Abstract
Cyberchondria refers to excessive and repeated online health-related searching, which is associated with increased distress and anxiety. The Cyberchondria Severity Scale (CSS) is the most widely used measure for assessment of cyberchondria, and its shortened version (CSS-12) has recently been developed. The aim of the present study was to develop the Spanish version of the CSS-12 and test its psychometric properties. A community sample of 432 Spanish-speaking adults (67.6% women; mean age = 36.00 ± 15.22 years) completed the Spanish translation of CSS-12 along with measures of health anxiety, obsessive-compulsive, anxiety and depressive symptoms. The Spanish version of the CSS-12 comprises a general cyberchondria factor and four specific factors (‘excessiveness’, ‘compulsion’, ‘distress’, and ‘reassurance’). Multi-group confirmatory factor analysis indicated measurement invariance across gender groups. Internal consistency values for the total score and subscales were good to excellent. The CSS-12 showed strong correlations with health anxiety, and moderate to low correlations with anxiety, obsessive-compulsive and depressive symptoms, supporting the convergent and divergent validity of the CSS-12, respectively. In conclusion, these results show that the CSS-12 is a valid and reliable tool for measuring cyberchondria in both genders in the general Spanish population.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
The Internet and digital tools have had a great impact on how individuals access health information. In this sense, the Internet has gained ground over traditional sources of health information, such as medical books and encyclopedias or consults with physicians. In part because searching for medical information on the Internet has many advantages, the Internet is considered a low-cost tool for accessing information quickly, easily, and anonymously. These online searches can also empower individuals, allowing them to have more control over their personal health and their health care decisions (McManus et al., 2014; Starcevic et al., 2020). In some cases, however, individuals may feel distress or anxiety during or after online health research (OHR). This exacerbation of anxiety or distress about health because of excessive and repetitive health-related searches on the Internet is known as cyberchondria (Starcevic & Berle, 2013). Although the term “cyberchondria” has been criticized as potentially misleading and otherwise pejorative or stigmatizing because of its link with the concept of hypochondriasis (e.g., Brown, Skelly, & Chew-Graham, 2020), it has been widely used and generally accepted in the scientific literature (Starcevic, 2020).
A recently proposed “working definition” of cyberchondria includes excessive online health searches that are compulsive, serve the purpose of seeking reassurance, worsen anxiety or distress, and continue despite their negative consequences (Vismara et al., 2020). The concept of cyberchondria has been related to different disorders and symptoms (Starcevic et al., 2019). In this sense, recent studies indicate that, although cyberchondria and health anxiety may share similar symptom presentations (e.g., an excessive and/or repetitive pattern of OHR may also be present in individuals with health anxiety), they can also reflect separate concepts (Fergus & Russell, 2016; Mathes et al., 2018; Starcevic et al., 2019). Likewise, cyberchondria has also been associated with obsessive-compulsive symptoms, given the repetitive and unwanted nature of online health-related searches (Fergus & Russell, 2016; Norr et al., 2015b; Starcevic et al., 2019).
The Cyberchondria Severity Scale (CSS; McElroy & Shevlin, 2014) is a well-established and most commonly used measure of cyberchondria. McElroy and Shelvin developed the CSS based on the definition of cyberchondria as a multidimensional construct that reflects both anxiety and an element of compulsivity. Furthermore, the CSS was developed to measure the distress level associated with cyberchondria symptoms.
The CSS consists of 33 items, which comprise five key domains (Compulsion, Distress, Excessiveness, Reassurance, and Mistrust of Medical Professionals) assessed on separate subscales and derived from exploratory factor analysis. As described by McElroy & Shevlin (2014), the ‘Compulsion’ factor refers to interference of OHR with different aspects of a person’s life (e.g., Researching symptoms or perceived medical conditions online interrupts my work [e.g., writing emails, working on word documents or spreadsheets]). The ‘Distress’ factor refers to the negative emotional responses that result from OHR (e.g., I find it hard stop worrying about symptoms or perceived medical conditions that I have researched online). The ‘Excessiveness’ factor denotes the repetitive and time-consuming nature of OHR (e.g., I read different web pages about the same perceived condition). The ‘Reassurance’ factor reflects the extent to which OHR leads a person to consult with a medical professional (e.g., Discuss my online medical findings with my GP/health professional reassures me). Finally, the ‘Mistrust of Medical Professionals’ factor refers to the conflict that arises when the professional diagnosis does not match the individual’s self-diagnosis from OHR (e.g., I take the opinion of my GP/medical professional more seriously than my online medical research [reverse-scored]).
Several studies have tested the factor structure and psychometric properties of the original English version of the CSS (Fergus, 2014; Norr et al., 2015a), as well as the CSS translations into languages such as German (Barke et al., 2016), Turkish (Selvi et al., 2018; Uzun & Zencir, 2018), Polish (Bajcar et al., 2019) and Portuguese (Silva et al., 2016).
Although the original version of the CSS presents good psychometric properties, it has been suggested that it could be improved by shortening it and removing the items of the Mistrust of Medical Professionals factor because of its theoretical ambiguity (e.g., Barke et al., 2016; Fergus, 2014; Norr et al., 2015a). Several proposals have been made in this regard. Fergus (2014) observed that a second-order CSS model including all the CSS items fit the data well once the Mistrust of Medical Professionals factor was excluded and concluded that this factor did not measure the same construct as the other CSS factors. Similarly, Norr et al. (2015a) proposed a model of cyberchondria that comprised a separate Mistrust of Medical Professionals factor and a bifactorial model consisting of a General Cyberchondria factor and specific orthogonal factors (Compulsion, Distress, Excessiveness, and Reassurance). The first attempt to reduce the CSS was carried out by Barke et al. (2016) as part of the German validation of the CSS. They proposed a short version with 15 items (CSS-15), which retained the good psychometric properties of the original version. The CSS-15 included the original five CSS subscales to assess the same domains of cyberchondria. In contrast to CSS-15, Fergus and Spada (2018) proposed a 12-item version of the CSS that excludes items of the Mistrust of Medical Professionals factor. This scale presented better internal consistency and convergent validity than the CSS-15 (Fergus & Spada, 2018).
The creators of the CSS also developed a 12-item version (CSS-12), excluding the Mistrust of Medical Professionals subscale, and selecting three items from each of the remaining four subscales (McElroy et al., 2019). The three items of each factor were chosen based on the following criteria: factor loadings, endorsement rates, impact on subscale internal consistency, length, and content. An analysis of the factor structure of these 12 items showed that the bifactorial model provided the best fit for the data, as Norr et al. (2015a) concluded after analyzing the full scale. Thus, McElroy et al. (2019) proposed that the structure of the CSS-12 consisted of a general and specific (orthogonal) cyberchondria factors (compulsion, distress, excessiveness, reassurance). The CSS-12 demonstrated good psychometric properties, including internal consistency and convergent validity.
Besides the original validation study by McElroy et al. (2019), only the Italian version of the CSS-12 has been validated (Soraci et al., 2020). This version of the CSS-12 has demonstrated good psychometric properties, although the authors only tested a unidimensional model, without testing the originally proposed bifactorial model of the CSS-12.
In summary, the CSS has presented with a number of issues. First, several abbreviated versions of the CSS have been proposed, and they all have different properties. However, the CSS-12 of McElroy et al. seems to be the most appropriate because the criteria used to reduce the number of items appear justified and most comprehensive. Second, there are different views about the most appropriate factor structure for the CSS (e.g., four factors, four first-order factors and one second-order factor, bifactor, etc.), but no study has compared the fit of all of these different factor structure proposals. In other words, there is a need to ascertain the most appropriate factor structure for the scale. Third, previous validation studies of the CSS, including both studies of the full version and those of the shorter versions, did not assess whether the structure of the instrument remained unchanged across genders. This is important because gender differences in the related construct of health anxiety have been observed (Bleichhardt & Hiller, 2007; Clarke et al., 2008; Fink et al., 2004), although no gender differences have been found with regard to searching for health information on the Internet (e.g., Berle et al., 2020; Muse et al., 2012). Furthermore, to the best of our knowledge, no version of the CSS has been translated into Spanish, limiting assessment of cyberchondria in the Spanish-speaking countries/communities.
Accordingly, the specific goals of the current study are as follows: (a) translating the CSS-12 from English to Spanish; (b) establishing the psychometric properties (factor structure, internal consistency, convergent and divergent validity) of the Spanish version of the CSS-12; and (c) analyzing measurement invariance according to gender (configural, metric, structural, and error variance invariance).
Method
Participants and Procedure
Data were collected from a convenience sample between 2019 and 2020. Participants were recruited from the general community and university setting by snowball sampling, after providing relevant information via multiple channels, including face-to-face classes and social media, and inviting participants to share a link to the survey with their acquaintances.
Participants completed all the measures through a secure survey platform (Limesurvey) and gave informed consent for their participation in this research. Approval for the study was obtained from the University of Valencia Human Research Ethics Committee.
The inclusion criteria for participation in the study were as follows: 1) age between 18 and 65 years, and 2) absence of any mental disorder or significant medical illness in the previous year due to a possible effect of these conditions on the pattern of online health searches.
Data initially obtained from the online platform were screened to exclude duplicates, inconsistent or obviously erroneous responses (e.g., current age of >100 years). The survey was completed by 459 individuals, but 27 individuals reported a current, diagnosed medical illness requiring treatment and were excluded from the analyses. Therefore, the final sample comprised 432 non-clinical community adults (67.6% females; 32.4% males), ranging in age from 18 to 63 years (Mean = 36.00; SD = 15.22). Most participants were single (49.8%), reported a medium socio-economic status (62.5%), and had a University-level education (68.1%).
Instruments
We administered four self-report instruments to assess cyberchondria, health anxiety, obsessive and compulsive symptoms and symptoms of depression and anxiety: CSS-12, Short Health Anxiety Inventory (SHAI), Obsessive-Compulsive Inventory-Revised (OCI-R), and Depression Anxiety Stress Scale 21 (DASS-21).
Cyberchondria
Severity of cyberchondria was assessed using the Short Form of the Cyberchondria Severity Scale (CSS-12; McElroy et al., 2019). It is a 12-item self-report instrument, with responses recorded on a 5-point scale (from 1 = ‘never’ to 5 = ‘always’) and total scores ranging between 12 and 60. The CSS-12 has demonstrated an appropriate reliability (Cronbach’s α for its subscales ranging between .73 and .90), as well as convergent and divergent validity (McElroy et al., 2019). Psychometric properties of the Spanish version of the CSS-12 are reported in the Results section.
The adaptation of the CSS-12 into Spanish was conducted according to the procedure described by Beaton et al. (2000). First, two members of the research team with experience in translation/validation of questionnaires and expertise in the area of health behaviors (SA and GGS) independently translated the scale into Spanish. These two versions were subsequently compared and adjusted to agree on a preliminary Spanish version of the scale. This preliminary version was then back-translated into English by a bilingual professional translator. There were minimal discrepancies that were discussed and considered until optimal agreement was reached. The final version is included in the Supplementary Information 2.
Health Anxiety
This construct was assessed using the Short Health Anxiety Inventory (SHAI; Salkovskis et al., 2002; Spanish version: Arnáez et al., 2019). The SHAI is an 18-item self-report measure that assesses health anxiety (i.e., concern for health, monitoring of changes in bodily sensations, and fear of the consequences of suffering from a serious illness) independently of actual physical health status. It is composed of two subscales: ‘Likelihood of becoming ill’ and ‘Negative consequences of illnesses’. Responses on each item are rated on a 4-point Likert scale. The SHAI has demonstrated good reliability and validity in both clinical and non-clinical samples (Arnáez et al., 2019; Salkovskis et al., 2002). In the present study, the internal consistency for the ‘total score’ (α = .90; ω = .90) and the ‘Likelihood of becoming ill’ subscale (α = .90; ω = .90) was excellent, and acceptable for the ‘Negative consequences of illness’ subscale (α = .67; ω = .70).
Obsessive and Compulsive Symptoms
The Obsessive-Compulsive Inventory-Revised (OCI-R; Foa et al., 2002; Spanish version: Fullana et al., 2005) is an 18-item self-report questionnaire that assesses distress associated with obsessions and compulsions, using a 5-point Likert scale. The OCI-R provides a total score (ranging from 0 to 72) and scores on six subscales: ‘washing’, ‘checking’, ‘neutralizing’, ‘obsessing’, ‘ordering’, and ‘hoarding’. The OCI-R has demonstrated excellent psychometric properties in the original (Foa et al., 2002) and Spanish versions (Belloch et al., 2013; Fullana et al., 2005). Internal consistency in the present study was excellent (α = .90; ω = .90).
Symptoms of Depression and Anxiety
The Depression Anxiety Stress Scale-21 (DASS-21; Lovibond & Lovibond, 1995; Spanish version: Daza et al., 2002) is a 21-item self-report questionnaire that assesses symptoms of emotional distress. The DASS-21 comprises three subscales: (a) ‘depression’, measuring symptoms typically associated with dysphoric mood; (b) ‘anxiety’, assessing symptoms of physical arousal, panic attack, and fear; and (c) ‘stress’, measuring symptoms such as tension, irritability, or the tendency to overreact to stressful events. Each subscale is composed of seven items, and respondents rate each item on a 4-point Likert scale. The DASS-21 has shown high internal reliability and validity in both clinical (Osman et al., 2012) and non-clinical samples (Henry & Crawford, 2005). The Spanish version has also demonstrated strong internal consistency and good convergent and discriminant validity (Daza et al., 2002). In the current study, only the anxiety and depression subscales were used; their internal consistency was excellent (α = .90, ω = .91 for anxiety and α = .93, ω = .93 for depression).
Statistical Analyses
The online platform employed to collect the data required participants to answer all the questions before proceeding to the next survey section, in order to avoid missing data. In a first step, descriptive statistics concerning sociodemographic characteristics were calculated to compile a profile of the sample using the SPSS statistical package (version 24.0). Then, Confirmatory Factor Analyses (CFAs) were conducted in order to check the goodness of fit of different factorial solutions for the CSS-12. The software used to perform these analyses was the EQS. 6.4 (Bentler, 2006). Non-normal distribution of categorical data was addressed by applying robust estimation methods (robust Maximum Likelihood, ML) (Finney & DiStefano, 2013). Goodness of fit for the CFA models was assessed through the following indices: The Root Mean Square Error of Approximation (RMSEA), the Comparative and Incremental Fit Indexes (CFI and IFI, respectively), and the Standardized Root Mean Square Residual (SRMR). Satorra-Bentler Chi-Square (χ2), general model significance (p), and Relative Chi-Square (χ2/df) are also reported. Excellent model fit was considered when χ2 was not significant (p > .05), χ2/df was between 1 and 2, the CFI and the IFI were ≥ .95, the RMSEA ≤ .05, and the SRMR ≤ .05 (Bagozzi & Yi, 2011; Schermelleh-Engel & Müller, 2003). Using less restrictive criteria, values between 2 and 3 for χ2/df, ≥ .90 for the CFI and the IFI, ≤ .08 for the RMSEA, and ≤ .10 for the SRMR were considered acceptable (Hooper et al., 2008).
To assess whether the factor structure of the CSS-12 was valid in both males and females, multi-group CFAs according to gender were carried out. Specifically, we tested four levels of measurement invariance: 1) configural (testing whether items load on the same factor across groups), 2) metric (testing whether item factorial loadings are equal across groups); 3) scalar (testing whether item intercepts are equal across groups) and 4) error variance invariance (testing whether item measurement errors are equal across groups). The adequacy of the increasingly constrained models was assessed through the difference between pairs of nested models (△) in the RMSEA, CFI and SRMR. A change ≥ .01 in the CFI, ≥ .015 in the RMSEA, and ≥ .03 in the SRMR indicates a significant decrease in the model fit when testing for measurement invariance (Chen, 2007).
Internal consistency was assessed through the Ordinal Cronbach’s alpha (α) and the McDonald’s Omega (ω) (including both total and hierarchical ω). These indices were calculated using the R package “userfriendlyscience” (Peters, 2014). According to the criterion proposed by Hunsley & Mash (2008), an internal consistency between .70 and .79 was considered appropriate, between .80 and .89 good and ≥ .90 excellent.
To test convergent validity of the CSS-12, we explored the relationships between cyberchondria and health anxiety; and in order to test the divergent validity we analyzed associations between cyberchondria and obsessive-compulsive symptoms, and anxiety and depressive symptoms. To address this aim, we calculated Pearson zero-order correlations between the CSS-12, the SHAI, the OCI-R, and the DASS-21. Finally, in order to test the robustness of these associations and to identify variables that predict cyberchondria, a hierarchical linear regression analysis was performed using the stepwise method (for a detailed description of the method, see Hair et al. (2010)).
Results
Structural Analysis and Measurement Invariance According to Gender
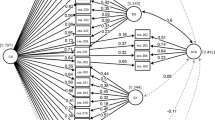
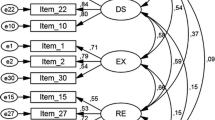
To assess whether the factor structure proposed by McElroy et al. (2019) was equivalent for the Spanish version of the CSS-12, we tested the adequacy of four factorial solutions: (a) the one-factor solution (i.e., all the items under a 1st order factor), (b) the four correlated 1st order-factor solution; (c) the bifactor model (i.e., a general cyberchondria factor together with four specific factors); and (d) a 2nd order model (i.e., grouping the four first-order factors under a second-order factor that explained the shared variance). Goodness-of-fit indices from all of the tested models are presented in Table 1.
As Table 1 shows, the models with the most satisfactory fit indices were the bifactor model and the 2nd order model. Both models were almost indistinguishable in most of the goodness-of-fit indices assessed. As both models may be considered nested (Yung et al., 1999), a suitable approach to estimate their competing adequacy is to compute the difference in the χ2 test (△χ2). Given the non-normal distribution of our data and the use of a robust method for the estimation of our CFA models, the △χ2 was calculated by using the formula for the “scaled difference χ2 test” (i.e., a more complex approach that allows testing of significance of χ2 changes in nested models not following a classical chi-square distribution) (Bryant & Satorra, 2012). When doing so, we observed a significant worsening of χ2 in the 2nd order model compared to the bifactor model (scaled △χ2 = 24.28; df = 7; p < .01), indicating the statistical superiority of the latter over the former. In the bifactor model, the level of significance of the Satorra–Bentler χ2 did not exceed the .05 value necessary to consider it a satisfactory fit for the model. Nevertheless, it has been shown that this statistic is highly conditioned by sample size (Jöreskog & Sörbom, 1993; Markland, 2007). For this reason, it may be more appropriate to use other indices considered less sensitive to sample size to assess the adequacy of the factorial solutions. In this sense, the value of the relative χ2 (χ2/df) was 2.86, with acceptable fit considered to be values below 3. The RMSEA was .066 which is lower than .08 (a threshold deemed to be indicative of an acceptable-fitting model). The SRMR was below the .05 value required by the strictest criteria to consider a perfect-fit model. Finally, the CFI and the IFI reached a value of .93, which is very close to the cut-off point established to consider it an excellent fit to the model. This model is comprised of a general cyberchondria factor (range of scores 12-60) and four specific factors (three items per factor; range of scores 3-15): ‘excessiveness’, ‘compulsion’, ‘distress’, and ‘reassurance’. The resulting bifactorial model is presented in Fig. 1.
To test measurement invariance of the CSS-12 according to gender, we conducted a series of model comparisons with multi-group CFA. As displayed in Table 2, gender configural invariance of the CSS-12 was supported (RMSEA = .040; CFI = .977; IFI = .979; SRMR = .040), and we subsequently estimated models with increasing levels of constraints to test higher levels of invariance. Regarding metric invariance, changes in the RMSEA, CFI, and SRMR did not show a significant worsening in the model fit for gender invariance (△RMSEA = .011; △CFI = .010; △SRMR = .023). Similarly, model fit did not significantly decrease when error invariance according to gender was tested (△RMSEA = .005; △CFI = .005; △SRMR = .006). However, when scalar invariance according to gender was tested, △CFI (.044) and △SRMR (.042) suggested the presence of differences at this level of measurement according to the gender.
Internal Consistency
Internal consistency for the general and specific cyberchondria scales ranges from .83 to .93 (Table 3). A slight difference was only observed between ordinal Cronbach’s alpha (α) and McDonald’s Omega (ω) in the reassurance subscale (α = .83 and ω = .84). Convergence between both indices was considered a good indicator of the scale internal consistency under different conditions (Zinbarg et al., 2005).
Convergent and Divergent Validity
Table 3 also shows the Pearson zero-order correlations between study measures. Supporting convergent validity of the CSS-12, correlations between the general cyberchondria factor and health anxiety symptoms as measured by the total score on the Short Health Anxiety Inventory (SHAI) were positive and significant (r between .42-.60). As for divergent validity, correlations between the CSS-12 and the Obsessive-Compulsive Inventory-Revised (OCI-R) (r between .16-.24) were positive, but weak. Similarly, the correlations between the CSS-12 and the subscales of ‘anxiety’ (r between .25-.39) and ‘depression’ (r between .21-.30) were positive, but moderate.
Finally, a multiple linear regression was calculated to predict cyberchondria (CSS-12) based on health anxiety symptoms (SHAI), anxiety and depressive symptoms (DASS-21), and obsessive-compulsive symptoms (OCI-R). A significant regression equation was found (F (4, 427) = 64.9320, p < .001), with an R2 of .378. The results of the multiple linear regression analysis revealed that depressive (β = .00, t = .043, p = .966) and OCD (β = .02, t = .466, p = .641) symptoms were not statistically significant predictors of the model, whereas health anxiety symptoms (β = .54, t = 12.678, p < .001) and anxiety symptoms (β = .13, t = 2.341, p < .001) significantly predicted cyberchondria.
Discussion
The aim of this study was threefold: (a) to translate the CSS-12 (McElroy et al., 2019) into Spanish and validate it in a Spanish-speaking adult population; (b) to further analyze the factor structure of the scale by comparing the competing factorial solutions; and (c) to explore the applicability of the resulting factorial solution in both males and females (i.e., gender invariance). In this sense, the main conclusion derived from this study is that the Spanish version of CSS-12 is a reliable and valid measurement tool for assessment of cyberchondria in both genders, supporting the original bifactor model.
We examined four models to determine the best-fitting factor structure of the CSS-12 (i.e., one-factor, four-factor, bifactor, second-order). The bifactor model had the best fit to the data, as proposed by McElroy et al. (2019) for the original CSS-12 and Norr et al. (2015a) for the full 33-item version of the scale. According to this factorial solution, the scale measures a unitary construct (i.e., a general cyberchondria factor), and contains meaningful specific dimensions (i.e., excessiveness, compulsion, distress, and reassurance factors) assessed via subscales. These dimensions are of relevance as they allow us to compare results with previous studies and analyze in detail various characteristics of the cyberchondria construct, which provides important information. However, as recommended by McElroy et al. (2019) and Norr et al. (2015a), the subscales should not be used in isolation due to a high degree of covariance with the general factor.
Regarding psychometric properties, this study demonstrates that the Spanish version of the CSS-12 is a reliable and valid measure of cyberchondria. Cronbach’s α and ω of the total score was .93, while these values for the CSS-12 subscales ranged from .83 to. 88. These values are similar to those reported in the original CSS-12 validation study (total score: α = 90; subscales: α = .73 to .87) (McElroy et al., 2019) and for the Italian version of the CSS-12 (total score: α = .93; ω = .90) (Soraci et al., 2020), while also being consistent with internal consistency values reported for the full 33-item measure (i.e., Bajcar et al., 2019; Barke et al., 2016; Fergus, 2014; Norr et al., 2015a; McElroy & Shevlin, 2014; Selvi et al., 2018; Uzun & Zencir, 2018).
Our results support convergent and divergent validity of the CSS-12. With regard to convergent validity, the CSS-12 total score and subscale scores showed moderate to high correlations with an established measure of health anxiety (r from .42 to .60). Furthermore, health anxiety significantly predicted cyberchondria (total score). This strong relationship between cyberchondria and health anxiety is consistent with findings of the previous studies (e.g., Fergus & Russell, 2016; McElroy & Shevlin, 2014; McElroy et al., 2019; McMullan et al., 2019; Norr et al., 2015a; Starcevic et al., 2019). Therefore, individuals with health anxiety may be particularly prone to experiencing counterproductive outcomes from online health information seeking. However, although cyberchondria and health anxiety are closely related, they have also been shown to be distinct (Fergus & Russell, 2016; Mathes et al., 2018; Starcevic et al., 2019).
The divergent validity of the CSS-12 was supported to the extent that OCD and depression, and to a lesser extent general anxiety, are considered conceptually distinct from cyberchondria. Specifically, the CSS-12 showed significant and positive correlations with anxiety (r from .25 to .39), depressive (r from .21 to .30) and OCD (r from .16 to .24) symptoms, although the correlation sizes were moderate to weak. These findings are somewhat in agreement with those reported by previous research. Thus, in contrast to the levels of health anxiety, levels of general anxiety were not found to predict the severity of cyberchondria (Arsenakis et al., 2021). Several studies showed a significant, but relatively weak relationship between depressive symptoms and cyberchondria (Barke et al., 2016; McElroy & Shevlin, 2014; Starcevic et al., 2019; Uzun & Zencir, 2018). A network analysis reported a significant, but weak relationship between OCD symptoms and cyberchondria (Starcevic et al., 2019), while other research reported this relationship to be weaker than that between health anxiety and cyberchondria (e.g., Fergus, 2014).
With regard to the CSS-12 subscales, the Distress subscale showed the strongest associations with psychopathological measures (obsessive-compulsive, anxiety and depressive symptoms) compared to other CSS-12 subscales. This finding may have implications for further refinement of the construct of cyberchondria, given that Distress subscale assesses negative emotional responses to OHR.
During the validation process of the Spanish version of the CSS-12, a particular attention was paid to its applicability to men and women because this issue has been neglected in research. Findings show that the factor structure of the CSS-12 (i.e., the bifactor structure) is equally applicable to both men and women (configural invariance). In addition, the saturation of each item in each factor (metric invariance) is also equivalent for both genders. However, the latent mean scores in men and women on the factors and items of the CSS-12 were different (scalar invariance). At a practical level, these findings suggest that the “factor structure” of the CSS-12 (i.e., the distribution of the items among the different subscales and the factorial loadings of the items on their corresponding subscale) is comparable in men and women. However, the clinical significance (or contribution) of certain items in the determination of cyberchondria differs according to gender. In this sense, increased scores in certain CSS items are related to increased levels of cyberchondria in one gender but not the other. Thus, gender differences in item contribution to the measurement of cyberchondria warrants further research.
Limitations of the present study should be mentioned. First, due to the scarcity of measures in Spanish to assess cyberchondria, we did not use any other instruments that assess the same construct to further test the concurrent validity. Second, we evaluated gender only via two categories (male/female). This categorization does not represent the wide variety of gender expressions; for this reason, we encourage the use of measures that assess both cisgender and transgender identities (Tate, Ledbetter, & Youssef, 2013). Third, individuals with a serious or chronic illness were excluded from the sample, which could have affected the representativeness of the sample. However, we did it as we consider that the pattern of internet searches and anxiety associated could be different in those individuals and influenced by their diagnosis.
Despite the limitations, this is the first study to report solid reliability and validity of the Spanish translation of the CSS-12, while supporting its bifactor model and use in both genders. We believe that this is an important contribution both in terms of making the most widely used cyberchondria instrument available to Spanish-speaking individuals around the globe and better understanding of the construct of cyberchondria itself.
Data Availability
The datasets generated during and/or analysed during the current study are available in the RODERIC repository: https://hdl.handle.net/10550/82392
References
Arnáez, S., García-Soriano, G., López-Santiago, J., & Belloch, A. (2019). The Spanish validation of the short health anxiety inventory: Psychometric properties and clinical utility. International Journal of Clinical and Health Psychology, 19(3), 251–260. https://doi.org/10.1016/j.ijchp.2019.05.003
Arsenakis, S., Chatton, A., Penzenstadler, L., Billieux, J., Berle, D., Starcevic, V., Viswasam, K., & Khazaal, Y. (2021). Unveiling the relationships between cyberchondria and psychopathological symptoms. Journal of Psychiatric Research, 143, 254–261. https://doi.org/10.1016/j.jpsychires.2021.09.014
Bagozzi, R. P., & Yi, Y. (2011). Specification, evaluation, and interpretation of structural equation models. Journal of the Academy of Marketing Science, 40, 8–34. https://doi.org/10.1007/s11747-011-0278-x
Bajcar, B., Babiak, J., & Olchowska-Kotala, A. (2019). Cyberchondria and its measurement. The polish adaptation and psychometric properties of the Cyberchondria severity scale CSS-PL. polish. Psychiatry, 53(1), 49–60. https://doi.org/10.12740/PP/81799
Barke, A., Bleichhardt, G., Rief, W., & Doering, B. K. (2016). The Cyberchondria severity scale (CSS): German validation and development of a short form. International Journal of Behavioral Medicine, 23(5), 595–605. https://doi.org/10.1007/s12529-016-9549-8
Beaton, D. E., Bombardier, C., Guillemin, F., & Ferraz, M. B. (2000). Guidelines for the process of cross-cultural adaptation of self-report measures. Spine, 25(24), 3186–3191.
Belloch, A., Roncero, M., García-Soriano, G., Carrió, C., Cabedo, E., & Fernández-Álvarez, H. (2013). The Spanish version of the obsessive-compulsive inventory-revised (OCI-R): Reliability, validity, diagnostic accuracy, and sensitivity to treatment effects in clinical samples. Journal of Obsessive-Compulsive and Related Disorders, 2(3), 249–256. https://doi.org/10.1016/j.jocrd.2013.05.001
Bentler, P. M. (2006). EQS structural equations program manual. Multivariate Software.
Berle, D., Starcevic, V., Khazaal, Y., Viswasam, K., Hede, V., & McMullan, R. D. (2020). Relationships between online health information seeking and psychopathology. General Hospital Psychiatry, 62, 96–97. https://doi.org/10.1016/j.genhosppsych.2019.04.006
Bleichhardt, G., & Hiller, W. (2007). Hypochondriasis and health anxiety in the German population. British Journal of Health Psychology, 12(4), 511–523. https://doi.org/10.1348/135910706X146034
Brown, R. J., Skelly, N., & Chew-Graham, C. A. (2020). Online health research and health anxiety: A systematic review and conceptual integration. Clinical Psychology: Science and Practice, 27(2), e12299. https://doi.org/10.1111/cpsp.12299
Bryant, F. B., & Satorra, A. (2012). Principles and practice of scaled difference chi-square testing. Structural Equation Modeling: A Multidisciplinary Journal, 19(3), 372–398. https://doi.org/10.1080/10705511.2012.687671
Chen, F. F. (2007). Sensitivity of goodness of fit indexes to lack of measurement invariance. Structural Equation Modeling: A Multidisciplinary Journal, 14, 464–504. https://doi.org/10.1080/10705510701301834
Clarke, D. M., Piterman, L., Byrne, C. J., & Austin, D. W. (2008). Somatic symptoms, hypochondriasis and psychological distress: A study of somatisation in Australian general practice. Medical Journal of Australia, 189(10), 560–564. https://doi.org/10.5694/j.1326-5377.2008.tb02180.x
Daza, P., Novy, D. M., Stanley, M. A., & Averill, P. (2002). The depression anxiety stress scale-21: Spanish translation and validation with a Hispanic sample. Journal of Psychopathology and Behavioral Assessment, 24(3), 195–205. https://doi.org/10.1023/A:1016014818163
Fergus, T. A. (2014). The Cyberchondria severity scale (CSS): An examination of structure and relations with health anxiety in a community sample. Journal of Anxiety Disorders, 28(6), 504–510. https://doi.org/10.1016/j.janxdis.2014.05.006
Fergus, T. A., & Russell, L. H. (2016). Does cyberchondria overlap with health anxiety and obsessive–compulsive symptoms? An examination of latent structure and scale interrelations. Journal of Anxiety Disorders, 38, 88–94. https://doi.org/10.1016/j.janxdis.2016.01.009
Fergus, T. A., & Spada, M. M. (2018). Moving toward a metacognitive conceptualization of cyberchondria: Examining the contribution of metacognitive beliefs, beliefs about rituals, and stop signals. Journal of Anxiety Disorders, 60, 11–19. https://doi.org/10.1016/j.janxdis.2018.09.003
Fink, P., Hansen, M. S., & Oxhoj, M. L. (2004). The prevalence of somatoform disorders among internal medical inpatients. Journal of Psychosomatic Research, 56(4), 413–418. https://doi.org/10.1016/S0022-3999(03)00624-X
Finney, S. J., & DiStefano, C. (2013). Nonnormal and categorical data in structural equation models. In Structural equation modeling: A second course (2nd ed.). Information Age Publishing.
Foa, E., Huppert, J., Leiberg, S., Langner, R., Kichic, R., Hajcak, G., & Salkovskis, P. (2002). The obsessive-compulsive inventory: Development and validation of a short version. Psychological Assessment, 14(4), 485–496. https://doi.org/10.1037/1040-3590.14.4.485
Fullana, M. A., Tortella, M., Caseras, X., Andión, O., Torrubia, R., & y Mataix, D. (2005). Psychometric properties of the Spanish version of the obsessive-compulsive inventory-revised in a non-clinical simple. Journal of Anxiety Disorders, 19, 893–903. https://doi.org/10.1016/j.janxdis.2004.10.004
Hair, J. F., Black, W. C., & Babin, B. J. (2010). Multivariate data analysis: A global perspective. Pearson.
Henry, J. D., & Crawford, J. R. (2005). The short-form version of the depression anxiety stress scales (DASS-21): Construct validity and normative data in a large non-clinical sample. British Journal of Clinical Psychology, 44(2), 227–239. https://doi.org/10.1348/014466505X29657
Hooper, D., Coughlan, J., & Mullen, M. R. (2008). Structural equation modeling: Guidelines for determining model fit. Electronic Journal of Business Research Methods, 6, 53–60.
Hunsley, J., & Mash, E. J. (2008). A guide to assessments that work. Oxford University Press.
Jöreskog, K., & Sörbom, D. (1993). LISREL 8: Structural equation modeling with the SIMPLIS command language. Scientific Software International Inc..
Lovibond, S. H., & Lovibond, P. F. (1995). Manual for the depression anxiety stress scales (2nd ed.). Psychological Foundation.
Markland, D. (2007). The golden rule is that there are no golden rules: A commentary on Paul Barrett’s recommendations for reporting model fit in structural equation modelling. Personality and Individual Differences, 42(5), 851–858. https://doi.org/10.1016/j.paid.2006.09.023
Mathes, B. M., Norr, A. M., Allan, N. P., Albanese, B. J., & Schmidt, N. B. (2018). Cyberchondria: Overlap with health anxiety and unique relations with impairment, quality of life, and service utilization. Psychiatry Research, 261, 204–211. https://doi.org/10.1016/j.psychres.2018.01.002
McElroy, E., & Shevlin, M. (2014). The development and initial validation of the cyberchondria severity scale (CSS). Journal of Anxiety Disorders, 28(2), 259–265. https://doi.org/10.1016/j.janxdis.2013.12.007
McElroy, E., Kearney, M., Touhey, J., Evans, J., Cooke, Y., & Shevlin, M. (2019). The CSS-12: Development and validation of a short-form version of the cyberchondria severity scale. Cyberpsychology, Behavior and Social Networking, 22(5), 330–335. https://doi.org/10.1089/cyber.2018.0624
McManus, F., Leung, C., Muse, K., & Williams, J. M. G. (2014). Understanding ‘cyberchondria’: An interpretive phenomenological analysis of the purpose, methods and impact of seeking health information online for those with health anxiety. The Cognitive Behaviour Therapist, 7(21), 1–13. https://doi.org/10.1017/S1754470X14000270
McMullan, R. D., Berle, D., Arnáez, S., & Starcevic, V. (2019). The relationships between health anxiety, online health information seeking, and cyberchondria: Systematic review and meta-analysis. Journal of Affective Disorders, 245, 270–278.
Muse, K., McManus, F., Leung, C., Meghreblian, B., & Williams, J. M. G. (2012). Cyberchondriasis: Fact or fiction? A preliminary examination of the relationship between health anxiety and searching for health information on the internet. Journal of Anxiety Disorders, 26(1), 189–196. https://doi.org/10.1016/j.janxdis.2011.11.005
Norr, A. M., Allan, N. P., Boffa, J. W., Raines, A. M., & Schmidt, N. B. (2015a). Validation of the Cyberchondria severity scale (CSS): Replication and extension with bifactor modeling. Journal of Anxiety Disorders, 31, 58–64.
Norr, A. M., Oglesby, M. E., Raines, A. M., Macatee, R. J., Allan, N. P., & Schmidt, N. B. (2015b). Relationships between cyberchondria and obsessive-compulsive symptom dimensions. Psychiatry Research, 230(2), 441–446. https://doi.org/10.1016/j.psychres.2015.09.034
Osman, A., Wong, J. L., Bagge, C. L., Freedenthal, S., Gutierrez, P. M., & Lozano, G. (2012). The depression anxiety stress scales—21 (DASS-21): Further examination of dimensions, scale reliability, and correlates. Journal of Clinical Psychology, 68(12), 1322–1338. https://doi.org/10.1002/jclp.21908
Peters, G.-J. Y. (2014). The alpha and the omega of scale reliability and validity: Why and how to abandon Cronbach’s alpha and the route towards more comprehensive assessment of scale quality. European Health Psychologist, 16, 56–69.
Salkovskis, P., Rimes, K., Warwick, H., & Clark, D. (2002). The health anxiety inventory: Development and validation of scales for the measurement of health anxiety and hypochondriasis. Psychological Medicine, 32(5), 843–853. https://doi.org/10.1017/S0033291702005822
Schermelleh-Engel, K., & Müller, H. (2003). Evaluating the fit of structural equation models: Tests of significance and descriptive goodness-of-fit measures. Methods of Psychological Research, 8, 28–74.
Selvi, Y., Turan, S. G., Sayin, A. A., Boysan, M., & Kandeger, A. (2018). The Cyberchondria severity scale (CSS): Validity and reliability study of the Turkish version. Sleep and Hypnosis: A Journal of Clinical Neuroscience and Psychopathology, 20(4), 241–246. https://doi.org/10.5350/Sleep.Hypn.2018.20.0157
Silva, F. G. D., Andrade, R., Silva, I., & Cardoso, A. (2016). Cross-cultural adaptation of the Cyberchondria severity scale for Brazilian Portuguese. Trends in Psychiatry and Psychotherapy, 38(2), 90–95. https://doi.org/10.1590/2237-6089-2015-0063
Soraci, P., Lagattolla, F., Parente, G., Guaitoli, E., Cimaglia, R., Del Fante, E., & Puoti, C. (2020). Analisi esplorativa della cybercondria severity scale forma breve (css-12) nel contesto italiano. Mente e Cura, 184–206.
Starcevic, V. (2020). Problematic and compulsive online health research: The two faces of cyberchondria. Clinical Psychology: Science and Practice, 27(2), e12320. https://doi.org/10.1111/cpsp.12320
Starcevic, V., & Berle, D. (2013). Cyberchondria: Towards a better understanding of excessive health-related internet use. Expert Review of Neurotherapeutics, 13(2), 205–213. https://doi.org/10.1586/ern.12.162
Starcevic, V., Baggio, S., Berle, D., Khazaal, Y., & Viswasam, K. (2019). Cyberchondria and its relationships with related constructs: A network analysis. Psychiatric Quarterly, 90(3), 491–505. https://doi.org/10.1007/s11126-019-09640-5
Starcevic, V., Berle, D., & Arnáez, S. (2020). Recent insights into cyberchondria. Current Psychiatry Reports, 22(11), 1–8. https://doi.org/10.1007/s11920-020-01179-8
Tate, C. C., Ledbetter, J. N., & Youssef, C. P. (2013). A two-question method for assessing gender categories in the social and medical sciences. Journal of Sex Research, 50(8), 767–776.
Uzun, S. U., & Zencir, M. (2018). Reliability and validity study of the Turkish version of cyberchondria severity scale. Current Psychology, 1-7. https://doi.org/10.1007/s12144-018-0001-x
Vismara, M., Caricasole, V., Starcevic, V., Cinosi, E., Dell'Osso, B., Martinotti, G., & Fineberg, N. A. (2020). Is cyberchondria a new trans digital compulsive syndrome? A systematic review of the evidence. Comprehensive Psychiatry, 152167. https://doi.org/10.1016/j.comppsych.2020.152167.
Yung, Y. F., Thissen, D., & McLeod, L. D. (1999). On the relationship between the higher-order factor model and the hierarchical factor model. Psychometrika, 64, 113–128.
Zinbarg, R. E., Revelle, W., Yovel, I., & Li, W. (2005). Cronbach’s α, revelle’s β, and mcdonald’s ω H: Their relations with each other and two alternative conceptualizations of reliability. Psychometrika, 70, 123–133. https://doi.org/10.1007/s11336-003-0974-7
Funding
Open Access funding provided thanks to the CRUE-CSIC agreement with Springer Nature.
Author information
Authors and Affiliations
Contributions
All authors contributed to the study conception and design. Material preparation, data collection and analysis were performed by Sandra Arnáez, Gemma García-Soriano and Jesús Castro. The first draft of the manuscript was written by Sandra Arnáez and all authors commented on previous versions of the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Ethical Statements
The authors have abided by the Ethical Principles of Psychologists and the Code of Ethics.
Conflict of Interest
On behalf of all authors, the corresponding author states that there is no conflict of interest.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
ESM 1
(DOCX 37 kb)
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Arnáez, S., García-Soriano, G., Castro, J. et al. The Spanish version of the short form of the Cyberchondria Severity Scale (CSS-12): Testing the factor structure and measurement invariance across genders. Curr Psychol 42, 20686–20695 (2023). https://doi.org/10.1007/s12144-022-03170-3
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12144-022-03170-3