Abstract
Objectives
To study the clinical profile, and outcome of children with anti-N-methyl-D-aspartate receptor (NMDAR) encephalitis.
Methods
This is a retrospective case series of children <12 y of age, diagnosed with anti-NMDAR encephalitis at a tertiary care institute during the period, May 2013 through June 2015.
Results
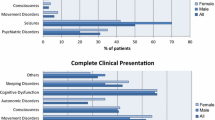
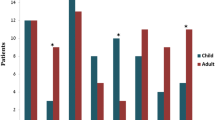
Twenty patients were tested for suspected anti-NMDAR encephalitis over this 2 y period. Of these, six children were positive for anti-NMDAR antibodies. Four of these six children had completed treatment and two are currently receiving immunotherapy. Behavioral changes, psychosis, seizures and oro-lingual-facial dyskinesia were the presenting features. Extreme irritability, insomnia and mutism were noted in all the children. The symptoms were persistent, and the course was progressive over 4–8 wk duration. Neuroimaging and electroencephalography were non-specific. Intravenous pulse methylprednisolone and immunoglobulins were used as first-line therapeutic agents. Only one patient responded to first line immunotherapy; five out of six children required second-line immunotherapy. One patient recovered following rituximab, and two patients showed a good response to cyclophosphamide pulse therapy; two patients are currently under treatment with second line immunotherapeutic agents. Tumor screen was negative in all children.
Conclusions
Anti-NMDAR encephalitis is rare but a potentially treatable condition. Timely recognition is essential because treatment is entirely different from other viral encephalitis. Aggressive immunotherapy is the key to a favourable outcome.
Similar content being viewed by others
References
Vitaliani R, Mason W, Ances B, Zwerdling T, Jiang Z, Dalmau J. Paraneoplastic encephalitis, psychiatric symptoms, and hypoventilation in ovarian teratoma. Ann Neurol. 2005;58:594–604.
Dalmau J, Lancaster E, Martinez-Hernandez E, Rosenfeld MR, Balice-Gordon R. Clinical experience and laboratory investigations in patients with anti-NMDAR encephalitis. Lancet Neurol. 2011;10:63–74.
Dalmau J, Tüzün E, Wu HY, et al. Paraneoplastic anti-N-methyl-D-aspartate receptor encephalitis associated with ovarian teratoma. Ann Neurol. 2007;61:25–36.
Gable MS, Sheriff H, Dalmau J, Tilley DH, Glaser CA. The frequency of autoimmune N-methyl-D-aspartate receptor encephalitis surpasses that of individual viral etiologies in young individuals enrolled in the California encephalitis project. Clin Infect Dis. 2012;54:899–904.
Wandinger KP, Saschenbrecker S, Stoecker W, Dalmau J. Anti-NMDA-receptor encephalitis: a severe, multistage, treatable disorder presenting with psychosis. J Neuroimmunol. 2011;231:86–91.
Raha S, Gadgil P, Sankhla C, Udani V. Nonparaneoplastic anti-N-methyl-D-aspartate receptor encephalitis: a case series of four children. Pediatr Neurol. 2012;46:246–9.
Chakrabarty B, Tripathi M1, Gulati S, et al. Pediatric anti-N-methyl-D-aspartate (NMDA) receptor encephalitis: experience of a tertiary care teaching center from north India. J Child Neurol. 2014;29:1453–9.
Titulaer MJ, McCracken L, Gabilondo I, et al. Treatment and prognostic factors for long-term outcome in patients with anti-NMDA receptor encephalitis: an observational cohort study. Lancet Neurol. 2013;12:157–65.
Irani SR, Bera K, Waters P, et al. N-methyl-D-aspartate antibody encephalitis: temporal progression of clinical and paraclinical observations in a predominantly non-paraneoplastic disorder of both sexes. Brain. 2010;133:1655–67.
Peery HE, Day GS, Dunn S, et al., anti-NMDA receptor encephalitis. The disorder, the diagnosis and the immunobiology. Autoimmun Rev. 2012;11:863–72.
Florance NR, Davis RL, Lam C, et al. Anti-N-methyl-D-aspartate receptor (NMDAR) encephalitis in children and adolescents. Ann Neurol. 2009;66:11–8.
Armangue T, Titulaer MJ, Málaga I, et al. Pediatric anti-N-methyl-D-aspartate receptor encephalitis-clinical analysis and novel findings in a series of 20 patients. J Pediatr 2013;162:850–6. e2.
Goldberg EM, Titulaer M, de Blank PM, Sievert A, Ryan N. Anti-N-methyl-D-aspartate receptor-mediated encephalitis in infants and toddlers: case report and review of the literature. Pediatr Neurol. 2014;50:181–4.
DeSena AD, Greenberg BM, Graves D.”light switch” mental status changes and irritable insomnia are two particularly salient features of anti-NMDA receptor antibody encephalitis. Pediatr Neurol. 2014;51:151–3.
Stamelou M, Plazzi G, Lugaresi E, et al. The distinct movement disorder in anti-NMDA receptor encephalitis may be related to status dissociatus: a hypothesis. Mov Disord. 2012;27:1360–3.
Hacohen Y, Dlamini N, Hedderly T, et al. N-methyl-D-aspartate receptor antibody-associated movement disorder without encephalopathy. Dev Med Child Neurol. 2014;56:190–3.
Titulaer MJ, Höftberger R, Iizuka T, et al. Overlapping demyelinating syndromes and anti-N-methyl-D-aspartate receptor encephalitis. Ann Neurol. 2014;75:411–28.
Titulaer MJ, Leypoldt F, Dalmau J. Antibodies to N-methyl-D-aspartate and other synaptic receptors in choreoathetosis and relapsing symptoms post-herpes virus encephalitis. Mov Disord. 2014;29:3–6.
Prüss H, Finke C, Höltje M, et al. N-methyl-D-aspartate receptor antibodies in herpes simplex encephalitis. Ann Neurol. 2012;72:902–11.
Benarroch EE. NMDA receptors: recent insights and clinical correlations. Neurology. 2011;76:1750–7.
Zhang Q, Tanaka K, Sun P, et al. Suppression of synaptic plasticity by cerebrospinal fluid from anti-NMDA receptor encephalitis patients. Neurobiol Dis. 2012;45:610–5.
Moscato EH, Peng X, Jain A, Parsons TD, Dalmau J, Balice-Gordon RJ. Acute mechanisms underlying antibody effects in anti-N-methyl-D-aspartate receptor encephalitis. Ann Neurol. 2014;76:108–19.
da Silva-Júnior FP, Castro LH, Andrade JQ, et al. Serial and prolonged EEG monitoring in anti-N-methyl-d-aspartate receptor encephalitis. Clin Neurophysiol. 2014;125:1541–4.
Schmitt SE, Pargeon K, Frechette ES, Hirsch LJ, Dalmau J, Friedman D. Extreme delta brush: a unique EEG pattern in adults with anti-NMDA receptor encephalitis. Neurology. 2012;79:1094–100.
Finke C, Kopp UA, Scheel M, et al. Functional and structural brain changes in anti-N-methyl-D-aspartate receptor encephalitis. Ann Neurol. 2013;74:284–96.
Pillai SC, Gill D, Webster R, Howman-Giles R, Dale RC. Cortical hypometabolism demonstrated by PET in relapsing NMDA receptor encephalitis. Pediatr Neurol. 2010;43:217–20.
Gresa-Arribas N, Titulaer MJ, Torrents A, et al. Antibody titres at diagnosis and during follow-up of anti-NMDA receptor encephalitis: a retrospective study. Lancet Neurol. 2014;13:167–77.
Appu M, Noetzel M. Clinically significant response to zolpidem in disorders of consciousness secondary to anti-N-methyl-D-aspartate receptor encephalitis in a teenager: a case report. Pediatr Neurol. 2014;50:262–4.
Kashyape P, Taylor E, Ng J, Krishnakumar D, Kirkham F, Whitney A. Successful treatment of two pediatric cases of anti-NMDA receptor encephalitis with cyclophosphamide: the need for early aggressive immunotherapy in tumour negative pediatric patients. Eur J Paediatr Neurol. 2012;16:74–8.
Acknowledgments
The authors wish to thank Dr. Josep Dalmau, (ICREA Senior Investigator, Institutd’InvestigacionsBiomèdiques August Pi iSunyer (IDIBAPS), Hospital Clinic, University of Barcelona, Spain) for his support in testing the samples.
Contributions
RS, AGS: Patient management, draft of manuscript and review of literature; JKS: Patient management, critical review of manuscript for important intellectual content and final approval of the version to be published; NS: Patient management, critical review of manuscript for important intellectual content and final approval of the version to be published; PS: Clinician-in-charge, concept and design of the study, critical review of manuscript for important intellectual content and final approval of the version to be published. She will act as guarantor for the paper.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
None.
Source of Funding
None.
Rights and permissions
About this article
Cite this article
Suthar, R., Saini, A.G., Sankhyan, N. et al. Childhood Anti-NMDA Receptor Encephalitis. Indian J Pediatr 83, 628–633 (2016). https://doi.org/10.1007/s12098-015-1988-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12098-015-1988-8