Abstract
Background
Development of secondary tumor after CART treatment is not well investigated. We report a pediatric B-cell acute lymphoblastic leukemia (B-ALL) patient who developed histiocytic sarcoma shortly after CART therapy.
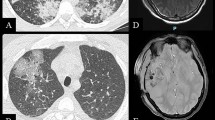
Case report: A 9-year-old boy diagnosed with relapsed B-ALL presenting the KRAS A146T mutation received autologous mouse-derived CD19 and CD22 chimeric antigen receptor T-cell therapy at our center (Chinese Clinical Trial Registry: ChiCTR2000032211). Thirty days post-CART therapy, the bone marrow showed complete remission. At 85 days post-CART therapy, the boy presented with fever and chills. An abdominal CT scan showed massive hepatomegaly with multiple low-density lesions in the liver. At 130 days post-CART therapy, a bone marrow smear showed abnormal proliferation of macrophages, some of which exhibited phagocytosis. On day 136 post-CART therapy, laparoscopic liver biopsy was performed, revealing multiple yellow–white lesions on the surface of the liver. Microscopically, multifocal lesions were observed, predominantly composed of cells with abundant cytoplasm. Immunohistochemical staining indicated histiocytic origin. Based on the immunohistochemical results, histiocytic sarcoma was diagnosed. The same cytogenetic markers were identified in histiocytic sarcoma. Conclusion: Our case illustrates a rare complication after CART therapy. The diagnosis and treatment of histiocytic sarcoma pose many challenges.


Similar content being viewed by others
Data availability
Data will be available through reasonable requests.
References
Wang T, Tang Y, Cai J, et al. Coadministration of CD19- and CD22-directed chimeric antigen receptor T-cell therapy in childhood B-cell acute lymphoblastic leukemia: a single-arm, multicenter, phase II trial. J Clin Oncol. 2023;41(9):1670–83. https://doi.org/10.1200/JCO.22.01214.
.Jacobson CA, Chavez JC, Sehgal AR, et al. Axicabtagene ciloleucel in relapsed or refractory indolent non-Hodgkin lymphoma (ZUMA-5): a single-arm, multicentre, phase 2 trial. Lancet Oncol. 2022;23(1):91–103. https://doi.org/10.1016/S1470-2045(21)00591-X
Fajgenbaum DC, June CH. Cytokine storm. N Engl J Med. 2020;383(23):2255–73. https://doi.org/10.1056/NEJMra2026131.
Cohen AD, Parekh S, Santomasso BD, et al. Incidence and management of CAR-T neurotoxicity in patients with multiple myeloma treated with ciltacabtagene autoleucel in CARTITUDE studies. Blood Cancer J. 2022;12(2):32. Published 2022 Feb 24. https://doi.org/10.1038/s41408-022-00629-1
Wang Y, Qi K, Cheng H, et al. Coagulation disorders after chimeric antigen receptor T cell therapy: analysis of 100 patients with relapsed and refractory hematologic malignancies. Biol Blood Marrow Transplant. 2020;26(5):865–75. https://doi.org/10.1016/j.bbmt.2019.11.027.
Alvi RM, Frigault MJ, Fradley MG, et al. Cardiovascular events among adults treated with chimeric antigen receptor T-cells (CAR-T). J Am Coll Cardiol. 2019;74(25):3099–108. https://doi.org/10.1016/j.jacc.2019.10.038.
Chong EA, Ruella M, Schuster SJ. Lymphoma Program Investigators at the University of Pennsylvania. Five-year outcomes for refractory B-cell lymphomas with CAR T-cell therapy. N Engl J Med. 2021;384(7):673–674. https://doi.org/10.1056/NEJMc2030164
Meniailo ME, Malashchenko VV, Shmarov VA, et al. Interleukin-8 favors pro-inflammatory activity of human monocytes/macrophages. Int Immunopharmacol. 2018;56:217–21. https://doi.org/10.1016/j.intimp.2018.01.036.
Kommalapati A, Tella SH, Durkin M, Go RS, Goyal G. Histiocytic sarcoma: a population-based analysis of incidence, demographic disparities, and long-term outcomes. Blood. 2018;131(2):265–8. https://doi.org/10.1182/blood-2017-10-812495.
Aparicio-Pérez C, Carmona M, Benabdellah K, Herrera C. Failure of ALL recognition by CAR T cells: a review of CD 19-negative relapses after anti-CD 19 CAR-T treatment in B-ALL. Front Immunol. 2023;14:1165870. Published 2023 Apr 14. https://doi.org/10.3389/fimmu.2023.1165870
Gauto-Mariotti E, Nguyen AJ, Waters C, et al. Transdifferentiation of high-grade B-cell lymphoma with MYC and BCL2 rearrangements into histiocytic sarcoma after CAR T-cell therapy: a case report. J Hematopathol. 2022;15:229–37. https://doi.org/10.1007/s12308-022-00519-2.
Gounder MM, Solit DB, Tap WD. Trametinib in histiocytic sarcoma with an activating MAP2K1 (MEK1) mutation. N Engl J Med. 2018;378(20):1945–7. https://doi.org/10.1056/NEJMc1511490.
Hu B, Patel JL, Tao R, Cannon RB, Monroe M, Goyal G. Near complete response to trametinib treatment in histiocytic sarcoma harboring a somatic KRAS mutation. J Natl Compr Canc Netw. 2022;20(6):618–621. Published 2022 Mar 24. https://doi.org/10.6004/jnccn.2022.7001
Zhao Y, Deng Y, Jiang Y, et al. Case report: Targeting the PD-1 receptor and genetic mutations validated in primary histiocytic sarcoma with hemophagocytic lymphohistiocytosis. Front Immunol. 2023;14:1127599. Published 2023 Mar 8. https://doi.org/10.3389/fimmu.2023.1127599
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of interests
The authors declare that they have no competing interests.
Ethical approval
The study was approved by the institutional review board of SCMC.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
New findings: Chimeric antigen receptor T-cell therapy (CART) has emerged as a novel treatment modality for relapsed and refractory leukemia and lymphoma patients. The study of secondary tumor after CART treatment is limited. We report a pediatric B-ALL patient who developed histiocytic sarcoma shortly after CART therapy. In our study, the patient presented fever and liver mass shortly after CART cell therapy. The same cytogenetic markers (KRAS A146T) were identified in histiocytic sarcoma. Same cytogenetic markers have suggested a common clonal origin between primary hematolymphoid disorders and histiocytic sarcoma.
About this article
Cite this article
An, K., He, Y., Tang, Y. et al. Histiocytic sarcoma following CAR T-cell therapy: a case report. Int J Hematol 119, 338–341 (2024). https://doi.org/10.1007/s12185-023-03695-8
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12185-023-03695-8