Abstract
Purpose
Treatment of recurrent ovarian carcinoma is a challenge, particularly for the clear cell (CCC) subtype. However, there is a preclinical rationale that these patients could achieve a benefit from antiangiogenic therapy. To assess this hypothesis, we used the growth modulation index (GMI), which represents an intrapatient comparison of two successive progression-free survival (PFS).
Methods
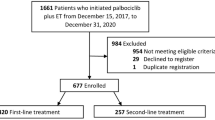
We conducted a retrospective real-world study performed on 34 patients with recurrent ovarian cancer, treated with bevacizumab-containing regimens from January 2009 to December 2017. The primary endpoint was GMI. An established cut-off > 1.33 was defined as a sign of drug activity.
Results
73.5% of patients had high-grade serous ovarian carcinoma (HGSOC), and 17.7% had CCC; 70.6% of patients received carboplatin/gemcitabine/bevacizumab, and 29.4% received weekly paclitaxel/bevacizumab. According to histological subtype, the overall response rate and median PFS were 52% and 14 months for HGSOC and 83.3% and 20 months for CCC, respectively. The overall population median GMI was 0.99; it was 0.95 and 2.36 for HGSOC and CCC, respectively. CCC subtype was significantly correlated with GMI > 1.33 (odds ratio 41.67; 95% confidence interval 3.6–486.94; p = .03).
Conclusion
Adding bevacizumab to chemotherapy in recurrent CCC is associated with a remarkable benefit in this cohort. The efficacy of antiangiogenic drugs in CCC warrants further prospective evaluation.



Similar content being viewed by others
Availability of data and material
We will provide our data for the reproducibility of this study in other centers if such is requested.
References
Burger RA, Brady MF, Bookman MA, et al. Incorporation of bevacizumab in the primary treatment of ovarian cancer. N Engl J Med. 2011;365(26):2473–83.
Perren TJ, Swart AM, Pfisterer J, et al. A phase 3 trial of bevacizumab in ovarian cancer. N Engl J Med. 2011;365(26):2484–96.
Aghajanian C, Goff B, Nycum LR, et al. Final overall survival and safety analysis of OCEANS, a phase 3 trial of chemotherapy with or without bevacizumab in patients with platinum-sensitive recurrent ovarian cancer. Gynecol Oncol. 2015;139(1):10–6.
Coleman RL, Brady MF, Herzog TJ, et al. Bevacizumab and paclitaxel-carboplatin chemotherapy and secondary cytoreduction in recurrent, platinum-sensitive ovarian cancer (NRG Oncology/Gynecologic Oncology Group study GOG-0213): a multicentre, open-label, randomised, phase 3 trial. Lancet Oncol. 2017;18(6):779–91.
Pujade-Lauraine E, Hilpert F, Weber B, et al. Bevacizumab combined with chemotherapy for platinum-resistant recurrent ovarian cancer: the AURELIA open-label randomized phase III trial. J Clin Oncol. 2014;32(13):1302–8.
Winter WE 3rd, Maxwell GL, Tian C, et al. Prognostic factors for stage III epithelial ovarian cancer: a Gynecologic Oncology Group Study. J Clin Oncol. 2007;25(24):3621–7.
Kajiyama H, Suzuki S, Yoshikawa N, et al. Oncologic outcomes after secondary surgery in recurrent clear-cell carcinoma of the ovary. Int J Gynecol Cancer. 2019;29(5):910–5.
Hogen L, Vicus D, Ferguson SE, et al. Patterns of recurrence and impact on survival in patients with clear cell ovarian carcinoma. Int J Gynecol Cancer. 2019;29(7):1164–9.
Lee S, Garner EI, Welch WR, et al. Over-expression of hypoxia-inducible factor 1 alpha in ovarian clear cell carcinoma. Gynecol Oncol. 2007;106(2):311–7.
Mabuchi S, Sugiyama T, Kimura T. Clear cell carcinoma of the ovary: molecular insights and future therapeutic perspectives. J Gynecol Oncol. 2016;27(3):e31.
Von Hoff DD. There are no bad anticancer agents, only bad clinical trial designs—twenty-first richard and hinda rosenthal foundation award lecture. Clin Cancer Res. 1998;4(5):1079–86.
Penel N, Demetri GD, Blay JY, et al. Growth modulation index as metric of clinical benefit assessment among advanced soft tissue sarcoma patients receiving trabectedin as a salvage therapy. Ann Oncol. 2013;24(2):537–42.
Oza AM, Cook AD, Pfisterer J, et al. ICON7 trial investigators. Standard chemotherapy with or without bevacizumab for women with newly diagnosed ovarian cancer (ICON7): overall survival results of a phase 3 randomised trial. Lancet Oncol. 2015;16(8):928–36.
Lee JY, Park JY, Park SY, et al. Real-world effectiveness of bevacizumab based on AURELIA in platinum-resistant recurrent ovarian cancer (REBECA): a Korean Gynecologic Oncology Group study (KGOG 3041). Gynecol Oncol. 2019;152(1):61–7.
Crotzer DR, Sun CC, Coleman RL, et al. Lack of effective systemic therapy for recurrent clear cell carcinoma of the ovary. Gynecol Oncol. 2007;105(2):404–8.
Oliver KE, Brady WE, Birrer M, et al. An evaluation of progression free survival and overall survival of ovarian cancer patients with clear cell carcinoma versus serous carcinoma treated with platinum therapy: an NRG Oncology/Gynecologic Oncology Group experience. Gynecol Oncol. 2017;147(2):243–9.
Rocha AL, Reis FM, Taylor RN. Angiogenesis and endometriosis. Obstet Gynecol Int. 2013;2013:859619.
Laschke MW, Elitzsch A, Vollmar B, et al. Combined inhibition of vascular endothelial growth factor (VEGF), fibroblast growth factor and platelet-derived growth factor, but not inhibition of VEGF alone, effectively suppresses angiogenesis and vessel maturation in endometriotic lesions. Hum Reprod. 2006;21(1):262–8.
Zorn KK, Bonome T, Gangi L, et al. Gene expression profiles of serous, endometrioid, and clear cell subtypes of ovarian and endometrial cancer. Clin Cancer Res. 2005;11(18):6422–30.
Chandler RL, Damrauer JS, Raab JR, et al. Coexistent ARID1A–PIK3CA mutations promote ovarian clear-cell tumorigenesis through pro-tumorigenic inflammatory cytokine signalling. Nat Commun. 2015;6:6118.
Anglesio MS, George J, Kulbe H, et al. IL6–STAT3–HIF signaling and therapeutic response to the angiogenesis inhibitor sunitinib in ovarian clear cell cancer. Clin Cancer Res. 2011;17(8):2538–48.
Mabucci S, Kawase C, Altomare DA, et al. VEGF is a promising therapeutic target for the treatment of clear cell carcinoma of the ovary. Mol Cancer Ther. 2010;9(8):2411–22.
Ji JX, Wang YK, Cochrane DR, Huntsman DG. Clear cell carcinomas of the ovary and kidney: clarity through genomics. J Pathol. 2018;244(5):550–64.
Fogli S, Porta C, Del Re M, et al. Optimizing treatment of renal cell carcinoma with VEGFR-TKIs: a comparison of clinical pharmacology and drug-drug interactions of anti-angiogenic drugs. Cancer Treat Rev. 2020;84:101966.
Ishikura N, Yorozu K, Kurasawa M, et al. Sustained effect of continuous treatment with bevacizumab following bevacizumab in combination with chemotherapy in a human ovarian clear cell carcinoma xenograft model. Oncol Rep. 2019;42(3):1057–65.
Chan JK, Brady W, Monk BJ, et al. A phase II evaluation of sunitinib in the treatment of persistent or recurrent clear cell ovarian carcinoma: an NRG Oncology/Gynecologic Oncology Group Study (GOG-254). Gynecol Oncol. 2018;150(2):247–52.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
Author information
Authors and Affiliations
Contributions
Conceptualization: AR, AG, JR-P, JB; data collection: JB, AG, JR-P; data analysis: JR-P, JB, AG; writing—original draft preparation: AG, JR-P, AR; writing—review and editing: MM, AB, GC, BC, EE, AH, DH, JF, AR; supervision: AR.
Corresponding author
Ethics declarations
Conflict of interest
AG reports honoraria and advisory/consultancy (Pharmamar), travel/accommodation/expenses (Roche, Tesaro-GSK, Pierre-Fabre, Pharmamar, MSD), speakers bureau (Roche, Clovis, Astra Zeneca, MSD), outside the submitted work. EE reports personal fees from Roche, outside the submitted work. JF reports advisory/consultancy (Amgen, Ipsen, Eisai, Merck, Roche, Novartis) and others (Amgen), outside the submitted work. AR reports honoraria and advisory/consultancy (AstraZeneca, Roche, Tesaro, Clovis, PharmaMar, Lilly, Amgen), honoraria (Eisai), research grant/funding to institution (Eisai, PharmaMar, Roche), travel/accommodation/expenses (AstraZeneca, Tesaro, PharmaMar, Roche), and others (Amgen), outside the submitted work. The remaining authors (JR-P, JB, MM, AB, GC, BC, AH, DH) have declared no conflicts of interest.
Ethics approval
The study was approved by local Ethics Committee.
Informed consent
For this type of study no informed consent is required.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Gallego, A., Ramon-Patino, J., Brenes, J. et al. Bevacizumab in recurrent ovarian cancer: could it be particularly effective in patients with clear cell carcinoma?. Clin Transl Oncol 23, 536–542 (2021). https://doi.org/10.1007/s12094-020-02446-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12094-020-02446-z