Abstract
Objective
The present study aimed at assessing the population prevalence of goiter and iodine deficiency in school children of 6–12 yr living in urban slums of Bhubaneswer, the capital city of Orissa.
Methods
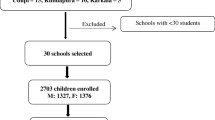
A cross-sectional study was performed using the 30-cluster sampling methodology and surveillance methods for iodine deficiency as recommended by WHO/ICCIDD/UNICEF. The total goitre rate (n=1248), urinary iodine concentration (UIC) (n=411) and iodine content of edible salt (n=368) were measured.
Results
The goitre prevalence was 23.6% (grade 1=18.9%, grade 2=4.7%) with no significant gender variation. Goitre prevalence was significantly higher in children of 10–12 yr (P=0.012) and scheduled caste and tribe (P=0.003). Median urinary iodine concentration was 50.0 μg/l with 85.7% of children having values less than 100 μg/l, indicating as biochemical iodine deficiency. Median UIC was inversely in association with gradations of goitre. Children of 10–12 yr and scheduled caste/tribe communities had significantly higher median UIC (P=0.001) than their counterpart peers. About 51% of children were consuming salt having stipulated iodine content of 15 ppm.
Conclusion
The study indicates moderate iodine deficiency in the population, despite a mandatory salt iodization programme in Orissa that has been in force since 1989. There is a need to improve the situation through enforcing monitoring of salt iodization to ensure quality and increasing the level of awareness about the iodized salt for sustainable prevention and control of iodine deficiency.
Similar content being viewed by others
References
Mehta M, Pandav CS, Kochupillai N. Intellectual assessment of school children from severely iodine deficient villages. Indian Pediatr 1987; 24: 467–473.
National Iodine Deficiency Disorders Control Program: National Health Program Series 5. Published by Department of Communication, National Institute of Health and Family Welfare, New Delhi, 2003; 99.
National Family Health Survey (NFHS-2) 1998–1999. Mumbai; India. Institute for Population Science, 2001; 170–172.
Report of the District Level Household Survey 2002–2003. Mumbai; Reproductive and Child Health, India. Round-2, Phase-I. Institute for Population Science, 2003; 18–19.
Current status of IDD in Selected Districts of Different Regions of the country: Eastern Region. Hyderabad; National Institute of Nutrition, 2003; 47–59.
Dodd NS, Samuel AM. Iodine deficiency in adolescents from Bombay slums. Natl Med J India 1993; 6: 110–113.
Kapil U, Pathak P, Tandon M, Singh C, Pradhan R, Dwivedi SN. Micronutrient deficiency disorders amongst pregnant women in three urban slum communities of Delhi. Indian Pediatr 1999; 36: 983–989.
Ghosh S, Shah D. Nutritional problems in urban slum children. Indian Pediatr 2004; 41: 682–696.
Registrar General & Census Commissioner, India. Census of India 2001. Slum population in States and Union Territories. Part A. 2001
WHO/UNICEF/ICCIDD. Assessment of Iodine Deficiency Disorders and Monitoring their Elimination. Geneva; World Health Organization (WHO/NHD/01.1), 2001; 3–36.
WHO/UNICEF/ICCIDD. Indicators for Assessing Iodine Deficiency Disorders and their Control through Salt Iodization. Report of Joint Consultation. WHO/NUT/94.6, Geneva; World Health Organization, 1994; 13–55.
Dunn JT, Crutchfield HE, Gutekunst R, Dunn D. Methods for Measuring Iodine in Urine. A Joint Publication of WHO/UNICEF/ICCIDD, 1993; 18–23.
Sullivan KM, Houston R, Gorstein J, Cervinskas J. Monitoring Universal Salt Iodization Programmes. Atlanta, GA; UNICEF/PAMM/MI/ICCIDD/WHO, 1995; 86–101.
Mohapatra SSS, Bulliyya G, Kerketta AS, Marai NS, Acharya AS. Iodine deficiency disorders in Bargarh district of western Orissa. Indian Pediatr 2000; 37: 536–539.
Sahu T, Sahani NC, Satapathy DM, Behera TR. Prevalence of goitre in 6–12 year children of Kandhamal district of Orissa. Indian J Community Med 2005; 30: 51–52.
State Government of Orissa/National Institte of Epidemiology/National Institute of Nutrition/All India Institute of Medical Sciences/ICCIDD/UNICEF. Orissa: Towards Sustaining Elimination of IDD. 2004; 40–53.
Dunn JT, Van der Haar P. A Practical Guide for Correction of Iodine Deficiency. International Council for the Control of Iodine Deficiency Disorders. The Netherlands; ICCIDD/WHO/UNICEF, 1990; 62.
Office of the Salt Commisioner. Annual Report 2001–2002, Salt Department, Government of India, Jaipur; Ministry of Commerce and Industry, 2003; 65–71.
Pandav CS, Karmarkar MG. Recommended levels of salt iodination in India. Indian J Pediatr 1984; 51: 53–54.
de Benoist B, Andersson M, Egli I, Takkouche B, Allen H, eds. Iodine status worldwide. WHO Global Database on Iodine Deficiency. Geneva; World Health Organization, 2004; 1–3.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Sethy, P.G.S., Bulliyya, G., Mallick, G. et al. Iodine deficiency in urban slums of Bhubaneswar. Indian J Pediatr 74, 917–921 (2007). https://doi.org/10.1007/s12098-007-0169-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12098-007-0169-9