Abstract
Necrotising fasciitis (NF) is a rapidly progressing soft tissue infection having high risk of morbidity and mortality. Though it is a common condition encounter in surgical practice for adults, it’s incidence in children are very low. In children also abdomen is the most common site for NF. It’s involvement in head and neck is extremely rare. Here we discuss the clinical features and management of three cases of NFs in head and neck region of infants and also look for the etiology, clinical presentation and management for same.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Necrotising fasciitis (NF) is a rare, rapidly progressive, bacterial infection primarily involving the subcutaneous tissue and fascia with thrombosis of the subcutaneous blood vessels. The infection spreads rapidly through the fascial planes. Mostly caused by toxin producing virulent bacteria such as Group A streptococcus, enterobacteriaceae and non-group A streptococci. Vibrio and Aeromonas species and bacteroides are also responsible to some extent. Hippocrates was the first to recognise Necrotising fasciitis in 500 BC [1]. Wilson [2] proposed the term necrotising fasciitis in year 1950 from his observation that fascial necrosis is a constant feature of the syndrome not the cutaneous gangrene. The global prevalence of necrotising fasciitis is around 0.40 cases per 100,000 population [3]. It is very rare in children and particularly in infants. The incidence of NF in children is around 0.08 per 100,000 population. On the other hand in children, it has a fulminant course [4]. There was hardly any mention about the disease in pediatric textbooks before 1973 [5]. Although the disease affects all age groups but middle aged and elderly patients are very much prone for NF [6]. Here we describe three case of necrotising fasciitis of head and neck region in infants.
Case 1
Four months female child presented with swelling over right pinna and fever for 10 days, history of pus discharge for 5 days. On examination there was blackish discolouration of the overlying skin of right pinna, postaural region and right temporal region with oozing of foul smelling discharge. The swelling was fluctuant with multiple erythematous pustules present around it (Fig. 1). He was having haemoglobin 11.4 gm/dl and pus culture suggestive of MRSA.
Case 2
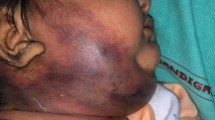
Eight months male child presented with swelling over left pre auricular region for 8 days with history of left ear discharge. He was having high grade fever since last 5 days. On examination there was an erythematous swelling over left pre-auricular area surrounded by focal erosion of the cartilaginous external auditory canal with the accumulation of purulent discharge and skin loss (Fig. 2). He was having haemoglobin 9.9 gm/dl and pus culture suggestive of Pseudomonas aeruginosa.
Case 3
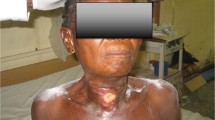
Nine months male child presented with swelling over neck since last 14 days. He was having fever since last seven days. On examination there was erythematous swelling present over the anterior neck with blackish discolouration of the overlying skin and subcutaneous tissue (Fig. 3). He was having haemoglobin 10.5 gm/dl and pus culture suggestive of Pseudomonas aeruginosa.
There is no history of any insect bite, trauma, drug allergy and all three were immunized as per the national programme schedule. All three had raised total leucocyte count and no growth was found in blood and urine culture.
Management
Debridement of the necrosed skin and subcutaneous tissue of the involved area was done under general anaesthesia until healthy margins were achieved. All three were put on intravenous antibiotics according to pus culture and sensitivity. Daily dressings was done. After improvement of the general condition, spilt skin grafting of the defect was done except case-2 which was healed by secondary intention (Figs. 4, 5, 6).
Discussion
We have focused our discussion of necrotizing fasciitis in infants only. Though lots of literature of necrotising fasciitis in adults are available, the knowledge is very scarce for children, particularly for infants. The most common site of involvement in paediatric patients is the abdominal wall followed by the thorax, back, scalp and extremities. There is no gender variation but occurs slightly more often in males [7]. It has a seasonal variation with higher incident in winter months [8]. Usually there is the presence of anaerobic bacteria that proliferate in a hypoxic environment and produce gas and accumulate in soft tissue spaces [9]. Tissue damage and systemic toxicity are believed to result from the release of endogenous cytokines and bacterial toxins. The common underlying predisposing factor for NF in children are omphalitis, mammilitis, balanitis, fetal scalp monitoring, post surgical complication, necrotising entero colitis, bullous impetigo, maternal mastitis, septicemia, immunodeficiency [10]. Fournier’s gangrene [11], Meleney’s gangrene [12], Phagadena gangrenosum, Hemolytic streptococcal gangrene, Flesh eating bacteria, Hospital gangrene are the synonyms of Necrotising fascitis described in accordance with it’s location in different region of body. Goldberg et al [13] found only 14 reported cases of NF in infants mostly resulting from circumcision or fetal scalp monitoring. Some reports also suggests the association of Haemophilus influenza type b and Chickenpox with NF [14, 15]. Fournier’s syndrome of six children aged between 3 and 12 weeks were reported by Adeyokunnu [16] where he suspected the portal of entry may be circumcision, diaper rash or may be perianal skin abscess. Necrotising enterocolitis and urachus anomalies [17] may also be responsible for NF. History of trauma which might be very minor, insect bite, unnoticed minor abrasions and lacerations may lead to development of NF [18]. Dental infections, tooth extractions, peritonsillar abscess, fracture of maxilla and mandible are some of the initiating factor for cervicofascial necrotizing fasciitis [19, 20].
Cellulitis, fever, tachycardia, swelling, skin discolouration, blistering, pain are the common clinical features of NF. Progression of the inflammation is terribly rapid. Severe sepsis, disseminated intravascular coagulation and multiple-organ failure are the late manifestation of NF.
Hundred years ago Meleny [21] recognized the importance of early surgical intervention, according to him surgery should not be delayed an hour after the diagnosis of NF has been made. At the same time one should not divert from the basic protocols like primary resuscitation and control of infection. All the discoloured, dead and necrotic tissue should be desloughed. Debridement of necrotic material must be continued until the skin and subcutaneous tissue can no longer be separated from the deep fascia [[2, 22]]. Every patients require thorough enteral or parenteral nutritional support, along with steroids and application of regional antibiotic.
Conclusion
Neonatal NF is an uncommon but often deadly bacterial infection of the skin, subcutaneous tissue. It is distinguished by obvious tissue edema, necrosis of tissue and signs of systemic toxicity. High index of suspicion, adequate antibiotics, aggressive surgical therapy and supportive care are the mainstays of management of neonatal necrotizing fasciitis.
References
Descamps V, Aitken J, Lee MG (1994) Hippocrates on necrotising fasciitis. Lancet 344:556. https://doi.org/10.1016/S0140-6736(94)91956-9
Wilson B (1952) Necrotizing fasciitis. Am Surg 18:416–431
Kaul R, McGeer A, Low DE, Green K, Schwartz B (1997) Population based surveillance for group A streptococcal necrotizing fasciitis: clinical features, prognostic indicators, and microbiologic analysis of seventy-seven cases. Ontario Group A Streptococcal Study. Am J Med 103:18–24. https://doi.org/10.1016/S0002-9343(97)00160-5
Fustes-Morales A, Gutierrez-Castrellon P, Duran-McKinster C, Orozco-Covarrubias L, Tamayo-Sanchez L, Ruiz-Maldonado R (2002) Necrotizing fascii-tis: report of 390 pediatric cases. Arch Dermatol 138:893–899
David WH (1973) Acute necrotizing fasciitis in childhood. Am J Dis Child 125(4):591. https://doi.org/10.1001/archpedi.1973.04160040087018
Misiakos EP, Bagias G, Patapis P, Sotiropoulos D, Kanavidis P, Machairas A (2014) Current concepts in the management of necrotizing fasciitis. Front Surg 1:36. https://doi.org/10.3389/fsurg.2014.00036
Hsieh WS, Yang PH, Chao HC, Lai JY (1999) Neonatal necrotizing fasciitis: a report of three cases and review of the literature. Paediatrics 103:e53
Luca-Harari B, Ekelund K, van der Linden M, Staum-Kaltoft M, Hammerum AM, Jasir A (2008) Clinical and epidemiological aspects of invasive Streptococcus pyogenes infections in Denmark during 2003 and 2004. J Clin Microbiol 46:79–86
Kaafarani HM, King DR (2014) Necrotizing skin and soft tissue infections. Surg Clin North Am 94:155–163. https://doi.org/10.1016/j.suc.2013.10.011
American Academy of Pediatrics (1998) Committee on infectious diseases. Severe invasive group A streptococcal infections: a subject review. Pediatrics 101:136–140
Fournier JA (1883) Gangrene foudroyante de la verge. Med Pract 4:589–597
Brewer GE, Meleney FL (1926) Progressive gangrenous infection of the skin and subcutaneous tissues, following operation for acute perforative appendicitis: a study in symbiosis. Ann Surg 84:438–450. https://doi.org/10.1097/00000658-192684030-00017
Goldberg GN, Hansen RC, Lynch DJ (1984) Necrotising fasciitis in infancy: report of three cases and review of the literature. Pediatr Dermatol 2:55–63
Collette CJ, Southerland D, Corrall CJ (1987) Necrotising fasciitis associated with Haemophilus influenzae type b. Am J Dis Child 141:1146–1148
Falcone PA, Pricolo VE, Edstorm LE (1988) Necrotising fasciitis as a complication of chicken pox. Clin Pediatr 27:339–343
Adeyokunnu AA (1983) Fournier's syndrome in infants. A review of cases from Ibadan, Nigeria. Clin Pediatr 22:101–103
Kosloske AM, Cushing AH, Borden TA, Woodside JR, Klein MD, Kulasinghe HP et al (1981) Cellulitis and necrotising fasciitis of the abdominal wall in pediatric patients. J Pediatr Surg 16:246–251
Rea WJ, Wyrick WJ (1970) Necrotising fasciitis. Ann Surg 172:957–964
Wenig BL, Shikowitz MJ, Abramson AL (1984) Necrotising fasciitis as a lethal complication of peritionsillar abscess. Laryngosc 94:1576–1579
Crowson WN (1973) Fatal necrotising fasciitis developing after tooth extraction. Am Surg 39:525–527
Meleney FL (1933) A differential diagnosis between certain types of infectious gangrene of the skin—with particular reference to hemolytic streptococcus gangrene and bacterial synergistic gangrene. Surg Gynecol Obstet 56:847–867
Kaiser RE, Cerra FB (1981) Progressive necrotising surgical infections—a unified approach. J Trauma 21:349–355
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflicts of Interest.
Ethics Approval
In our articles the management was well established in literature and standard text books. Our institute ethics committee has confirmed that no ethical approval is required.
Informed Consent
Written Informed consent was obtained from the parents.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Sahoo, A., Singh, I., Dhakal, S. et al. Necrotising Fasciitis of Head and Neck in Infants. Indian J Otolaryngol Head Neck Surg 74 (Suppl 2), 2049–2052 (2022). https://doi.org/10.1007/s12070-020-01992-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12070-020-01992-w