Abstract
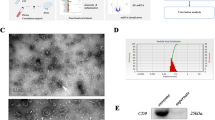
Intraventricular or intrathecal administration of polymyxins are increasingly used to treat multidrug-resistant (MDR) Gram-negative bacteria caused infections in the central nervous system (CNS). However, our limited knowledge of the mechanisms underpinning polymyxin-induced neurotoxicity significantly hinders the development of safe and efficacious polymyxin dosing regimens. To this end, we conducted transcriptomic analyses of the rat brain and spinal cord 1 h following intracerebroventricular administration of polymyxin B into rat lateral ventricle at a clinically relevant dose (0.5 mg/kg). Following the treatment, 66 differentially expressed genes (DEGs) were identified in the brain transcriptome while none for the spinal cord (FDR ≤ 0.05, fold-change ≥ 1.5). DEGs were enriched in signaling pathways associated with hormones and neurotransmitters, including dopamine and (nor)epinephrine. Notably, the expression levels of Slc6a3 and Gabra6 were decreased by 20-fold and 4.3-fold, respectively, likely resulting in major perturbations of dopamine and γ-aminobutyric acid signaling in the brain. Mass spectrometry imaging of brain sections revealed a distinct pattern of polymyxin B distribution with the majority accumulating in the injection-side lateral ventricle and subsequently into third and fourth ventricles. Polymyxin B was not detectable in the left lateral ventricle or brain tissue. Electrophysiological measurements on primary cultured rat neurons revealed a large inward current and significant membrane leakage following polymyxin B treatment. Our work demonstrates, for the first time, the key CNS signaling pathways associated with polymyxin neurotoxicity. This mechanistic insight combined with pharmacokinetic/pharmacodynamic dosing strategies will help guide the design of safe and effective intraventricular/intrathecal polymyxin treatment regimens for CNS infections caused by MDR Gram-negative pathogens.






Similar content being viewed by others
Data Availability
The datasets used and/or analyzed during the current study are available from the corresponding author on reasonable request.
References
Serra-Burriel M, Keys M, Campillo-Artero C, Agodi A, Barchitta M, Gikas A, Palos C, Lopez-Casasnovas G (2020) Impact of multi-drug resistant bacteria on economic and clinical outcomes of healthcare-associated infections in adults: systematic review and meta-analysis. PLoS ONE 15(1):e0227139. https://doi.org/10.1371/journal.pone.0227139
Velkov T, Dai C, Ciccotosto GD, Cappai R, Hoyer D, Li J (2018) Polymyxins for CNS infections: pharmacology and neurotoxicity. Pharmacol Ther 181:85–90. https://doi.org/10.1016/j.pharmthera.2017.07.012
Bergen PJ, Li J, Rayner CR, Nation RL (2006) Colistin methanesulfonate is an inactive prodrug of colistin against Pseudomonas aeruginosa. Antimicrob Agents Chemother 50(6):1953–1958. https://doi.org/10.1128/AAC.00035-06
Li Z, Velkov T (2019) Polymyxins: mode of action. Adv Exp Med Biol 1145:37–54. https://doi.org/10.1007/978-3-030-16373-0_4
Zhu Y, Lu J, Han ML, Jiang X, Azad MAK, Patil NA, Lin YW, Zhao J, Hu Y, Yu HH, Chen K, Boyce JD, Dunstan RA, Lithgow T, Barlow CK, Li W, Schneider-Futschik EK, Wang J, Gong B, Sommer B, Creek DJ, Fu J, Wang L, Schreiber F, Velkov T, Li J (2020) Polymyxins bind to the cell surface of unculturable Acinetobacter baumannii and cause unique dependent resistance. Adv Sci (Weinh) 7(15):2000704. https://doi.org/10.1002/advs.202000704
Pardridge WM (2012) Drug transport across the blood-brain barrier. J Cereb Blood Flow Metab 32(11):1959–1972. https://doi.org/10.1038/jcbfm.2012.126
Azad MAK, Nation RL, Velkov T, Li J (2019) Mechanisms of polymyxin-induced nephrotoxicity. Adv Exp Med Biol 1145:305–319. https://doi.org/10.1007/978-3-030-16373-0_18
Remes F, Tomas R, Jindrak V, Vanis V, Setlik M (2013) Intraventricular and lumbar intrathecal administration of antibiotics in postneurosurgical patients with meningitis and/or ventriculitis in a serious clinical state. J Neurosurg 119(6):1596–1602. https://doi.org/10.3171/2013.6.JNS122126
Pan S, Huang X, Wang Y, Li L, Zhao C, Yao Z, Cui W, Zhang G (2018) Efficacy of intravenous plus intrathecal/intracerebral ventricle injection of polymyxin B for post-neurosurgical intracranial infections due to MDR/XDR Acinectobacter baumannii: a retrospective cohort study. Antimicrob Resist Infect Control 7:8. https://doi.org/10.1186/s13756-018-0305-5
Sayyahfar S, Choobdar FA, Mashayekhi M, Jazi FM (2021) Successful management of pan-resistant Acinetobacter baumannii meningitis without intrathecal or intraventricular antibiotic therapy in a neonate. Infect Chemother 53(1):146–150. https://doi.org/10.3947/ic.2020.0202
Ng J, Gosbell IB, Kelly JA, Boyle MJ, Ferguson JK (2006) Cure of multiresistant Acinetobacter baumannii central nervous system infections with intraventricular or intrathecal colistin: case series and literature review. J Antimicrob Chemother 58(5):1078–1081. https://doi.org/10.1093/jac/dkl347
Karaiskos I, Galani L, Baziaka F, Katsouda E, Ioannidis I, Andreou A, Paskalis H, Giamarellou H (2013) Successful treatment of extensively drug-resistant Acinetobacter baumannii ventriculitis and meningitis with intraventricular colistin after application of a loading dose: a case series. Int J Antimicrob Agents 41(5):480–483. https://doi.org/10.1016/j.ijantimicag.2013.02.010
Lopez-Alvarez B, Martin-Laez R, Farinas MC, Paternina-Vidal B, Garcia-Palomo JD, Vazquez-Barquero A (2009) Multidrug-resistant Acinetobacter baumannii ventriculitis: successful treatment with intraventricular colistin. Acta Neurochir (Wien) 151(11):1465–1472. https://doi.org/10.1007/s00701-009-0382-6
Sueke H, Marsh H, Dhital A (2005) Using intrathecal colistin for multidrug resistant shunt infection. Br J Neurosurg 19(1):51–52. https://doi.org/10.1080/02688690500080729
Dai C, Ciccotosto GD, Cappai R, Tang S, Li D, Xie S, Xiao X, Velkov T (2018) Curcumin attenuates colistin-induced neurotoxicity in N2a cells via anti-inflammatory activity, suppression of oxidative stress, and apoptosis. Mol Neurobiol 55(1):421–434. https://doi.org/10.1007/s12035-016-0276-6
Dai C, Ciccotosto GD, Cappai R, Wang Y, Tang S, Hoyer D, Schneider EK, Velkov T, Xiao X (2018) Rapamycin confers neuroprotection against colistin-induced oxidative stress, mitochondria dysfunction, and apoptosis through the activation of autophagy and mTOR/Akt/CREB signaling pathways. ACS Chem Neurosci 9(4):824–837. https://doi.org/10.1021/acschemneuro.7b00323
Dai C, Ciccotosto GD, Cappai R, Wang Y, Tang S, Xiao X, Velkov T (2017) Minocycline attenuates colistin-induced neurotoxicity via suppression of apoptosis, mitochondrial dysfunction and oxidative stress. J Antimicrob Chemother 72(6):1635–1645. https://doi.org/10.1093/jac/dkx037
Dai C, Tang S, Biao X, Xiao X, Chen C, Li J (2019) Colistin induced peripheral neurotoxicity involves mitochondrial dysfunction and oxidative stress in mice. Mol Biol Rep 46(2):1963–1972. https://doi.org/10.1007/s11033-019-04646-5
Dai C, Tang S, Velkov T, Xiao X (2016) Colistin-induced apoptosis of neuroblastoma-2a cells involves the generation of reactive oxygen species, mitochondrial dysfunction, and autophagy. Mol Neurobiol 53(7):4685–4700. https://doi.org/10.1007/s12035-015-9396-7
Xing H, Cheng C, Zhang Y, Cai Y, Wang X, Deng D, Xu L, Xu M, Chen J (2021) Successful treatment with intrathecal and intravenous polymyxin B-based combination against MDR Acinetobacter baumannii meningitis in pediatric patient: a case report. Front Pediatr 9:564991. https://doi.org/10.3389/fped.2021.564991
Yu X, Huang Y, Zhang X, Wang Y, Shi D, Zhang C, Chen J, Wang X, Lin G (2022) Intraventricular colistin sulphate as a last resort therapy in a patient with multidrug-resistant Acinetobacter baumannii induced post-neurosurgical ventriculitis. Br J Clin Pharmacol 88(7):3490–3494. https://doi.org/10.1111/bcp.15238
Oberrauch S, Lu J, Cornthwaite-Duncan L, Hussein M, Li J, Rao G, Velkov T (2022) Intraventricular drug delivery and sampling for pharmacokinetics and pharmacodynamics study. J Vis Exp (181):e63540. https://doi.org/10.3791/63540
Pristupa ZB, Wilson JM, Hoffman BJ, Kish SJ, Niznik HB (1994) Pharmacological heterogeneity of the cloned and native human dopamine transporter: disassociation of [3H]WIN 35,428 and [3H]GBR 12,935 binding. Mol Pharmacol 45(1):125–135
Mishra A, Singh S, Shukla S (2018) Physiological and functional basis of dopamine receptors and their role in neurogenesis: possible implication for Parkinson’s disease. J Exp Neurosci 12:1179069518779829. https://doi.org/10.1177/1179069518779829
Schwartz RD (1988) The GABAA receptor-gated ion channel: biochemical and pharmacological studies of structure and function. Biochem Pharmacol 37(18):3369–3375. https://doi.org/10.1016/0006-2952(88)90684-3
Jie F, Yin G, Yang W, Yang M, Gao S, Lv J, Li B (2018) Stress in regulation of GABA amygdala system and relevance to neuropsychiatric diseases. Front Neurosci 12:562. https://doi.org/10.3389/fnins.2018.00562
Diaz-Rodriguez SM, Lopez-Lopez D, Herrero-Turrion MJ, Gomez-Nieto R, Canal-Alonso A, Lopez DE (2020) Inferior colliculus transcriptome after status epilepticus in the genetically audiogenic seizure-prone hamster GASH/Sal. Front Neurosci 14:508. https://doi.org/10.3389/fnins.2020.00508
Hammaren HM, Virtanen AT, Raivola J, Silvennoinen O (2019) The regulation of JAKs in cytokine signaling and its breakdown in disease. Cytokine 118:48–63. https://doi.org/10.1016/j.cyto.2018.03.041
Smith JR, Hayman GT, Wang SJ, Laulederkind SJF, Hoffman MJ, Kaldunski ML, Tutaj M, Thota J et al (2020) The year of the rat: the rat genome database at 20: a multi-species knowledgebase and analysis platform. Nucleic Acids Res 48(D1):D731–D742. https://doi.org/10.1093/nar/gkz1041
Waterhouse BD, Navarra RL (2019) The locus coeruleus-norepinephrine system and sensory signal processing: a historical review and current perspectives. Brain Res 1709:1–15. https://doi.org/10.1016/j.brainres.2018.08.032
Biason-Lauber A, Boscaro M, Mantero F, Balercia G (2010) Defects of steroidogenesis. J Endocrinol Invest 33(10):756–766. https://doi.org/10.3275/686910.1007/BF03346683
Busada JT, Peterson KN, Khadka S, Xu X, Oakley RH, Cook DN, Cidlowski JA (2021) Glucocorticoids and androgens protect from gastric metaplasia by suppressing group 2 innate lymphoid cell activation. Gastroenterology 161(2):637–652. https://doi.org/10.1053/j.gastro.2021.04.075
Petrova R, Joyner AL (2014) Roles for Hedgehog signaling in adult organ homeostasis and repair. Development 141(18):3445–3457. https://doi.org/10.1242/dev.083691
Raudvere U, Kolberg L, Kuzmin I, Arak T, Adler P, Peterson H, Vilo J (2019) g:Profiler: a web server for functional enrichment analysis and conversions of gene lists (2019 update). Nucleic Acids Res 47(W1):W191–W198. https://doi.org/10.1093/nar/gkz369
Paxinos C, Watson W (2014) The rat brain in stereotaxic coordinates. Elsevier
Nang SC, Azad MAK, Velkov T, Zhou QT, Li J (2021) Rescuing the last-line polymyxins: achievements and challenges. Pharmacol Rev 73(2):679–728. https://doi.org/10.1124/pharmrev.120.000020
Jimenez-Mejias ME, Pichardo-Guerrero C, Marquez-Rivas FJ, Martin-Lozano D, Prados T, Pachon J (2002) Cerebrospinal fluid penetration and pharmacokinetic/pharmacodynamic parameters of intravenously administered colistin in a case of multidrug-resistant Acinetobacter baumannii meningitis. Eur J Clin Microbiol 21(3):212–214. https://doi.org/10.1007/s10096-001-0680-2
Jin L, Li J, Nation RL, Nicolazzo JA (2009) Brain penetration of colistin in mice assessed by a novel high-performance liquid chromatographic technique. Antimicrob Agents Chemother 53(10):4247–4251. https://doi.org/10.1128/AAC.00485-09
Markantonis SL, Markou N, Fousteri M, Sakellaridis N, Karatzas S, Alamanos I, Dimopoulou E, Baltopoulos G (2009) Penetration of colistin into cerebrospinal fluid. Antimicrob Agents Chemother 53(11):4907–4910. https://doi.org/10.1128/AAC.00345-09
Version 12.0 (2022) The European committee on antimicrobial susceptibility testing. Breakpoint tables for interpretation of MICs and zone diameters. http://www.eucast.org. Accessed 1 Jan 2022
Tunkel AR, Hartman BJ, Kaplan SL, Kaufman BA, Roos KL, Scheld WM, Whitley RJ (2004) Practice guidelines for the management of bacterial meningitis. Clin Infect Dis 39(9):1267–1284. https://doi.org/10.1086/425368
Ziaka M, Markantonis SL, Fousteri M, Zygoulis P, Panidis D, Karvouniaris M, Makris D, Zakynthinos E (2013) Combined intravenous and intraventricular administration of colistin methanesulfonate in critically ill patients with central nervous system infection. Antimicrob Agents Chemother 57(4):1938–1940. https://doi.org/10.1128/AAC.01461-12
Dudhani RV, Turnidge JD, Nation RL, Li J (2010) fAUC/MIC is the most predictive pharmacokinetic/pharmacodynamic index of colistin against Acinetobacter baumannii in murine thigh and lung infection models. J Antimicrob Chemother 65(9):1984–1990. https://doi.org/10.1093/jac/dkq226
Bergen PJ, Bulitta JB, Forrest A, Tsuji BT, Li J, Nation RL (2010) Pharmacokinetic/pharmacodynamic investigation of colistin against Pseudomonas aeruginosa using an in vitro model. Antimicrob Agents Chemother 54(9):3783–3789. https://doi.org/10.1128/AAC.00903-09
Imberti R, Cusato M, Accetta G, Marino V, Procaccio F, Del Gaudio A, Iotti GA, Regazzi M (2012) Pharmacokinetics of colistin in cerebrospinal fluid after intraventricular administration of colistin methanesulfonate. Antimicrob Agents Chemother 56(8):4416–4421. https://doi.org/10.1128/AAC.00231-12
Mohammed N, Savardekar AR, Patra DP, Narayan V, Nanda A (2017) The 21st-century challenge to neurocritical care: the rise of the superbug Acinetobacter baumannii. A meta-analysis of the role of intrathecal or intraventricular antimicrobial therapy in reduction of mortality. Neurosurg Focus 43(5):E8. https://doi.org/10.3171/2017.8.Focus17443
Couet W, Gregoire N, Gobin P, Saulnier PJ, Frasca D, Marchand S, Mimoz O (2011) Pharmacokinetics of colistin and colistimethate sodium after a single 80-mg intravenous dose of CMS in young healthy volunteers. Clin Pharmacol Ther 89(6):875–879. https://doi.org/10.1038/clpt.2011.48
Karaiskos I, Galani L, Baziaka F, Giamarellou H (2013) Intraventricular and intrathecal colistin as the last therapeutic resort for the treatment of multidrug-resistant and extensively drug-resistant Acinetobacter baumannii ventriculitis and meningitis: a literature review. Int J Antimicrob Agents 41(6):499–508. https://doi.org/10.1016/j.ijantimicag.2013.02.006
Chen L, Li X, Li D, Dong X, Chen H (2022) Efficacy and safety of intraventricular polymyxin B plus continuous ventricular drainage for the treatment of intracranial infection caused by drug-resistant Acinetobacter baumannii. Ann Palliat Med 11(2):490–497. https://doi.org/10.21037/apm-21-3149
Li Z, An Y, Li L, Yi H (2022) Intrathecal injection of tigecycline and polymyxin B in the treatment of extensively drug-resistant intracranial Acinetobacter baumannii infection: a case report and review of the literature. Infect Drug Resist 15:1411–1423. https://doi.org/10.2147/IDR.S354460
Takamata A, Seo Y, Ogino T, Tanaka K, Fujiki N, Morita H, Murakami M (2001) Effects of pCO(2) on the CSF turnover rate in T(1)-weighted magnetic resonance imaging. Jpn J Physiol 51(5):555–562. https://doi.org/10.2170/jjphysiol.51.555
Sakka L, Coll G, Chazal J (2011) Anatomy and physiology of cerebrospinal fluid. Eur Ann Otorhinolaryngol Head Neck Dis 128(6):309–316. https://doi.org/10.1016/j.anorl.2011.03.002
Spector S, Sjoerdsma A, Udenfriend S (1965) Blockade of endogenous norepinephrine synthesis by alpha-methyl-tyrosine, an inhibitor of tyrosine hydroxylase. J Pharmacol Exp Ther 147:86–95
Brouwer M, McIntyre P, Prasad K, van de Beek D (2015) Corticosteroids for acute bacterial meningitis. Cochrane Database Syst Rev 2015(9):CD004405. https://doi.org/10.1002/14651858.CD004405.pub5
Bertelli A, Soldani G (1979) Polymyxin B-induced oedema in hind paw of the rat as an assay for antiinflammatory drugs. Arzneimittelforschung 29(5):777–778
Salman MM, Kitchen P, Halsey A, Wang MX, Tornroth-Horsefield S, Conner AC, Badaut J, Iliff JJ, Bill RM (2022) Emerging roles for dynamic aquaporin-4 subcellular relocalization in CNS water homeostasis. Brain 145(1):64–75. https://doi.org/10.1093/brain/awab311
Nakamura T, Fujiwara N, Sato E, Kawagoe Y, Ueda Y, Yamada S, Koide H (2009) Effect of polymyxin B-immobilized fiber hemoperfusion on serum high mobility group box-1 protein levels and oxidative stress in patients with acute respiratory distress syndrome. ASAIO J 55(4):395–399. https://doi.org/10.1097/MAT.0b013e3181a5290f
Nishizaki N, Shima T, Watanabe A, Obinata K, Shimizu T (2021) Unsatisfactory short-term neurodevelopmental outcomes of preterm infants who received polymyxin B-Immobilized fiber column-direct hemoperfusion for septic shock. Tohoku J Exp Med 253(4):275–281. https://doi.org/10.1620/tjem.253.275
Roberts KD, Zhu Y, Azad MAK, Han ML, Wang J, Wang L, Yu HH, Horne AS et al (2022) A synthetic lipopeptide targeting top-priority multidrug-resistant Gram-negative pathogens. Nat Commun 13(1):1625. https://doi.org/10.1038/s41467-022-29234-3
Cornett DS, Reyzer ML, Chaurand P, Caprioli RM (2007) MALDI imaging mass spectrometry: molecular snapshots of biochemical systems. Nat Methods 4(10):828–833. https://doi.org/10.1038/nmeth1094
Castellino S, Groseclose MR, Wagner D (2011) MALDI imaging mass spectrometry: bridging biology and chemistry in drug development. Bioanalysis 3(21):2427–2441. https://doi.org/10.4155/bio.11.232
Brinker T, Stopa E, Morrison J, Klinge P (2014) A new look at cerebrospinal fluid circulation. Fluids Barriers Cns 11:10. https://doi.org/10.1186/2045-8118-11-10
Lu J, Azad MAK, Moreau JLM, Zhu Y, Jiang X, Tonta M, Lam R, Wickremasinghe H et al (2022) Inwardly rectifying potassium channels mediate polymyxin-induced nephrotoxicity. Cell Mol Life Sci 79(6):296. https://doi.org/10.1007/s00018-022-04316-z
Wevers NR, Kasi DG, Gray T, Wilschut KJ, Smith B, van Vught R, Shimizu F, Sano Y et al (2018) A perfused human blood-brain barrier on-a-chip for high-throughput assessment of barrier function and antibody transport. Fluids Barriers Cns 15(1):23. https://doi.org/10.1186/s12987-018-0108-3
Salman MM, Marsh G, Kusters I, Delince M, Di Caprio G, Upadhyayula S, de Nola G, Hunt R et al (2020) Design and validation of a human brain endothelial microvessel-on-a-chip open microfluidic model enabling advanced optical imaging. Front Bioeng Biotechnol 8:573775. https://doi.org/10.3389/fbioe.2020.573775
Aldewachi H, Al-Zidan RN, Conner MT, Salman MM (2021) High-throughput screening platforms in the discovery of novel drugs for neurodegenerative diseases. Bioengineering (Basel) 8(2):30. https://doi.org/10.3390/bioengineering8020030
Salman MM, Al-Obaidi Z, Kitchen P, Loreto A, Bill RM, Wade-Martins R (2021) Advances in applying computer-aided drug design for neurodegenerative diseases. Int J Mol Sci 22(9):4688. https://doi.org/10.3390/ijms22094688
DeVos SL, Miller TM (2013) Direct intraventricular delivery of drugs to the rodent central nervous system. J Vis Exp 75:e50326. https://doi.org/10.3791/50326
Lu J, Zhu Y, Williams S, Watts M, Tonta MA, Coleman HA, Parkington HC, Claudianos C (2020) Autism-associated miR-873 regulates ARID1B, SHANK3 and NRXN2 involved in neurodevelopment. Transl Psychiatry 10(1):418. https://doi.org/10.1038/s41398-020-01106-8
Liao Y, Smyth GK, Shi W (2014) featureCounts: an efficient general purpose program for assigning sequence reads to genomic features. Bioinformatics 30(7):923–930. https://doi.org/10.1093/bioinformatics/btt656
Ritchie ME, Phipson B, Wu D, Hu Y, Law CW, Shi W, Smyth GK (2015) limma powers differential expression analyses for RNA-sequencing and microarray studies. Nucleic Acids Res 43(7):e47. https://doi.org/10.1093/nar/gkv007
Yu G, Wang LG, Han Y, He QY (2012) clusterProfiler: an R package for comparing biological themes among gene clusters. OMICS 16(5):284–287. https://doi.org/10.1089/omi.2011.0118
Shannon P, Markiel A, Ozier O, Baliga NS, Wang JT, Ramage D, Amin N, Schwikowski B et al (2003) Cytoscape: a software environment for integrated models of biomolecular interaction networks. Genome Res 13(11):2498–2504. https://doi.org/10.1101/gr.1239303
Funding
This research was supported by the National Institute of Allergy and Infectious Diseases (NIAID) of the National Institutes of Health (NIH, R01 AI132154 to GR and TV). G.G.R., T.V., and J.L. are supported by the National Institute of Allergy and Infectious Diseases, award number R01AI146241. The content is solely the responsibility of the authors and does not necessarily represent the official views of the NIAID or NIH.
Author information
Authors and Affiliations
Contributions
T.V., J.L., and G.G.R conceived and supervised the project and were involved in manuscript editing. J.Lu conducted the experiment and wrote the manuscript. Y.Z analyzed the RNA-seq data. S.O and L.C conducted the surgery on the animals. H.P and M.T conducted and analyzed the electrophysiology measurements. D.R. conducted the MALDI-MS imaging experiment. P.B, M.H, R.S., and R.A were involved in project discussions and manuscript editing. All authors reviewed and agreed to the final manuscript.
Corresponding authors
Ethics declarations
Ethics Approval
All animal experiments were approved by the University of Melbourne ethics committee (Number #1914890). All animal experiments were conducted in accordance with the Australian code for the care and use of animals for scientific purposes.
Consent to Participate
Not applicable.
Consent for Publication
All authors reviewed and agreed to the final manuscript to publish.
Competing Interests
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Lu, J., Zhu, Y., Parkington, H.C. et al. Transcriptomic Mapping of Neurotoxicity Pathways in the Rat Brain in Response to Intraventricular Polymyxin B. Mol Neurobiol 60, 1317–1330 (2023). https://doi.org/10.1007/s12035-022-03140-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12035-022-03140-7