Abstract
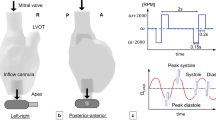
The SynCardia total artificial heart (TAH) is the only Food and Drug Administration (FDA) approved device for replacing hearts in patients with congestive heart failure. It pumps blood via pneumatically driven diaphragms and controls the flow with mechanical valves. While it has been successfully implanted in more than 1300 patients, its size precludes implantation in smaller patients. This study’s aim was to evaluate the viability of scaled-down TAHs by quantifying thrombogenic potentials from flow patterns. Simulations of systole were first conducted with stationary valves, followed by an advanced full-cardiac cycle model with moving valves. All the models included deforming diaphragms and platelet suspension in the blood flow. Flow stress accumulations were computed for the platelet trajectories and thrombogenic potentials were assessed. The simulations successfully captured complex flow patterns during various phases of the cardiac cycle. Increased stress accumulations, but within the safety margin of acceptable thrombogenicity, were found in smaller TAHs, indicating that they are clinically viable.






Similar content being viewed by others
References
Copeland, J. G., Smith, R. G., Arabia, F. A., Nolan, P. E., Sethi, G. K., Tsau, P. H., McClellan, D., & Slepian, M. J. (2004). Cardiac replacement with a total artificial heart as a bridge to transplantation. The New England Journal of Medicine, 351(9), 859–867. doi:10.1056/NEJMoa040186.
Slepian, M. J., Smith, R. G., & Copeland, J. C. (2006). The SynCardia CardioWest total artificial heart. In K. L. Baughman & W. A. Baumgartner (Eds.), Treatment of advanced heart disease, vol 56. Fundamental and clinical cardiology series (pp. 473–490). New York: Taylor & Francis Group.
Frazier, O. H., & Cohn, W. E. (2012). Continuous-flow total heart replacement device implanted in a 55-year-old man with end-stage heart failure and severe amyloidosis. Texas Heart Institute journal / from the Texas Heart Institute of St Luke’s Episcopal Hospital, Texas Children’s Hospital, 39(4), 542–546.
Slepian, M. J., Alemu, Y., Girdhar, G., Soares, J. S., Smith, R. G., Einav, S., & Bluestein, D. (2013). The Syncardia total artificial heart: in vivo, in vitro, and computational modeling studies. Journal of Biomechanics, 46(2), 266–275. doi:10.1016/j.jbiomech.2012.11.032.
Platis, A., & Larson, D. F. (2009). CardioWest temporary total artificial heart. Perfusion, 24(5), 341–346. doi:10.1177/0267659109351330.
Girdhar, G., Xenos, M., Alemu, Y., Chiu, W. C., Lynch, B. E., Jesty, J., Einav, S., Slepian, M. J., & Bluestein, D. (2012). Device thrombogenicity emulation: a novel method for optimizing mechanical circulatory support device thromboresistance. PLoS One, 7(3), e32463. doi:10.1371/journal.pone.0032463.
Xenos, M., Girdhar, G., Alemu, Y., Jesty, J., Slepian, M., Einav, S., & Bluestein, D. (2010). Device Thrombogenicity Emulator (DTE)—design optimization methodology for cardiovascular devices: a study in two bileaflet MHV designs. Journal of Biomechanics, 43(12), 2400–2409. doi:10.1016/j.jbiomech.2010.04.020.
Kroll, M. H., Hellums, J. D., McIntire, L. V., Schafer, A. I., & Moake, J. L. (1996). Platelets and shear stress. Blood, 88(5), 1525–1541.
Leshnower, B. G., Smith, R. G., Ohara, M. L., Woo, J., Pochettino, A., Morris, R. J., Gardner, T. J., Slepian, M. J., Copeland, J. G., Acker, M. A. (2007). Is the total artificial heart superior to BIVAD therapy as a method of bridging patients to heart transplantation? Paper presented at the 43rd Annual meeting of the Society of Thoracic Surgeons, San Diego, CA, January 29–31.
Copeland, J. G., Copeland, H., Gustafson, M., Mineburg, N., Covington, D., Smith, R. G., & Friedman, M. (2012). Experience with more than 100 total artificial heart implants. The Journal of Thoracic and Cardiovascular Surgery, 143(3), 727–734. doi:10.1016/j.jtcvs.2011.12.002.
Richards, K. E., Deserranno, D., Donal, E., Greenberg, N. L., Thomas, J. D., & Garcia, M. J. (2004). Influence of structural geometry on the severity of bicuspid aortic stenosis. American Journal of Physiology. Heart and Circulatory Physiology, 287(3), H1410–H1416. doi:10.1152/ajpheart.00264.2003.
Alemu, Y., & Bluestein, D. (2007). Flow-induced platelet activation and damage accumulation in a mechanical heart valve: numerical studies. Artificial Organs, 31(9), 677–688. doi:10.1111/j.1525-1594.2007.00446.x.
Borazjani, I., Ge, L., & Sotiropoulos, F. (2010). High-resolution fluid-structure interaction simulations of flow through a bi-leaflet mechanical heart valve in an anatomic aorta. Annals of Biomedical Engineering, 38(2), 326–344. doi:10.1007/s10439-009-9807-x.
Hong, T., & Kim, C. N. (2011). A numerical analysis of the blood flow around the bileaflet mechanical heart valves with different rotational implantation angles. Journal of Hydrodynamics, 23(5), 607–614. doi:10.1016/S1001-6058(10)60156-4.
Dumont, K., Vierendeels, J., Kaminsky, R., van Nooten, G., Verdonck, P., & Bluestein, D. (2007). Comparison of the hemodynamic and thrombogenic performance of two bileaflet mechanical heart valves using a CFD/FSI model. Journal of Biomechanical Engineering, 129(4), 558–565. doi:10.1115/1.2746378.
Hose, D. R., Narracott, A. J., Penrose, J. M., Baguley, D., Jones, I. P., & Lawford, P. V. (2006). Fundamental mechanics of aortic heart valve closure. Journal of Biomechanics, 39(5), 958–967. doi:10.1016/j.jbiomech.2005.01.029.
Dasi, L. P., Ge, L., Simon, H. A., Sotiropoulos, F., & Yoganathan, A. P. (2007). Vorticity dynamics of a bileaflet mechanical heart valve in an axisymmetric aorta. Physics of Fluids, 19(6), 067105. doi:10.1063/1.2743261.
Chiu, W. C., Slepian, M. J., & Bluestein, D. (2014). Thrombus formation patterns in the HeartMate II ventricular assist device: clinical observations can be predicted by numerical simulations. ASAIO Journal, 60(2), 237–240. doi:10.1097/MAT.0000000000000034.
Zhang, J., Zhang, P., Fraser, K. H., Griffith, B. P., & Wu, Z. J. (2013). Comparison and experimental validation of fluid dynamic numerical models for a clinical ventricular assist device. Artificial Organs, 37(4), 380–389. doi:10.1111/j.1525-1594.2012.01576.x.
Sonntag, S. J., Kaufmann, T. A. S., Busen, M. R., Laumen, M., Linde, T., Schmitz-Rode, T., & Steinseifer, U. (2013). Simulation of a pulsatile total artificial heart: development of a partitioned Fluid Structure Interaction model. Journal of Fluid and Structures, 38, 187–204. doi:10.1016/j.jfluidstructs.2012.11.011.
Penrose, J. M. T., & Staples, C. J. (2002). Implicit fluid-structure coupling for simulation of cardiovascular problems. International Journal for Numerical Methods in Fluids, 40(3–4), 467–478. doi:10.1002/Fld.306.
Avrahami, I., Rosenfeld, M., Raz, S., & Einav, S. (2006). Numerical model of flow in a sac-type ventricular assist device. Artificial Organs, 30(7), 529–538. doi:10.1111/j.1525-1594.2006.00255.x.
Medvitz, R. B., Reddy, V., Deutsch, S., Manning, K. B., & Paterson, E. G. (2009). Validation of a CFD methodology for positive displacement LVAD analysis using PIV data. Journal of Biomechanical Engineering, 131(11), 111009. doi:10.1115/1.4000116.
Topper, S. R., Navitsky, M. A., Medvitz, R. B., Paterson, E. G., Siedlecki, C. A., Slattery, M. J., Deutsch, S., Rosenberg, G., & Manning, K. B. (2014). The use of fluid mechanics to predict regions of microscopic thrombus formation in pulsatile VADs. Cardiovascular Engineering and Technology, 5(1), 54–69. doi:10.1007/s13239-014-0174-x.
Govindarajan, V., Udaykumar, H. S., Herbertson, L. H., Deutsch, S., Manning, K. B., & Chandran, K. B. (2010). Two-dimensional FSI simulation of closing dynamics of a tilting disk mechanical heart valve. Journal of Medical Devices, 4(1), 011001. doi:10.1115/1.4000876.
Pelliccioni, O., Cerrolaza, M., & Herrera, M. (2007). Lattice Boltzmann dynamic simulation of a mechanical heart valve device. Mathematics and Computers in Simulation, 75(1–2), 1–14. doi:10.1016/j.matcom.2006.08.005.
Marom, G. (2014). Numerical methods for fluid–structure interaction models of aortic valves. Archives of Computational Methods in Engineering 1–26. doi:10.1007/s11831-014-9133-9.
Donovan, F. M. (1975). Design of a hydraulic analog of the circulatory system for evaluating artificial hearts. Biomaterials, Medical Devices, and Artificial Organs, 3(4), 439–449. doi:10.3109/10731197509118635.
Yoganathan, A. P., Chandran, K. B., & Sotiropoulos, F. (2005). Flow in prosthetic heart valves: state-of-the-art and future directions. Annals of Biomedical Engineering, 33(12), 1689–1694. doi:10.1007/s10439-005-8759-z.
Fraser, K. H., Zhang, T., Taskin, M. E., Griffith, B. P., & Wu, Z. J. (2012). A quantitative comparison of mechanical blood damage parameters in rotary ventricular assist devices: shear stress, exposure time and hemolysis index. Journal of Biomechanical Engineering, 134(8), 081002. doi:10.1115/1.4007092.
Nobili, M., Morbiducci, U., Ponzini, R., Gaudio, C. D., Balducci, A., Grigioni, M., Montevecchi, F. M., & Redaelli, A. (2008). Numerical simulation of the dynamics of a bileaflet prosthetic heart valve using a fluid–structure interaction approach. Journal of Biomechanics, 41, 2539–2550. doi:10.1016/j.jbiomech.2008.05.004.
Acknowledgments
We thank Matthew Pollack from Boston University for his help in reconstructing the geometry. We also thank Doug Nutter and Richard Smith for information on TAH engineering drawings and operating conditions. The software was provided by an ANSYS Academic Partnership with Stony Brook University.
Conflict of Interest
Dr. Slepian declares participation in review activities for SynCardia Inc. All the other authors declare no conflict of interest. No human or animal studies were carried out by the authors for this article.
Sources of Funding
This study was funded by grants from the National Institute of Health: National Institute of Biomedical Imaging and Bioengineering Quantum Award: Implementation Phase II-U01 EB012487-04 (D.B.).
Author information
Authors and Affiliations
Corresponding author
Additional information
Editor-in-Chief Jennifer L. Hall oversaw the review of this article
Electronic Supplementary Material
Below is the link to the electronic supplementary material.
(MPG 193154 kb)
Rights and permissions
About this article
Cite this article
Marom, G., Chiu, WC., Crosby, J.R. et al. Numerical Model of Full-Cardiac Cycle Hemodynamics in a Total Artificial Heart and the Effect of Its Size on Platelet Activation. J. of Cardiovasc. Trans. Res. 7, 788–796 (2014). https://doi.org/10.1007/s12265-014-9596-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12265-014-9596-y