Cite this article
Su, X., Jin, Y., Shen, Y. et al. Exosome-Derived Dystrophin from Allograft Myogenic Progenitors Improves Cardiac Function in Duchenne Muscular Dystrophic Mice. J. of Cardiovasc. Trans. Res. 11, 412–419 (2018). https://doi.org/10.1007/s12265-018-9826-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12265-018-9826-9