Abstract
Objective
To assess whether serum levels of neuronal biomarkers (S100 calcium-binding protein B and Neuron specific enolase) correlate with the neurodevelopmental outcome of term neonates at 18 mo who had hypoxic ischemic encephalopathy and underwent therapeutic hypothermia.
Methods
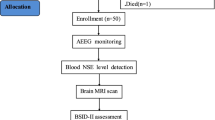
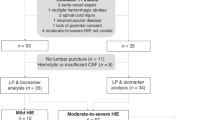
This randomized controlled trial was conducted in a tertiary care teaching hospital, south India. There were 162 term infants with moderate to severe hypoxic ischemic encephalopathy who were randomized into 2 groups (Group A and B). Neonates in Group A and B received normothermia and therapeutic hypothermia respectively. Serum levels of neuronal biomarkers were estimated at 0, 24 (±1) and 72 (±1) h after birth using sandwich ELISA in both groups. All neonates were carefully monitored till discharge. Infants who survived the neonatal period were followed up in the high risk clinic for 18 mo and neurodevelopmental assessment was done using Developmental Assessment Scale for Indian Infants (DASII). Neurodevelopmental outcomes between the two groups were compared using Chi square test and neuronal biomarker levels between the groups were compared using Mann Whitney test.
Results
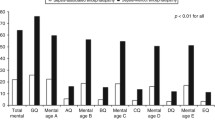
The baseline maternal and neonatal characteristics in both groups were comparable. There was statistically insignificant lesser mortality in therapeutic hypothermia group compared to normothermia group with Risk Ratio (RR): 0.82 (28.2% vs. 34.5%, 95% CI: 0.52–1.29, p = 0.38). Among the survivors, children in therapeutic hypothermia group had better motor and mental scores compared to those in normothermia group at 18 mo. There was no significant correlation between S100B and Neuron specific enolase levels and neurodevelopmental outcome.
Conclusions
Serum levels of neuronal biomarkers (S100B and Neuron specific enolase) do not correlate with the long term neurodevelopmental outcome among these infants.


Similar content being viewed by others
References
Kurinczuk JJ, White-Koning M, Badawi N. Epidemiology of neonatal encephalopathy and hypoxic-ischaemic encephalopathy. Early Hum Dev. 2010;86:329–38.
Shankaran S. Current status of hypothermia for hypoxemic ischemia of the newborn. Indian J Pediatr. 2014;81:578–84.
Jacobs SE, Berg M, Hunt R, Tarnow-Mordi WO, Inder TE, Davis PG. Cooling for newborns with hypoxic ischaemic encephalopathy. Cochrane Database Syst Rev. 2013;1:CD003311.
Bhat BV, Adhisivam B. Therapeutic cooling for perinatal asphyxia-Indian experience. Indian J Pediatr. 2014;81:585–91.
Bhat BV, Adhisivam B. Therapeutic hypothermia in hypoxic-ischemic encephalopathy. Indian J Pediatr. 2015;82:105–6.
Goncalves CA, Leite MC, Nardin P. Biological and methodological features of the measurement of S100B, a putative marker of brain injury. Clin Biochem. 2008;41:755–63.
Kaiser E, Kuzmits R, Pregant P, Burghuber O, Worofka W. Clinical biochemistry of neuron-specific enolase. Clin Chim Acta. 1989;183:13–31.
Massaro N, Chang T, Kadom N, Tsuchida T, Scafidi J, Glass P. Biomarkers of brain injury in neonatal encephalopathy treated with hypothermia. J Pediatr. 2012;161:434–40.
Celtik C, Acunas B, Oner N, Pala O. Neuron-specific enolase as a marker of the severity and outcome of hypoxic ischemic encephalopathy. Brain Dev. 2004;26:398–402.
Bharadwaj SK, Bhat BV. Therapeutic hypothermia using gel packs for term neonates with hypoxic ischaemic encephalopathy in resource-limited settings: a randomized controlled trial. J Trop Pediatr. 2012;58:382–8.
Thomas N, Abiramalatha T, Bhat V, et al. Phase changing material for therapeutic hypothermia in neonates with hypoxic ischemic encephalopathy - a multi-centric study. Indian Pediatr. 2018;55:201–5.
Phatak P. Developmental assessment scales for Indian infants (DASII) – revised Baroda norms manual. 1997.
Bharadwaj SK, Bhat BV, Vickneswaran V, Adhisivam B, Bobby Z, Habeebullah S. Oxidative stress, antioxidant status and neurodevelopmental outcome in neonates born to pre-eclamptic mothers. Indian J Pediatr. 2018;85:351–7.
Pauliah SS, Shankaran S, Wade A, Cady EB, Thayyil S. Therapeutic hypothermia for neonatal encephalopathy in low- and middle-income countries: a systematic review and meta-analysis. PLoS One. 2013;8:e58834.
Graham EM, Everett AD, Delpech JC, Northington FJ. Blood biomarkers for evaluation of perinatal encephalopathy: state of the art. Curr Opin Pediatr. 2018;30:199–203.
Massaro AN, Chang T, Baumgart S, McCarter R, Nelson KB, Glass P. Biomarkers S100B and neuron-specific enolase predict outcome in hypothermia-treated encephalopathic newborns. Pediatr Crit Care Med. 2014;15:615–22.
Nagdyman N, Komen W, Ko HK, Muller C, Obladen M. Early biochemical indicators of hypoxic-ischemic encephalopathy after birth asphyxia. Pediatr Res. 2001;49:502–6.
Nagdyman N, Grimmer I, Scholz T, Muller C, Obladen M. Predictive value of brain- specific proteins in serum for neurodevelopmental outcome after birth asphyxia. Pediatr Res. 2003;54:270–5.
Roka A, Kelen D, Halasz J, Beko G, Azzopardi D, Szabo M. Serum S100B and neuron- specific enolase levels in normothermic and hypothermic infants after perinatal asphyxia. Acta Paediatr. 2012;101:319–23.
Massaro AN, Jeromin A, Kadom N, et al. Serum biomarkers of MRI brain injury in neonatal hypoxic ischemic encephalopathy treated with whole-body hypothermia: a pilot study. Pediatr Crit Care Med. 2013;14:310–7.
Douglas-Escobar M, Yang C, Bennett J, et al. A pilot study of novel biomarkers in neonates with hypoxic-ischemic encephalopathy. Pediatr Res. 2010;68:531–6.
Chalak LF, Sanchez PJ, Adams-Huet B, Laptook AR, Heyne RJ, Rosenfeld CR. Biomarkers for severity of neonatal hypoxic-ischemic encephalopathy and outcomes in newborns receiving hypothermia therapy. J Pediatr. 2014;164:468–74.
Douglas-Escobar MV, Heaton SC, Bennett J, et al. UCH- L1 and GFAP serum levels in neonates with hypoxic-ischemic encephalopathy: a single center pilot study. Front Neurol. 2014;5:273.
Thorngren-Jerneck K, Alling C, Herbst A, Amer-Wahlin I, Marsal K. S100 protein in serum as a prognostic marker for cerebral injury in term newborn infants with hypoxic ischemic encephalopathy. Pediatr Res. 2004;55:406–12.
Liu F, Yang S, Du Z, Guo Z. Dynamic changes of cerebral-specific proteins in full-term newborns with hypoxic-ischemic encephalopathy. Cell Biochem Biophys. 2013;66:389–96.
Ennen CS, Huisman TA, Savage WJ, et al. Glial fibrillary acidic protein as a biomarker for neonatal hypoxic-ischemic encephalopathy treated with whole-body cooling. Am J Obstet Gynecol. 2011;205:251.
Alshweki A, Pérez-Muñuzuri A, López-Suárez O, Baña A, Couce ML, Wane D. Relevance of urinary S100B protein levels as a short-term prognostic biomarker in asphyxiated infants treated with hypothermia. Medicine. 2017;96:e8453.
Massaro AN, Wu YW, Bammler TK, et al. Plasma biomarkers of brain injury in neonatal hypoxic-ischemic encephalopathy. J Pediatr. 2018;194:67–75.e1.
Author information
Authors and Affiliations
Contributions
RCC: helped in data collection; BVB: designed and supervised study and edited manuscript; BA: helped in designing study, data analysis and drafting manuscript; SKB: helped in data collection and clinical management; VV: helped in biomarker assay; PC: data analysis. BVB is the guarantor for this paper.
Corresponding author
Ethics declarations
Conflict of Interest
None.
Source of Funding
Department of Biotechnology, Government of India (Grant No. BT/PR8717/MED/97/141/2013).
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Catherine, R.C., Bhat, B.V., Adhisivam, B. et al. Neuronal Biomarkers in Predicting Neurodevelopmental Outcome in Term Babies with Perinatal Asphyxia. Indian J Pediatr 87, 787–792 (2020). https://doi.org/10.1007/s12098-020-03283-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12098-020-03283-2