Abstract
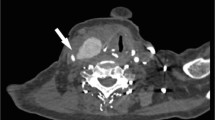
This is a case report of a 63-year-old man who presented with a pseudoaneurysm of the left common carotid artery following a previous neck injury. The pseudoaneurysm was discovered incidentally during a routine Doppler ultrasound of the neck after the patient suffered a stroke with right-sided hemiparesis and dysphasia. A multi-detector computed tomography angiography scan showed a 25-mm pseudoaneurysm with a partial thrombus in the lumen, originating from the left common carotid artery. The patient underwent open surgery with reconstruction done by the interposition of a prosthetic graft between the common and internal carotid arteries. The postoperative course was uneventful, and the patient was discharged on the third postoperative day. The rarity of extracranial carotid artery pseudoaneurysms and their potential to cause serious complications such as stroke and rupture underscores the need for prompt diagnosis and management. The question of the best treatment remains controversial, and there are no studies that directly compare the success of open surgery and endovascular treatment of extracranial carotid artery pseudoaneurysm. Regular ultrasound monitoring should be performed in patients with confirmed neck trauma and/or operations to detect any delayed onset of carotid pseudoaneurysms.


Similar content being viewed by others
Data Availability
The data that support the findings of this study are available from the corresponding author, upon reasonable request.
References
Miksic K, Flis V, Kosir G, Pavlovic M, Tetickovic E (1997) Surgical aspects of fusiform and saccular extracranial carotid artery aneurysms. Cardiovasc Surg 5:190–195. https://doi.org/10.1016/s0967-2109(96)00088-9
Srivastava SD, Eagleton MJ, O’Hara P, Kashyap VS, Sarac T, Clair D (2010) Surgical repair of carotid artery aneurysms: a 10-year, single-center experience. Ann Vasc Surg 24:100–105. https://doi.org/10.1016/j.avsg.2009.09.006
Garg K, Rockman CB, Lee V, Maldonado TS, Jacobowitz GR, Adelman MA, Mussa FF (2012) Presentation and management of carotid artery aneurysms and pseudoaneurysms. J Vasc Surg 55:1618–1622. https://doi.org/10.1016/j.jvs.2011.12.054
Fankhauser GT, Stone WM, Fowl RJ, O’Donnell ME, Bower TC, Meyer FB, Money SR (2015) Surgical and medical management of extracranial carotid artery aneurysms. J Vasc Surg 61:389–393. https://doi.org/10.1016/j.jvs.2014.07.092
Zhou W, Lin PH, Bush RL, Peden E, Guerrero MA, Terramani T, Lubbe DF, Nguyen L, Lumsden AB (2006) Carotid artery aneurysm: evolution of management over two decades. J Vasc Surg 43:493–496. https://doi.org/10.1016/j.jvs.2005.11.023
Magge D, Farber A, Vladimir F, Woodson J, Collins K, Shaw P, Gibbons G (2008) Diagnosis and management of traumatic pseudoaneurysm of the carotid artery: case report and review of the literature. Vascular 16:350–355. https://doi.org/10.2310/6670.2008.00047
Spanos K, Karathanos C, Stamoulis K, Giannoukas AD (2016) Endovascular treatment of traumatic internal carotid artery pseudoaneurysm. Injury 47:307–312. https://doi.org/10.1016/j.injury.2015.09.015
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethics Approval and Consent to Participate
The ethics committee of our Institution approved this manuscript. Written informed consent for patient information and images to be published, was obtained.
Competing Interests
The authors declare that there is no conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Gajin, P., Petrovic, J., Cimbaljevic, N. et al. Symptomatic Carotid Artery Pseudoaneurysm 28 Years After Neck Trauma. Indian J Surg 86, 214–216 (2024). https://doi.org/10.1007/s12262-023-03827-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12262-023-03827-8