Abstract
Objective
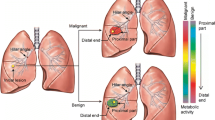
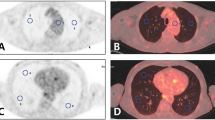
The dependent-density of computed tomography (CT) images of positron emission tomography (PET)/CT is sometimes difficult to distinguish from chronic interstitial lung disease (ILD) when it accompanies increased 18F-fluorodeoxy-d-glucose (18FDG) uptake. Though the possible utility of 18FDG-PET for the diagnosis of active ILD has been reported, the clinical relevance of mild lung 18FDG uptake in ILD cases without signs and symptoms suggesting acute progression has not been described. This study aimed to test relationships between 18FDG uptake and lung density on CT using PET/CT in patients with normal lung as well as clinically stable chronic ILD.
Methods
Thirty-six patients with normal lungs (controls) and 28 patients with chronic ILD (ILD cases) without acute exacerbation were retrospectively selected from 18FDG-PET/CT scans performed in examination of malignant neoplasms. Elliptical regions of interest (ROIs) were placed on the lung. The relationships between CT density and 18FDG uptake between the control and ILD cases were tested.
Results
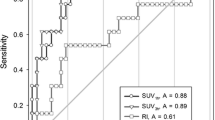
The CT density and 18FDG uptake had a linear correlation in both the controls and the ILD cases without a difference in their regression slopes, and they were overlapped between the controls and the ILD cases with higher mean values in the ILD cases.
Conclusions
Lung 18FDG uptake was considered to reflect a gravity-dependent tissue density in the normal lung. Though the lung 18FDG uptake as well as the CT density tended to be higher in chronic ILD patients, it may be difficult to distinguish them in normal dependent regions from those related to chronic ILD in some cases.



Similar content being viewed by others
References
Volpe J, Storto ML, Lee K, Webb WR. High-resolution CT of the lung: determination of the usefulness of CT scans obtained with the patient prone based on plain radiographic findings. Am J Roentgenol. 1997;169:369–74.
Kashiwabara K, Kohshi S. Additional computed tomography scans in the prone position to distinguish early interstitial lung disease from dependent density on helical computed tomography screening patient characteristics. Respirology. 2006;11:482–7.
Kuehl H, Veit P, Rosenbaum SJ, Bockisch A, Antoch G. Can PET/CT replace separate diagnostic CT for cancer imaging? Optimizing CT protocols for imaging cancers of the chest and abdomen. J Nucl Med. 2007;48(Suppl 1):45S–57S.
Pantin CF, Valind SO, Sweatman M, Lawrence R, Rhodes CG, Brudin L, et al. Measures of the inflammatory response in cryptogenic fibrosing alveolitis. Am Rev Respir Dis. 1988;138:1234–41.
Meissner HH, Soo Hoo GW, Khonsary SA, Mandelkern M, Brown CV, Santiago SM. Idiopathic pulmonary fibrosis: evaluation with positron emission tomography. Respiration. 2006;73:197–202.
Lyburn ID, Lowe JE, Wong WL. Idiopathic pulmonary fibrosis on F-18 FDG positron emission tomography. Clin Nucl Med. 2005;30:27.
Kirsch J, Arrossi AV, Yoon JK, Wu G, Neumann DR. FDG positron emission tomography/computerized tomography features of bleomycin-induced pneumonitis. J Thorac Imaging. 2006;21:228–30.
Miyauchi T, Wahl RL. Regional 2-[18F]fluoro-2-deoxy-d-glucose uptake varies in normal lung. Eur J Nucl Med. 1996;23:517–23.
Verschakelen JA, Van Fraeyenhoven L, Laureys G, Demedts M, Baert AL. Differences in CT density between dependent and nondependent portions of the lung: influence of lung volume. Am J Roentgenol. 1993;161:713–7.
Robinson PJ, Kreel L. Pulmonary tissue attenuation with computed tomography: comparison of inspiration and expiration scans. J Comput Assist Tomogr. 1979;3:740–8.
Brudin LH, Rhodes CG, Valind SO, Wollmer P, Hughes JM. Regional lung density and blood volume in nonsmoking and smoking subjects measured by PET. J Appl Physiol. 1987;63:1324–34.
Aberle DR, Gamsu G, Ray CS, Feuerstein IM. Asbestos-related pleural and parenchymal fibrosis: detection with high-resolution CT. Radiology. 1988;166:729–34.
Wollmer P, Rhodes CG, Hughes JM. Regional extravascular density and fractional blood volume of the lung in interstitial disease. Thorax. 1984;39:286–93.
Jones HA, Schofield JB, Krausz T, Boobis AR, Haslett C. Pulmonary fibrosis correlates with duration of tissue neutrophil activation. Am J Respir Crit Care Med. 1998;158:620–8.
Kaim AH, Weber B, Kurrer MO, Gottschalk J, Von Schulthess GK, Buck A. Autoradiographic quantification of 18F-FDG uptake in experimental soft-tissue abscesses in rats. Radiology. 2002;223:446–51.
Yamada S, Kubota K, Kubota R, Ido T, Tamahashi N. High accumulation of fluorine-18-fluorodeoxyglucose in turpentine-induced inflammatory tissue. J Nucl Med. 1995;36:1301–6.
Chen DL, Mintun MA, Schuster DP. Comparison of methods to quantitate 18F-FDG uptake with PET during experimental acute lung injury. J Nucl Med. 2004;45:1583–90.
Gotway MB, Freemer MM, King TE Jr. Challenges in pulmonary fibrosis. 1: Use of high resolution CT scanning of the lung for the evaluation of patients with idiopathic interstitial pneumonias. Thorax. 2007;62:546–53.
Selman M, King TE, Pardo A. Idiopathic pulmonary fibrosis: prevailing and evolving hypotheses about its pathogenesis and implications for therapy. Ann Intern Med. 2001;134:136–51.
Wallace WE, Gupta NC, Hubbs AF, Mazza SM, Bishop HA, Keane MJ, et al. Cis-4-[(18)F]fluoro-L-proline PET imaging of pulmonary fibrosis in a rabbit model. J Nucl Med. 2002;43:413–20.
Lebtahi R, Moreau S, Marchand-Adam S, Debray MP, Brauner M, Soler P, et al. Increased uptake of 111In-octreotide in idiopathic pulmonary fibrosis. J Nucl Med. 2006;47:1281–7.
Acknowledgments
The authors thank the technical staff of Tohoku University Hospital for PET data acquisition. This study was supported, in part, by the Japanese Ministry of Education, Science, Sports and Culture, a Grant-in-Aid for Young Scientists (B), 19790852, and a Grant-in-Aid for Cancer Research (17-12) from the Ministry of Health, Labour, and Welfare.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Inoue, K., Okada, K., Taki, Y. et al. 18FDG uptake associated with CT density on PET/CT in lungs with and without chronic interstitial lung diseases. Ann Nucl Med 23, 277–281 (2009). https://doi.org/10.1007/s12149-009-0234-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12149-009-0234-8