Abstract
Poor emotion regulation, along with elevated perfectionism, is recognised as a risk factor for the development of eating disorder (ED) symptoms. Therefore, the aim of our study was to examine the relationship between emotion regulation difficulties and perfectionism with ED symptoms, while controlling for emotional eating, uncontrolled eating, and cognitive restraint as mediators. In total, 482 adolescents (246 girls and 236 boys; M = 15.00, SD = 0.31) participated in this study. Based on the participants’ body height and weight measured by the medical team during their regular preventive health examinations, the body mass index (BMI) was calculated. Participants also answered the Difficulties in Emotion Regulation Scale, Multidimensional Perfectionism Scale, Three-Factor Eating Questionnaire, and Eating Disorder Examination Questionnaire. According to the results obtained, adolescent girls in our sample reported more difficulties in emotion regulation, more uncontrolled and emotional eating, and more ED symptoms. A significant direct effect was found for difficulties in emotion regulation and ED symptoms but not for perfectionism. In addition, only emotional eating and cognitive restraint (not uncontrolled eating) mediated the relationship between difficulties in emotion regulation and perfectionism and ED symptoms. The results suggest that difficulties in emotion regulation may be more important than perfectionism in explaining ED symptoms in a sample of healthy adolescents. When adolescents experience problems in emotion regulation in combination with emotional or uncontrolled eating, they might be at a higher risk of experiencing concerns about weight and a variety of other ED symptoms, and this should be considered when planning preventive interventions for adolescents.
Similar content being viewed by others
Introduction
Eating disorders (ED) occur in people of different ages, but the average age of onset is adolescence. During the second half of the 20th century, the prevalence rates of ED increased and remained relatively stable over the last 20 years (Voderholzer et al., 2012). ED ranks as the third most common chronic illness in adolescent females, with an incidence of up to 5% (Croll et al., 2002). A high percentage of girls and young women (38.9%) reported subclinical ED symptoms, including preoccupation with eating, shape and weight concerns, dietary restraint, and excessive exercise (Cain et al., 2010; Tng & Yang, 2021). Several risk factors are associated with ED development (Cella et al., 2020; Rohde et al., 2015; Solmi et al., 2021), and recent research has focused on characteristics such as emotion regulation skills (Christensen & Haynos, 2020; Leppanen et al., 2022; Ruscitti et al., 2016; Weinbach et al., 2018), perfectionism (Cella et al., 2020; Jacobi et al., 2018; Keel & Forney, 2013; Stice, 2002), and eating patterns (Krug et al., 2008; Zambrowicz et al., 2019).
Emotion regulation
Emotion regulation has been conceptualised as a process through which individuals modulate their emotions (Aldao et al., 2010; Rottenberg & Gross, 2003) to respond appropriately to environmental demands (Thompson, 1994). Roots of the idea that intrapersonal mechanisms could regulate drives and emotions (as a predecessor of the present conception of ER) can be found in the classical psychoanalytic tradition (Gross, 1999; Palmieri et al., 2022), especially in the distinction between implicit and explicit ER processes (Gyurak et al., 2011). Explicit ER mechanisms can be conceptualized as deliberate cognitive manipulations responsible for monitoring, adjustment, and selection of the emotional and/or behavioural responses from a range of options, while implicit ER depends on external influences and self-evaluations, together with immediate response tendencies. Deficits in implicit ER, rather than in explicit ER, may be more accountable for psychopathology, including anxiety disorders (Etkin et al., 2010) and mood disorders (Ehring et al., 2010).
Theoretical models associate successful emotion regulation with good health outcomes, social functioning, well-being, and academic performance (John & Gross, 2004). On the other hand, difficulties with emotion regulation are associated with mental disorders (Aldao et al., 2010; Mennin & Farach, 2007) and have been incorporated into several models of specific psychopathologies, including major depressive disorder, bipolar disorder, generalised anxiety, social anxiety, and ED (Aldao et al., 2010). Emotion regulation includes several main features such as awareness of one’s emotions and naming them, identifying their causes, actively changing emotions, accepting and tolerating negative emotions, dealing with situations that could provoke negative emotions, and self-support in stressful situations (Berking & Whitley, 2014). In their model of emotion regulation, Gratz and Roemer (2004) included different dimensions: the ability to use appropriate strategies to modulate emotions; the ability to inhibit impulsive behaviours; the capacity to engage in goal-directed behaviour; and the acceptance, awareness, and understanding of emotions. Deficits in these dimensions reflect emotional dysregulation (Lavender et al., 2015), which has been associated with ED severity (Pisetsky et al., 2017; Vieira et al., 2021). In adolescence, decisions about different emotion regulation strategies depend on motivation, type of emotion, and social context (Zeman et al., 2006).
Research has shown that a stressful or negative event can lead to poorer emotion regulation which in turn poses a risk factor for developing maladaptive coping strategies (Berking & Whitley, 2014). Maladaptive strategies include rumination, avoidance, and suppression of emotions, while adaptive strategies include reappraisal, active problem-solving, and mindfulness strategies based on awareness and acceptance of emotions (Aldao et al., 2010). Individuals with ED have been reported to use more maladaptive emotion regulation strategies (Leppanen et al., 2022; Trompeter et al., 2021; Aparicio et al., 2016) emphasised that the use of maladaptive emotion regulation strategies can create a vicious circle, as it may increase the negative emotions which are involved in developing maladaptive strategies (Aparicio et al., 2016; Berking & Whitley, 2014).
The role of perfectionism in eating disorders
In addition to emotion regulation, perfectionism is another construct that is commonly researched in relation to ED. Perfectionism is a multidimensional construct that consists of several factors. According to Frost et al. (1990), six dimensions can be differentiated when discussing perfectionism: concerns about mistakes, personal standards, parental expectations and parental criticism, self-doubt, procedures, and organisation. Various studies using multidimensional measures of perfectionism have suggested two underlying factors. Conceptually, the literature distinguishes between dimensions of normal (reasonable standards that lead to satisfaction) and neurotic perfectionism (excessively high standards motivated by fear of failure) (Hamachek, 1978), as well as positive (behaviour driven by positive reinforcement) and negative perfectionism (behaviour driven by negative reinforcement) (Terry-Short et al., 1995).
Fairburn et al. (2003) hypothesised that perfectionism could be a maintenance factor in ED. They see perfectionism as a predictor of enhanced concerns about eating and weight, which can further be associated with weight control behaviours (e.g. diet) and later development of ED symptoms. According to Bulik et al. (2003), higher scores on perfectionism subscales (e.g. concerns about mistakes and self-doubt) are associated with a higher likelihood of developing anorexia and bulimia nervosa symptoms. Similar results were reported by Boone et al. (2010), who obtained a correlation between concerns about mistakes and self-doubt with the pathology of ED. Bardone-Cone et al. (2010) found that patients with EDs scored significantly higher than healthy controls on the maladaptive perfectionism. Several studies have reported that elevated levels of both adaptive and maladaptive perfectionism are associated with body dissatisfaction and ED symptomatology (Bardone-Cone et al., 2007; Limburg et al., 2017).
Donahue et al. (2018) found a significant interaction effect of socially prescribed perfectionism (an indicator of maladaptive perfectionism) and difficulties in emotion regulation in explaining the variance of ED symptoms. Perfectionism and difficulties in emotional regulation are probably interrelated through the process of rumination, and both are related to ED symptoms. Several meta-analyses (Meule et al., 2021; Prefit et al., 2019) have illustrated the relationship between ED symptoms and elevated levels of rumination. Rivière and Douilliez (2017) found that rumination, as a maladaptive way of dealing with negative emotions, mediates between perfectionism and ED symptoms. Different studies suggest that ED symptoms are linked to the use of maladaptive strategies such as rumination, catastrophising, and self-blame, which are characterised by persevering thoughts or self-criticism (Meule et al., 2021; Prefit et al., 2019; Tng & Yang, 2021; Bardone-Cone et al., 2007) in their review concluded that EDs are characterised by high-level perfectionism which persists after recovery and has a predispositional effect on the development of EDs.
Cognitive eating patterns and disturbed eating habits
Another relevant construct commonly related to disturbed eating habits is a cognitive eating pattern e.g. the cognitive and behavioural components of eating (Karlsson et al., 2000). Uncontrolled eating, cognitive restraint, and emotional eating are the three factors of cognitive eating patterns related to disturbed eating. Inability to control eating, emotional eating, and mental preoccupation with food might predict ED symptoms through various behaviours, such as weight loss attempts (e.g. food intake restriction, fasting), guilt over eating, body and weight dissatisfaction, and adherence to certain dietary rules. In stressful situations, some individuals might use maladaptive coping strategies or maladaptive eating behaviours, such as emotional eating, to deal with emotions (Taut et al., 2012). Emotional eating may occur when a person lacks the ability to regulate emotions, which may explain the relationship between emotional dysregulation and disturbed eating by modifying dietary intake (Francis & Susman, 2009; Graziano et al., 2010; Isasi et al., 2013). Research on children and adolescents has emphasised the connection between maladaptive emotion regulation strategies and emotional eating (Harrist et al., 2013; Kubiak et al., 2008; Vandewalle et al., 2014).
Study aims and hypotheses
In conclusion, ED is associated with serious biological, psychological, and sociological morbidity, and significant mortality (Golden et al., 2003). During adolescence, young people undergo many changes as they reach physical maturity. Particularly in girls, puberty leads to weight gain and accumulation of body fat in specific body parts such as the waist, hips, thighs, and buttocks. As they mature, girls move away from the ideal of thinness, which can be associated with body dissatisfaction (Pokrajac-Bulian et al., 2004), and makes them more vulnerable to the development of ED symptoms. The unique features and developmental process of adolescents are critical considerations in determining the diagnosis, treatment, and outcome of ED at this age (Golden et al., 2003). Research shows that perfectionism and emotion regulation are significantly associated with ED symptoms (i.e. shape, weight, eating concerns, and dietary restraint) in adolescents (Tng & Yang, 2021) and are implicated as risk (Cella et al., 2020; Hilbert et al., 2014; Stice, 2002) and maintenance factors (Cella et al., 2020; Fairburn et al., 2003; Stice, 2002).
Based on previous findings and theoretical relations between studied constructs, the aim of this study was to examine the relationship between difficulties in emotion regulation and perfectionism with ED symptoms by controlling for emotional eating, uncontrolled eating, and cognitive restraint as mediators. We hypothesised that the relationship between emotion dysregulation and perfectionism with ED symptoms is mediated by different cognitive eating patterns (emotional eating, uncontrolled eating, and cognitive restraint). We hope to clarify the possible paths between emotion regulation difficulties and perfectionism with ED symptoms, since cognitive eating factors might predict ED symptoms through various behaviours. By revealing the interactions between specific risk factors for eating disorder symptoms, we sought to advance the theoretical understanding and intervention strategies taking into account multiple psychosocial factors.
Method
Participants
This research was conducted on first-grade high school students who came to school medicine doctors to perform a regular preventive health examination. A total of 482 adolescents (246 girls and 236 boys) participated in this study. The average age was 15.00 years (SD = 0.31). Based on the participants’ body height and weight measured by the medical team during the examination, the body mass index was calculated [weight (kg)/height (m)2] and expressed as a percentile. In the current sample, 2.8% of participants were underweight, 74% had normal weight, 12.9% were overweight, and 10.3% were obese.
Instruments
Difficulties in Emotion Regulation Scale (DERS-16; Bjureberg et al., 2016) is a 16-item self-report measure that examines different aspects of emotion regulation difficulties. Items form five subscales measuring the lack of clarity of emotions, problems with goal-directed behaviours, difficulty in impulse control, insufficient strategies of emotion regulation, and non-acceptance of negative emotions. Participants responded to statements on a 5-point response scale (1 = almost never to 5 = almost always), indicating how often they feel or behave in the described way. The total score can be calculated by summing up the responses on all items, with higher scores representing greater emotion dysregulation, that is, more problems in emotion regulation. Only the total score was used in this study. The overall scale showed excellent reliability (α = 0.91).
The Multidimensional Perfectionism Scale (MPS-F; Frost et al., 1990), with its 35 items divided into six subscales, allows the assessment of specific domains of perfectionism but may also provide an overall perfectionism score. Participants estimated the extent to which they agreed with a particular statement on a 5-point response scale (1 = strongly disagree to 5 = strongly agree). For the purposes of the present study, only a total score was used based on 12 items from four subscales which measured the tendency to set high performance standards and practice excessive self-criticism (Personal Standards and Concern Over Mistakes subscales) and perception of high parental expectations and criticism (Parental Expectations and Parental Criticism subscales). Items from subscales Doubts about actions (a tendency to be uncertain about the correctness of one’s decisions or behaviours) and Organisation (a tendency to be overly orderly, organised, and tidy) were not included. Twelve items were selected based on the highest item-factor saturation in the exploratory factor analysis. Good reliability (α = 0.82) was obtained for the scale.
The Three-Factor Eating Questionnaire (TFEQ-R18; Karlsson et al., 2000) is an 18-item self-report measure. Items form three subscales examining different eating patterns: cognitive restraint, uncontrolled eating, and emotional eating. The cognitive restraint subscale refers to a person’s conscious effort to limit food intake to control or reduce their body weight. The Uncontrolled Eating subscale refers to a person’s tendency to consume more food than usual, with a sense of losing control, while the emotional eating subscale refers to eating in response to negative emotions. Item 15 (How frequently do you avoid “stocking up” on tempting foods?) was removed from the questionnaire because most grocery shopping is done by parents, not by adolescents. Participants responded on a 4-point scale about how often they behave in a certain way or how true a certain statement is for them. Higher scores indicate more of the behaviour. In our sample, Cronbach’s alphas were satisfactory for all subscales, ranging from 0.75 0.83.
The Eating Disorder Examination Questionnaire (EDE-Q 6.0; Fairburn & Beglin, 2008) is a self-report measure that examines symptomatology and behaviours related to eating disorders over the previous 28 days. It consists of 28 items, 22 of which form four subscales (Restraint, Eating Concern, Shape Concern, and Weight Concern), while the other six measure the frequency of specific behaviours, such as self-induced vomiting and excessive exercise. The questionnaire also included questions on height, weight, menstruation, and the use of contraceptive pills. Participants responded to questionnaire items using a 7-point scale to estimate the frequency (0 = no days to 6 = every day) or severity (0 = not at all to 6 = markedly) of specific behaviours or eating disorder symptoms or by providing the exact number of days or episodes in which the behaviour occurred. In the present study, only the overall score (mean of the four subscale scores) was used, which showed good reliability (α = 0.86).
Procedure
The study was conducted prior to the COVID-19 pandemic, from February to March 2020. Data were collected in the offices of school medicine physicians during regular preventive health examinations organised every year for first-grade high school students by the [anonymized for review]. Participants completed self-report questionnaires in the presence of the researcher’s assistants, and the medical team measured the height and weight of each student. In addition, through conversation with each student, the physicians collected information about taking medications, previous psychotherapy, chronic illness, and dieting for weight loss. Informed consent was obtained from all participants; parents, school principals, and teachers were informed in writing about the research. The research was anonymous and voluntary, and the participants received no compensation. This study was part of a research project reviewed and approved by the [anonymized for review]. In addition, [anonymized for review] also reviewed and approved the research.
Data analysis
First, descriptive statistics (mean, standard deviation, skewness, and kurtosis) and zero-order correlations (Pearson’s coefficient) were calculated. Second, to test the hypothesised relationship between variables, a mediation analysis was performed. To determine whether the three dimensions of cognitive eating patterns (uncontrolled eating, emotional eating, and cognitive restraint) mediated the relationship between difficulties in emotion regulation and perfectionism with ED symptoms, mediation analysis was performed using R language and environment for statistical computing (R Development Core Team, 2013), with the package “mediation” (Tingley et al., 2019) and the JASP (2020) software. The bootstrapping technique with 5,000 subsamples was used to estimate the confidence interval (95%). Estimates of the indirect effects of multiple mediators, along with standard errors (SE) and confidence intervals (CI), were obtained. Indirect effects were considered statistically significant if the confidence intervals (CI of 95%) did not contain zero (Hayes & Preacher, 2013).
Results
Descriptive statistics
The means, standard deviations, and intercorrelations between the variables are shown in Table 1, which also includes internal consistency measures for each composite measure in the present sample.
Three variables had skewness lower than ± 1, as suggested by Muthen & Kaplan (1985), and there were three variables with skewness above 1 (one was above 2). In line with Tabachnick and Fidell’s (2013) recommendation, a distribution can be treated as normal if its skewness does not exceed ± 2, whereas Kline (2005) allows it to reach ± 3. Since there are many different criteria for deciding on the acceptable limits of skewness and kurtosis, we also visually examined each variable distribution, as suggested by Tabachnick and Fidell (2013), and concluded that there are no major deviations from normality. All the variables had satisfactory reliability coefficients. It is worth noting that all mean values shifted towards lower values because the sample did not include individuals with known ED problems, but a general high school population. The results of the correlation analysis are presented in Table 2.
Girls in our sample reported more difficulties in emotion regulation, uncontrolled and emotional eating, and more ED symptoms. Body mass index (BMI) was positively correlated with ED symptoms (r = .42, p < .01) and cognitive restraint (r = .36, p < .01) but not with emotional or uncontrolled eating. A significant positive correlation was found between difficulties in emotion regulation and perfectionism (r = .39, p < .01). Furthermore, adolescents who reported more problems with emotion regulation also reported more uncontrolled eating (r = .32, p < .01), emotional eating (r = .35, p < .01), cognitive restraint (r = .19, p < .05), and more ED symptoms (r = .39, p < .01). Cognitive restraint had the highest correlation with ED symptoms (r = .65, p < .01).
Mediation analysis
In the present study, we hypothesised that difficulties in emotion regulation and perfectionism would affect ED symptoms both directly and indirectly through cognitive eating patterns (emotional eating, uncontrolled eating, and cognitive restraint).
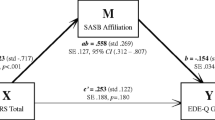
The results regarding the mediating effect of the three cognitive eating patterns (emotional eating, uncontrolled eating, and cognitive restraint) on the relationship between difficulties in emotion regulation, perfectionism, and ED symptoms revealed a significant direct association between difficulties in emotion regulation and ED symptoms (β = .22, SE = 0.05, p < .001; 95% CI [0.10, 0.33]), but the direct effect of perfectionism on ED symptoms was not significant (β = .12, SE = 0.05, p = .021; 95% CI [-0.02, 0.27]). The direct, indirect, and total effects of emotional dysregulation, perfectionism, cognitive eating patterns, and ED symptoms are shown in Table 3.
The analyses of indirect effects suggested significant paths from difficulties in emotion regulation to ED symptoms through cognitive restraint and emotional eating. Similar to perfectionism, the analysis revealed significant paths from perfectionism to ED symptoms, through cognitive restraint and emotional eating. For both emotion regulation difficulties and perfectionism, the indirect effect of uncontrolled eating on ED symptoms was insignificant. Regarding total effects, both difficulties in emotion regulation and perfectionism had significant total effects on ED symptoms. The total indirect effect was also significant for both the variables.
A path model showing the effects of difficulties in emotion regulation, perfectionism, and cognitive eating patterns on ED symptoms is shown in Fig. 1.
As can be seen from the path model, the highest path coefficients were found between difficulties in emotion regulation and uncontrolled eating (β = .40) and emotional eating (β = .42). Perfectionism had lower path coefficients for cognitive eating patterns, and the highest was found for cognitive restraint (β = .30). Cognitive restraint also had the highest coefficient for ED symptoms (β = .57). The results indicated that cognitive eating patterns (cognitive restraint, emotional, and uncontrolled eating) mediated the relationship between ED symptoms and emotion (dis) regulation and perfectionism, with cognitive restraint having the strongest path coefficients and the path for uncontrolled eating being insignificant. Adolescents with emotion regulation difficulties reported more emotional and uncontrolled eating. Furthermore, difficulties in emotion regulation are directly associated with ED symptoms. In contrast, perfectionism showed weaker relationships with cognitive eating patterns and ED symptoms.
Discussion
The present study aimed to examine the mediating role of cognitive eating patterns (emotional eating, uncontrolled eating, and cognitive restraint) in the relationship between difficulties in emotion regulation and perfectionism and ED symptoms in a sample of adolescent girls and boys. The data analysis partially confirmed the research hypotheses. A significant direct effect was found for difficulties in emotion regulation and ED symptoms but not for perfectionism. In addition, only emotional eating and cognitive restraint (but not uncontrolled eating) mediated the relationship between difficulties in emotion regulation, perfectionism, and ED symptoms.
As expected from previous studies (Forrester-Knauss et al., 2012; Nikolić et al., 2018; Zehr et al., 2007), adolescent girls in our sample reported more difficulties in emotion regulation, uncontrolled and emotional eating, and more ED symptoms. Adolescent girls frequently report poorer body image, a stronger desire for thinness and weight loss, the need for diets, and similar behaviours in order to control their own body shape and weight (Pokrajac-Bulian et al., 2004), which may lead to the development of ED symptoms. Zehr et al. (2007) also found that adolescent girls and young women achieved higher scores on all EDE-Q subscales than men, suggesting that females were more prone to developing an ED. Results showing that girls have more ED symptoms than boys have been found in numerous studies (e.g. Bento et al., 2010; White et al., 2014; Yucel et al., 2011). Significantly more female adolescents and young women in comparison to men reported that they often felt that they could not control what or how much they ate; however, more men than women reported overeating (Striegel-Moore et al., 2009). This may be due to the higher levels of perceived social pressure and awareness in females of what they “must” look like and what their body “must” be like, and their internalisation of such beauty standards.
In our study, BMI was positively correlated with cognitive restraint and ED symptoms. Megalakaki et al. (2013) showed that adolescents with higher BMI, especially those with obesity, were more likely to use cognitive restraint than adolescents with average weight, despite its ineffectiveness as a weight-control management strategy. Studies on the relationship between cognitive restraint and BMI (e.g. Anglé et al., 2009; Quick & Byrd-Bredbenner, 2012) suggest that mental food preoccupation leads to weight gain rather than weight loss, as might be expected. It is difficult to determine whether cognitive restraint preceding weight gain is an antecedent of cognitive restraint. However, a longitudinal study by de Lauzon-Guillain et al. (2006) found that mental preoccupation with food and dietary behaviour does not necessarily predict later weight gain, although it is associated with the accumulation of fat in average-weight individuals but not in persons with obesity. In our study, we also found that cognitive restraint had the strongest correlation with ED symptoms. More longitudinal research is needed to examine the complex relationship between BMI and cognitive eating patterns, particularly cognitive restraint.
Higher BMI was related to an increase in ED symptoms, which has been confirmed in other studies (e.g. Rø et al., 2012; Yucel et al., 2011). A study conducted on a random sample from the general population found that increases in body shape and weight concerns are mainly responsible for elevated EDE-Q scores and appear to be normative among people with obesity (Rø et al., 2012). It does not seem unusual that overweight people, or at least some of them, are dissatisfied with their weight and body shape and are uncomfortable in front of other people (e.g. in locker rooms, during physical education classes) and then want to lose weight in different ways, such as, for example, the exclusion of certain foods and following certain dietary rules, attempts at fasting, and intentional restriction of eating. This may especially apply to adolescents, who are already in a very sensitive developmental phase.
We found a significant positive correlation between difficulty in emotion regulation and perfectionism. Adolescents who reported more problems with emotion regulation also reported more uncontrolled and emotional eating, cognitive restraint, and ED symptoms. The relationship between perfectionism and ED symptoms is often found in the literature, either directly (Barnett & Sharp, 2016; Esposito et al., 2019) or indirectly through other variables, such as perfectionist thinking (Downey et al., 2014) and body dissatisfaction (Downey & Chang, 2007). Adolescents who set very high standards for themselves or feel that others are setting high standards for them can sometimes direct such standards toward their own bodies. In an effort to achieve a perfect appearance, a person may end up developing ED symptoms. Byrne et al. (2016) found that perfectionism alone may not have much influence on clinical impairment in college-aged women at high risk for ED; it may have a greater impact in conjunction with emotional dysregulation. Perhaps, some individuals who struggle to regulate emotions may use perfectionism as a maladaptive attempt of emotional control.
Perfectionism had a significant indirect effect on ED symptoms only through cognitive restraint and emotional eating. This is not surprising because perfectionism is recognised as a risk factor for ED in many studies (e.g. Boone et al., 2010; Brosof et al., 2019; Cella et al., 2020; Hilbert et al., 2014), and is correlated with feelings of concern related to eating (e.g., Peixoto-Plácido et al., 2015) because high personal standards can be reflected in attitudes toward eating and dieting. Eating concerns include, but are not limited to, preoccupation with food and calories (similar to cognitive restraint), fear of losing control during meals (similar to uncontrolled eating), and guilt over eating (possibly associated with emotional eating).
A significant direct effect was found between difficulties in emotion regulation and ED symptoms but not between perfectionism and ED symptoms. Emotion regulation is considered an important factor in the development and maintenance of ED. Lavender and Anderson (2010) and Sim and Zeman (2006) believe that the connection between these two constructs may arise from a person’s disposition to resort to specific (maladaptive) behaviours characteristic of ED in a bid to regulate or avoid negative emotions. Avoiding negative emotions by secretly eating or overeating or by monitoring one’s weight and body shape can lead to the development of ED symptoms. ED symptoms may foster emotions that are difficult to regulate and accept, especially in adolescence (Whiteside et al., 2007), which can aggravate maladaptive behaviours.
Racine and Wildes (2013) underline four links or similar characteristics between difficulties in emotion regulation and ED. First, problems in recognising and understanding emotions were present in both the cases. Second, individuals with ED, especially AN, have maladaptive beliefs about emotions, particularly those that contribute to strategies for avoiding or changing emotions. Third, people with overeating or purgative disorders often have control problems in the presence of strong emotions, and the inability to prevent inappropriate behaviours when experiencing strong emotions is one of the characteristics of emotional dysregulation. Finally, maladaptive strategies for emotion regulation are often found in people with ED (Racine & Wildes, 2013). Lack of skills and strategies for emotion regulation may mean that individuals, in order to cope with emotions, will resort to inappropriate eating habits (Donahue et al., 2018), as cognitive restraint or emotional eating. Other studies have also shown a correlation between emotional regulation difficulties and ED symptomatology (Donahue et al., 2018; Griffiths et al., 2014; Harrison et al., 2010; Racine & Wildes, 2013; Rowsell et al., 2016).
Limitations and strengths
The present findings should be interpreted in the light of some limitations. Similar to many other community-based studies, we relied on self-report questionnaires to measure ED symptoms, eating habits, emotion regulation, and perfectionism. Students filled in paper-and-pencil forms of the questionnaires in a group, which might have affected the sincerity of their answers. In addition, owing to the large number of questionnaires, fatigue may have occurred. The participants were first-grade high school students, most of whom were not used to completing such questionnaires. Some complained about the length and repetitiveness of the items and often asked for explanations. We can assume that some participants were too ashamed to ask for clarification or were not interested in the task, so the answers should be interpreted with caution. Nevertheless, the research included a relatively large sample of first-grade high school students from the two cities. The sample was balanced by sex, which is often not the case. Furthermore, collaboration with school physicians has enabled the inclusion of medical data and more accurate measurements of height and weight rather than a self-reported details, which often tend to be unreliable.
Implications
This study has implications for both future clinical work and clinical research. Maladaptive perfectionism as a specific risk factor for eating disorder behaviours already has its well-established place in the protocols of preventive programs and psychotherapy treatments, especially cognitive-behavioural ones (e.g., Dalle Grave & Calugi, 2020). The results of our research indicate that perfectionism should also be considered in the context of other variables, such as cognitive restraint and emotional eating. On the other hand, the research results show how important it is for clinicians to focus on the regulation of clients’ emotions in the prevention and treatment of eating disorders, specifically by increasing access to adaptive strategies. In working with adolescents who manifest symptoms of eating disorders, it is necessary to focus on education on emotion regulation skills as an adaptive way of coping with the pressure imposed by social ideals of body appearance. Consequences of eating disorders can reduce the quality of life and impair the physical and mental health of the person and should be taken seriously. The results of this research enable a better theoretical understanding of the ED symptoms and their correlates, focusing on psychosocial factors that should be included in early interventions with adolescents.
Conclusion
Although high levels of self-reported perfectionism were often found in individuals with ED (Egan et al., 2011), our results suggest that difficulties in emotion regulation may be more important than perfectionism in explaining ED in a sample of generally healthy adolescents. When adolescents experience problems in emotion regulation in combination with emotional or uncontrolled eating, they may be at a higher risk of experiencing concerns about weight while also being prone to a variety of eating disorders. Therefore, treatment and preventive interventions for adolescents should focus on emotion regulation.
References
Aldao, A., Nolen-Hoeksema, S., & Schweizer, S. (2010). Emotion-regulation strategies across psychopathology: A meta-analytic review. Clinical Psychology Review, 30(2), 217–237. https://doi.org/10.1016/j.cpr.2009.11.004
Anglé, S., Engblom, J., Eriksson, T., Kautiainen, S., Saha, M. T., Lindfors, P., Lehtinen, M., & Rimpela, A. (2009). Three factor eating questionnaire-R18 as a measure of cognitive restraint, uncontrolled eating and emotional eating in a sample of young Finnish females. International Journal of Behavioral Nutrition and Physical Activity, 6. https://doi.org/10.1186/1479-5868-6-41
Aparicio, E., Canals, J., Arija, V., De Henauw, S., & Michels, N. (2016). The role of emotion regulation in childhood obesity: Implications for prevention and treatment. Nutrition Research Reviews, 29, 17–29. https://doi.org/10.1017/S0954422415000153
Bardone-Cone, A. M., Sturm, K., Lawson, M. A., Robinson, D. P., & Smith, R. (2010). Perfectionism across stages of recovery from eating disorders. International Journal of Eating Disorders, 43(2), 139–148. https://doi.org/10.1002/eat.20674
Bardone-Cone, A. M., Wonderlich, S. A., Frost, R. O., Bulik, C. M., Mitchell, J. E., Uppala, S., & Simonich, H. (2007). Perfectionism and eating disorders: Current status and future directions. Clinical Psychology Review, 27(3), 384–405. https://doi.org/10.1016/j.cpr.2006.12.005
Barnett, M. D., & Sharp, K. J. (2016). Maladaptive perfectionism, body image satisfaction, and disordered eating behaviors among U.S. college women: The mediating role of self-compassion. Personality and Individual Differences, 99, 225–234. https://doi.org/10.1016/j.paid.2016.05.004
Bento, C., Pereira, A. T., Maia, B., Marques, M., Soares, M. J., Bos, S., Valente, J., Gomes, A., Azevedo, M. H. P., & Macedo, A. (2010). Perfectionism and eating behaviour in Portuguese adolescents. European Eating Disorders Review, 18(4), 328–337. https://doi.org/10.1002/erv.981
Berking, M., & Whitley, B. (2014). Affect Regulation Training. Springer Naure. https://doi.org/10.1007/978-1-4939-1022-9
Bjureberg, J., Ljótsson, B., Tull, M. T., Hedman, E., Sahlin, H., Lundh, L. G., Bjärehed, J., DiLillo, D., Messman-Moore, T., Gumpert, C. H., & Gratz, K. L. (2016). Development and validation of a brief version of the Difficulties in Emotion Regulation Scale: The DERS-16. Journal of Psychopathology and Behavioral Assessment, 38(2), 284–296. https://doi.org/10.1007/s10862-015-9514-x
Boone, L., Soenens, B., Braet, C., & Goossens, L. (2010). An empirical typology of perfectionism in early-to-mid adolescents and its relation with eating disorder symptoms. Behaviour Research and Therapy, 48, 686–691. https://doi.org/10.1016/j.brat.2010.03.022
Brosof, L. C., Egbert, A. H., Reilly, E. E., Wonderlich, J. A., Karam, A., Vanzhula, I., Steward, T., & Levinson, C. A. (2019). Intolerance of uncertainty moderates the relationship between high personal standards but not evaluative concerns perfectionism and eating disorder symptoms cross-sectionally and prospectively. Eating Behaviors, 35, 101340. https://doi.org/10.1016/j.eatbeh.2019.101340
Bulik, C. M., Tozzi, F., Anderson, C., Mazzeo, S. E., Aggen, S., & Sullivan, P. F. (2003). The relation between eating disorders and components of perfectionism. The American Journal of Psychiatry, 160, 366–368. https://doi.org/10.1176/appi.ajp.160.2.366
Byrne, M. E., Eichen, D. M., Fitzsimmons-Craft, E. E., Taylor, C. B., & Wilfley, D. E. (2016). Perfectionism, emotion dysregulation, and affective disturbance in relation to clinical impairment in college-age women at high risk for or with eating disorders. Eating behaviors, 23, 131–136. https://doi.org/10.1016/j.eatbeh.2016.09.004
Cain, A. S., Epler, A. J., Steinley, D., & Sher, K. J. (2010). Stability and change in patterns of concerns related to eating, weight, and shape in young adult women: A latent transition analysis. Journal of abnormal psychology, 119(2), 255–267. https://doi.org/10.1037/a0018117
Cella, S., Iannaccone, M., Cipriano, A., & Cotrufo, P. (2020). Risk and maintenance factors for eating disorders: An exploration of multivariate models on clinical and non-clinical populations. In H. Himmerich (Ed.), Weight management (pp. 1–23). IntechOpen. https://doi.org/10.5772/intechopen.91063
Christensen, K. A., & Haynos, A. F. (2020). A theoretical review of interpersonal emotion regulation in eating disorders: Enhancing knowledge by bridging interpersonal and affective dysfunction. Journal of Eating Disorders, 8(1), 1–10. https://doi.org/10.1186/s40337-020-00298-0
Croll, J., Neumark-Sztainer, D., Story, M., & Ireland, M. (2002). Prevalence and risk and protective factors related to disordered eating behaviors among adolescents: Relationship to gender and ethnicity. Journal of Adolescent Health, 31(2), 166–175. https://doi.org/10.1016/S1054-139X(02)00368-3
Dalle Grave, R., & Calugi, S. (2020). Cognitive behavior therapy for adolescents with eating disorders. Guilford Press.
de Lauzon-Guillain, B., Basdevant, A., Romon, M., Karlsson, J., Borys, J. M., & Charles, M. A. (2006). Is restrained eating a risk factor for weight gain in a general population? American Journal of Clinical Nutrition, 83(1), 132–138. https://doi.org/10.1093/ajcn/83.1.132
Donahue, J. M., Reilly, E. E., Anderson, L. M., Scharmer, C., & Anderson, D. A. (2018). Evaluating associations between perfectionism, emotion regulation, and eating disorder symptoms in a mixed-gender sample. The Journal of Nervous and Mental Disease, 206, 900–904. https://doi.org/10.1097/NMD.0000000000000895
Downey, C. A., & Chang, E. C. (2007). Perfectionism and symptoms of eating disturbances in female college students: Considering the role of negative affect and body dissatisfaction. Eating Behaviors, 8(4), 497–503. https://doi.org/10.1016/j.eatbeh.2007.02.002
Downey, C. A., Reinking, K. R., Gibson, J. M., Cloud, J. A., & Chang, E. C. (2014). Perfectionistic cognitions and eating disturbance: Distinct mediational models for males and females. Eating Behaviors, 15(3), 419–426. https://doi.org/10.1016/j.eatbeh.2014.04.020
Egan, S. J., Wade, T. D., & Shafran, R. (2011). Perfectionism as a transdiagnostic process: A clinical review. Clinical Psychology Review, 31(2), 203–212. https://doi.org/10.1016/j.cpr.2010.04.009
Ehring, T., Tuschen-Caffier, B., Schnülle, J., Fischer, S., & Gross, J. J. (2010). Emotion regulation and vulnerability to depression: Spontaneous versus instructed use of emotion suppression and reappraisal. Emotion, 10, 563–572. https://doi.org/10.1037/a0019010
Esposito, R. M., Stoeber, J., Damian, L. E., Alessandri, G., & Lombardo, C. (2019). Eating disorder symptoms and the 2 × 2 model of perfectionism: Mixed perfectionism is the most maladaptive combination. Eating and Weight Disorders, 24(4), 749–755. https://doi.org/10.1007/s40519-017-0438-1
Etkin, A., Prater, K. E., Hoeft, F., Menon, V., & Schatzberg, A. F. (2010). Failure of anterior cingulate activation and connectivity with the amygdala during implicit regulation of emotional processing in generalized anxiety disorder. American Journal of Psychiatry, 167, 545–554. https://doi.org/10.1176/appi.ajp.2009.09070931
Fairburn, C. G., & Beglin, S. J. (2008). Eating Disorder Examination Questionnaire (6.0). In C. G. Fairburn (Ed.), Cognitive behaviour therapy and eating disorders (p. 309). Guilford Press.
Fairburn, C. G., Cooper, Z., & Shafran, R. (2003). Cognitive behaviour therapy for eating disorders: A “transdiagnostic” theory and treatment. Behaviour Research and Therapy, 41, 509–528. https://doi.org/10.1016/S0005-7967(02)00088-8
Forrester-Knauss, C., Perren, S., & Alsaker, F. D. (2012). Does body mass index in childhood predict restraint eating in early adolescence? Appetite, 59(3), 921–926. https://doi.org/10.1016/j.appet.2012.08.026
Francis, L. A., & Susman, E. J. (2009). Self-regulation and rapid weight gain in children from age 3 to 12 years. Archives of Pediatric & Adolescent Medicine, 163, 297–302. https://doi.org/10.1001/archpediatrics.2008.579
Frost, R. O., Marten, P., Lahart, C., & Rosenblate, R. (1990). The dimensions of perfectionism. Cognitive Therapy and Research, 14(5), 449–468. https://doi.org/10.1007/BF01172967
Golden, N. H., Katzman, D. K., Kreipe, R. E., Stevens, S. L., Sawyer, S. M., Rees, J., Nicholls, D., & Rome, E. S. (2003). Eating disorders in adolescents: Position paper of the Society for Adolescent Medicine. Journal of Adolescent Health, 33(6), 496–503. https://doi.org/10.1016/j.jadohealth.2003.08.004
Gratz, K. L., & Roemer, L. (2004). Multidimensional assessment of emotion regulation and dysregulation: Development, factor structure, and initial validation of the difficulties in emotion regulation scale. Journal of Psychopathology and Behavioral Assessment, 26, 41–54. https://doi.org/10.1023/B:JOBA.0000007455.08539.94
Graziano, P. A., Calkins, S. D., & Keane, S. P. (2010). Toddler selfregulation skills predict risk for pediatric obesity. International Journal of Obesity, 34, 633–641. https://doi.org/10.1038/ijo.2009.288
Griffiths, S., Angus, D., Murray, S. B., & Touyz, S. (2014). Unique associations between young adult men’s emotional functioning and their body dissatisfaction and disordered eating. Body Image, 11, 175–178. https://doi.org/10.1016/j.bodyim.2013.12.002
Gross, J. J. (1999). Emotion regulation: Past, present, future. Cognition & Emotion, 13(5), 551–573. https://doi.org/10.1080/026999399379186
Gyurak, A., Gross, J. J., & Etkin, A. (2011). Explicit and implicit emotion regulation: A dual-process framework. Cognition & Emotion, 25, 400–412. https://doi.org/10.1080/02699931.2010.544160
Hamachek, D. E. (1978). Psychodynamics of normal and neurotic perfectionism. Psychology, 15, 27–33.
Harrison, A., Sullivan, S., Tchanturia, K., & Treasure, J. (2010). Emotional functioning in eating disorders: Attentional bias, emotion recognition and emotion regulation. Psychological Medicine, 40, 1887–1897. https://doi.org/10.1017/S0033291710000036
Harrist, A. W., Hubbs-Tait, L., Topham, G. L., Shriver, L. H., & Page, M. C. (2013). Emotion regulation is related to children’s emotional and external eating. Journal of Developmental and Behavioral Pediatrics, 34, 557–565. https://doi.org/10.1097/DBP.0b013e3182a5095f
Hayes, A. F., & Preacher, K. J. (2013). Conditional process modeling: Using structural equation modeling to examine contingent causal processes. In G. R. Hancock, & R. O. Mueller (Eds.), Structural equation modeling: A second course (pp. 219–266). IAP Information Age Publishing.
Hilbert, A., Pike, K. M., Goldschmidt, A. B., Wilfley, D. E., Fairburn, C. G., Dohm, F. A., Walsh, T., & Weissman, R. S. (2014). Risk factors across the eating disorders. Psychiatry research, 220(1–2), 500–506. https://doi.org/10.1016/j.psychres.2014.05.054
Isasi, C. R., Ostrovsky, N. W., & Wills, T. (2013). The association of emotion regulation with lifestyle behaviors in inner-city adolescents. Eating Behaviors, 14, 518–521. https://doi.org/10.1016/j.eatbeh.2013.07.009
Jacobi, C., Hütter, K., & Fittig, E. (2018). Psychosocial risk factors for eating disorders. In W. S. Agras, & A. Robinson (Eds.), The Oxford handbook of eating disorders (pp. 106–125). Oxford University Press. https://doi.org/10.1093/oxfordhb/9780190620998.001.000
JASP. (2020). JASP (Version 0.16) [Computer Software]. The JASP Team.
John, O. O., & Gross, J. J. (2004). Healthy and unhealthy emotion regulation: Personality processes, individual differences, and life span development. Journal of Personality, 72, 1301–1334. https://doi.org/10.1111/j.1467-6494.2004.00298.x
Karlsson, J., Persson, L. O., Sjöström, L., & Sullivan, M. (2000). Psychometric properties and factor structure of the Three-Factor Eating Questionnaire (TFEQ) in obese men and women. Results from the Swedish Obese Subjects (SOS) study. International Journal of Obesity, 24(12), 1715–1725. https://doi.org/10.1038/sj.ijo.0801442
Keel, P. K., & Forney, K. J. (2013). Psychosocial risk factors for eating disorders. International Journal of Eating Disorders, 46(5), 433–439. https://doi.org/10.1002/eat.22094
Kline, R. B. (2005). Methodology in the social sciences. Principles and practice of structural equation modeling. The Guilford Press.
Krug, I., Treasure, J., Anderluh, M., Bellodi, L., Cellini, E., Collier, D., di Bernardo, M., Granero, R., Karwautz, A., Nacmias, B., Penelo, E., Ricca, V., Sorbi, S., Tchanturia, K., Wagner, G., & Fernández-Aranda, F. (2008). Associations of individual and family eating patterns during childhood and early adolescence: A multicentre European study of associated eating disorder factors. British Journal of Nutrition, 101(6), 909–918. https://doi.org/10.1017/S0007114508047752
Kubiak, T., Vögele, C., Siering, M., Schiel, R., & Weber, H. (2008). Daily hassles and emotional eating in obese adolescents under restricted dietary conditions – the role of ruminative thinking. Appetite, 51, 206–209. https://doi.org/10.1016/j.appet.2008.01.008
Lavender, J. M., & Anderson, D. A. (2010). Contribution of emotion regulation difficulties to disordered eating and body dissatisfaction in college men. The International Journal of Eating Disorders, 43, 352–357. https://doi.org/10.1002/eat.20705
Lavender, J. M., Wonderlich, S. A., Engel, S. G., Gordon, K. H., Kaye, W. H., & Mitchell, J. E. (2015). Dimensions of emotion dysregulation in anorexia nervosa and bulimia nervosa: A conceptual review of the empirical literature. Clinical Psychology Review, 40, 111–122. https://doi.org/10.1016/j.cpr.2015.05.010
Leppanen, J., Brown, D., McLinden, H., Williams, S., & Tchanturia, K. (2022). The role of emotion regulation in eating disorders: A network meta-analysis approach. Frontiers in Psychiatry, 13, 793094. https://doi.org/10.3389/fpsyt.2022.793094
Limburg, K., Watson, H. J., Hagger, M. S., & Egan, S. J. (2017). The relationship between perfectionism and psychopathology: A meta-analysis. Journal of Clinical Psychology, 73(10), 1301–1326. https://doi.org/10.1002/jclp.22435
Megalakaki, O., Mouveaux, M., Hubin-Gayte, M., & Wypych, L. (2013). Body image and cognitive restraint are risk factors for obesity in French adolescents. Eating and Weight Disorders, 18(3), 289–295. https://doi.org/10.1007/s40519-013-0027-x
Mennin, D. S., & Farach, F. J. (2007). Emotion and evolving treatments for adult psychopathology. Clinical Psychology: Science and Practice, 14, 329–352. https://doi.org/10.1111/j.1468-2850.2007.00094.x
Meule, A., Richard, A., Schnepper, R., Reichenberger, J., Georgii, C., Naab, S., Voderholzer, U., & Blechert, J. (2021). Emotion regulation and emotional eating in anorexia nervosa and bulimia nervosa. Eating Disorders, 29(2), 175–191. https://doi.org/10.1080/10640266.2019.1642036
Muthen, B., & Kaplan, D. (1985). A comparison of some methodologies for the factor analysis of non-normal Likert variables. British Journal of Mathematical and Statistical Psychology, 38, 171–189.
Nikolić, M., Tokić, A., & Moretić, N. (2018). Trofaktorski upitnik obrazaca hranjenja [The Three-Factor Eating Questionnaire]. In A. Slišković, I. Burić, V. Ćubela Adorić, M. Nikolić, & I. Tucak Junaković (Eds.), Zbirka psihologijskih skala i upitnika - Svezak 9 (str. 39–46). Department of Psychology University of Zadar.
Palmieri, A., Fernandez, K. C., Cariolato, Y., Kleinbub, J. R., Salvatore, S., & Gross, J. J. (2022). Emotion regulation in psychodynamic and cognitive-behavioural therapy: An integrative perspective. Clinical Neuropsychiatry, 19(2), 103–113. https://doi.org/10.36131/cnfioritieditore20220204
Peixoto-Plácido, C., Soares, M. J., Pereira, A. T., & Macedo, A. (2015). Perfectionism and disordered eating in overweight women. Eating Behaviors, 18, 76–80. https://doi.org/10.1016/j.eatbeh.2015.03.009
Pisetsky, E. M., Haynos, A. F., Lavender, J. M., Crow, S. J., & Peterson, C. B. (2017). Associations between emotion regulation difficulties, eating disorder symptoms, non-suicidal self‐injury, and suicide attempts in a heterogeneous eating disorder sample. Comprehensive Psychiatry, 73, 143–150. https://doi.org/10.1016/j.comppsych.2016.11.012
Pokrajac-Bulian, A., Stubbs, L., & Ambrosi-Randić, N. (2004). Različiti aspekti slike tijela i navike hranjenja u adolescenciji [Different aspects of body image and eating habits in adolescence]. Psihologijske teme, 13, 91–104.
Prefit, A. B., Cândea, D. M., & Szentagotai-Tătar, A. (2019). Emotion regulation across eating pathology: A meta-analysis. Appetite, 143, 104438. https://doi.org/10.1016/j.appet.2019.104438
Quick, V. M., & Byrd-Bredbenner, C. (2012). Weight regulation practices of young adults. Predictors of restrictive eating. Appetite, 59(2), 425–430. https://doi.org/10.1016/j.appet.2012.06.004
R Development Core Team (2013). R: A language and environment for statistical computing. R Foundation for Statistical Computing, Vienna, Austria. http://www.R-project.org/
Racine, S. E., & Wildes, J. E. (2013). Emotion dysregulation and symptoms of anorexia nervosa: The unique roles of lack of emotional awareness and impulse control difficulties when upset. The International Journal of Eating Disorders, 46, 713–720. https://doi.org/10.1002/eat.22145
Rivière, J., & Douilliez, C. (2017). Perfectionism, rumination, and gender are related to symptoms of eating disorders: A moderated mediation model. Personality and Individual Differences, 116, 63–68. https://doi.org/10.1016/j.paid.2017.04.041
Rø, Ø., Reas, D. L., & Rosenvinge, J. (2012). The impact of age and BMI on Eating Disorder Examination Questionnaire (EDE-Q) scores in a community sample. Eating behaviors, 13, 158–161. https://doi.org/10.1016/j.eatbeh.2011.12.001
Rohde, P., Stice, E., & Marti, C. N. (2015). Development and predictive effects of eating disorder risk factors during adolescence: Implications for prevention efforts. International Journal of Eating Disorders, 48(2), 187–198. https://doi.org/10.1002/eat.22270
Rottenberg, J., & Gross, J. J. (2003). When emotion goes wrong: Realizing the promise of affective science. Clinical Psychology Science and Practice, 10(2), 227–232. https://doi.org/10.1093/clipsy.bpg012
Rowsell, M., MacDonald, D. E., & Carter, J. C. (2016). Emotion regulation difficulties in anorexia nervosa: Associations with improvements in eating psychopathology. Journal of Eating Disorders, 4, 1–10. https://doi.org/10.1186/s40337-016-0108-0
Ruscitti, C., Rufino, K., Goodwin, N., & Wagner, R. (2016). Difficulties in emotion regulation in patients with eating disorders. Borderline Personality Disorder and Emotion Dysregulation, 3(1), 1–7. https://doi.org/10.1186/s40479-016-0037-1
Sim, L., & Zeman, J. (2006). The contribution of emotion regulation to body dissatisfaction and disordered eating in early adolescent girls. Journal of Youth and Adolescence, 35, 219–228. https://doi.org/10.1007/s10964-005-9003-8
Solmi, M., Radua, J., Stubbs, B., Ricca, V., Moretti, D., Busatta, D., Carvalho, A. F., Dragioti, E., Favaro, A., Monteleone, A. M., Shin, J. I., Fusar-Poli, P., & Castellini, G. (2021). Risk factors for eating disorders: An umbrella review of published meta-analyses. Brazilian Journal of Psychiatry, 43(3), 314–323. https://doi.org/10.1590/1516-4446-2020-1099
Stice, E. (2002). Risk and maintenance factors for eating pathology: A meta-analytic review. Psychological Bulletin, 128(5), 825–848. https://doi.org/10.1037/0033-2909.128.5.825
Striegel-Moore, R. H., Rosselli, F., Perrin, N., DeBar, L., Wilson, G. T., May, A., & Kraemer, H. C. (2009). Gender difference in the prevalence of eating disorder symptoms. International Journal of Eating Disorders, 42(5), 471–474. https://doi.org/10.1002/eat.20625
Tabachnick, B. G., & Fidell, L. S. (2013). Using multivariate statistics. Pearson Education.
Taut, D., Renner, B., & Baban, A. (2012). Reappraise the situation but express your emotions: Impact of emotion regulation strategies on ad libitum food intake. Frontiers in Psychology, 3, 359. https://doi.org/10.3389/fpsyg.2012.00359
Terry-Short, L. A., Owens, R. G., Slade, P. D., & Dewey, M. E. (1995). Positive and negative perfectionism. Personality and Individual Differences, 18, 663–668. https://doi.org/10.1016/0191-8869(94)00192-U
Thompson, R. A. (1994). Emotion regulation: A theme in search of definition. Monographs of the Society for Research in Child Development, 59(2–3), 25–52. https://doi.org/10.2307/1166137
Tingley, D., Yamamoto, T., Hirose, K., Keele, L., Imai, K., Trinh, M., & Wong, W. (2019). Package ‘mediation’. https://imai.princeton.edu/projects/mechanisms.html
Tng, G. Y., & Yang, H. (2021). Interactional effects of multidimensional perfectionism and cognitive emotion regulation strategies on eating disorder symptoms in female college students. Brain Sciences, 11(11), 1374. https://doi.org/10.3390/brainsci11111374
Trompeter, N., Bussey, K., Forbes, M. K., & Mitchison, D. (2021). Emotion dysregulation within the CBT-E model of eating disorders: A narrative review. Cognitive Therapy and Research, 45(6), 1021–1036. https://doi.org/10.1007/s10608-021-10225-5
Vandewalle, J., Moens, E., & Braet, C. (2014). Comprehending emotional eating in obese youngsters: The role of parental rejection and emotion regulation. International Journal of Obesity, 38, 525–530. https://doi.org/10.1038/ijo.2013.233
Vieira, A. I., Moreira, C. S., Rodrigues, T. F., Brandão, I., Timóteo, S., Nunes, P., & Gonçalves, S. (2021). Nonsuicidal self-injury, difficulties in emotion regulation, negative urgency, and childhood invalidation: A study with outpatients with eating disorders. Journal of Clinical Psychology, 77(3), 607–628. https://doi.org/10.1002/jclp.23038
Voderholzer, U., Cuntz, U., & Schlegl, S. (2012). Eating disorders: State of the art research and future challenges. Der Nervenarzt, 83(11), 1458–1467. https://doi.org/10.1007/s00115-012-3686-3
Weinbach, N., Sher, H., & Bohon, C. (2018). Differences in emotion regulation difficulties across types of eating disorders during adolescence. Journal of Abnormal Child Psychology, 46(6), 1351–1358. https://doi.org/10.1007/s10802-017-0365-7
White, H. J., Haycraft, E., Goodwin, H., & Meyer, C. (2014). Eating Disorder Examination Questionnaire: Factor structure for adolescent girls and boys. International Journal of Eating Disorders, 47(1), 99–104. https://doi.org/10.1002/eat.22199
Whiteside, U., Chen, E., Neighbors, C., Hunter, D., Lo, T., & Larimer, M. (2007). Difficulties regulating emotions: Do binge eaters have fewer strategies to modulate and tolerate negative affect? Eating Behaviors, 8, 162–169. https://doi.org/10.1016/j.eatbeh.2006.04.001
Yucel, B., Polat, A., Ikiz, T., Dusgor, B. P., Yavuz, A. E., & Berk, O. S. (2011). The Turkish version of the Eating Disorder Examination Questionnaire: Reliability and validity in adolescents. European Eating Disorders Review, 19(6), 509–511. https://doi.org/10.1002/erv.1104
Zambrowicz, R., Schebendach, J., Sysko, R., Mayer, L. E., Walsh, B. T., & Steinglass, J. E. (2019). Relationship between three factor eating questionnaire-restraint subscale and food intake. International Journal of Eating Disorders, 52(3), 255–260. https://doi.org/10.1002/eat.23014
Zehr, J. L., Culbert, K. M., Sisk, C. L., & Klump, K. L. (2007). An association of early puberty with disordered eating and anxiety in a population of undergraduate women and men. Hormones and Behavior, 52, 427–435. https://doi.org/10.1016/j.yhbeh.2007.06.005
Zeman, J., Cassano, M., Perry-Parrish, C., & Stegall, S. (2006). Emotion regulation in children and adolescents. Journal of Developmental and Behavioral Pediatrics, 27, 155–168. https://doi.org/10.1097/00004703-200604000-00014
Acknowledgements
This study was supported by the University of Rijeka grant as a part of research project Risk and protective factors in the development of excessive weight and obesity in adolescence (uniri-drustv-18-63).
Author information
Authors and Affiliations
Corresponding authors
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Mohorić, T., Pokrajac-Bulian, A., Anić, P. et al. Emotion regulation, perfectionism, and eating disorder symptoms in adolescents: the mediating role of cognitive eating patterns. Curr Psychol 42, 28505–28516 (2023). https://doi.org/10.1007/s12144-022-03824-2
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12144-022-03824-2