Abstract
Pulmonary arterial hypertension (PAH) is driven by vascular remodelling due to inflammation and cellular stress, including endoplasmic reticulum stress (ER stress). The main ER-stress chaperone, glucose-regulated protein 78 kDa (GRP78), is known to have protective effects in inflammatory diseases through extracellular signalling. The aim of this study is to investigate its significance in PAH. Human pulmonary arterial smooth muscle cells (PASMC) were stimulated with compounds that induce ER stress, after which the secretion of GRP78 into the cell medium was analysed by western blot. We found that when ER stress was induced in PASMC, there was also a time-dependent secretion of GRP78. Next, naïve PASMC were treated with conditioned medium (CM) from the ER-stressed donor PASMC. Incubation with CM from ER-stressed PASMC reduced the viability, oxidative stress, and expression of inflammatory and ER-stress markers in target cells. These effects were abrogated when the donor cells were co-treated with Brefeldin A to inhibit active secretion of GRP78. Direct treatment of PASMC with recombinant GRP78 modulated the expression of key inflammatory markers. Additionally, we measured GRP78 plasma levels in 19 PAH patients (Nice Group I) and correlated the levels to risk stratification according to ESC guidelines. Here, elevated plasma levels of GRP78 were associated with a favourable risk stratification. In conclusion, GRP78 is secreted by PASMC under ER stress and exhibits protective effects from the hallmarks of PAH in vitro. Circulating GRP78 may serve as biomarker for risk adjudication of patients with PAH.
Graphical abstract
Proposed mechanism of ER-stress-induced GRP78 secretion by PASMC. Extracellular GRP78 can be measured as a circulating biomarker and is correlated with favourable clinical characteristics. Conditioned medium from ER-stressed PASMC reduces extensive viability, ROS formation, inflammation, and ER stress in target cells. These effects can be abolished by blocking protein secretion in donor cells by using Brefeldin A.

Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Pulmonary arterial hypertension (PAH) is characterized by progressive vascular remodelling of the pulmonary arteries, thus causing an increase in pulmonary arterial pressure and, consequently, right heart failure (Rabinovitch 2012; Thenappan et al. 2018). Excessive proliferation of pulmonary arterial smooth muscle cells (PASMC) and chronic inflammation strongly contribute to the progression of the disease (Huertas et al. 2020). Due to its devastating consequences, there is unmet need for prognosis parameters and novel therapeutic targets for PAH.
The endoplasmic reticulum (ER) is a central organelle that is necessary for the synthesis, folding, and modification of cellular proteins. This crucial task is carefully controlled by physiological conditions and any perturbations to this homeostasis promote ER stress and, subsequently, an accumulation of misfolded proteins. This, in turn, activates a well-orchestrated cellular process known as the unfolded-protein response (UPR). The ER chaperone glucose-regulated protein 78 kDa (GRP78, also known as BiP: binding immunoglobulin protein) serves as the main regulator of the UPR by sensing misfolded proteins and then inducing differential signalling cascades. The aim of the UPR is to restore the cell to physiological conditions, but prolonged activation of the UPR leads to inflammatory and apoptotic signalling. ER stress and excessive UPR activation are involved in the pathogenesis of a large variety of diseases, including cancer, atherosclerosis, and PAH (Zhao and Ackerman 2006; Hotamisligil 2010; Hetz 2012). Animal studies suggest that supplementation of chemical chaperones could be a feasible option for treating PAH (Dromparis et al. 2013; Koyama et al. 2014).
In recent years, novel functions of GRP78 have been proposed. It was shown in one study that ER stress also triggers extracellular secretion of GRP78 (Delpino and Castelli 2002). Biomarker studies have proven that GRP78 is elevated in patients with obesity and metabolic syndrome, both related to chronic inflammation (Girona et al. 2019). Moreover, administration of GRP78 was found to resolve inflammation in mononuclear cells in vitro (Corrigall et al. 2004; Qin et al. 2017). Additionally, GRP78 was found to exhibit disease-modifying and immunomodulatory effects in murine models of rheumatoid arthritis (RA) (Brownlie et al. 2006; Zaiss et al. 2019). These results suggest a pivotal and protective role for extracellular GRP78 on cellular inflammation.
Thus far, data on the secretion and extracellular effects of GRP78 in PAH are lacking. The aim of this study was, first, to analyse the role of GRP78 in in vitro models of PAH and, secondly, to analyse its potential as a biomarker in a cohort of patients suffering from PAH.
Methods
Cell culture
Primary human pulmonary artery smooth muscle cells (PASMC) were purchased (PromoCell, Germany; Cat# C-12521) and cultured in their respective cell medium (PromoCell, Cat# C-22062) under standard conditions (37°C, 5% CO2, 100% relative humidity). Once the cells reached 70–90% confluence, the medium was removed, and the cells were washed once before passaging by using trypsinisation. The cells used for experiments were from passages 6–8.
Additionally, PASMC were cultured under hypoxic conditions in an incubator (37°C, 1% O2, 5% CO2, 100% relative humidity) for 24 h. Hypoxia-challenged cells were otherwise treated as described above.
ER-stress induction and conditioned medium
PASMC (“donor cells”) were seeded into 6-well plates and stimulated with vehicle (DMSO), tunicamycin (5 μg/ml) or thapsigargin (0.1 μM) for 4, 6, 12, 24, or 48 h in serum-containing medium. Additionally, PASMC were stimulated for 48 h with either tunicamycin or thapsigargin combined with Brefeldin A (BFA), an inhibitor of Golgi-ER protein trafficking. The cell medium was aspirated and centrifuged at 800×g for 5 min to remove cellular debris. The supernatant was frozen at -80°C until it was used as conditioned medium. For the cell-culture experiments, new PASMC (“target cells”) were treated with a combination of 60% fresh, serum-containing medium, and 40% of the respective pre-warmed conditioned medium (CM). The optimal ratio of these media was previously determined by viability experiments, which found that the cell viability was unaltered when using the 60:40 ratio. The effects of CM from cells under ER stress on different cell types were previously investigated (Mahadevan et al. 2011; Blackwood et al. 2020).
In some experiments, PASMC were incubated for 48 h with different concentrations of recombinant GRP78 (Prospec Bio, Cat# HSP-037) that was diluted in DMSO. Thereafter, the readout experiments were conducted as described below.
Protein isolation and western blot
For the analysis of extracellular proteins, the cell medium was collected and incubated for 10 min at 4°C with one volume of 100% trichloroacetic acid per four volumes of protein sample, then centrifuged at 14,000× g for 5 min. The supernatant was removed and the remaining cell pellet was washed twice with 200 μl cold acetone followed by centrifugation at 14,000× g for 5 min. The pellet was then dried for 5 min at 95°C before adding 100μl H2O and 30μl 2x Laemmli buffer (4% SDS, 10% ß-mercaptoethanol, 20% glycerol, 0.004% bromophenol blue, 0.125 M Tris HCl pH 6.8) and the sample loaded onto an SDS-PAGE gel (Bio-Rad, CT# 456-1084).
Intracellular proteins from cells in the same well were isolated by lysing with RIPA Buffer (Sigma-Aldrich, Cat# R0278) containing 1:25 Protease Inhibitor Cocktail (Roche, Cat# 4693132001). The lysates were centrifuged at 13,000×g for 10 min at 4°C. The supernatant was removed and the protein concentration was measured by using a Qubit Protein Assay (Thermo Fisher Scientific, Cat# Q33211) in a Qubit-4 Fluorometer (Thermo Fisher Scientific). Twenty micrograms of the resulting protein were loaded onto an SDS-PAGE gel.
Electrophoresis was performed by using a Mini Protean system (Bio-Rad), and the proteins were transferred to a nitrocellulose membrane (Carl Roth, HP40.1) for western blotting. The membrane was blocked with 5% BSA for 1 h at room temperature before it was incubated overnight with primary antibodies at 4°C.
The next day, the membranes were washed three times with 0.1% tris-buffered saline containing 0.1% Tween 20. Then, secondary antibodies that were conjugated with horseradish peroxidase (HRP) were added for 1 h at room temperature. The membrane was then washed again three times before detection was performed with an ECL Western Blot Detection Reagent (Sigma-Aldrich, Cat# RPN2232) on a ChemoCam HR16-3200 Imager (Intas).
The following antibodies were used: GRP78 (dilution 1:1000, Cell Signaling Technology, Cat# 3177S), ß-actin (dilution 1:2000, Sigma-Aldrich, Cat# A1978), anti-mouse-IgG secondary antibody (dilution 1:10,000, Sigma-Aldrich, Cat# A9044), and anti-rabbit-IgG secondary antibody (dilution 1:10,000, Sigma-Aldrich Cat# A0545).
Viability assay
alamarBlueTM HS Cell Viability Reagent (Thermo Fisher Scientific, USA; Cat# A50100) was added to cells treated by CM or recombinant GRP78. The mixtures of viability reagent and cells were incubated for 4 h under standard culture conditions, as outlined above, and protected from light. Then, the absorbance was measured by using an Infinite M200 Microplate Reader (Tecan, Switzerland). Alamarblue is a resazurin-based solution that is reduced to the fluorescent form resorufin by cells that are undergoing respiration and thus are viable.
Reactive oxygen species (ROS) measurement
The formation of ROS was measured by using a 2′,7′-dichlorofluorescein diacetate (DCFDA, Sigma-Aldrich, USA; Cat# D6883) assay. For this assay, cells were seeded one day prior to the experiment unto a dark-bottomed 96-well microplate, protected from light, and were treated with CM or recombinant GRP78. After 24 h, the cells were stimulated with 75 μM hydrogen peroxide (H2O2) for 1 h. Then, DCFDA was added at a final concentration of 50 μM for 45 min. Finally, the supernatant containing DCFDA was removed and the cells were washed before the addition of 100μl PBS. Fluorescence was detected immediately using a microplate reader with a maximum excitation and emission of 492 nm and 527 nm, respectively.
Quantitative real-time polymerase chain reaction
Total RNA was isolated from the cells by using TRIzolTM (Thermo Fisher Scientific, Cat# 15596018) and chloroform phase separation. The amount of RNA collected was quantified using a Nanodrop spectrophotometer (Nanodrop Technologies, USA). Then, 0.5–2 μg of RNA were reverse transcribed by using an Omniscript RT Kit (Qiagen, Cat# 205113). Finally, quantitative real-time PCR was performed on a 7500 HT Real-Time PCR machine (Applied Biosystems, USA) by using the TaqMan gene expression assays (Thermo Fisher Scientific) and Gene Expression Master Mix (Thermo Fisher Scientific, Cat# 4369542). CT values up to 40 were used for analysis and all samples were run in triplicate. The values were analysed using the ΔΔCT method, by normalising to 18S ribosomal RNA.
The following TaqMan Assays were used: Interleukin-6 (IL-6, Hs00174131_m1), nuclear factor “kappa-light-chain-enhancer” of activated B-cells (NF-κB, Hs00765730_m1), glucose-regulated protein 78 (GRP78, Hs00607129_gH), C/EBP homologous protein (CHOP, Hs00358796_g1), hypoxia inducible factor α (HIFα, Hs00153153_m1), and 18S ribosomal RNA (18S, Hs99999901_s1).
Subjects
For the prospective study, consecutive PAH patients routinely presenting to our tertiary care university hospital outpatient clinic were enrolled. In all patients, PAH was previously confirmed by using right-heart catheterization, with a mean pulmonary artery pressure (mPAP) ≥ 25 mmHg. Patients were categorized according to the Nice classification (Simonneau et al. 2019) and only patients with Nice Group I were enrolled.
Risk stratification was performed according to Boucly et al., who proposed to use a number of low-risk criteria to facilitate an accurate prediction of prognosis in PAH (Boucly et al. 2017; Hoeper et al. 2018). Therefore, we assessed six different criteria: 6-min walk distance (6MWD), WHO functional class (FC), N-terminal pro-brain natriuretic peptide (NT-proBNP) level, right atrial pressure (RAP), cardiac index (CI), and central venous oxygen saturation (SvO2). Using the cut-off values proposed in the current ESC guidelines (Galiè et al. 2016), we defined the low-risk criteria as 6MWD > 440m, WHO FC I or II, NT-proBNP < 300 ng/L, RAP < 8 mmHg, CI ≥ 2.5 L/(min*m2), and SvO2 > 65%, with the first three criteria being assessed at baseline and also at follow-up. RAP, CI, and SvO2 were only reassessed at follow-up if there was a clinical indication for repeated right-heart catheterization.
The study complied with the principles of the declaration of Helsinki and was approved by the local ethics committee. Written informed consent was obtained from all patients.
Blood sampling and biomarker measurement
Blood was drawn from a peripheral vein of PAH patients routinely presenting to our outpatient clinic and collected directly into EDTA tubes. The samples were kept on ice and centrifuged (1500×g, 15 min at 4°C) for a maximum of 30 min. Thereafter, plasma was transferred into coded aliquots and frozen at −80°C until the time of analysis.
The plasma concentrations of GRP78 (Enzo Life Sciences, Inc, Farmingdale, New York, USA) and HSP27 (R&D Systems, Bio-Techne, Minneapolis, USA) were analysed by using commercially available enzyme-linked immunosorbent assay (ELISA) kits. 4-Parameters Logistic Regression (Graphpad Prism 9.0.0) was used to plot the concentrations.
Statistical analysis
Continuous variables are presented as means ± the standard deviation if normally distributed and as the median and interquartile range if not normally distributed, as assessed with the Kolmogorov–Smirnov test. Depending on the distribution, continuous variables were tested using either a Student’s t test or Mann–Whitney U test. Simple linear models (ANOVA) or the Kruskal–Wallis-test were used for more than two groups. Categorical variables are given as absolute numbers and percentages. Differences in categorical variables were assessed by the use of Fisher’s exact test. For correlation analyses, bivariate correlation was assessed by using Pearson’s r.
Statistical analyses were performed with SPSS version 25 (IBM Corporation, Somer, NY) and GraphPad Prism (9.0.0). Statistical significance was considered as a 2-tailed probability value ≤0.05. All authors vouch for the data and analyses.
Results
GRP78 is secreted by PASMC under ER stress
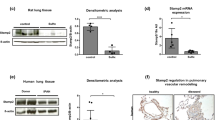
PASCM were treated with the inducers of ER stress tunicamycin (5 μg/ml) or thapsigargin (0.1 μM) for 2, 4, 6, 12, 24, or 48 h (Abdullahi et al. 2017). Treatment with tunicamycin and thapsigargin promoted intracellular GRP78 expression in a time-dependent manner (Figure 1A,B). Interestingly, also when we determined the extracellular concentration of GRP78 in the cell medium, there was a time-dependent increase in its expression (Figure 1C,D). Significant expression of GRP78 could be detected in the medium after 48 h of either tunicamycin or thapsigargin treatment (Figure 1C,D). The housekeeping (and strictly intracellular) protein ß-actin was not detected in the extracellular medium, indicating that the GRP78 detected in the medium is not a result of apoptotic cell debris. Finally, co-treatment with Brefeldin A (BFA), an inhibitor of ER–Golgi protein trafficking, abolished GRP78 expression in the cell medium of tunicamycin (Figure 1C), but not thapsigargin (Figure 1D), treated cells. These results suggest that there is active ER–Golgi-dependent secretion of GRP78 by tunicamycin treated PASMC.
GRP78 is secreted by PASMC. A Representative western blot of PASMC treated with DMSO, tunicamycin (2, 4, 6, 12, 24, 48 h, 5 μg/ml) or tunicamycin (48 h, 5 μg/ml) and BFA (5 μg/ml). Left panel: intracellular proteins. C Extracellular proteins. Incubated with antibodies against GRP78 or ß-actin (housekeeping intracellular protein). B Representative western blot of PASMC treated with DMSO, thapsigargin (2, 4, 6, 12, 24, 48 h, 0.1 μM) or thapsigargin (48 h, 0.1 μM) and BFA (5 μg/ml). Left panel: intracellular proteins. D Extracellular proteins. Incubated with antibodies against GRP78 or ß-actin (housekeeping intracelluar protein). n = 3
GRP78 containing CM reduces the viability of PASMC under the stimulation of PDGF-BB
To investigate the effect of secreted GRP78, we established a model utilising conditioned medium (CM) collected from ER-stressed donor PASMC. The target PASMC were incubated with CM from donor PASMC treated with DMSO (control), tunicamycin, tunicamycin + BFA, thapsigargin, or thapsigargin + BFA for 48 h. Utilizing this model, we analysed the effects of a presence or absence of secreted proteins (including GRP78) from ER-stressed donor cells on target cells.
It is known that excessive proliferation and viability of PASMC are major contributor to PAH. We found no difference in the basal viability of the target cells when treated with the above-mentioned CM (Fig. 2A). In the next step, PAH conditions were simulated by incubating cells with 30 ng/ml platelet-derived growth factor BB (PDGF) for 48 h. In the final 24 h of the PDGF treatment, the respective CM was added. PASMC treated with tunicamycin CM had significantly lower viability than PASMC treated with CM of tunicamycin + BFA donor cells (CM Cntrl: 1.0-fold vs. CM Tun 1.10 vs. CM Tun + BFA 1.262, ANOVA p=0.0008, Fig. 2B). These effects were mirrored when the cells were treated with CM from thapsigargin/thapsigargin + BFA-treated donor cells (CM Cntrl: 1.0-fold vs. CM Tpg 1.03 vs. CM Tpg + BFA 1.21, ANOVA p=0.0001, Fig. 2C).
ER-stress conditioned medium modulates viability. A Viability of PASMC measured by alamarblue® assay, after treatment with conditioned medium (CM) for 24 h. n = 10. B Viability of PASMC measured by alamarblue® after treatment with PDGF (30 ng/ml) for 48 h, followed by treatment with CM (control CM, tunicamycin CM: CM Tun, or tunicamycin + Brefeldin A CM: CM Tun + BFA) for 24 h. n = 7. C Viability of PASMC measured by alamarblue®, after treatment with PDGF (30 ng/ml) for 48 h, followed by treatment with CM (control CM, thapsigargin CM: CM Tpg, or thapsigargin + BFA CM: CM Tpg + BFA) for 24 h. n = 8. Simple linear models (ANOVA). *p < 0.05, **p < 0.01, ***p < 0.001, ****p <0.0001
In another approach, target PASMC were treated with the respective CM under hypoxic conditions (1% O2, 5% CO2 for 24 h) to mimic the conditions of PAH. We could not detect a difference in viability under these conditions (Supplementary Fig. S1A, B).
ER-stress conditioned medium modulates the formation of reactive oxygen species (ROS)
ROS formation has repeatedly been demonstrated to be involved in the development of PAH (Sommer et al. 2016). Hence, we measured ROS formation, by using DCFDA assays, in PASMC that were treated with the CM as described above. Under basal conditions (Figure 3A) and when mimicking oxidative stress by treating the target with H2O2 (Figure 3B,C), PASMC treated with tunicamycin CM, but not tunicamycin + BFA CM, had significantly lower ROS formation than the control CM (Figure 3A: CM Cntrl: 1.0-fold vs. CM Tun 0.61 vs. CM Tun + BFA 0.78, ANOVA p=0.029; Fig. 3B: CM Cntrl: 1.0-fold vs. CM Tun 0.71 vs. CM Tun + BFA 0.76, ANOVA p=0.039). There was no difference in ROS formation between thapsigargin and thapsigargin + BFA CM under both conditions (Fig. 3A,C).
Reactive Oxygen Species (ROS) formation is altered by conditioned medium from cells under ER stress. A ROS formation in PASMC, measured by DCFDA assay, after treatment with conditioned medium (CM) for 24 h. n = 16. B, C ROS formation in PASMC, measured by DCFDA assay, after treatment with CM for 24 h and simultaneous treatment with 75 μM H2O2 for 1 h. n = 16. Simple linear models (ANOVA). *p < 0.05, **p < 0.01, ***p < 0.001, ****p <0.0001
GRP78 containing CM alters inflammatory gene expression in target cells
Next, we sought to elucidate the effects of CM from cells under ER stress on mRNA expression in target cells. CM from donor cells that were additionally treated with BFA significantly increased GRP78 expression in the target cells compared to tunicamycin/thapsigargin alone (Fig. 4A: CM Cntrl: 1.0-fold vs. CM Tun 6.5-fold vs. CM Tun + BFA 26.0-fold; Fig. 4B: CM Cntrl: 1.0-fold vs. CM Tpg 17.1-fold vs. CM Tun + BFA 27.7-fold). There was no significant difference in the expression of CHOP mRNA, another marker of ER stress (Supplementary Fig. S2A, B).
Conditioned medium from cells under ER stress regulates gene expression in target cells. A, B mRNA expression levels of GRP78 in target PASMC, treated for 24 h with conditioned medium (CM) from tunicamycin- (A) or thapsigargin- (B) stimulated donor PASMC. n = 3–5. C, D mRNA expression levels of NF-κB in target PASMC, treated for 24 h with conditioned medium (CM) from tunicamycin- (C) or thapsigargin- (D) stimulated donor PASMC. n = 3-5. n = 4–5. E, F mRNA expression levels of IL-6 in target PASMC, treated for 24 h with conditioned medium (CM) from tunicamycin- (E) or thapsigargin- (F) stimulated donor PASMC. n = 3-5. n = 5. mRNA expression was measured by qPCR and quantified by using the 2-ddCT method. Simple linear models (ANOVA). *p < 0.05, **p < 0.01, ***p < 0.001, ****p <0.0001
NF-κB is a transcription factor involved in moderating cellular inflammation. Activation of NF-κB is known to occur during the development of PAH (Raychaudhuri et al. 1999). NF-κB expression was unaltered between treatments with CM from control cells or tunicamycin treated cells, but administration of CM from tunicamycin + BFA-treated PASMC increased NF-κB expression in target cells (Fig. 4C: CM Cntrl: 1.0-fold vs. CM Tun 0.49-fold vs. CM Tun + BFA 4.55-fold, ANOVA p=0.016).
Another inflammatory marker involved in PAH pathogenesis is interleukin-6 (IL-6). Interestingly, CM from tunicamycin treated PASMC increased IL-6 mRNA expression compared to control CM or tunicamycin + BFA CM (Fig. 4E: CM Cntrl: 1.0-fold vs. CM Tun 3.5-fold vs. CM Tun + BFA 1.2-fold, ANOVA p=0.005). There was no significant difference detectable regarding NF-κB and IL-6 expression between thapsigargin CM and thapsigargin + BFA CM treated cells (Figure S2C, S2D).
Recombinant GRP78 mimics the effect of CM on gene expression
Next, we explored if direct treatment with recombinant GRP78 can exhibit similar effects on PASMC as treatment with CM. Therefore, PASMC were incubated with recombinant GRP78 (48 h, 10 ng/ml, 100 ng/ml, or 1000 ng/ml). There was no difference in viability under basal conditions (Figure 5A: Cntrl: 1.0-fold vs. 10 ng/ml GRP78: 1.06-fold vs. 100 ng/ml GRP78: 1.04-fold vs. 1000 ng/ml GRP78: 1.02-fold, ANOVA p=0.36) and also no difference in viability after PDGF stimulation or hypoxia treatment (Supplementary Fig. S3A and B). By analysing gene expression, we found that adding recombinant GRP78 decreased the expression of GRP78 mRNA in target cells in a dose-dependent manner (Figure 5B: Cntrl: 1.0-fold vs. 10 ng/ml GRP78: 1.52-fold vs. 100 ng/ml GRP78: 1.25-fold vs. 1000 ng/ml GRP78: 0.39-fold, ANOVA p=0.048). There was also a similar alteration in NF-κB and HIFα expression (Figure 5C,D). Intriguingly, the lower concentrations of recombinant GRP78 caused an increase in expression of these markers and higher concentrations of GRP78 reduced expression, which shows a trend toward the dose-dependancy of this effect.
Effects of recombinant GRP78 on viability and mRNA expression. A Viability of PASMC measured by alamarblue® assay after treatment with recombinant GRP78 (10 ng/ml, 100 ng/ml, 1000 ng/ml for 48 h). n = 9. B, C, D mRNA expression of GRP78 (A), NF-κB (B), and HIFα (C) in target PASMC, treated with recombinant GRP78 (10 ng/ml, 100 ng/ml, 1000 ng/ml for 48 h). n = 3. mRNA expression was measured by qPCR and quantified by using the 2-ddCT method. Simple linear models (ANOVA). *p < 0.05, **p < 0.01, ***p < 0.001, ****p <0.0001
Circulating GRP78 in PAH patients
Nineteen consecutive patients with PAH corresponding to Nice group I were included into the study. Baseline characteristics of the PAH patients are presented in Table 1 (female 52%, mean age of 62.5 ± 17 years). The majority of patients were classified as WHO FC II (42.1%) or III to IV (47.3%) and were predominantly receiving PAH combination therapy (68.4%). The mean pulmonary artery pressure (mPAP) was 37.29 ± 13.06 mmHg, with a pulmonary arterial wedge pressure (PAWP) of 11.2 ± 3.5 mmHg and a pulmonary vascular resistance (PVR) of 6.1 ± 3.1 Wood units. At the time of enrollment into our study, 68.4% (13/19) of patients had more than two low-risk risk factors (“low-risk” patients) and 31.6% (6/19) presented with zero to two low-risk factors (“high-risk” patients). Low-risk patients had lower PVR (4.8 ± 2.7 vs. 8.8 ± 1.6, p = 0.001) and were more likely to have COPD or asthma as a comorbidity.
Interestingly, low-risk patients had significantly higher GRP78 plasma levels (1346 ± 299 ng/ml vs. 796 ± 203 ng/ml, p = 0.0008, Fig. 6A). However, there was no association between low-risk criteria and plasma levels of heat shock protein 27 (HSP27), another prominent chaperone with well-known extracellular properties in cardiovascular disease (Supplementary Fig. 4A). There was no difference in GRP78 levels when comparing patients with PAH monotherapy and combination therapy (Monotherapy: 1199 ± 346 ng/ml, combination therapy: 1160 ± 399.8 ng/ml, p = 0.833).
GRP78 as a biomarker in PAH patients. A GRP78 concentration in PAH patients of Nice Group I with a low number of low-risk criteria (0–2, “high-risk” patients) and a higher number of low-risk criteria (3–6, “low-risk” patients). n = 19. Student’s t test. *p < 0.05, **p < 0.01, ***p < 0.001, ****p <0.0001
We furthermore measured GRP78 plasma levels in ten healthy volunteers with a mean age of 21.9 ± 2.3 years, 40% were male. GRP78 plasma concentration was below the assay detection limit of 25 ng/ml in all volunteers. Next, we mined available biostatistic data of plasma proteomics in humans (Farrah et al. 2011). Most of the used data sets were gathered from healthy individuals. The normal GRP78 plasma concentration was estimated to be 100 ng/ml.
Discussion
Because of its devastating effects on patients, finding novel therapeutic targets for PAH is highly important. Here, we have demonstrated that PASMC actively secrete GRP78 in response to the induction of ER stress. GRP78-containing conditioned medium from ER-stressed PASMC dampens viability, oxidative stress, NF-κB activation, and ER stress in target cells. Intercellular transmission of ER stress signals, e.g. by connexins, has been well-characterized and is mostly attributed deleterious properties (Tirosh et al. 2021). However, thus far, there is only scarce evidence examining any potential protective effects of the intercellular responses to ER stress. Our patient-derived data shows that circulating levels of the ER-stress protein GRP78 strongly correlate with favourable risk stratification in PAH. Our study introduces a novel, anti-inflammatory feedback mechanism that occurs during pulmonary vascular ER stress.
We found that incubating cells with the well-established ER-stress inducers tunicamycin and thapsigargin promoted the secretion of GRP78. Utilising a similar approach, Blackwood et al. found that thapsigargin, but not tunicamycin, promoted GRP78 secretion in cardiomyocytes (Blackwood et al. 2020). In our study, both ER-stress inducers promoted extracellular GRP78 secretion. Interestingly, however, we found that treatment with BFA inhibited tunicamycin-, but not thapsigargin-induced secretion. These results indicate that there are cell-type specific effects on ER-stress-induced protein secretion. In the current study, administration of both tunicamycin and thapsigargin in donor cells modulated the viability and GRP78 expression of target cells, while the effects on ROS formation and expression of inflammatory markers were only observed when using tunicamycin CM. Tunicamycin induces ER stress by directly inhibiting N-linked glycosylation of proteins while thapsigargin depletes the Ca2+ levels in the ER by inhibiting the endoplasmic reticulum Ca2+ ATPase. Thus, it appears that the mechanism of ER stress induction in donor cells influences the effects exhibited in target cells. These findings might be explained by specific secretion of additional, yet unknown, proteins. Additionally, thapsigargin-induced secretion of GRP78 is not altered by inhibition of the canonical ER–Golgi protein trafficking, suggesting the existence of non-canonical protein secretion pathways. For example, secretion by exosomes is another well-known way of protein secretion. Exosomes can be secreted by donor cells by membrane budding and contain proteins, lipids, and nucleic acids that deliver signals to recipient cells (Pegtel and Gould 2019). Secretion of GRP78-containing extracellular vesicles was previously described to play a role in vascular biology (Furmanik et al. 2021).
In addition, Blackwood et al. found GRP78 secretion to exert paracrine, cytoprotective effects on cardiomyocytes (Blackwood et al. 2020). Since myocardial dysfunction of the right ventricle is an important issue in clinically advanced PAH (Olsson et al. 2018), these proposed cardioprotective properties are of great clinical significance. Our data supports the idea that GRP78 secretion serves as a protective feedback mechanism, induced by cardiovascular ER stress.
Under basal conditions, we found no alteration of cell viability in PASMC treated with CM containing or not containing GRP78. But when the cells were stimulated with the PAH-promoting growth factor PDGF (Schermuly et al. 2005), an increase in viability was more pronounced in PASMC treated with CM where GRP78 secretion was inhibited. Direct treatment with recombinant GRP78 did not alter the viability under basal or PAH-promoting conditions. Thus, GRP78 alone does not limit the viability of cells and only limits PASMC viability in combination with disease-promoting growth factors. These findings are important to be able to exclude toxicity to cells, such as coronary smooth muscle cells. Moreover, additional components of the conditioned medium are required to exert anti-proliferative effects on target cells. Intracellular GRP78 exists in a multi-protein complex and might also be secreted in a similar complex (Meunier et al. 2002). Hence, modulation of the secretion of GRP78 rather than direct GRP78 treatment might be a more feasible therapeutic option. In a previously published study using hypoxia-challenged rats, treatment with the peptide intermedin increased cellular GRP78 levels and attenuated PASMC proliferation and PAH development (Mao et al. 2014). This study further supports our findings.
When analysing gene expression, the absence of GRP78 in the CM promoted mRNA expression of GRP78 in target cells. Hence, the protective properties of extracellular GRP78 might be mediated by a reduction of the intracellular activation of UPR in target cells. However, there were no alterations in CHOP expression, hinting at a modulation of distinct UPR pathways. Vascular inflammation is a well-established feature of PAH and NF-κB was frequently ascribed a prominent role in initiating pulmonary vascular inflammation (Fiordelisi et al. 2019; Huertas et al. 2020). Intriguingly, we found that an absence of GRP78 in the CM promotes NF-κB expression in target cells. When analysing IL-6 expression, we found that the presence of GRP78 in CM increased IL-6 mRNA. There are conflicting reports regarding the role of IL-6 in PAH biology. However, a recent multicentre analysis found circulating IL-6 to be secreted by PASMC and to be associated with positive clinical outcomes (Simpson et al. 2020).
To the best of our knowledge, this is the first study measuring circulating ER-stress proteins in patients with PAH. We found that elevated GRP78 levels are associated with favourable risk stratification. These findings are highly relevant because a dramatic, rapid deterioration is frequent in patients with PAH (Galiè et al. 2016). For risk stratification, we used the number of low-risk criteria present to stratify patients. This approach was found to be more accurate than an approach using the average risk category for prognosis prediction in PAH patients (Hoeper et al. 2018).
Contrarily, there was no association between HSP27, another chaperone with well-established extracellular signalling properties in CVD (Seibert et al. 2013), and risk stratification. These results emphasize a specific, presumably protective, role for GRP78 in PAH. Previous studies have reported alterations of plasma GRP78 levels in a variety of diseases (Girona et al. 2019; Doerflinger et al. 2020). In a recent study from our group, we found GRP78 to have beneficial prognostic implications in patients undergoing transcatheter aortic valve replacement (Aksoy et al. 2021). However, there is so far only scarce knowledge regarding the biological significance of elevated plasma levels.
Limitations of our study are the limited number of patient samples and the lack of animal data, e.g. of PAH model animals. Additionally, in vitro PAH conditions do not a hundred percent resemble in vivo the vascular environment in PAH in humans. Furthermore, we only analysed PASMC and did not additionally examine endothelial cells. Moreover, in this current study we mainly focussed on the effects of GRP78-containing CM and did not perform in-depth analysis of the mechanisms of GRP78 secretion. While we found that Tunicamycin-induced secretion is most likely mediated by canonical ER-Golgi transport, the mechanism of Thapsigargin-induced secretion remains unknown. Future studies have to focus on additional ways of secretion including exosomes and usage of specific GRP78-antibodies.
Our results are in line with other studies proposing an anti-inflammatory effect for extracellular GRP78 (Shields et al. 2011; Zaiss et al. 2019). In human trials, treatment with GRP78 was well-tolerated and did not induce toxicity in rheumatoid arthritis patients (Kirkham et al. 2016). Because of its presumably protective effects on both cardiomyocytes and PASMC, GRP78 administration may be a feasible therapeutic option in patients with PAH. An additional therapeutic approach might be direct modulation of GRP78 secretion. Future studies are required to further characterize the mechanisms of secretion and action of GRP78. Moreover, larger clinical cohorts are needed to elucidate the significance of circulating GRP78 as a biomarker for PAH.
Availability of data and material
The data that support the findings of this study are available from the corresponding author upon reasonable request.
References
Abdullahi A, Stanojcic M, Parousis A et al (2017) Modeling acute ER stress in vivo and in vitro. Shock 47:506–513. https://doi.org/10.1097/SHK.0000000000000759
Aksoy A, Al-Kassou B, Al Zaidi M et al (2021) Circulating chaperones in patients with aortic valve stenosis undergoing TAVR: impact of concomitant chronic kidney disease. Transl Res 233:117–126. https://doi.org/10.1016/j.trsl.2021.03.003
Blackwood EA, Thuerauf DJ, Stastna M et al (2020) Proteomic analysis of the cardiac myocyte secretome reveals extracellular protective functions for the ER stress response. J Mol Cell Cardiol 143:132–144. https://doi.org/10.1016/j.yjmcc.2020.04.012
Boucly A, Weatherald J, Savale L et al (2017) Risk assessment, prognosis and guideline implementation in pulmonary arterial hypertension. Eur Respir J 50:1–10. https://doi.org/10.1183/13993003.00889-2017
Brownlie RJ, Myers LK, Wooley PH et al (2006) Treatment of murine collagen-induced arthritis by the stress protein BiP via interleukin-4-producing regulatory T cells: a novel function for an ancient protein. Arthritis Rheum 54:854–863. https://doi.org/10.1002/art.21654
Corrigall VM, Bodman-Smith MD, Brunst M et al (2004) Inhibition of antigen-presenting cell function and stimulation of human peripheral blood mononuclear cells to express an antiinflammatory cytokine profile by the stress protein BiP: relevance to the treatment of inflammatory arthritis. Arthritis Rheum 50:1164–1171. https://doi.org/10.1002/art.20134
Delpino A, Castelli M (2002) The 78 kDa glucose-regulated protein (GRP78/BIP) is expressed on the cell membrane, is released into cell culture medium and is also present in human peripheral circulation. Biosci Rep 22:407–420. https://doi.org/10.1023/A:1020966008615
Doerflinger M, Reljic B, Menassa J et al (2020) Circulating BiP/Grp78 is a novel prognostic marker for sepsis-mediated immune cell death. FEBS J. https://doi.org/10.1111/febs.15552
Dromparis P, Paulin R, Stenson TH et al (2013) Attenuating endoplasmic reticulum stress as a novel therapeutic strategy in pulmonary hypertension. Circulation 127:115–125. https://doi.org/10.1161/CIRCULATIONAHA.112.133413
Farrah T, Deutsch EW, Omenn GS et al (2011) A High-Confidence Human Plasma Proteome Reference Set with Estimated Concentrations in PeptideAtlas. Molecular & Cellular Proteomics 10(9):M110.006353. https://doi.org/10.1074/mcp.M110.006353
Fiordelisi A, Iaccarino G, Morisco C et al (2019) NfkappaB is a key player in the crosstalk between inflammation and cardiovascular diseases. Int J Mol Sci 20:1599. https://doi.org/10.3390/ijms20071599
Furmanik M, van Gorp R, Whitehead M et al (2021) Endoplasmic reticulum stress mediates vascular smooth muscle cell calcification via increased release of Grp78 (glucose-regulated protein, 78 kDa)-loaded extracellular vesicles. Arterioscler Thromb Vasc Biol 41:898–914. https://doi.org/10.1161/atvbaha.120.315506
Galiè N, Humbert M, Vachiery JL et al (2016) 2015 ESC/ERS Guidelines for the diagnosis and treatment of pulmonary hypertension. Eur Heart J 37:67–119. https://doi.org/10.1093/eurheartj/ehv317
Girona J, Rodríguez-Borjabad C, Ibarretxe D et al (2019) The circulating GRP78/BiP is a marker of metabolic diseases and atherosclerosis: bringing endoplasmic reticulum stress into the clinical scenario. J Clin Med 8:1793. https://doi.org/10.3390/jcm8111793
Hetz C (2012) The unfolded protein response: controlling cell fate decisions under ER stress and beyond. Nat Rev Mol Cell Biol 13:89–102. https://doi.org/10.1038/nrm3270
Hoeper MM, Pittrow D, Opitz C et al (2018) Risk assessment in pulmonary arterial hypertension. Eur Respir J. https://doi.org/10.1183/00000000.00000000
Hotamisligil GS (2010) Endoplasmic Reticulum stress and the inflammatory basis of metabolic disease. Cell 140:900–917. https://doi.org/10.1016/j.cell.2010.02.034
Huertas A, Tu L, Humbert M, Guignabert C (2020) Chronic inflammation within the vascular wall in pulmonary arterial hypertension: more than a spectator. Cardiovasc Res 116:885–893. https://doi.org/10.1093/cvr/cvz308
Kirkham B, Chaabo K, Hall C et al (2016) Safety and patient response as indicated by biomarker changes to binding immunoglobulin protein in the phase I/IIA RAGULA clinical trial in rheumatoid arthritis. Rheumatology (United Kingdom) 55:1993–2000. https://doi.org/10.1093/rheumatology/kew287
Koyama M, Furuhashi M, Ishimura S et al (2014) Reduction of endoplasmic reticulum stress by 4-phenylbutyric acid prevents the development of hypoxia-induced pulmonary arterial hypertension. Am J Physiol Heart Circ Physiol 306:1314–1323. https://doi.org/10.1152/ajpheart.00869.2013
Mahadevan NR, Rodvold J, Sepulveda H et al (2011) Transmission of endoplasmic reticulum stress and pro-inflammation from tumor cells to myeloid cells. Proc Natl Acad Sci U S A 108:6561–6566. https://doi.org/10.1073/pnas.1008942108
Mao SZ, Fan XF, Xue F et al (2014) Intermedin modulates hypoxic pulmonary vascular remodeling by inhibiting pulmonary artery smooth muscle cell proliferation. Pulm Pharmacol Ther 27:1–9. https://doi.org/10.1016/j.pupt.2013.06.004
Meunier L, Usherwood YK, Chung KTHL (2002) A subset of chaperones and folding enzymes form multiprotein complexes in endoplasmic reticulum to bind nascent proteins. Mol Biol Cell 13:4456–4469. https://doi.org/10.1091/mbc.E02
Olsson KM, Halank M, Egenlauf B et al (2018) Decompensated right heart failure, intensive care and perioperative management in patients with pulmonary hypertension: Updated recommendations from the Cologne Consensus Conference 2018. Int J Cardiol 272:46–52. https://doi.org/10.1016/j.ijcard.2018.08.081
Pegtel DM, Gould SJ (2019) Exosomes. Annu Rev Biochem 88:487–514. https://doi.org/10.1146/annurev-biochem-013118-111902
Qin K, Ma S, Li H et al (2017) GRP78 impairs production of lipopolysaccharide-induced cytokines by interaction with CD14. Front Immunol 8:1–11. https://doi.org/10.3389/fimmu.2017.00579
Rabinovitch M (2012) Molecular pathogenesis of pulmonary arterial hypertension. J Clin Invest 122:4306–4313. https://doi.org/10.1172/JCI60658DS1
Raychaudhuri B, Dweik R, Connors MJ et al (1999) Nitric oxide blocks nuclear factor-κB activation in alveolar macrophages. Am J Respir Cell Mol Biol 21:311–316. https://doi.org/10.1165/ajrcmb.21.3.3611
Schermuly RT, Dony E, Ghofrani HA et al (2005) Reversal of experimental pulmonary hypertension by PDGF inhibition. J Clin Investig 115:2811–2821. https://doi.org/10.1172/JCI24838
Seibert TA, Hibbert B, Chen YX et al (2013) Serum heat shock protein 27 levels represent a potential therapeutic target for atherosclerosis: Observations from a human cohort and treatment of female mice. J Am Coll Cardiol 62:1446–1454. https://doi.org/10.1016/j.jacc.2013.05.041
Shields AM, Panayi GS, Corrigall VM (2011) Resolution-associated molecular patterns (RAMP): RAMParts defending immunological homeostasis? Clin Exp Immunol 165:292–300. https://doi.org/10.1111/j.1365-2249.2011.04433.x
Simonneau G, Montani D, Celermajer DS et al (2019) Haemodynamic definitions and updated clinical classification of pulmonary hypertension. Eur Respir J 53:1801913. https://doi.org/10.1183/13993003.01913-2018
Simpson CE, Chen JY, Damico RL et al (2020) Cellular sources of IL-6 and associations with clinical phenotypes and outcomes in PAH. Eur Respir J 55:1901761. https://doi.org/10.1183/13993003.01761-2019
Sommer N, Strielkov I, Pak O, Weissmann N (2016) Oxygen sensing and signal transduction in hypoxic pulmonary vasoconstriction. Eur Respir J 47:288–303. https://doi.org/10.1183/13993003.00945-2015
Thenappan T, Ormiston ML, Ryan JJ, Archer SL (2018) Pulmonary arterial hypertension: Pathogenesis and clinical management. BMJ 360:j5492. https://doi.org/10.1136/bmj.j5492
Tirosh A, Tuncman G, Calay ES et al (2021) Intercellular transmission of hepatic ER stress in obesity disrupts systemic metabolism. Cell Metab 33:1–15. https://doi.org/10.1016/j.cmet.2020.11.009
Zaiss MM, Hall C, McGowan NWA et al (2019) Binding immunoglobulin protein (BIP) inhibits TNF-α–induced osteoclast differentiation and systemic bone loss in an erosive arthritis model. ACR Open Rheumatol 1:382–393. https://doi.org/10.1002/acr2.11060
Zhao L, Ackerman SL (2006) Endoplasmic reticulum stress in health and disease. Curr Opin Cell Biol 18:444–452. https://doi.org/10.1016/j.ceb.2006.06.005
Acknowledgements
We thank Dr. Meghan Lucas for critical reading of the manuscript. Furthermore, we thank Dr. Stilla Freede from the anesthesiology department of the University Hospital Bonn for providing the hypoxia incubator.
Funding
Open Access funding enabled and organized by Projekt DEAL. This work was supported by the medical faculty of the University of Bonn (BONFOR Grant No. 2018-1A-02 and 2021-2A-04 to AA). CB was supported by the German Society for Internal Medicine (Peter Scriba Scholarship).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethics approval/consent to participate
All procedures were in accordance with the ethical standards of the responsible committee on human experimentation (institutional and national) and with the Helsinki Declaration of 1975, as revised in 2000. Ethical approval was granted from the Ethics Committee of the University of Bonn. Informed consent was obtained from all patients for being included in the study.
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
ESM 1
(PDF 207 kb)
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Al Zaidi, M., Pizarro, C., Bley, C. et al. ER-stress-induced secretion of circulating glucose-regulated protein 78kDa (GRP78) ameliorates pulmonary artery smooth muscle cell remodelling. Cell Stress and Chaperones 27, 561–572 (2022). https://doi.org/10.1007/s12192-022-01292-y
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12192-022-01292-y