Abstract
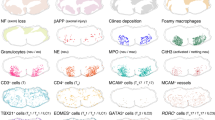
Angiostrongylus cantonensis infection is a typical cause of eosinophilic encephalitis (EM), which has been reported to induce serious damage in the central nervous system. Both parasite and host factors contribute to the onset of EM, but the related immune-inflammation pathogenesis remains poorly characterised. An A. cantonensis infection model was generated through the infection of mice by gavage. Transmission electron microscopy and immunohistochemistry were used to assess the pathologic changes in the brain. The mRNA expression of inflammatory factors was tested using qRT-PCR. A combination of flow cytometry and western blotting was used to evaluate the alteration of leukocytes and related cytokines. A critical role of IL-17 was found by injecting IL-17A monoclonal antibody into naïve and A. cantonensis-infected mice. A. cantonensis larvae altered the immune homeostasis in the brain, leading to the destruction of myelin sheaths and activation of microglia and macrophage. During this process, IL-17A accumulation was observed, and IL-17RA was expressed in oligodendrocytes and microglia during the infection. Notably, γδ T cell was the major origin of IL-17A production induced by the parasite. After an IL-17A-neutralising antibody was applied, alterations in myelination and the state of the microglia/macrophage were discovered; the neurobehavioural scores of the mice also improved. Our study reveals one unrecognised impact of the γδ T cells in parasitic encephalopathy and emphasises that blocking IL-17A signalling can attenuate microglia and macrophage activation, thus reducing CNS demyelination and ameliorating the neurobehavioural deficit in A. cantonensis-infected mice.






Similar content being viewed by others
Data Availability
The research article data used to support the findings of this study are included within the article.
References
Wan S, Sun X, Wu F, Yu Z, Wang L, Lin D et al (2018) Chi3l3: a potential key orchestrator of eosinophil recruitment in meningitis induced by Angiostrongylus cantonensis. J Neuroinflammation 15:1–31. https://doi.org/10.1186/s12974-018-1071-2
Wang QP, Lai DH, Zhu XQ, Chen XG, Lun ZR (2008) Human angiostrongyliasis. Lancet Infect Dis 8(10):621–630. https://doi.org/10.1016/S1473-3099(08)70229-9
Barratt J, Chan D, Sandaradura I, Malik R, Spielman D, Lee R et al (2016) Angiostrongylus cantonensis: a review of its distribution, molecular biology and clinical significance as a human pathogen. Parasitology. 143(9):1087–1118. https://doi.org/10.1017/S0031182016000652
Hidelaratchi MD, Riffsy MT, Wijesekera JC (2005) A case of eosinophilic meningitis following monitor lizard meat consumption, exacerbated by anthelminthics. Ceylon Med J 50(2):84–86. https://doi.org/10.4038/cmj.v50i2.1577
Chotmongkol V, Sawanyawisuth K (2002) Clinical manifestations and outcome of patients with severe eosinophilic meningoencephalitis presumably caused by Angiostrongylus cantonensis. Southeast Asian J Trop Med Public Health 33(2):231–234
Reynolds JM, Angkasekwinai P, Dong C (2010) IL-17 family member cytokines: regulation and function in innate immunity. Cytokine Growth Factor Rev 21(6):413–423. https://doi.org/10.1016/j.cytogfr.2010.10.002
Paintlia MK, Paintlia AS, Singh AK, Singh I (2011) Synergistic activity of interleukin-17 and tumor necrosis factor-alpha enhances oxidative stress-mediated oligodendrocyte apoptosis. J Neurochem 116(4):508–521. https://doi.org/10.1111/j.1471-4159.2010.07136.x
Zimmermann J, Krauthausen M, Hofer MJ, Heneka MT, Campbell IL, Muller M (2013) CNS-targeted production of IL-17A induces glial activation, microvascular pathology and enhances the neuroinflammatory response to systemic endotoxemia. PLoS One 8(2):e57307. https://doi.org/10.1371/journal.pone.0057307
Gaffen SL (2009) Structure and signalling in the IL-17 receptor family. Nat Rev Immunol 9(8):556–567. https://doi.org/10.1038/nri2586
Kim CF, Moalem-Taylor G (2011) Interleukin-17 contributes to neuroinflammation and neuropathic pain following peripheral nerve injury in mice. J Pain 12(3):370–383. https://doi.org/10.1016/j.jpain.2010.08.003
Chang SH, Dong C (2007) A novel heterodimeric cytokine consisting of IL-17 and IL-17F regulates inflammatory responses. Cell Res 17(5):435–440. https://doi.org/10.1038/cr.2007.35
Kipnis J (2016) Multifaceted interactions between adaptive immunity and the central nervous system. Science. 353(6301):766–771. https://doi.org/10.1126/science.aag2638
Hayday AC (2000) [gamma][delta] cells: a right time and a right place for a conserved third way of protection. Annu Rev Immunol 18:975–1026. https://doi.org/10.1146/annurev.immunol.18.1.975
Hayday AC (2009) Gammadelta T cells and the lymphoid stress-surveillance response. Immunity. 31(2):184–196. https://doi.org/10.1016/j.immuni.2009.08.006
Petermann F, Rothhammer V, Claussen MC, Haas JD, Blanco LR, Heink S et al (2010) gammadelta T cells enhance autoimmunity by restraining regulatory T cell responses via an interleukin-23-dependent mechanism. Immunity 33(3):351–363. https://doi.org/10.1016/j.immuni.2010.08.013
Sutton CE, Lalor SJ, Sweeney CM, Brereton CF, Lavelle EC, Mills KH (2009) Interleukin-1 and IL-23 induce innate IL-17 production from gammadelta T cells, amplifying Th17 responses and autoimmunity. Immunity. 31(2):331–341. https://doi.org/10.1016/j.immuni.2009.08.001
Kawanokuchi J, Shimizu K, Nitta A, Yamada K, Mizuno T, Takeuchi H, Suzumura A (2008) Production and functions of IL-17 in microglia. J Neuroimmunol 194(1-2):54–61. https://doi.org/10.1016/j.jneuroim.2007.11.006
Lv M, Liu Y, Zhang J, Sun L, Liu Z, Zhang S, Wang B, Su D et al (2011) Roles of inflammation response in microglia cell through Toll-like receptors 2/interleukin-23/interleukin-17 pathway in cerebral ischemia/reperfusion injury. Neuroscience. 176:162–172. https://doi.org/10.1016/j.neuroscience.2010.11.066
Parra A, McGirt MJ, Sheng H, Laskowitz DT, Pearlstein RD, Warner DS (2002) Mouse model of subarachnoid hemorrhage associated cerebral vasospasm: methodological analysis. Neurol Res 24(5):510–516. https://doi.org/10.1179/016164102101200276
OuYang L, Wei J, Wu Z, Zeng X, Li Y, Jia Y, Ma Y, Zhan M et al (2012) Differences of larval development and pathological changes in permissive and nonpermissive rodent hosts for Angiostrongylus cantonensis infection. Parasitol Res 111(4):1547–1557. https://doi.org/10.1007/s00436-012-2995-6
Miron VE, Boyd A, Zhao JW, Yuen TJ, Ruckh JM, Shadrach JL, van Wijngaarden P, Wagers AJ et al (2013) M2 microglia and macrophages drive oligodendrocyte differentiation during CNS remyelination. Nat Neurosci 16(9):1211–1218. https://doi.org/10.1038/nn.3469
Ying F, Cunjing Z, Feng F, Shuo W, Xin Z, Fukang X et al (2017) Inhibiting interleukin 17 can ameliorate the demyelination caused by A. cantonensis via iNOS inhibition. Mediat Inflamm 2017:3513651. https://doi.org/10.1155/2017/3513651
Zimmermann J, Emrich M, Krauthausen M, Saxe S, Nitsch L, Heneka MT, Campbell IL, Müller M (2018) IL-17A Promotes granulocyte infiltration, myelin loss, microglia activation, and behavioral deficits during cuprizone-induced demyelination. Mol Neurobiol 55(2):946–957. https://doi.org/10.1007/s12035-016-0368-3
Wang C, Zhang CJ, Martin BN, Bulek K, Kang Z, Zhao J, Bian G, Carman JA et al (2017) IL-17 induced NOTCH1 activation in oligodendrocyte progenitor cells enhances proliferation and inflammatory gene expression. Nat Commun 8:15508. https://doi.org/10.1038/ncomms15508
Murphy AC, Lalor SJ, Lynch MA, Mills KH (2010) Infiltration of Th1 and Th17 cells and activation of microglia in the CNS during the course of experimental autoimmune encephalomyelitis. Brain Behav Immun 24(4):641–651. https://doi.org/10.1016/j.bbi.2010.01.014
Shichita T, Sugiyama Y, Ooboshi H, Sugimori H, Nakagawa R, Takada I, Iwaki T, Okada Y et al (2009) Pivotal role of cerebral interleukin-17-producing gammadeltaT cells in the delayed phase of ischemic brain injury. Nat Med 15(8):946–950. https://doi.org/10.1038/nm.1999
Chen AL, Sun X, Wang W, Liu JF, Zeng X, Qiu JF et al (2016) Activation of the hypothalamic-pituitary-adrenal (HPA) axis contributes to the immunosuppression of mice infected with Angiostrongylus cantonensis. J Neuroinflammation 13(1):266. https://doi.org/10.1186/s12974-016-0743-z
Papotto PH, Ribot JC, Silva-Santos B (2017) IL-17(+) gammadelta T cells as kick-starters of inflammation. Nat Immunol 18(6):604–611. https://doi.org/10.1038/ni.3726
Waisman A, Hauptmann J, Regen T (2015) The role of IL-17 in CNS diseases. Acta Neuropathol 129(5):625–637. https://doi.org/10.1007/s00401-015-1402-7
Wei J, Wu F, He A, Zeng X, Ouyang LS, Liu MS, Zheng HQ, Lei WL et al (2015) Microglia activation: one of the checkpoints in the CNS inflammation caused by Angiostrongylus cantonensis infection in rodent model. Parasitol Res 114(9):3247–3254. https://doi.org/10.1007/s00436-015-4541-9
Feng Y, Zheng C, Zhou Z, Xiong H, Feng F, Xie F et al (2019) IL-17A neutralizing antibody attenuates eosinophilic meningitis caused by Angiostrongylus cantonensis by involving IL-17RA/Traf6/NF-kappaB signaling. Exp Cell Res 384(1):111554. https://doi.org/10.1016/j.yexcr.2019.111554
Sonakul D (1978) Pathological findings in four cases of human angiostrongyliasis. Southeast Asian J Trop Med Public Health 9(2):220–227
Ji L, Yiyue X, Xujin H, Minghui Z, Mengying Z, Yue H, Yanqi W, Langui S et al (2017) Study on the tolerance and adaptation of rats to Angiostrongylus cantonensis infection. Parasitol Res 116(7):1937–1945. https://doi.org/10.1007/s00436-017-5472-4
Slom TJ, Cortese MM, Gerber SI, Jones RC, Holtz TH, Lopez AS, Zambrano CH, Sufit RL et al (2002) An outbreak of eosinophilic meningitis caused by Angiostrongylus cantonensis in travelers returning from the Caribbean. N Engl J Med 346(9):668–675. https://doi.org/10.1056/NEJMoa012462
Hasek M, Chutna J, Sladecek M, Lodin Z (1977) Immunological tolerance and tumor allografts in the brain. Nature. 268(5615):68–69. https://doi.org/10.1038/268068a0
Louveau A, Smirnov I, Keyes TJ, Eccles JD, Rouhani SJ, Peske JD, Derecki NC, Castle D et al (2015) Structural and functional features of central nervous system lymphatic vessels. Nature. 523(7560):337–341. https://doi.org/10.1038/nature14432
Komiyama Y, Nakae S, Matsuki T, Nambu A, Ishigame H, Kakuta S, Sudo K, Iwakura Y (2006) IL-17 plays an important role in the development of experimental autoimmune encephalomyelitis. J Immunol 177(1):566–573. https://doi.org/10.4049/jimmunol.177.1.566
Kang Z, Wang C, Zepp J, Wu L, Sun K, Zhao J, Chandrasekharan U, DiCorleto PE et al (2013) Act1 mediates IL-17-induced EAE pathogenesis selectively in NG2+ glial cells. Nat Neurosci 16(10):1401–1408. https://doi.org/10.1038/nn.3505
Haak S, Croxford AL, Kreymborg K, Heppner FL, Pouly S, Becher B, Waisman A (2009) IL-17A and IL-17F do not contribute vitally to autoimmune neuro-inflammation in mice. J Clin Invest 119(1):61–69. https://doi.org/10.1172/JCI35997
Sonderegger I, Kisielow J, Meier R, King C, Kopf M (2008) IL-21 and IL-21R are not required for development of Th17 cells and autoimmunity in vivo. Eur J Immunol 38(7):1833–1838. https://doi.org/10.1002/eji.200838511
Gagliani N, Amezcua Vesely MC, Iseppon A, Brockmann L, Xu H, Palm NW et al (2015) Th17 cells transdifferentiate into regulatory T cells during resolution of inflammation. Nature. 523(7559):221–225. https://doi.org/10.1038/nature14452
Gaffen SL (2011) Recent advances in the IL-17 cytokine family. Curr Opin Immunol 23(5):613–619. https://doi.org/10.1016/j.coi.2011.07.006
Zhang Q, Atsuta I, Liu S, Chen C, Shi S, Shi S, le AD (2013) IL-17-mediated M1/M2 macrophage alteration contributes to pathogenesis of bisphosphonate-related osteonecrosis of the jaws. Clin Cancer Res 19(12):3176–3188. https://doi.org/10.1158/1078-0432.CCR-13-0042
Ribeiro M, Brigas HC, Temido-Ferreira M, Pousinha PA, Regen T, Santa C et al (2019) Meningeal gammadelta T cell-derived IL-17 controls synaptic plasticity and short-term memory. Sci Immunol 4:40. https://doi.org/10.1126/sciimmunol.aay5199
Wucherpfennig KW, Newcombe J, Li H, Keddy C, Cuzner ML, Hafler DA (1992) Gamma delta T-cell receptor repertoire in acute multiple sclerosis lesions. Proc Natl Acad Sci U S A 89(10):4588–4592. https://doi.org/10.1073/pnas.89.10.4588
Gelderblom M, Weymar A, Bernreuther C, Velden J, Arunachalam P, Steinbach K, Orthey E, Arumugam TV et al (2012) Neutralization of the IL-17 axis diminishes neutrophil invasion and protects from ischemic stroke. Blood. 120(18):3793–3802. https://doi.org/10.1182/blood-2012-02-412726
Benakis C, Brea D, Caballero S, Faraco G, Moore J, Murphy M, Sita G, Racchumi G et al (2016) Commensal microbiota affects ischemic stroke outcome by regulating intestinal gammadelta T cells. Nat Med 22(5):516–523. https://doi.org/10.1038/nm.4068
Ribot JC, Neres R, Zuzarte-Luis V, Gomes AQ, Mancio-Silva L, Mensurado S et al (2019) gammadelta-T cells promote IFN-gamma-dependent Plasmodium pathogenesis upon liver-stage infection. Proc Natl Acad Sci U S A 116(20):9979–9988. https://doi.org/10.1073/pnas.1814440116
Cardona AE, Teale JM (2002) Gamma/delta T cell-deficient mice exhibit reduced disease severity and decreased inflammatory response in the brain in murine neurocysticercosis. J Immunol 169(6):3163–3171. https://doi.org/10.4049/jimmunol.169.6.3163
Carding SR, Egan PJ (2002) Gammadelta T cells: functional plasticity and heterogeneity. Nat Rev Immunol 2(5):336–345. https://doi.org/10.1038/nri797
Yu L, Wu X, Wei J, Liao Q, Xu L, Luo S, Zeng X, Zhao Y et al (2015) Preliminary expression profile of cytokines in brain tissue of BALB/c mice with Angiostrongylus cantonensis infection. Parasit Vectors 8:328. https://doi.org/10.1186/s13071-015-0939-6
de Oliveira Henriques MD, Penido C (2012) gammadelta T Lymphocytes Coordinate Eosinophil Influx during Allergic Responses. Front Pharmacol 3:200. https://doi.org/10.3389/fphar.2012.00200
Funding
This work was supported by the National Natural Science Foundation of China (no. 81401688); Fundamental Research Funds for the Central Universities, SCUT (No. 2018MS81); Medical Scientific Research Foundation of Guangdong Province (No. A2018362); Fundamental Research Funds for the Central Universities (no. 2017MS090); South China University of Technology Scientific Research Funding (no. D6172910); and Medical Scientific Research Foundation of Guangdong Province (No. A2018362).
Author information
Authors and Affiliations
Contributions
Zongpu Zhou, Zhen Liu, Cunjing Zheng, and Feng Feng carried out the experiments and performed the statistical analyses. Zongpu Zhou drafted the manuscript. Zhong-Dao Wu, Fukang Xie, and Ying Feng conceived and coordinated the study. All authors read and approved the final manuscript.
Corresponding authors
Ethics declarations
Ethics Approval
All procedures applied to the canines were approved by the Institutional Animal Care and Use Committee of Sun Yat-Sen University and approved by the Laboratory Animal Regulations of Guangdong Province. Animal welfare was in compliance with Laboratory animal Guideline for Ethical Review of Animal Welfare, General Administration of Quality Supervision, Inspection and Quarantine of the People’s Republic of China/Standardization Administration of China (GB/T35892-2018).
Consent to Participate
Not applicable.
Consent for Publication
Not applicable.
Conflict of Interest
The authors declare no competing interests.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
ESM 1
(DOCX 2324 kb)
Rights and permissions
About this article
Cite this article
Feng, Y., Zhou, Z., Liu, Z. et al. Interleukin 17A Derived from γδ T Cell Induces Demyelination of the Brain in Angiostrongylus cantonensis Infection. Mol Neurobiol 58, 3968–3982 (2021). https://doi.org/10.1007/s12035-021-02366-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12035-021-02366-1