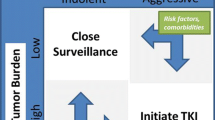
Summary
Established systemic treatment options for advanced thyroid cancer include the multityrosine kinase inhibitors lenvatinib and sorafenib for radioactive iodine refractory differentiated thyroid cancer (DTC) and vandetanib and cabozantinib for medullary thyroid cancer (MTC). Recently, the COSMIC-311 study resulted in approval of cabozantinib for DTC with progression upon lenvatinib and/or sorafenib; thus, for the first time a specific second-line therapy has been defined for these patients. In addition, the therapeutic landscape of thyroid cancer has been expanded by targeted therapies based on molecular tumor profiles. Selective RET inhibitors such as selpercatinib and pralsetinib show high activity in DTC with RET fusions and MTC with RET mutations, respectively. Further targeted treatment options include NTRK inhibitors for thyroid cancers with NTRK fusions and BRAF-targeted therapy for BRAF V600E-mutated (anaplastic) thyroid cancer.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
In recent decades, an increase in thyroid cancer (TC) incidence has been observed, mainly due to rising numbers of localized differentiated thyroid cancers (DTC) detected by routine screening for thyroid nodules [1]. However, while limited stage cases and papillary thyroid cancers (PTC) in particular are diagnosed more frequently, the number of patients with metastatic TC remains stable. According to the recently updated World Health Organization (WHO) classification, thyroid cancer can be subdivided into papillary thyroid cancer (PTC) and follicular thyroid cancer (FTC), supplemented by the more aggressive cohorts termed differentiated high-grade thyroid carcinoma/poorly differentiated thyroid cancer (PDTC) and rare histological entities such as oncocytic carcinomas, which all follow comparable therapeutic algorithms [2]. Formally, the term DTC referring mainly to PTC and FTC has been withdrawn from the classification but will colloquially still be used in the near future—and in this review—as current studies were designed based on prior classifications. In addition, medullary thyroid cancer (MTC), a rare type of neuroendocrine neoplasm, and anaplastic thyroid cancer (ATC), the most aggressive type of TC, still constitute distinct entities subject to individual treatment algorithms. This review focuses on current standards and recent (clinical practice-changing) novelties presented from the medical oncologist’s point of view.
Differentiated thyroid cancer—new second-line options
The 10-year overall survival (OS) for initially localized DTC is reported to be > 90% but it decreases depending on the histological subtype (e.g., 66% 5‑year OS for PDTC) [3]. Surgery with or without TSH suppression and adjuvant radioactive iodine therapy (RAIT) is the only curative approach for DTC [4]. Even in case of relapsed disease or primary metastases, RAIT is the standard of care if all deposits are RAI-positive and response intervals between treatments remain reasonable. While different definitions circulate, the current ESMO guideline defines RAIT-refractory disease based on the following criteria: (1) absence of RAI uptake in all or some relevant lesions and/or (2) radiological RECIST progression 6–12 months following RAIT. To the current knowledge, other systemic treatment options discussed in the following article should be exclusively applied in this cohort of patients.
In the past, the two multityrosine kinase inhibitors (TKIs) lenvatinib and sorafenib have been approved for first-line treatment of progressive, RAIT-refractory DTC. Formally, both compounds have proven a progression-free survival (PFS) benefit in placebo-controlled phase III studies but there is no direct head-to-head comparison and diverging inclusion criteria as well as supplementary data preclude a straight-forward comparability. In summary, lenvatinib (an inhibitor of VEGFR 1–3, FGFR 1–4, PDGFR alpha, KIT, and RET) was tested in the phase III SELECT study (392 patients randomized in a 2:1 ratio) and resulted in a significant prolongation of median PFS from 3.6 months for placebo to 18.3 months for lenvatinib (hazard ratio [HR] 0.21, 99% confidence interval [CI] 0.14–0.31) [5]. Documentation of radiological disease progression within 12 months before study entry was required. The objective response rate (ORR) was high at 65% despite the protocol allowing pretreatment with other TKIs. Formal OS analyses were negative, but a subgroup investigation suggested a benefit for patients aged 65 + [6]. Sorafenib (an inhibitor of VEGFR 1–3, RET, and RAF) was studied in the DECISION trial (417 patients randomized in a 1:1 ratio) and also demonstrated a significant PFS benefit of median 5.8 months for placebo versus 10.8 months for sorafenib (HR 0.59, 95%CI 0.45–0.76) [7]. The ORR was lower at 12%, and radiological progression was required only within 14 months prior to treatment initiation. Toxicities nevertheless are considerable for both compounds with mainly hypertension (41% grade III+), diarrhea (8% grade III+), and fatigue (9% grade III+) for lenvatinib and hand–foot syndrome (20% grade III), diarrhea (6% grade III+), and fatigue (6% grade III+) for sorafenib. To date, both drugs are approved for the upfront treatment of progressive RAIT-refractory DTC. The compound of choice remains at the physician’s discretion, often based on the toxicity profile, comorbidities, and tumor burden.
Until recently there was no defined second-line treatment for DTC patients available, due to the lack of sound scientific data except the “hint” of post-TKI activity of lenvatinib based on a small subgroup of pretreated patients in the SELECT study and the loose (eminence-based) guideline recommendation that sequencing of both first-line drugs appears reasonable [4, 5]. This changed following the publication of the COSMIC-311 trial in 2021 [8], which resulted in approval of cabozantinib for this distinct patient cohort. COSMIC-311 was a randomized phase III study including RAIT-refractory DTC patients with radiological progression following one or two of the approved TKI therapies. In this trial, cabozantinib was applied at a dose of 60 mg daily (i.e., at a lower dose than approved for MTC and importantly in another, not interchangeable formulation). In all, 227 patients were randomized (2:1) to receive cabozantinib or placebo. While the first evaluated endpoint, an objective response rate increase with a prespecified significance level of 0.01, was not met (15% versus 0%, p = 0.028), a planned interim analysis of PFS demonstrated a significant benefit for cabozantinib with an HR of 0.22 (95% CI 0.13–0.36). The median PFS was not reached for cabozantinib versus 1.9 months for placebo, underlining the biological poor prognosis of these patients. The PFS benefit for cabozantinib was independent of prior therapies, i.e., lenvatinib, sorafenib, or both. Toxicities of cabozantinib were in the spectrum of known side effects and included mainly hand–foot syndrome (10% grade III+), hypertension (9% grade III+), and fatigue (8% grade III+), and approximately 55% of patients needed a dose reduction. Following these data, cabozantinib should be considered the second-line therapy of choice in DTC patients who do not have actionable molecular targets, as discussed in the next section of this review.
The optimal time point for performing a molecular profile on DTC tissues is currently a matter of debate, not at least considering the potential of a changing molecular profile during disease as observed in other tumor entities. However, while the proportion of DTC patients eligible for targeted therapies remains low, the growing evidence for applying drugs in the presence of driver mutations urges its assessment already at progression following first-line TKI therapy or even at diagnosis of RAIT refractoriness in our opinion. The probably most cited compounds in this context are selective RET inhibitors, namely selpercatinib and pralsetinib, which are both approved by the USA Food and Drug Administration (FDA), and selpercatinib is also European Medicines Agency (EMA) approved for RET-fusion-positive DTC after progression of TKI therapies [9,10,11]. While the numbers of DTC patients with RET fusions (mainly CCDC6 or NCOA4-RET fusions) in the respective pivotal publications were low with 19 in the LIBRETTO-001 trial for selpercatinib and 11 in the ARROW trial for pralsetinib, the ORR of 80% and the favorable toxicity profile in both studies were judged sufficient for approval by authorities. Several updates on the LIBRETTO-001 and ARROW trial have been published at scientific meetings in the last few months. Furthermore, entrectinib and larotrectinib have both tumor agnostic approval for NTRK-fusion-positive malignancies but again the explicit evidence for TC is scarce given the low incidence, with NTRK fusions being mainly found in pediatric patients [11]. Finally, BRAF V600E mutation is a common finding in advanced PTC, as BRAF mutations per se have been associated with a more aggressive clinically course [12]. Interestingly, while BRAF inhibitors have been successfully implemented for non-small cell lung cancer, the evidence for TC is low and pivotal studies suggested increased toxicities in TC patients as compared to lung cancer [13]. Thus, no clear recommendation for daily practice can be given, but use on an individual basis might be considered.
Medullary thyroid cancer—selective RET inhibitors have arrived in clinical routine
The most important practice-changing development in the field of TC in recent years in our opinion was the introduction of selective RET inhibitors for patients with advanced MTC. While in DTC the number of patients eligible for these agents is small, more than two thirds of patients with MTC harbor an activating RET mutation [14]. This specific driver can be either germline (approximately 25%, MEN2A/B syndrome) or sporadic and detectable in the tumor tissue only (60% of cases), with the point mutation M918T representing the most common alteration. In the USA, both selpercatinib and pralsetinib have unrestricted approval for RET-mutated MTC, while initially in Europe only selpercatinib was approved and exclusively for pretreated patients. However, in September 2022, selpercatinib received EMA approval for the upfront therapy of RET-mutated MTC and RET testing prior to any systemic therapy must be considered standard practice.
Selpercatinib and pralsetinib are both selective RET inhibitors with comparable activity for RET-altered cancers (evidence available mainly in TC and non-small cell lung cancer) including proven intracranial activity [15, 16]. Selpercatinib was tested in the LIBRETTO-001 study, a single arm phase I/II trial assessing the final phase II dose of 160 mg twice daily in patients with RET-altered thyroid cancer [10]. The first ORR reported for 55 TKI-pretreated MTC patients was 69% with a 1-year PFS rate of 82%. In an additional cohort of 88 with no prior therapy, the response rate was 73% with 92% PFS at 1 year. While the median PFS was not reached in the initial publication, the lower 95% confidence intervals were convincing at 19 and 22 months, both for pretreated and treatment-naïve patients, respectively. The toxicity profile of selpercatinib is relatively benign (particularly if compared to previous standard multi-TKIs given the lack of off-RET-target toxicities), with grade III adverse events being mainly hypertension (20%) and elevated liver enzymes (10%), both well manageable and not directly affecting the quality of life of patients. The second compound, pralsetinib, was evaluated in the phase I/II ARROW study, including 15 treatment-naïve and 55 pretreated MTC patients in the initial publication [9]. The ORR was high at 71% and 60%, respectively, and (indirectly) comparable to selpercatinib. The toxicity profile of pralsetinib differs from selpercatinib, as hematological toxicities are also part of the spectrum of side effects (grade III neutropenia 13%, lymphopenia 12%, anemia 10%), which are, however, also well manageable. Pralsetinib is currently only FDA approved for TCs but European approval is awaited.
Nevertheless, while selpercatinib appears to be a legitimate and attractive treatment option for RET-altered advanced MTC, previously available multi-TKIs still remain important: first, one third of patients do not present with an activating RET mutation and are thus not eligible for selpercatinib and second, we need to keep in mind that both approved multi-TKIs vandetanib and cabozantinib have been confirmed in phase III studies, and this level of evidence is not as robust for RET inhibitors yet. Cabozantinib (an inhibitor of MET, VEGFR, and RET) was the first approved drug for advanced MTC following the phase III EXAM study, where 330 patients were randomized in a 2:1 ratio [17]. The median PFS was significantly improved from 4.0 months to 11.2 months (HR 0.28; 95% CI 0.19–0.40), and the ORR was 28% versus 0% for placebo. The tested dose in the study was 140 mg, which was probably retrospectively considered too high given the data deriving from other tumor entities, and resulted in the dose reduction rate of 79%. The full dose is rarely reached in clinical practice. Vandetanib (an inhibitor of RET, VEGFR and EGFR) was tested in the ZETA study including 331 patients randomized in a 2:1 ratio [18]. The median PFS was 30.5 months for vandetanib versus 19.1 months for placebo (HR 0.46, 95% CI 0.31–0.69). Whereas one reason for the numerically longer PFS in both active and placebo group for vandetanib versus cabozantinib could be that radiological progression was not a prerequisite for this study, the high response rate of 45% (versus 13% for placebo) also supports its activity. Toxicities are mainly diarrhea, fatigue, and QTC prolongation, with the latter requiring close monitoring. Again, in line with DTC, no head-to-head comparison of both compounds is available and the substance of choice remains at the discretion of the treating physician. Also, the important question what to do upon progression of a selective RET inhibitor is currently unanswered but switch to multi-TKIs appears to be an option even in the absence of specific data.
Anaplastic thyroid cancer—small steps
ATC remains a diagnosis with a disastrous prognosis complicated by early occurrence of quality-of-life (QOL)-limiting disease-related comorbidities such as dysphagia and dyspnea due to local progression. While the ESMO guidelines offer only limited advice regarding these patients, we recommend the updated guidelines of the American Thyroid Association (ATA) for further study [19]. Concurrent chemoradiotherapy, for instance, with concomitant flat dose docetaxel is still considered standard of care for patients with locally advanced ATCs [20]. In addition, testing for BRAF V600E mutation is reasonable, as the combination of a BRAF and a MEK inhibitor has resulted in promising results for a subgroup of patients, based on a phase II study including 16 patients with ATC, with an astonishing response rate of 69% (11/16, 95%CI 41–89%) reported [21]. This treatment is currently FDA but not EMA approved, Screening for BRAF or other targets (e.g., NTRK, ALK, TMB high, MSI high) is highly recommended in this cohort of high unmet clinical need [4].
An interesting approach only recently shown at ESMO 2022, is the ATLEP study protocol evaluating lenvatinib plus the checkpoint inhibitor pembrolizumab in ATC and PDTC patients [22]. While for the latter the exclusion criteria of lenvatinib pretreatment complicates applicability, the results for ATC appear of interest: in 27 patients with ATC, a partial response was documented in 52% and stable disease in 44%. The median PFS was 9.5 months and the median OS 10.25 months. This regimen is not approved but might serve as proof of concept and in fact represents probably the only “niche” in TC where immunotherapy might be justified for the treatment of TCs except for the minority of patients with MSI-high or TMB-high status and availability of tumor-agnostic immunotherapy following standard treatment.
Conclusion
Until recently, lenvatinib and sorafenib for DTC and vandetanib and cabozantinib for MTC were the only approved drugs for advanced thyroid cancer patients. Selective RET inhibitors are currently the rising stars, but are, however, limited to RET-fusion-positive DTC and RET-mutated MTC. In addition, NTRK and BRAF inhibitors are recommended for certain indications, justifying a broad use of next generation sequencing (NGS) panels for the detection of molecular targets. Despite first positive data for ATC, immunotherapy does not (yet?) play a significant role for TCs and further investigations are needed. An exception might be in MSI-high or TMB-high patients, which can be infrequently detected. Finally, it would be of interest to define more precisely the optimal therapy of rare histologies such as oncocytic carcinomas, which remain clearly underrepresented in all available studies.
References
Davies L, Hoang JK. Thyroid cancer in the USA: current trends and outstanding questions. Lancet Diabetes Endocrinol. 2021;9(1):11–2. https://doi.org/10.1016/s2213-8587(20)30372-7.
Baloch ZW, Asa SL, Barletta JA, et al. Overview of the 2022 WHO Classification of Thyroid Neoplasms. Endocr Pathol. 2022;33(1):27–63. https://doi.org/10.1007/s12022-022-09707-3.
Ibrahimpasic T, Ghossein R, Shah JP, et al. Poorly differentiated carcinoma of the thyroid gland: current status and future prospects. Thyroid. 2019;29(3):311–21. https://doi.org/10.1089/thy.2018.0509.
Filetti S, Durante C, Hartl D, et al. Thyroid cancer: ESMO Clinical Practice Guidelines for diagnosis, treatment and follow-up. Ann Oncol. 2019;30(12):1856–83. https://doi.org/10.1093/annonc/mdz400.
Schlumberger M, Tahara M, Wirth LJ, et al. Lenvatinib versus placebo in radioiodine-refractory thyroid cancer. N Engl J Med. 2015;372(7):621–30. https://doi.org/10.1056/NEJMoa1406470.
Brose MS, Worden FP, Newbold KL, et al. Effect of age on the efficacy and safety of lenvatinib in radioiodine-refractory differentiated thyroid cancer in the phase III SELECT trial. J Clin Oncol. 2017;35(23):2692–9. https://doi.org/10.1200/jco.2016.71.6472.
Brose MS, Nutting CM, Jarzab B, et al. Sorafenib in radioactive iodine-refractory, locally advanced or metastatic differentiated thyroid cancer: a randomised, double-blind, phase 3 trial. Lancet. 2014;384(9940):319–28. https://doi.org/10.1016/s0140-6736(14)60421-9.
Brose MS, Robinson B, Sherman SI, et al. Cabozantinib for radioiodine-refractory differentiated thyroid cancer (COSMIC-311): a randomised, double-blind, placebo-controlled, phase 3 trial. Lancet Oncol. 2021;22(8):1126–38. https://doi.org/10.1016/s1470-2045(21)00332-6.
Subbiah V, Hu MI, Wirth LJ, et al. Pralsetinib for patients with advanced or metastatic RET-altered thyroid cancer (ARROW): a multi-cohort, open-label, registrational, phase 1/2 study. Lancet Diabetes Endocrinol. 2021;9(8):491–501. https://doi.org/10.1016/s2213-8587(21)00120-0.
Wirth LJ, Sherman E, Robinson B, et al. Efficacy of selpercatinib in RET-altered thyroid cancers. N Engl J Med. 2020;383(9):825–35. https://doi.org/10.1056/NEJMoa2005651.
Filetti S, Durante C, Hartl DM, et al. ESMO Clinical Practice Guideline update on the use of systemic therapy in advanced thyroid cancer. Ann Oncol. 2022;33(7):674–84. https://doi.org/10.1016/j.annonc.2022.04.009.
Lee MY, Ku BM, Kim HS, et al. Genetic alterations and their clinical implications in high-recurrence risk papillary thyroid cancer. Cancer Res Treat. 2017;49(4):906–14. https://doi.org/10.4143/crt.2016.424.
Brose MS, Cabanillas ME, Cohen EE, et al. Vemurafenib in patients with BRAF(V600E)-positive metastatic or unresectable papillary thyroid cancer refractory to radioactive iodine: a non-randomised, multicentre, open-label, phase 2 trial. Lancet Oncol. 2016;17(9):1272–82. https://doi.org/10.1016/s1470-2045(16)30166-8.
Kiesewetter B, Riss P, Scheuba C, et al. How I treat medullary thyroid cancer. ESMO Open. 2021;6(3):100183. https://doi.org/10.1016/j.esmoop.2021.100183.
Subbiah V, Gainor JF, Oxnard GR, et al. Intracranial efficacy of selpercatinib in RET fusion-positive non-small cell lung cancers on the LIBRETTO-001 trial. Clin Cancer Res. 2021;27(15):4160–7. https://doi.org/10.1158/1078-0432.Ccr-21-0800.
De Carlo E, Bertoli E, Del Conte A, et al. Brain metastases management in oncogene-addicted non-small cell lung cancer in the targeted therapies era. Int J Mol Sci. 2022; https://doi.org/10.3390/ijms23126477.
Elisei R, Schlumberger MJ, Müller SP, et al. Cabozantinib in progressive medullary thyroid cancer. J Clin Oncol. 2013;31(29):3639–46. https://doi.org/10.1200/jco.2012.48.4659.
Wells SA Jr., Robinson BG, Gagel RF, et al. Vandetanib in patients with locally advanced or metastatic medullary thyroid cancer: a randomized, double-blind phase III trial. J Clin Oncol. 2012;30(2):134–41. https://doi.org/10.1200/jco.2011.35.5040.
Bible KC, Kebebew E, Brierley J, et al. American thyroid association guidelines for management of patients with anaplastic thyroid cancer. Thyroid. 2021;31(3):337–86. https://doi.org/10.1089/thy.2020.0944.
Troch M, Koperek O, Scheuba C, et al. High efficacy of concomitant treatment of undifferentiated (anaplastic) thyroid cancer with radiation and docetaxel. J Clin Endocrinol Metab. 2010;95(9):E54–E7. https://doi.org/10.1210/jc.2009-2827.
Subbiah V, Kreitman RJ, Wainberg ZA, et al. Dabrafenib and trametinib treatment in patients with locally advanced or metastatic BRAF V600-mutant Anaplastic thyroid cancer. J Clin Oncol. 2018;36(1):7–13. https://doi.org/10.1200/jco.2017.73.6785. published Online First: 2017/10/27.
Dierks C, Ruf J, Seufert J, Kreissl M, Klein C, Spitzweg C, Kroiss M, Thomusch O, Lorenz K, Zielke A, Miething C. 1646MO—Phase II ATLEP trial: Final results for lenvatinib/pembrolizumab in metastasized anaplastic and poorly differentiated thyroid carcinoma. ESMO. 2022; https://doi.org/10.1016/annonc/annonc1077.
Funding
Not applicable
Funding
Open access funding provided by Medical University of Vienna.
Author information
Authors and Affiliations
Contributions
Concept: BK, MR. Writing and final approval: BK, LW, MR.
Corresponding author
Ethics declarations
Conflict of interest
L. Wolff declares that she has no competing interests. M. Raderer received honoraria for lectures or advisory board participation from the following for-profit companies (all outside of the submitted work): Celgene/BMS, Ipsen, Novartis, Roche, Eisai, Eli Lilly. B. Kiesewetter received honoraria for lectures or advisory board participation from the following for-profit companies (all outside of the submitted work): AAA, Boehringer Ingelheim, Ipsen, Novartis, MSD, Eli Lilly, Janssen Cilag.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Kiesewetter, B., Wolff, L. & Raderer, M. Essential news for clinical practice—thyroid cancer. memo 16, 47–51 (2023). https://doi.org/10.1007/s12254-022-00862-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12254-022-00862-1