Abstract
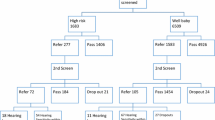
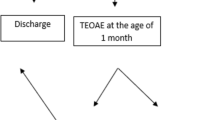
The study estimated the prevalence of hearing impairment in high-risk neonates and effect of high-risk factors on the hearing. A hospital-based cross sectional study was conducted on 327 neonates with high-risk factors. All the high-risk babies were screened using TEOAE and AABR followed by diagnostic ABR testing. Six (2%) of high-risk neonates were found to have bilateral severe sensorineural hearing loss. Risk factors associated with hearing impairment include multiple risk factors of Preterm delivery, hyperbilirubinemia, congenital anomalies, neonatal sepsis, viral or bacterial infection, positive family history of hearing loss and prolonged NICU stay. Further, the inclusion of AABR along with TEOAE has been shown to be a useful tool in reducing false-positive rates and identifying hearing loss.

Similar content being viewed by others
References
Bachmann KR, Arvedson JC (1998) Early identification and intervention for children who are hearing impaired. Pediatr Rev 1(19):155–165
Bhoovarahan S, Reddy HN (2021) Ototacoustic emissions-based hearing assessment of neonates in Tertiary Care Hospital. Indian J Otolaryngol Head Neck Surg 16:1–7
Gazia F, Abita P, Alberti G, Loteta S, Longo P, Caminiti F, Gargano R (2019) NICU Infants & SNHL: experience of a western Sicily tertiary care centre. Acta Med Mediterr 35(2):1001–1007
Garg S, Singh R, Khurana D (2015) Infant hearing screening in India: current status and way forward. Int J Prev Med. https://doi.org/10.4103/2008-7802.170027
Hajare P, Mudhol R (2021) A study of JCIH (Joint Commission on Infant Hearing) risk factors for hearing loss in babies of NICU and Well Baby Nursery at a Tertiary Care Center. Indian J Otolaryngol Head Neck Surg 15:1–8
JICH (2019) Year 2019 position statement: principles and guidelines for early hearing detection and intervention programs. J Hear Detect Interv 4(2):1–44. https://doi.org/10.15142/fptk-b748
Joint Committee on Infant Hearing (2007) Year 2007 position statement: principles and guidelines for early hearing detection and intervention programs. Pediatrics 120:898–921
Jose DJ, Renjit RE, Manonmony S (2016) Prevalence of hearing impairment among high risk neonates-A hospital based screening study. Inte J Biomed Adv Res 7(3):131–134
Joseph AY, Rasool TJ (2009) High frequency of connexin26 (GJB2) mutations associated with nonsyndromic hearing loss in the population of Kerala, India. Int J Pediatr Otorhinolaryngol 73(3):437–443
Kaveh M, Mirjalali SN, Shariat M, Zarkesh MR (2021) Perinatal factors influencing the neonatal hearing screening results. BMC Pediatr 21(1):1–6
Khaimook W, Pantuyosyanyong D, Pitathawatchai P (2019) Accuracy of otoacoustic emissions, and automated and diagnostic auditory brainstem responses, in high-risk infants. J Laryngol Otol 133(5):363–367
Kim SY, Bothwell NE, Backous DD (2002) The expanding role of the otolaryngologist in managing infants and children with hearing loss. Otolaryngol Clin North Am 35(4):699–710
Labaeka AA, Tongo OO, Ogunbosi BO, Fasunla JA (2018) Prevalence of hearing impairment among high-risk newborns in Ibadan, Nigeria. Front Pediatr 16(6):194
Martínez-Cruz CF, Poblano A, Fernández-Carrocera LA (2008) Risk factors associated with sensorineural hearing loss in infants at the neonatal intensive care unit: 15-year experience at the National Institute of Perinatology (Mexico City). Arch Med Res 39(7):686–694
Merugumala SV, Pothula V, Cooper M (2017) Barriers to timely diagnosis and treatment for children with hearing impairment in a southern Indian city: a qualitative study of parents and clinic staff. Int J Audiol 56(10):733–739
Nagapoornima P, Ramesh A, Rao S, Patricia PL, Gore M, Dominic M (2007) Universal hearing screening. Indian J Pediatr 74(6):545–549
Paul AK (2011) Early identification of hearing loss and centralized newborn hearing screening facility-the Cochin experience. Indian Pediatr 48(5):355–359
Poulakis Z, Barker M, Wake M (2003) Six month impact of false positives in an Australian infant hearing screening programme. Arch Dis Child 88(1):20–24
Ravi R, Gunjawate DR, Yerraguntla K, Rajashekhar B, Lewis LE (2016) Knowledge and attitude of parents/caregivers towards hearing loss and screening in newborns–a systematic review. Int J Audiol 55(12):715–722
Ricalde RR, Chiong CM, Labra PJ (2017) Current assessment of newborn hearing screening protocols. Curr Opin Otolaryngol Head Neck Surg 25(5):370–377
Salamy A, Eldredge L, Tooley WH (1989) Neonatal status and hearing loss in high-risk infants. J Pediatr 114(5):847–852
Schwarz Y, Kaufman GN, Daniel SJ (2017) Newborn hearing screening failure and maternal factors during pregnancy. Int J Pediatr Otorhinolaryngol 1(103):65–70
Selvarajan HG, Arunachalam RK, Bellur R, Mandke K, Nagarajan R (2013) Association of family history and consanguinity with permanent hearing impairment. Indian J Otol 19(2):62
Shetty HN, Kooknoor V, Rajalakshmi G (2016) Sensitivity and specificity of combined physiological tests in newborn hearing screening. J Phon Audiol. https://doi.org/10.4172/2471-9455.1000119
Yousefi J, Ajalloueyan M, Amirsalari S, Fard MH (2013) The specificity and sensitivity of transient otoacustic emission in neonatal hearing screening compared with diagnostic test of auditory brain stem response in Tehran hospitals. Iran J Pediatr 23(2):199
Acknowledgements
Thanks to the Gulbarga Institute of Medical Sciences, Kalaburagi, Government of Karnataka; and the All India Institute of Speech and Hearing, Mysuru under the Ministry of Health and Family Welfare, Government of India for their support.
Funding
No funding.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that there is no conflicts of interest.
Consent for publication
Consent was obtained for publication.
Ethical approval
Ethical approval was obtained from GIMS institutional ethical committee.
Consent to participate
Consent was obtained from the participants.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Appendix 1
Appendix 1

Rights and permissions
Springer Nature or its licensor holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Siddique, A.K., Melkundi, R.S., Karuppannan, A. et al. Prevalence of Hearing Impairment in High-Risk Neonates at Kalaburagi Region of Northern Karnataka: A Hospital-Based Cross-Sectional Study. Indian J Otolaryngol Head Neck Surg 75 (Suppl 1), 16–22 (2023). https://doi.org/10.1007/s12070-022-03138-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12070-022-03138-6