Abstract
Background
Gastric cancer (GC) is a malignant gastrointestinal tumor that can result in high mortality. Surgery and chemotherapy are often used for the effective treatment of GC. In addition, lymph node metastasis is a significant factor affecting the therapy of GC. Current researches have revealed that gut microbiota has the potential as biomarkers to distinguish healthy people and GC patients. However, the relationship between surgery, chemotherapy, and lymph node metastasis is still unclear.
Methods
In this study, 16S rRNA sequencing was used to investigate 157 GC fecal samples to identify the role of surgery, chemotherapy, and lymph node metastasis. Immunohistochemical analysis was used to value the expression of Ki67, HER2 in GC patient tissues.
Results
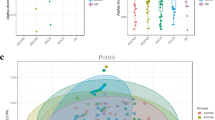
There exist some gut microbiotas which can distinguish surgery from non-surgery GC patients, including Enterococcus, Megasphaera, Corynebacterium, Roseburia, and Lachnospira. Differences between lymph node metastasis and chemotherapy in GC patients are not significant. Moreover, we found the abundance of Blautia, Ruminococcus, Oscillospira were related to the expression of Ki67 and the abundance of Prevotella, Lachnospira, Eubacterium, Desulfovibiro were correlated with the expression of HER2.
Conclusions
The choice of treatment has a certain impact on the intestinal flora of patients with gastric cancer. Our research shows that surgery has a great effect on the intestinal flora of patients with gastric cancer. However, there were no significant differences in the characteristics of intestinal flora in patients with gastric cancer whether they received chemotherapy or whether they had lymph node metastasis. In addition, the association of gut microbiota with Ki67 and HER2 indicators is expected to provide the possibility of gut microbiota as a tumor prognostic marker.





Similar content being viewed by others
Data availability
Sequences of this study have been deposited on NGDC under BioProject ID PRJCA006619 (available at https://ngdc.cncb.ac.cn/bioproject/browse/PRJCA006619).
References
Venerito M, Link A, Rokkas T, Malfertheiner P. Gastric cancer—clinical and epidemiological aspects. Helicobacter. 2016;21:39–44.
Thrift AP, El-Serag HB. Burden of gastric cancer. Clin Gastroenterol Hepatol. 2020;18:534–42.
Van Cutsem E, Sagaert X, Topal B, Haustermans K, Prenen H. Gastric cancer. The Lancet. 2016;388:2654–64.
Liang W, Yang Y, Wang H, Wang H, Yu X, Lu Y, et al. Gut microbiota shifts in patients with gastric cancer in perioperative period. Medicine. 2019;98: e16626.
Qi Y, Sun J, Ren L, Cao X, Dong J, Tao K, et al. Intestinal microbiota is altered in patients with gastric cancer from Shanxi province, China. Dig Dis Sci. 2019;64:1193–203.
Wu J, Zhang C, Xu S, Xiang C, Wang R, Yang D, et al. Fecal microbiome alteration may be a potential marker for gastric cancer. Dis Mark. 2020;2020:1–17.
Chen C, Chen L, Lin L, Jin D, Du Y, Lyu J. Research progress on gut microbiota in patients with gastric cancer, esophageal cancer, and small intestine cancer. Appl Microbiol Biotechnol. 2021;105:4415-25.
Zhang Y, Shen J, Shi X, Du Y, Niu Y, Jin G, et al. Gut microbiome analysis as a predictive marker for the gastric cancer patients. Appl Microbiol Biotechnol. 2021;105:803–14.
Shi W, Shen L, Zou W, Wang J, Yang J, Wang Y, et al. The gut microbiome is associated with therapeutic responses and toxicities of neoadjuvant chemoradiotherapy in rectal cancer patients—a pilot study. Front Cell Infect Microbiol. 2020;10: 562463.
Jang B-S, Chang JH, Chie EK, Kim K, Park JW, Kim MJ, et al. Gut microbiome composition is associated with a pathologic response after preoperative chemoradiation in patients with rectal cancer. Int J Radiat Oncol Biol Phys. 2020;107:736–46.
Li LT, Jiang G, Chen Q, Zheng JN. Ki67 is a promising molecular target in the diagnosis of cancer (review). Mol Med Rep. 2015;11:1566–72.
Bouzubar N, Walker K, Griffiths K, Ellis I, Elston C, Robertson J, et al. Ki67 immunostaining in primary breast cancer: pathological and clinical associations. Br J Cancer. 1989;59:943–7.
Scagliotti GV, Micela M, Gubetta L, Leonardo E, Cappia S, Borasio P, et al. Prognostic significance of Ki67 labelling in resected non small cell lung cancer. Eur J Cancer. 1993;29:363–5.
Tzanakis N, Peros G, Karakitsos P, Giannopoulos G, Efstathiou S, Rallis G, et al. Prognostic significance of p53 and Ki67 proteins expression in Greek gastric cancer patients. Acta Chirurg Belg. 2009;109:606–11.
Melling N, Kowitz CM, Simon R, Bokemeyer C, Terracciano L, Sauter G, et al. High Ki67 expression is an independent good prognostic marker in colorectal cancer. J Clin Pathol. 2016;69:209–14.
Shen Y, Wenjuan Q, Shen H. Association of expression of ki67 with metastasis, TNM staging and survival in patients with nasopharyngeal carcinoma. Chin J Stereol Image Anal. 2010;2:213–18.
Rubin I, Yarden Y. The basic biology of HER2. Ann Oncol. 2001;12:S3-8.
Tai W, Mahato R, Cheng K. The role of HER2 in cancer therapy and targeted drug delivery. J Control Release. 2010;146:264–75.
Ménard S, Fortis S, Castiglioni F, Agresti R, Balsari A. HER2 as a prognostic factor in breast cancer. Oncology. 2001;61(suppl 2):67–72.
Gravalos C, Jimeno A. HER2 in gastric cancer: a new prognostic factor and a novel therapeutic target. Ann Oncol. 2008;19:1523–9.
Navas-Molina JA, Peralta-Sánchez JM, González A, McMurdie PJ, Vázquez-Baeza Y, Xu Z, et al. Advancing our understanding of the human microbiome using QIIME. Methods Enzymol. 2013;531:371–444.
Magoc T, Salzberg SL. FLASH: fast length adjustment of short reads to improve genome assemblies. Bioinformatics. 2011;27:2957–63.
Edgar RC. Updating the 97% identity threshold for 16S ribosomal RNA OTUs. Bioinformatics. 2018;34:2371–5 (Valencia A, editor).
Chong J, Liu P, Zhou G, Xia J. Using MicrobiomeAnalyst for comprehensive statistical, functional, and meta-analysis of microbiome data. Nat Protoc. 2020;15:799–821.
Dhariwal A, Chong J, Habib S, King IL, Agellon LB, Xia J. MicrobiomeAnalyst: a web-based tool for comprehensive statistical, visual and meta-analysis of microbiome data. Nucleic Acids Res. 2017;45:W180–8.
Guyton K, Alverdy JC. The gut microbiota and gastrointestinal surgery. Nat Rev Gastroenterol Hepatol. 2017;14:43–54.
Lin X-H, Yang U-C, Luo J-C, Chang T-E, Lin H-H, Huang C-W, et al. Differences in intestinal microbiota profiling after upper and lower gastrointestinal surgery. J Chin Med Assoc. 2021;84:354–60.
Cong J, Zhu H, Liu D, Li T, Zhang C, Zhu J, et al. A pilot study: changes of gut microbiota in post-surgery colorectal cancer patients. Front Microbiol. 2018;9:2777.
Jin Y, Liu Y, Zhao L, Zhao F, Feng J, Li S, et al. Gut microbiota in patients after surgical treatment for colorectal cancer. Environ Microbiol. 2019;21:772–83.
Wang Z, Gao X, Zeng R, Wu Q, Sun H, Wu W, et al. Changes of the gastric mucosal microbiome associated with histological stages of gastric carcinogenesis. Front Microbiol. 2020;11:997.
Alexander JL, Wilson ID, Teare J, Marchesi JR, Nicholson JK, Kinross JM. Gut microbiota modulation of chemotherapy efficacy and toxicity. Nat Rev Gastroenterol Hepatol. 2017;14:356–65.
Kong C, Gao R, Yan X, Huang L, He J, Li H, et al. Alterations in intestinal microbiota of colorectal cancer patients receiving radical surgery combined with adjuvant CapeOx therapy. Sci China Life Sci. 2019;62:1178–93.
Power DG, Kelsen DP, Shah MA. Advanced gastric cancer—slow but steady progress. Cancer Treat Rev. 2010;36:384–92.
Wu Y, Shi L, Li Q, Wu J, Peng W, Li H, et al. Microbiota diversity in human colorectal cancer tissues is associated with clinicopathological features. Nutr Cancer. 2019;71:214–22.
Acknowledgements
We thank Guoqing Ru in Zhejiang Provincial People’s Hospital for assistance with GC tissue histological examination.
Funding
This study was supported by Zhejiang Provincial Natural Science Foundation of China (Grant No. LQ21H200007), Zhejiang Provincial People’s Hospital Excellent Scientific Research Start-up Foundation of China (Grant Nos. ZRY2019C008 and ZRY2019C0025), Zhejiang Provincial Science Research Project of Department of Education of China (Grant No. Y201942606), Zhejiang Provincial Medical and Health Science and Technology Project of China (Grant Nos. 2017KY216 and 2017KY486), and Zhejiang Provincial Ten Thousand People Plan for Outstanding Talents of China (Grant No. 00004A51901).
Author information
Authors and Affiliations
Contributions
LJL and YKS designed and supervised this study, CCC and JS drafted this manuscript, CCC, YFN, and GLJ provided technical and material support and data analysis, CCC, YXL and XWS provided the samples and clinical data. YQD and JXL revised the manuscript critically for important intellectual content.
Corresponding authors
Ethics declarations
Conflict of interest
Yaofang Niu and Gulei Jin are employed by the Hangzhou Guhe Information and Technology Company. The remaining authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest. The Ethics Committee of Zhejiang Provincial People’s Hospital approved this study (No. 2022QT010). Due to the retrospective nature of the study, the Medical Ethics Committee of Zhejiang Provincial People's Hospital waived the need for written informed consent by the patients, and all the samples were anonymous.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Chen, C., Shen, J., Du, Y. et al. Characteristics of gut microbiota in patients with gastric cancer by surgery, chemotherapy and lymph node metastasis. Clin Transl Oncol 24, 2181–2190 (2022). https://doi.org/10.1007/s12094-022-02875-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12094-022-02875-y