Abstract
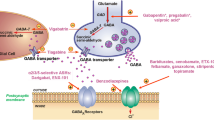
Although several pieces of evidence have indicated the ability of the serotonin-7 receptor (5-HTR7) to modulate N-methyl-D-aspartate receptor (NMDAR) activation, the possible impact on ketamine anesthesia has not been examined directly. The purpose of the present study is thus to investigate the possible role of the 5-HTR7 in ketamine anesthesia using a 5-HTR7 agonist and/or antagonist. The influence of a 5-HTR7 agonist/antagonist on ketamine anesthesia for behavioral impact was assessed by testing potential anesthetic parameters. Its functional impact was assessed by mRNA expression with real-time PCR and immunostaining in the hippocampus and prefrontal cortex of mice. Two different doses of ketamine—high and low—were administered to induce anesthesia. In the high-dose ketamine-applied group in particular, the administration of both the 5-HTR7 agonist and antagonist intensified the anesthetic effect of ketamine. The reflection of the change in anesthesia parameters to 5-HTR7 expression was observed as an increase in the hippocampus and a decrease in the prefrontal cortex in the anesthetized groups by stimulation of 5-HTR7. It is noteworthy that the results of NMDAR expressions are parallel to the results of the 5-HTR7 expressions of both the hippocampus and the prefrontal cortex. The 5-HTR7 may play a role in ketamine anesthesia. It may act through NMDAR in ketamine anesthesia, depending on the parallelism between both receptors.







Similar content being viewed by others
References
Alves HC, Valentim AM, Olsson IAS, Antunes LM (2007) Intraperitoneal propofol and propofol fentanyl sufentanil and remifentanil combinations for mouse anaesthesia . Lab Anim 41(329):336. https://doi.org/10.1258/0023677077812827671
Alves HC, Valentim AM, Olsson IAS, Antunes LM (2009) Intraperitoneal anaesthesia with propofol medetomidine and fentanyl in mice. Lab Anim 43(27):33. https://doi.org/10.1258/la.2008.007036
Amargós-Bosch M, López-Gil X, Artigas F, Adell A (2006) Clozapine and olanzapine but not haloperidol suppress serotonin efflux in the medial prefrontal cortex elicited by phencyclidine and ketamine. Int J Neuropsychopharmacol 9(565):573. https://doi.org/10.1017/S1461145705005900
Amargós‐Bosch M, Adell A, Artigas F (2007) Antipsychotic drugs reverse the AMPA receptor‐stimulated release of 5‐HT in the medial prefrontal cortex. J Neurochem 102:550–561. https://doi.org/10.1111/j.1471-4159.2007.04532.x
Antognini JF, Jinks SL, Atherley R, Clayton C, Carstens E (2003) Spinal anaesthesia indirectly depresses cortical activity associated with electrical stimulation of the reticular formation. Br J Anaesth 91:233–238. https://doi.org/10.1093/bja/aeg168
Antognini JF, Jinks SL, Carstens EE, Atherley RJ (2004) Preserved reticular neuronal activity during selective delivery of supra-clinical isoflurane concentrations to brain in goats and its association with spontaneous movement. Neurosci Lett 361:94–97. https://doi.org/10.1016/j.neulet.2003.12.024
Arras M, Autenried P, Rettich A, Spaeni D, Rülicke T (2001) Optimization of intraperitoneal injection anesthesia in mice drugs dosages adverse effects and anesthesia depth. Comp Med 51:443–456
Arvanov VL, Liang X, Magro P, Roberts R, Wang RY (1999) A pre‐and postsynaptic modulatory action of 5‐HT and the 5‐HT2A, 2C receptor agonist DOB on NMDA‐evoked responses in the rat medial prefrontal cortex European. J Neurosci 11:2917–2934. https://doi.org/10.1046/j.1460-9568.1999.00708.x
Bosker FJ et al (2009) Antagonism of 5‐HT1A receptors uncovers an excitatory effect of SSRIs on 5‐HT neuronal activity, an action probably mediated by 5‐HT7 receptors. J Neurochem 108:1126–1135. https://doi.org/10.1111/j.1471-4159.2008.05850.x
Brenchat A, Rocasalbas M, Zamanillo D, Hamon M, Vela JM, Romero L (2012) Assessment of 5-HT7 receptor agonists selectivity using nociceptive and thermoregulation tests in knockout versus wild-type mice Advances in pharmacological sciences 2012. https://doi.org/10.1155/2012/312041
Cadirci E, Ugan RA, Dincer B, Gundogdu B, Cinar I, Akpinar E, Halici Z (2019) Urotensin receptors as a new target for CLP induced septic lung injury in mice. Naunyn-Schmiedeberg’s archives of pharmacology 392:135–145. https://doi.org/10.1007/s00210-018-1571-8
Diazgranados N et al (2010) A randomized add-on trial of an N-methyl-D-aspartate antagonist in treatment-resistant bipolar depression. Arch Gen Psychiatry 67:793–802. https://doi.org/10.1001/archgenpsychiatry.2010.90
Dringenberg HC (2000) Serotonergic receptor antagonists alter responses to general anaesthetics in rats. Br J Anaesth 85:904–906. https://doi.org/10.1093/bja/85.6.904
Ezquerra-Romano II, Lawn W, Krupitsky E, Morgan CJA (2018) Ketamine for the treatment of addiction: Evidence and potential mechanisms. Neuropharmacology 142:72–82. https://doi.org/10.1016/j.neuropharm.2018.01.017
Farahmandfar M, Bakhtazad A, Akbarabadi A, Zarrindast M-R (2016) The influence of dopaminergic system in medial prefrontal cortex on ketamine-induced amnesia in passive avoidance task in mice. Eur J Pharmacol 781:45–52. https://doi.org/10.1016/j.ejphar.2016.03.060
Forero A et al. (2020) Serotonin (5-HT) neuron-specific inactivation of Cadherin-13 impacts 5-HT system formation and cognitive function Neuropharmacology:108018. https://doi.org/10.1016/j.neuropharm.2020.108018
Forman SA, Chin VA (2008) General anesthetics and molecular mechanisms of unconsciousness International anesthesiology clinics 46:43. https://doi.org/10.1097/AIA.0b013e3181755da5
Gartside SE, Cole AJ, Williams AP, McQuade R, Judge SJ (2007) AMPA and NMDA receptor regulation of firing activity in 5‐HT neurons of the dorsal and median raphe nuclei European. J Neurosci 25:3001–3008. https://doi.org/10.1111/j.1460-9568.2007.05577.x
Gasbarri A, Cifariello A, Pompili A, Meneses A (2008) Effect of 5 HT7 antagonist SB 269970 in the modulation of working and reference memory in the rat. Behav Brain Res 195:164–170. https://doi.org/10.1016/j.bbr.2007.12.020
Golembiewski J (2017) Ketamine what is old is new again. Journal of PeriAnesthesia Nursing 32:660–663. https://doi.org/10.1016/j.jopan.2017.09.003
Goulart BK et al (2010) Ketamine impairs recognition memory consolidation and prevents learning-induced increase in hippocampal brain-derived neurotrophic factor levels. Neuroscience 167:969–973. https://doi.org/10.1016/j.neuroscience.2010.03.032
Guseva D, Wirth A, Ponimaskin E (2014) Cellular mechanisms of the 5-HT7 receptor-mediated signaling. Frontiers in behavioral neuroscience 8:306. https://doi.org/10.3389/fnbeh.2014.00306
Han L-C (2010) Yao L-n, Wu S-x, Yang Y-h, Xu L-X, Chai W. The effect of ketamine on N-methyl-D-aspartate receptor subunit expression in neonatal rats European Journal of Anaesthesiology (EJA) 27:181–186. https://doi.org/10.1097/EJA.0b013e328330d453
Harsing LG, Prauda I, Barkoczy J, Matyus P, Juranyi Z (2004) A 5-HT 7 heteroreceptor-mediated inhibition of [3 H] serotonin release in raphe nuclei slices of the rat: evidence for a serotonergic–glutamatergic interaction. Neurochem Res 29:1487–1497. https://doi.org/10.1023/B:NERE.0000029560.14262.39
Hedlund PB (2009) The 5-HT 7 receptor and disorders of the nervous system: an overview. Psychopharmacology 206:345–354. https://doi.org/10.1007/s00213-009-1626-0
Hedlund PB, Sutcliffe JG (2004) Functional, molecular and pharmacological advances in 5-HT7 receptor research. Trends Pharmacol Sci 25:481–486. https://doi.org/10.1016/j.tips.2004.07.002
Hemmings HC, Hopkins PM (2000) Foundations of anesthesia: basic and clinical sciences. Mosby Inc,
Irifune M et al (1997) Effects of ketamine on dopamine metabolism during anesthesia in discrete brain regions in mice: Comparison with the effects during the recovery and subanesthetic phases. Brain Res 763:281–284. https://doi.org/10.1016/S0006-8993(97)00510-6
Irifune M, Shimizu T, Nomoto M, Fukuda T (1992) Ketamine-induced anesthesia involves the N-methyl-D-aspartate receptor-channel complex in mice. Brain Res 596:1–9. https://doi.org/10.1016/0006-8993(92)91525-J
Koizuka S, Obata H, Sasaki M, Saito S, Goto F (2005) Systemic ketamine inhibits hypersensitivity after surgery via descending inhibitory pathways in rats. Canadian Journal of Anesthesia 52:498. https://doi.org/10.1007/BF03016530
Kose D, Cadirci E, Halici Z, Sirin B, Dincer B (2019) The investigation of possible roles of central 5-HT 7 receptors in antipyretic effect mechanism of paracetamol in LPS-induced hyperthermia model of mice. Inflammopharmacology 27:1169–1178. https://doi.org/10.1007/s10787-019-00617-1
Leopoldo M (2004) Serotonin7 receptors (5-HT7Rs) and their ligands. Curr Med Chem 11:629–661. https://doi.org/10.2174/0929867043455828
Leopoldo M, Lacivita E, Berardi F, Perrone R, Hedlund PB (2011) Serotonin 5-HT7 receptor agents: Structure-activity relationships and potential therapeutic applications in central nervous system disorders. Pharmacol Ther 129:120–148. https://doi.org/10.1016/j.pharmthera.2010.08.013
Lippiello P et al (2016) The 5-HT7 receptor triggers cerebellar long-term synaptic depression via PKC-MAPK. Neuropharmacology 101:426–438. https://doi.org/10.1016/j.neuropharm.2015.10.019
Livak KJ, Schmittgen TD (2013) Analysis of relative gene expression data using real-time quantitative PCR and the 2 (-Delta Delta C (T)) method. methods. 25: 402–408. 2001 View Article: Google Scholar: PubMed/NCBI
Liy‐Salmeron G, Meneses A (2008) Effects of 5‐HT drugs in prefrontal cortex during memory formation and the ketamine amnesia‐model. Hippocampus 18:965–974. https://doi.org/10.1002/hipo.20459
López-Gil X, Jiménez-Sánchez L, Romón T, Campa L, Artigas F, Adell A (2012) Importance of inter-hemispheric prefrontal connection in the effects of non-competitive NMDA receptor antagonists. Int J Neuropsychopharmacol 15:945–956. https://doi.org/10.1017/S1461145711001064
Lugli AK, Yost CS, Kindler CH (2009) Anaesthetic mechanisms: Update on the challenge of unravelling the mystery of anaesthesia. Eur J Anaesthesiol 26:807. https://doi.org/10.1097/EJA.0b013e32832d6b0f
Markov D, Goldman M (2006) Normal sleep and circadian rhythms: Neurobiologic mechanisms underlying sleep and wakefulness Psychiatric. Clinics 29:841–853. https://doi.org/10.1016/j.jsmc.2012.06.015
Matsunaga F, Gao L, Huang XP, Saven JG, Roth BL, Liu R (2015) Molecular interactions between general anesthetics and the 5HT2B receptor. J Biomol Struct Dyn 33:211–218. https://doi.org/10.1080/07391102.2013.869483
Matthys A, Haegeman G, Van Craenenbroeck K, Vanhoenacker P (2011) Role of the 5-HT7 receptor in the central nervous system: from current status to future perspectives. Mol Neurobiol 43:228–253. https://doi.org/10.1007/s12035-011-8175-3
McCardle CE, Gartside SE (2012) Effects of general anaesthetics on 5-HT neuronal activity in the dorsal raphe nucleus. Neuropharmacology 62:1787–1796
Meltzer HY, Horiguchi M, Massey BW (2011) The role of serotonin in the NMDA receptor antagonist models of psychosis and cognitive impairment. Psychopharmacology 213:289–305. https://doi.org/10.1007/s00213-010-2137-8
Meneses A, Perez-Garcia G, Liy-Salmeron G, Ponce-López T, Lacivita E, Leopoldo M (2015) 5-HT 7 receptor activation: procognitive and antiamnesic effects. Psychopharmacology 232:595–603. https://doi.org/10.1007/s00213-014-3693-0
Minami K, Uezono Y (2013) The recent progress in research on effects of anesthetics and analgesics on G protein-coupled receptors. Journal of anesthesia 27:284–292. https://doi.org/10.1007/s00540-012-1507-2
Mion G, Villevieille T (2013) Ketamine pharmacology: An update (pharmacodynamics and molecular aspects, recent findings). CNS Neurosci Ther 19:370–380. https://doi.org/10.1111/cns.12099
Monti JM, Leopoldo M, Jantos H (2008) The serotonin 5-HT7 receptor agonist LP-44 microinjected into the dorsal raphe nucleus suppresses REM sleep in the rat. Behav Brain Res 191:184–189. https://doi.org/10.1016/j.bbr.2008.03.025
Müller CP, Pum ME, Amato D, Schüttler J, Huston JP, De Souza Silva MA (2011) The in vivo neurochemistry of the brain during general anesthesia. J Neurochem 119:419–446. https://doi.org/10.1111/j.1471-4159.2011.07445.x
Nagatani H, Oshima T, Urano A, Saitoh Y, Yokota M, Nakata Y (2011) Blockade of 5-HT 2A and/or 5-HT 2C receptors modulates sevoflurane-induced immobility. Journal of anesthesia 25:225–228. https://doi.org/10.1007/s00540-011-1103-x
Neumaier JF, Sexton TJ, Yracheta J, Diaz AM, Brownfield M (2001) Localization of 5-HT7 receptors in rat brain by immunocytochemistry, in situ hybridization, and agonist stimulated cFos expression. J Chem Neuroanat 21:63–73. https://doi.org/10.1016/S0891-0618(00)00092-2
Pérez-García G, Gonzalez-Espinosa C, Meneses A (2006) An mRNA expression analysis of stimulation and blockade of 5-HT7 receptors during memory consolidation. Behav Brain Res 169:83–92. https://doi.org/10.1016/j.bbr.2005.12.013
Petrenko AB, Yamakura T, Sakimura K, Baba H (2014) Defining the role of NMDA receptors in anesthesia: are we there yet? Eur J Pharmacol 723:29–37. https://doi.org/10.1016/j.ejphar.2013.11.039
Pham TH, Mendez-David I, Defaix C, Guiard BP, Tritschler L, David DJ, Gardier AM (2017) Ketamine treatment involves medial prefrontal cortex serotonin to induce a rapid antidepressant-like activity in BALB/cJ mice. Neuropharmacology 112:198–209. https://doi.org/10.1016/j.neuropharm.2016.05.010
Rampil IJ (2000) Mechanisms and sites of action of general anaesthetics. In: Memory And Awareness In Anaesthesia IV. World Scientific, pp 223–231. https://doi.org/10.1142/9781848160231_0019
Rascón-Martínez DM, Carrillo-Torres O, Ramos-Nataren RG, Rendón-Jaramillo L (2018) Advantages of ketamine as a perioperative analgesic Revista Médica del Hospital General de México 81:253–261. https://doi.org/10.1016/j.hgmx.2016.10.007
Sengupta A, Bocchio M, Bannerman DM, Sharp T, Capogna M (2017) Control of amygdala circuits by 5-HT neurons via 5-HT and glutamate cotransmission. J Neurosci 37:1785–1796. https://doi.org/10.1523/JNEUROSCI.2238-16.2016
Serrano-Caballero JM, Molina AM, Lora AJ, Serrano-Rodriguez JM, Pena F, Moyano MR (2013) Evaluation of different central nervous system depressors combined with ketamine for anaesthesia in mice. Vet Med 58:364–372
Sleigh J, Harvey M, Voss L, Denny B (2014) Ketamine-More mechanisms of action than just NMDA blockade Trends in anaesthesia and critical care 4:76–81. https://doi.org/10.1016/j.tacc.2014.03.002
Sommer C (2010) Serotonin in pain and pain control. In: Handbook of behavioral neuroscience, vol 21. Elsevier, pp 457–471. https://doi.org/10.1016/S1569-7339(10)70096-5
Stahl SM (2010) The serotonin-7 receptor as a novel therapeutic target. The Journal of clinical psychiatry 71:1414–1415
Thomas DR et al. (2003) SB‐656104‐A, a novel selective 5‐HT7 receptor antagonist, modulates REM sleep in rats British journal of pharmacology 139:705–714. https://doi.org/10.1038/sj.bjp.0705290
Tso MM, Blatchford KL, Callado LF, McLaughlin DP, Stamford JA (2004) Stereoselective effects of ketamine on dopamine, serotonin and noradrenaline release and uptake in rat brain slices Neurochemistry international 44:1–7
Ugan RA, Cadirci E, Halici Z, Toktay E, Cinar I (2018) The role of urotensin-II and its receptors in sepsis-induced lung injury under diabetic conditions. Eur J Pharmacol 818:457–469. https://doi.org/10.1016/j.ejphar.2017.11.011
Varnäs K, Thomas DR, Tupala E, Tiihonen J, Hall H (2004) Distribution of 5-HT7 receptors in the human brain: A preliminary autoradiographic study using [3H] SB-269970 Neuroscience letters 367:313–316. https://doi.org/10.1016/j.neulet.2004.06.025
Vasefi MS et al. (2013) Acute 5-HT7 receptor activation increases NMDA-evoked currents and differentially alters NMDA receptor subunit phosphorylation and trafficking in hippocampal neurons Molecular brain 6:24. https://doi.org/10.1186/1756-6606-6-24
Wagner G, Gussew A, Koehler S, de la Cruz F, Smesny S, Reichenbach JR, Baer K-J (2016) Resting state functional connectivity of the hippocampus along the anterior–posterior axis and its association with glutamatergic metabolism Cortex 81:104–117. https://doi.org/10.1016/j.cortex.2016.03.022
Wang Y, Han S, Han R, Su Y, Li J (2017) Propofol‐induced downregulation of NR2B membrane translocation in hippocampus and spatial memory deficits of neonatal mice Brain and behavior 7:e00734. https://doi.org/10.1002/brb3.734
Yuen EY, Jiang Q, Chen P, Feng J, Yan Z (2008) Activation of 5-HT2A/C receptors counteracts 5-HT1A regulation of n-methyl-D-aspartate receptor channels in pyramidal neurons of prefrontal cortex Journal of Biological Chemistry 283:17194–17204. https://doi.org/10.1074/jbc.M801713200
Yuen EY, Jiang Q, Chen P, Gu Z, Feng J, Yan Z (2005) Serotonin 5-HT1A receptors regulate NMDA receptor channels through a microtubule-dependent mechanism Journal of Neuroscience 25:5488–5501. https://doi.org/10.1523/JNEUROSCI.1187-05.2005
Zanos P et al (2018) Ketamine and ketamine metabolite pharmacology: insights into therapeutic mechanisms. Pharmacol Rev 70:621–660. https://doi.org/10.1124/pr.117.015198
Zareifopoulos N, Papatheodoropoulos C (2016) Effects of 5-HT-7 receptor ligands on memory and cognition Neurobiology of learning and memory 136:204–209. https://doi.org/10.1523/JNEUROSCI.1187-05.2005
Zhang Y, Laster MJ, Eger EI, Stabernack CR, Sonner JM (2003) Blockade of 5-HT2A receptors may mediate or modulate part of the immobility produced by inhaled anesthetics Anesthesia & Analgesia 97:475–479. https://doi.org/10.1213/01.ANE.0000070229.94485.17
Zhao Y, Sun L (2008) Antidepressants modulate the in vitro inhibitory effects of propofol and ketamine on norepinephrine and serotonin transporter function. Journal of Clinical Neuroscience 15:1264–1269
Zhong P, Yuen EY, Yan Z (2008) Modulation of neuronal excitability by serotonin-NMDA interactions in prefrontal cortex. Mol Cell Neurosci 38:290–299
Funding
This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors. This study is derived from Busra DINCER's PhD thesis
Author information
Authors and Affiliations
Corresponding author
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Dincer, B., Halici, Z. & Cadirci, E. Investigation of the Role of Stimulation and Blockade of 5-HT7 Receptors in Ketamine Anesthesia.. J Mol Neurosci 71, 1095–1111 (2021). https://doi.org/10.1007/s12031-020-01732-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12031-020-01732-3