Abstract
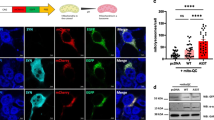
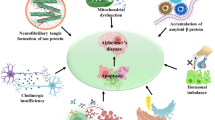
Accumulation and aggregation of β-amyloid (Aβ) peptides result in neuronal death, leading to cognitive dysfunction in Alzheimer’s disease. The self-assembled Aβ molecules form various intermediate aggregates including oligomers that are more toxic to neurons than the mature aggregates, including fibrils. Thus, one strategy to alleviate Aβ toxicity is to facilitate the conversion of Aβ intermediates to larger aggregates such as fibrils. In this study, we designed a peptide named A3 that significantly enhanced the formation of amorphous aggregates of Aβ by accelerating the aggregation kinetics. Thioflavin T fluorescence experiments revealed an accelerated aggregation of Aβ monomers, accompanying reduced Aβ cytotoxicity. Transgenic Caenorhabditis elegans over-expressing amyloid precursor protein exhibited paralysis due to the accumulation of Aβ oligomers, and this phenotype was attenuated by feeding the animals with A3 peptide. These findings suggest that the Aβ aggregation-promotion effect can potentially be useful for developing strategies to reduce Aβ toxicity.





Similar content being viewed by others
References
Selkoe, Dennis J. Physiological production of the β-amyloid protein and the mechanism of Alzheimer’s disease. Trends Neurosci 1993, 16: 403–409.
Pike CJ, Burdick D, Walencewicz AJ, Glabe CG, Cotman CW. Neurodegeneration induced by beta-amyloid peptides in vitro: The role of peptide assembly state. J Neurosci 1993, 13: 1676–1687.
Selkoe DJ. Alzheimer’s disease–genotypes, phenotype, and treatments. Science 1997, 275: 322–330.
Hardy J, Selkoe DJ. The amyloid hypothesis of Alzheimer’s disease: progress and problems on the road to therapeutics. Science 2002, 297: 353–356.
Drouet B, Pinçon-Raymond M, Chambaz J, Pillot T. Molecular basis of Alzheimer’s disease. Cell Mol Life Sci 2000, 57: 705–715.
Caughey B, Lansbury PT. Protofibrils, pores, fibrils, and neurodegeneration: separating the responsible protein aggregates from the innocent bystanders. Annu Rev Neurosci 2003, 26: 267–298.
Haass C, Selkoe DJ. Soluble protein oligomers in neurodegeneration: lessons from the Alzheimer’s amyloid beta-peptide. Nat Rev Mol Cell Biol 2007, 8: 101–112.
Morgado I, Fändrich M. Assembly of Alzheimer’s Aβ peptide into nanostructured amyloid fibrils. Curr Opin Colloid Interface Sci 2011, 16: 508–514.
Lambert MP, Barlow AK, Chromy BA, Edwards C, Freed R, Klein W L, et al. Diffusible, nonfibrillar ligands derived from A1-42 are potent central nervous system neurotoxins. Proc Natl Acad Sci U S A 1998, 95: 6448–6453.
Pallitto MM, Ghanta J, Heinzelman P, Kiessling LL, Murphy RM. Recognition sequence design for peptidyl modulators of beta-amyloid aggregation and toxicity. Biochemistry 1999, 38: 3570–3578.
Ward RV, Jennings KH, Jepras R, Neville W, Owen DE, Howlett DR, et al. Fractionation and characterization of oligomeric, protofibrillar and fibrillar forms of beta-amyloid peptide. Biochem J 2000, 348: 137–144.
Kirkitadze MD, Bitan G, Teplow DB. Paradigm shifts in Alzheimer’s disease and other neurodegenerative disorders: The emerging role of oligomeric assemblies. J Neurosci Res 2002, 69: 567–577.
Lu B, Nagappan G, Guan X, Wren P. BDNF-based synaptic repair as a disease-modifying strategy for neurodegenerative diseases. Nat Rev Neurosci 2013, 14: 401–416.
Klajnert B, Wasiak T, Ionov M, Fernandez-Villamarin M, Sousa-Herves A, Correa J, et al. Dendrimers reduce toxicity of Aβ 1-28 peptide during aggregation and accelerate fibril formation. Nanomedicine 2012, 8:1372.
Zhu LJ, Song Y, Cheng PN, Jeffrey SM. Molecular design for dual modulation effect of amyloid protein aggregation. J Am Chem Soc 2015, 137: 8062–8068.
Fändrich M, Fletcher MA, Dobson CM. Amyloid fibrils from muscle myoglobin. Nature 2001, 410: 165–166.
Kowalewski T, Holtzman DM. In situ atomic force microscopy study of Alzheimer’s β-amyloid peptide on different substrates: New insights into mechanism of β-sheet formation. Proc Natl Acad Sci U S A 1999, 96: 3688–3693.
Mao X, Wang Y, Liu L, Niu L, Yang YL, Wang W. Molecular-level evidence of the surface-induced transformation of peptide structures revealed by scanning tunneling microscopy. Langmuir 2009, 25: 8849–8853.
Lorenzo A, Yankner BA. β-amyloid neurotoxicity requires fibril formation and is inhibited by Congo Red. Proc Natl Acad Sci U S A 1995, 91: 12243–12247.
Woods LA, Platt GW, Hellewell AL, Hewitt EW, Homans SW, Ashcroft AE, et al. Ligand binding to distinct states diverts aggregation of an amyloid-forming protein. Nat Chem Biol 2011, 7: 730–739.
Geng J, Li M, Ren JS, Wang EB, Qu XG. Polyoxometalates as inhibitors of the aggregation of amyloid β peptides associated with Alzheimer’s disease. Angew Chem Int Ed Engl 2011, 50: 4184–4188.
Alavez S, Vantipalli MC, Zucker DJS, Klang IM, Lithgow GJ. Amyloid-binding compounds maintain protein homeostasis during ageing and extend lifespan. Nature 2011, 472: 226–229.
Fändrich M. Oligomeric intermediates in amyloid formation: Structure determination and mechanisms of toxicity. J Mol Biol 2012, 421: 427–440.
Morgado I, Fändrich M. Assembly of Alzheimer’s Aβ peptide into nanostructured amyloid fibrils. Curr Opin Colloid Interface Sci 2011, 16: 508–514.
Choi JS, Braymer JJ, Nanga RPR, Ramamoorthy A, Lim MH. Design of small molecules that target metal-A species and regulate metal-induced A aggregation and neurotoxicity. Proc Natl Acad Sci U S A 2010, 107: 21990–21995.
Yoo SI, Yang M, Brender JR, Subramanian V, Sun K, Joo NE. Innentitelbild: inhibition of amyloid peptide fibrillation by inorganic nanoparticles: functional similarities with proteins (Angew. Chem. 22/2011). Angew Chem, 2011, 123: 5096. doi:10.1002/ange.201102689.
Klajnert B, Wasiak T, Ionov M, Fernandez-Villamarin M, Sousa-Herves A, Correa J, et al. Dendrimers reduce toxicity of Aβ 1-28 peptide during aggregation and accelerate fibril formation. Nanomedicine 2012, 8: 1372–1378.
Moran PM, Higgins LS, Cordell B. Age-related learning deficits in transgenic mice expressing the 751-amino acid isoform of human beta-amyloid precursor protein. Proc Natl Acad Sci U S A 1995, 92: 5341–5345.
Ohno M, Chang L, Tseng W. Temporal memory deficits in Alzheimer’s mouse models: rescue by genetic deletion of BACE1. Eur J Neurosci, 2006, 23: 251–260.
Link CD. Expression of human beta-amyloid peptide in transgenic Caenorhabditis elegans. Proc Natl Acad Sci U S A 1995, 92: 9368–9372.
Link CD, Taft A, Kapulkin V, Duke K, Kim S, Fei Q, et al. Gene expression analysis in a transgenic Caenorhabditis elegans, Alzheimer’s disease model. Neurobiol Aging, 2003, 24: 397–413.
Cheng B, Gong H, Xiao H, Petersen RB, Zheng L, Huang K. Inhibiting toxic aggregation of amyloidogenic proteins: a therapeutic strategy for protein misfolding diseases. Biochim Biophys Acta 2013, 1830: 4860–4871.
Pike CJ, Walencewiczwasserman AJ, Kosmoski J, Cribbs DH, Glabe CG, Cotman CW, et al. Structure-activity analyses of beta-amyloid peptides: contributions of the beta 25-35 region to aggregation and neurotoxicity. J Neurochem 1995, 64: 253–265.
Scrocchi LA, Ha K, Chen Y, Wu L, Wang F, Fraser PE. Identification of minimal peptide sequences in the (8-20) domain of human islet amyloid polypeptide involved in fibrillogenesis. J Struct Biol 2003, 141: 218–227.
Du HN, Li HT, Zhang F, Lin XJ, Shi JH, Shi YH, et al. Acceleration of alpha-synuclein aggregation by homologous peptides. FEBS Lett 2006, 580: 3657–3664.
Kim JR, Murphy RM. Mechanism of accelerated assembly of beta-amyloid filaments into fibrils by KLVFFK(6). Biophys J 2004, 86: 3194–3203.
Re F, Airoldi C, Zona C, Masserini M, La FB, Quattrocchi N, et al. Beta amyloid aggregation inhibitors: small molecules as candidate drugs for therapy of Alzheimer’s disease. Curr Med Chem 2010, 17: 2990–3006.
Matthew B, Shohei K. Molecular mechanism of thioflavin-T binding to amyloid fibrils. Biochim Biophys Acta 2010, 1804: 1405–1412.
Krebs MR, Bromley EH, Donald AM. The binding of thioflavin-T to amyloid fibrils: localisation and implications. J Struct Biol 2005, 149: 30–37.
Wu Y, Wu Z, Butko P, Christen Y, Lambert MP, Klein WL, et al. Amyloid-beta-induced pathological behaviors are suppressed by Ginkgo biloba extract EGb 761 and ginkgolides in transgenic Caenorhabditis elegans. J Neurosci 2006, 26: 13102–13113.
Bharadwaj PR, Dubey AK, Masters CL, Martins RN, Macreadie IG. Aβ aggregation and possible implications in Alzheimer’s disease pathogenesis. J Cell Mol Med 2009, 13: 412–421.
Bieschke J, Lindquist S. EGCG remodels mature alpha-synuclein and amyloid-beta fibrils and reduces cellular toxicity. Proc Natl Acad Sci U S A 2010, 107: 7710–7715.
Acknowledgements
We gratefully acknowledge Prof. Bai Lu of Tsinghua University for his help and thoughtful suggestions on the manuscript. This work was supported by the National Natural Science Foundation of China (91127043, 31600803, and 21273051).
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Yang, A., Wang, C., Song, B. et al. Attenuation of β-Amyloid Toxicity In Vitro and In Vivo by Accelerated Aggregation. Neurosci. Bull. 33, 405–412 (2017). https://doi.org/10.1007/s12264-017-0144-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12264-017-0144-z