Abstract
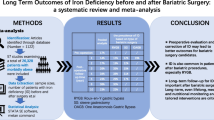
Iron deficiency anemia (IDA) is one of the most common nutritional problems in patients with obesity and after bariatric surgery. While it can be reduced with diet and oral supplementation, a subset of patients is refractory to these measures. Several factors have been implicated including high hepcidin levels reducing the release of absorbed iron into the circulation. We found 6 papers studying hepcidin levels before and after bariatric surgery. Patients with obesity have higher hepcidin and other inflammatory markers. Five out of six studies reported significant falls in hepcidin levels after bariatric surgery. This was accompanied by an improvement in the RBC morphology indices in restrictive surgeries. However, the fall in hepcidin is not uniform and may be a contributing factor for refractory IDA.

Similar content being viewed by others
References
Obinwanne KM, Fredrickson KA, Mathiason MA, Kallies KJ, Farnen JP, Kothari SN (2014) Incidence, treatment, and outcomes of iron deficiency after laparoscopic Roux-en-Y gastric bypass: a 10-year analysis. J Am Coll Surg 218:246–252. https://doi.org/10.1016/j.jamcollsurg.2013.10.023
Rojas P, Carrasco F, Codoceo J, Inostroza J, Basfi-Fer K, Papapietro K, Csendes A, Rojas J, Pizarro F, Olivares M, Ruz M (2011) Trace element status and inflammation parameters after 6 months of Roux-en-Y gastric bypass. Obes Surg 21:561–568. https://doi.org/10.1007/s11695-011-0368-3
Steenackers N, Van der Schueren B, Mertens A, Lannoo M, Grauwet T, Augustijns P, Matthys C (2018) Iron deficiency after bariatric surgery: what is the real problem? Proc Nutr Soc 77:445–455. https://doi.org/10.1017/S0029665118000149
Parrott J, Frank L, Rabena R, Craggs-Dino L, Isom KA, Greiman L (2016) American society for metabolic and bariatric surgery integrated health nutritional guidelines for the surgical weight loss patient 2016 update: micronutrients. Surg Obes Relat Dis 13:727–741. https://doi.org/10.1016/j.soard.2016.12.018
Thomas DW, Hinchliffe RF, Briggs C, Macdougall IC, Littlewood T, Cavill I, British Committee for Standards in Haematology (2013) Guideline for the laboratory diagnosis of functional iron deficiency. Br J Haematol 161:639–648. https://doi.org/10.1111/BJH.12311
Cheng HL, Bryant C, Cook R, O’Connor H, Rooney K, Steinbeck K (2012) The relationship between obesity and hypoferraemia in adults: a systematic review. Obes Rev 13:150–161
Tussing-Humphreys L, Pustacioglu C, Nemeth E, Braunschweig C (2012) Rethinking iron regulation and assessment in iron deficiency, anemia of chronic disease, and obesity: introducing hepcidin. J Acad Nutr Diet 112:391–400. https://doi.org/10.1016/J.JADA.2011.08.038
Muñoz M, Botella-Romero F, Gómez-Ramírez S, Campos A, García-Erce JA (2009) Iron deficiency and anaemia in bariatric surgical patients: causes, diagnosis and proper management. Nutr Hosp 24:640–654. https://doi.org/10.3305/NH.2009.24.6.4547
Careaga M, Moizé V, Flores L, Deulofeu R, Andreu A, Vidal J (2015) Inflammation and iron status in bariatric surgery candidates. Surg Obes Relat Dis 11:906–911. https://doi.org/10.1016/J.SOARD.2014.09.028
Macdougall IC, Malyszko J, Hider RC, Bansal SS (2010) Current status of the measurement of blood hepcidin levels in chronic kidney disease. Clin J Am Soc Nephrol 5:1681–1689. https://doi.org/10.2215/CJN.05990809
Pihan-Le Bars F, Bonnet F, Loréal O, Le Loupp AG, Ropert M, Letessier E, Prieur X, Bach K, Deugnier Y, Fromenty B, Cariou B (2016) Indicators of iron status are correlated with adiponectin expression in adipose tissue of patients with morbid obesity. Diabetes Metab 42:105–111. https://doi.org/10.1016/j.diabet.2015.10.007
Stoffel NU, El-Mallah C, Herter-Aeberli I, Bissani N, Wehbe N, Obeid O (2020) Zimmermann MB (2020) The effect of central obesity on inflammation, hepcidin, and iron metabolism in young women. Int J Obes 446(44):1291–1300. https://doi.org/10.1038/s41366-020-0522-x
Vuppalanchi R, Troutt JS, Konrad RJ, Ghabril M, Saxena R, Bell LN, Kowdley KV, Chalasani N (2014) Serum hepcidin levels are associated with obesity but not liver disease. Obesity (Silver Spring) 22:836–841. https://doi.org/10.1002/oby.20403
Tussing-Humphreys LM, Nemeth E, Fantuzzi G, Freels S, Holterman AXL, Galvani C, Ayloo S, Vitello J, Braunschweig C (2010) Decreased serum hepcidin and improved functional iron status 6 months after restrictive bariatric surgery. Obesity (Silver Spring) 18:2010–2016. https://doi.org/10.1038/oby.2009.490
Cepeda-Lopez AC, Allende-Labastida J, Melse-Boonstra A, Osendarp SJM, Herter-Aeberli I, Moretti D, Rodriguez-Lastra R, Gonzalez-Salazar F, Villalpando S, Zimmermann MB (2016) The effects of fat loss after bariatric surgery on inflammation, serum hepcidin, and iron absorption: a prospective 6-mo iron stable isotope study. Am J Clin Nutr 104:1030–1038. https://doi.org/10.3945/ajcn.115.115592
Gesquiere I, Foulon V, Augustijns P, Gils A, Lannoo M, Van der Schueren B, Matthys C (2017) Micronutrient intake, from diet and supplements, and association with status markers in pre- and post-RYGB patients. Clin Nutr 36:1175–1181. https://doi.org/10.1016/j.clnu.2016.08.009
Coimbra S, Ferreira C, Belo L, Rocha-Pereira P, Catarino A, Monteiro L, Catarino C, Santos-Silva A (2018) Impact of weight loss on inflammation and red blood cell biomarkers after laparoscopic gastric banding surgery. J Investig Med 66:304–308. https://doi.org/10.1136/jim-2017-000528
Gesquiere I, Steenackers N, Lannoo M, Foulon V, Mertens A, Gils A, de Hoon J, Augustijns P, Matthys C, Van der Schueren B (2019) Predicting iron absorption from an effervescent iron supplement in obese patients before and after Roux-en-Y gastric bypass: a preliminary study. J Trace Elem Med Biol 52:68–73. https://doi.org/10.1016/j.jtemb.2018.12.002
Marin FA, Verlengia R, Crisp AH, Novais PFS, Rasera-Junior I, de Oliveira MRM (2017) Suplementación con micronutrientes en pacientes con cirugía de bypass gástrico: Estudio prospectivo sobre la inflamación y el metabolismo del hierro en mujeres premenopáusicas. Nutr Hosp 34:369–375. https://doi.org/10.20960/nh.1162
Auguet T, Aragonès G, Berlanga A, Martínez S, Sabench F, Binetti J, Aguilar C, Porras JA, Molina A, Del Castillo D, Richart C (2017) Hepcidin in morbidly obese women with nonalcoholic fatty liver disease. PLoS One 12:e0187065. https://doi.org/10.1371/journal.pone.0187065
Ruz M, Carrasco F, Rojas P, Codoceo J, Inostroza J, Rebolledo A, Basfi-fer K, Csendes A, Papapietro K, Pizarro F, Olivares M, Sian L, Westcott JL, Hambidge KM, Krebs NF (2009) Iron absorption and iron status are reduced after Roux-en-Y gastric bypass. Am J Clin Nutr 90:527–532. https://doi.org/10.3945/ajcn.2009.27699
Ruz M, Carrasco F, Rojas P, Codoceo J, Inostroza J, Basfi-fer K, Valencia A, Csendes A, Papapietro K, Pizarro F, Olivares M, Westcott JL, Hambidge KM, Krebs NF (2012) Heme- and nonheme-iron absorption and iron status 12 mo after sleeve gastrectomy and Roux-en-Y gastric bypass in morbidly obese women. Am J Clin Nutr 96:810–817. https://doi.org/10.3945/ajcn.112.039255
Rhode BM, Shustik C, Christou NV, MacLean LD (1999) Iron absorption and therapy after gastric bypass. Obes Surg 9:17–21. https://doi.org/10.1381/096089299765553656
Gesquiere I, Lannoo M, Augustijns P, Matthys C, Van Der Schueren B, Foulon V (2014) Iron deficiency after Roux-en-Y gastric bypass: insufficient iron absorption from oral iron supplements. Obes Surg 24:56–61. https://doi.org/10.1007/s11695-013-1042-8
Rosa FT, De Oliveira-Penaforte FR, De Arruda LI, Padovan GJ, Ceneviva R, Marchini JS (2011) Altered plasma response to zinc and iron tolerance test after Roux-en-Y gastric bypass. Surg Obes Relat Dis 7:309–314. https://doi.org/10.1016/j.soard.2011.01.041
Hafida S, Mirshahi T, Nikolajczyk BS (2016) The impact of bariatric surgery on inflammation: quenching the fire of obesity? Curr Opin Endocrinol Diabetes Obes 23:373–378. https://doi.org/10.1097/MED.0000000000000277
Baig SJ, Priya P, Mahawar KK, Shah S (2019) Weight regain after bariatric surgery—a multicentre study of 9617 patients from indian bariatric surgery outcome reporting group. Obes Surg 29:1583–1592. https://doi.org/10.1007/s11695-019-03734-6
Al-Jamea LH, Woodman A, Heiba NM, Elshazly SA, Khalaf NB, Fathallah DM, Al-Nashmi ME, Quiambao JV, Deifalla AH (2021) Genetic analysis of TMPRSS6 gene in Saudi female patients with iron deficiency anemia. Hematol Oncol Stem Cell Ther 14:41–50. https://doi.org/10.1016/J.HEMONC.2020.04.007
ten Broeke R, Bravenboer B, Smulders FJF (2013) Iron deficiency before and after bariatric surgery: the need for iron supplementation. Neth J Med 71:412–417
Sazawal S, Black RE, Ramsan M, Chwaya HM, Stoltzfus RJ, Dutta A, Dhingra U, Kabole I, Deb S, Othman MK, Kabole FM (2006) Effects of routine prophylactic supplementation with iron and folic acid on admission to hospital and mortality in preschool children in a high malaria transmission setting: community-based, randomised, placebo-controlled trial. Lancet 367:133–143. https://doi.org/10.1016/S0140-6736(06)67962-2
Nemeth E, Ganz T (2009) The role of hepcidin in iron metabolism. Acta Haematol 122:78–86. https://doi.org/10.1159/000243791
Noguchi-Sasaki M, Sasaki Y, Shimonaka Y, Mori K (2016) Fujimoto-Ouchi K (2016) Treatment with anti-IL-6 receptor antibody prevented increase in serum hepcidin levels and improved anemia in mice inoculated with IL-6–producing lung carcinoma cells. BMC Cancer 161(16):1–11. https://doi.org/10.1186/S12885-016-2305-2
Poli M, Asperti M, Naggi A, Campostrini N, Girelli D, Corbella M, Benzi M, Besson-Fournier C, Coppin H, Maccarinelli F, Finazzi D, Arosio P (2014) Glycol-split nonanticoagulant heparins are inhibitors of hepcidin expression in vitro and in vivo. Blood 123:1564–1573. https://doi.org/10.1182/blood-2013-07-515221
Hepcidin behavior in patients with obesity and bariatric surgery - full text view - ClinicalTrials.gov. https://clinicaltrials.gov/ct2/show/NCT03990948. Accessed 13 Jun 2021
Author information
Authors and Affiliations
Contributions
Author 1 conceived the idea for the topic and initiated the research. Authors 1 and 2 wrote the manuscript. Both authors participated in the discussions on the topic. Both authors have seen the final version and approve of it.
Corresponding author
Ethics declarations
Human and Animal Rights
Not applicable.
Informed Consent
For this type of study formal consent is not required.
Conflict of Interest
The authors declare no competing interests.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Baig, S.J., Priya, P. Hepcidin: a New Serial Biomarker for Iron Deficiency Anemia in Bariatric Surgery. Indian J Surg 85, 1035–1043 (2023). https://doi.org/10.1007/s12262-023-03690-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12262-023-03690-7