Abstract
The p38 mitogen-activated protein kinase (MAPK) pathway plays a key role in pathological glial activation and neuroinflammatory responses. Our previous studies demonstrated that microglial p38α and not the p38β isoform is an important contributor to stressor-induced proinflammatory cytokine upregulation and glia-dependent neurotoxicity. However, the contribution of neuronal p38α and p38β isoforms in responses to neurotoxic agents is less well understood. In the current study, we used cortical neurons from wild-type or p38β knockout mice, and wild-type neurons treated with two highly selective inhibitors of p38α MAPK. Neurons were treated with one of three neurotoxic insults (L-glutamate, sodium nitroprusside, and oxygen-glucose deprivation), and neurotoxicity was assessed. All three stimuli led to neuronal death and neurite degeneration, and the degree of neurotoxicity induced in wild-type and p38β knockout neurons was not significantly different. In contrast, selective inhibition of neuronal p38α was neuroprotective. Our results show that neuronal p38β is not required for neurotoxicity induced by multiple toxic insults, but that p38α in the neuron contributes quantitatively to the neuronal dysfunction responses. These data are consistent with our previous findings of the critical importance of microglia p38α compared to p38β, and continue to support selective targeting of the p38α isoform as a potential therapeutic strategy.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Mitogen-activated protein kinase (MAPK) pathways are pivotal in linking stimuli to cellular responses. The involvement of MAPK pathways in many stress- and disease-induced responses throughout the body has heightened the interest to develop selective small molecule kinase inhibitors to modulate these signal transduction pathways. For example, the p38 branch of the MAPK family is a well-established therapeutic target for diseases with inflammation as a common mechanism. In the central nervous system (CNS), most studies of p38 function have focused on p38 in glia and its role in aberrant proinflammatory responses in acute and chronic neurodegenerative conditions (for reviews, see Bachstetter & Van Eldik 2010; Correa & Eales 2012). Much less is known about the relationship between neuronal p38 and CNS pathophysiology. In addition, whether the two major p38 isoforms in the CNS, p38α and p38β, play similar or distinct roles in neuronal responses to pathological stimuli is a major unanswered question.
Investigations to define the relative importance of neuronal p38α and p38β in stress-induced neuronal responses have been hampered by a lack of specific reagents. Mice with a genetic knockout of the p38β gene (p38β knockout (KO)) are healthy and fertile (Beardmore et al. 2005; O'Keefe et al. 2007), and therefore are a useful reagent to test the involvement of the p38β isoform in particular cellular functions. However, a similar approach cannot be taken with p38α knockout mice because these mice are embryonic lethal (Adams et al. 2000; Allen et al. 2000; Mudgett et al. 2000; Tamura et al. 2000). In addition, many small molecule p38 inhibitors such as the commercially available SB203580 compound do not distinguish between p38α and p38β, and actually react with a number of other cellular targets, including thromboxane synthase (Borsch-Haubold et al. 1998), cyclooxygenases (Borsch-Haubold et al. 1998), c-Raf (Hall-Jackson et al. 1999), and other kinases (Clerk & Sugden 1998; Lali et al. 2000; Godl et al. 2003; Bain et al. 2007). While one might assume that the effects of SB203580 are dependent on p38α, this assumption has not been rigorously tested with p38α- and p38β-specific reagents.
We recently reported (Watterson et al. 2013) the development of two highly specific small molecule p38α inhibitors, termed MW-108 and MW-181. The high level of selectivity of the inhibitors was demonstrated by large-scale kinome activity screens, functional GPCR agonist and antagonist assays, and cellular target engagement analyses. MW-108 targets a single kinase, p38α, and does not cross-react with p38β. MW-181 inhibits p38α, and has weaker cross-reactivity with p38β. The availability of these p38α inhibitors, along with the p38β KO mouse, provided us the opportunity to directly test the contribution of neuronal p38α and p38β in neurodegenerative responses to specific toxic stimuli.
The goal of the current study was to determine whether neuronal p38α or p38β is important for neurotoxic responses induced by three clinically relevant insults: L-glutamate (excitotoxicity), sodium nitroprusside (SNP; a nitric oxide donor), and oxygen-glucose deprivation (OGD; hypoxia ischemia). We chose these three neurotoxic insults because there is precedent for p38 playing a role in neurotoxicity responses induced by these agents (Kawasaki et al. 1997; Lin et al. 2001; Legos et al. 2002; Chen et al. 2003; Cao et al. 2004; Pi et al. 2004; Tabakman et al. 2004; Guo & Bhat 2007; Molz et al. 2008; Strassburger et al. 2008; Li et al. 2009; Lu et al. 2011). We used primary cortical neurons from wild-type (WT) and p38β global KO mice to determine if deletion of p38β affected the neuronal damage responses. To test the contribution of p38α to the neurotoxic responses and to determine if targeting a single kinase was neuroprotective, we treated WT mouse neurons with the neurotoxic agents in the presence of our p38α inhibitors MW-181 and MW-108 (Watterson et al. 2013). Consistent with our previous findings of a distinct role for p38α and p38β in microglia upon inflammatory insult (Xing et al. 2011; Xing et al. 2013), we report here that the absence of p38β in cortical neurons does not suppress the neurotoxic responses to any of the three insults. However, selective inhibition of p38α in neurons not only reduces cell death but also reduces the neurite damage in the surviving neurons. These results demonstrate the importance of the neuronal p38α isoform in neurotoxicity induced by multiple disease-relevant insults.
Materials and Methods
Ethics Statement
All mouse experiments were conducted in accordance with the principles of animal care and experimentation in the Guide for the Care and Use of Laboratory Animals. The Institutional Animal Care and Use Committee of the University of Kentucky approved the use of animals in this study (protocol #2010-0615).
Reagents
L-glutamate (Cat. no. G1251) and SNP (Cat. no. 228710) were obtained from Sigma-Aldrich. The highly selective p38α inhibitors MW01-10-181SRM (MW-181) and MW01-11-108SRM (MW-108) were synthesized and characterized as described (Watterson et al. 2013). Stock solutions of the inhibitors were prepared in sterile 0.9 % NaCl.
Animals
The p38β global KO mice were generated as described (O'Keefe et al. 2007), and a colony bred and maintained at University of Kentucky. C57BL/6 mice were purchased from Harlan Laboratories. The p38β gene KO was confirmed by Transnetyx, Inc (Cordova, TN, USA).
Determination of p38 Isoform RNA Levels
The levels of expression of p38α, β, δ, and γ RNA were determined as previously described (Xing et al. 2013). Briefly, RNA was isolated from primary cortical neuron cultures using RNeasy minicolumns with on-column DNase treatment (Qiagen), and RNA quantity and quality were determined by measuring the A260/A280 ratio by NanoDrop (Thermo Scientific). Reverse transcription (RT) was done with a High Capacity cDNA Reverse Transcription Kit (Applied Biosystems, Cat. no. 4368814), with no template and no RT controls included. Real-time PCR was done with the TaqMan Gene Expression assay kit (Applied Biosystems) on a ViiA 7 Real-Time PCR System (Applied Biosystems). The following TaqMan probes (Applied Biosystems) were used: p38α (MAPK14, Mm00442507_m1), p38β (MAPK11, Mm00440955_m1), p38δ (MAPK13, Mm00442488_m1), p38γ (MAPK12, Mm00443518_m1), and 18S rRNA (Hs99999901_s1). Relative gene expression was calculated by the 2−ΔΔCT method. Levels of p38β expression in WT neurons were normalized to 1.0.
Primary Neuronal Culture
Primary neuronal cultures were derived from embryonic day 18 WT or p38β KO mice, as previously described (Xing et al. 2011). Cells were dissociated from dissected cerebral cortices by trypsinization for 20–25 min at 37 °C, followed by passing through a 70-μm nylon mesh cell strainer. The cells were seeded at a density of 5 × 104 cells/well onto poly-d-lysine-coated 12-mm glass coverslips for L-glutamate and OGD experiments, or at 2 × 104 cells/well in 24-well plates for SNP experiments. Neurons were grown in neurobasal medium containing 2 % B27 supplement (Invitrogen), 0.5 mM l-glutamine, 100 IU/ml penicillin, and 100 μg/ml streptomycin; no serum or mitosis inhibitors were used. Every 3 days, 50 % of the media was replenished with fresh medium.
Cell Culture Treatments
Neurons from WT and p38β KO mice were subjected to L-glutamate, SNP, or OGD insults at 7 days in vitro (DIV7), and neurotoxicity measured at 24 h after insult. For L-glutamate studies, neurobasal/B27 medium was carefully removed from primary neuron cultures and saved. Neurons were then treated with 25 μM L-glutamate for 10 min in CSS buffer (120 mM NaCl, 5.4 mM KCl, 0.8 mM MgCl2, 1.8 mM CaCl2, 20 mM HEPES, and 15 mM glucose) (Schubert & Piasecki 2001). The cells were then washed three times with Hank’s balanced salt solution (HBSS), and returned back into the original neurobasal/B27 media for 24 h. WT neurons were treated with the p38α inhibitors MW-181 or MW-108 (60 μM) for 60 min before L-glutamate addition. For SNP studies, neurons were treated with 1 mM SNP dissolved in culture medium for 24 h before neurotoxicity assays. MW-181 or MW-108 (60 μM) was added at the same time as the SNP solution. For OGD studies, primary neurons were treated with the p38α inhibitor MW-181 or MW-108 (60 μM) for 60 min prior to OGD. OGD was done for 1 h in an anaerobic chamber saturated with 5 % CO2 and 95 % N2 in glucose-free DMEM medium. The OGD condition was terminated by switching cells back to normal culture conditions and incubating for 24 h until neurotoxicity assays were done. Control cells were incubated in DMEM with glucose in a normoxic incubator for the same period.
Neuronal Viability Assay
Neuron viability was assayed by trypan blue exclusion (Xie et al. 2004). Neuron-containing coverslips were incubated with 0.2 % trypan blue in HBSS for 2 min in a 37 °C incubator and then gently rinsed three times with HBSS. Neurons were viewed under bright field microscopy at × 200 final magnification. Five to eight fields were chosen randomly per coverslip, and a total of 485 to 761 cells were counted per coverslip. Trypan blue-positive and negative neurons were counted per field and the ratio of positive cells to the total cells was taken as the percent neuronal death.
Immunocytochemistry
Cells were fixed with 3.7 % formaldehyde containing 0.1 % Triton X-100 in PBS for 10 min at room temperature. After washing three times with PBS, the coverslips were incubated with blocking buffer (PBS containing 6 % goat serum, 3 % bovine serum albumin (fraction V), 0.1 % Triton X-100) for 30 min at room temperature. Primary chicken anti-MAP2 antibody (1:1,000, Neuromics, Cat. no. CH22103) was diluted in blocking buffer and incubated with the cells at room temperature for 2 h. For detection of MAP2 staining, the cells were incubated with secondary biotin SP-conjugated goat antichicken antibody (1:1,000, Jackson ImmunoResearch) for 1 h, followed by streptavidin Alexa Fluor® fluorescent 488 (1:1,000, Invitrogen) incubation in blocking buffer at room temperature for 1 h. Wide field fluorescent photomicrographs were obtained using a Nikon Eclipse Ti microscope with an Axiocam MRc5 digital camera (Carl Zeiss).
Semi-automated Sholl Analysis
The semi-automated Sholl assay was used to measure the neurite degeneration of MAP2-labeled neurons, essentially as we previously described with a manual Sholl analysis (Xing et al. 2011). The original images were binarized and thresholded using NIH ImageJ. Sholl semi-automated analysis program was loaded from ImageJ plugins (http://imagej.nih.gov/ij/plugins/). The central point on the soma of each neuron was selected, and a series of concentric circles were drawn automatically, with the radius of the smallest sampling circle at 8 μm from the central point and the radius of the largest sampling circle at 50 μm with a radius step size of 0.167 μm. The Sholl analysis then determined how many times the neurites intersected the sampling circles, and measured the average intersections over the whole area occupied by the neurite per neuron. The mean of average intersections of 107–188 neurons per group was calculated, and the mean from control group was normalized to 0 % damage.
Statistics
Statistical analysis was conducted using GraphPad prism software V.6 (GraphPad Software). Unless otherwise indicated, values are expressed as mean ± SEM. Groups of two were compared by unpaired t test. One-way ANOVA followed by Bonferroni’s multiple comparison test was used for comparisons among three or more groups. Statistical significance was defined as p < 0.05.
Results
Validation of p38β KO in Primary Cortical Neurons
As a first step, it was important to confirm the deletion of p38β in primary cortical neurons from the p38β KO mouse and verify that significant compensatory changes in the p38α, p38δ, and p38γ isoforms were not present. RNA was prepared from primary cortical neuron cultures derived from WT or p38β KO mouse fetuses, and the expression levels of the p38 isoforms were determined by qPCR. As expected, p38β mRNA was readily measurable in WT mice but was not detected in the p38β KO mice (Fig. 1). The mRNA level of p38α in both WT and p38β KO neurons was ~40-fold higher than that of p38β in WT neurons, but there was no significant difference between the p38α levels in the WT compared to the p38β KO mice. The levels of p38δ and p38γ mRNA were similar and very low in both WT and p38β KO mice (data not shown). Altogether, the data verify that, as expected, p38β is deficient in neurons from the p38β KO mice and there are no significant compensatory changes in any of the other p38 isoforms.
Verification of p38β KO in neurons. Primary cortical neurons from WT and p38β KO mice were prepared as described in the “Methods” section and plated at 5 × 104 cells/well in 24-well plates. Total RNA was isolated from neuronal cultures derived from WT (black bars) or p38β KO (white bars) mice, and the mRNA levels of different p38 MAPK isoforms were determined by qPCR. The result shows that p38β mRNA was readily measureable in WT mice but was not detected in the p38β KO mice. The p38α MAPK isoform in both WT and p38β KO neurons was expressed at much higher levels compared to p38β, but there was no significant difference between the levels of p38α in WT and p38β KO mice. The levels of p38δ and p38γ mRNA were very low to undetectable in both WT and p38β KO mice (data not shown). Results are expressed as fold change compared to p38β expression levels in WT neurons, and represent the mean ± SEM of four to eight determinations
Neurotoxicity Induced by L-Glutamate
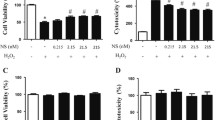
L-glutamate is a standard neurotoxic stimulus that is a model of excitotoxic cell death (Choi et al. 1987), and p38 has been reported to be involved in excitotoxic pathways leading to neuron damage/death (Kawasaki et al. 1997; Chen et al. 2003; Pi et al. 2004; Chaparro-Huerta et al. 2008; Molz et al. 2008; Bakuridze et al. 2009; Izumi et al. 2009). Therefore, we compared the degree of neuron death and neurite degeneration induced by L-glutamate in primary cortical neurons derived from WT and p38β KO mice. Under the culture conditions used, L-glutamate induced ~22 % neuron death as measured by trypan blue assay (Fig. 2a). L-glutamate also induced significant (22–25 %) neurite damage in the surviving neurons as measured by Sholl analysis (Fig. 2b), where the percentage of average intersections over the whole area occupied by the neurite is determined. L-glutamate treatment resulted in extensive neurite fragmentation, swelling, and blebbing (Fig. 2c). The degree of neuron death/neurite damage was not significantly different between WT and p38β KO neurons. In contrast, inhibition of neuronal p38α by MW-181 or MW-108 1 h prior to L-glutamate treatment significantly reduced both the neuron death and the neurite degeneration (Fig. 2a, b). As shown in Fig. 2c, the neurons treated with MW-181 or MW-108 showed less fragmentation and blebbing of the neurites.
p38α inhibition but not p38β KO protects neurons against L-glutamate insult. WT or p38β KO mouse primary cortical neurons were plated on cover slips at 5 × 104 cells/well and grown for 7 days in vitro (DIV7). After 1 h pretreatment of WT neurons with 60 μM MW-181 or MW-108, the media was removed and saved, then WT and p38β KO neurons were treated for 10 min with culture medium alone, L-glutamate (25 μM) alone, or L-glutamate plus 60 μM MW-181 or MW-108. After 10 min of incubation, cells were washed three times with HBSS, and the original culture media was added back into the appropriate wells. Trypan blue exclusion assay for neurotoxicity and Sholl analysis for neurite damage were performed after 24 h. a L-glutamate induced ~22 % neuronal death in both p38β KO and WT neurons. In contrast, p38α inhibition by MW-181 or MW-108 significantly reduced the neuron death after L-glutamate insult. b Similarly, L-glutamate-induced neurite fragmentation and blebbing in both p38β KO and WT neurons, with no significant difference between the two groups. In contrast, inhibition of p38α MAPK by MW-181 or MW-108 significantly protected neurites against L-glutamate-induced damage. c Representative photomicrographs of MAP2 immunocytochemistry show the morphology of neurons after 24 h. Arrows point to the appearance of damaged neurites after L-glutamate insult in both p38β KO and WT neurons (****p < 0.0001 vs. control; #p < 0.05 vs. L-glutamate treatment; ###p < 0.001 vs. L-glutamate treatment; ####p < 0.0001 vs. L-glutamate treatment, Bonferroni’s multiple comparison test). Data are from three independent experiments. Scale bar 10 μm
Neurotoxicity Induced by SNP
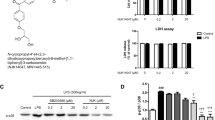
To determine whether the findings with L-glutamate implicating p38α but not p38β in neurotoxicity were generalizable to a different neurotoxic insult, we tested the effect of SNP on neuron death and neurite damage. SNP is a nitric oxide donor commonly used to induce neuronal apoptosis, and p38 activation has previously been implicated in promoting nitric oxide induced neuronal damage (Ghatan et al. 2000; Lin et al. 2001). SNP (1 mM) treatment for 24 h killed 32 % WT neurons and 28 % p38β KO neurons (Fig. 3a) and induced 27–32 % neurite damage in both groups (Fig. 3b, c). Although the KO neurons appeared to be slightly less susceptible to SNP toxicity compared to WT neurons, the levels of neuron death/neurite damage between WT and p38β KO neurons were not significantly different. Similar to the findings with L-glutamate, inhibition of p38α by MW-181 or MW-108 treatments of WT neurons significantly reduced SNP-induced neuronal death (Fig. 3a), and protected neurons against neurite degeneration (Fig. 3b, c).
p38α inhibition but not p38β KO protects neurons against SNP insult. DIV7 neurons on coverslips were treated with culture medium alone, SNP (1 mM) alone, or SNP plus 60 μM MW-181 or MW-108 for 24 h, followed by trypan blue exclusion assay and Sholl analysis. a SNP induced ~28–32 % neuronal death in both p38β KO and WT neurons, with no significant differences between the genotypes. In contrast, p38α inhibition by MW-181 or MW-108 significantly reduced the neuron death induced by SNP. b SNP induced a similar degree of neurite damage in both p38β KO and WT neurons. In contrast, WT neurons treated with SNP in the presence of the p38α inhibitors showed reduced levels of neurite degeneration. c Representative photomicrographs of MAP2 immunocytochemistry show the morphology of neurons after 24 h. Arrows point to the appearance of damaged neurites induced by SNP treatment in both p38β KO and WT neurons (****p < 0.0001 vs. control; ##p < 0.01 vs. SNP; ####p < 0.0001 vs. SNP, Bonferroni’s multiple comparison test). Data are from three independent experiments. Scale bar 10 μm
Neurotoxicity Induced by OGD
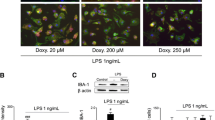
We also tested the relative contribution of p38α and p38β to neurotoxic responses induced by OGD, a model of ischemic injury (Kaku et al. 1991; Dawson et al. 1996; Legos et al. 2002). Treatment with OGD for 1 h induced 45–50 % of neuron death measured at 24 h after insult, in both WT and p38β KO groups (Fig. 4a), and again no significant difference in the degree of cell death was found between these two groups. OGD treatment induced 30–34 % neurite damage in both groups (Fig. 4b, c), and there was no significant difference in the degree of neurite degeneration between WT and p38β KO neurons. Similar to the results with L-glutamate and SNP, treatment of WT neurons with MW-181 or MW-108 led to a significant reduction in the neuronal death (Fig. 4a) and neurite degeneration (Fig. 4b) induced by OGD. Again, the neurites in the compound-treated cultures appeared smoother and had more neurite branches compared to OGD treatment in the absence of compounds (Fig. 4c).
p38α inhibition but not p38β KO protects neurons against OGD insult. DIV7 neurons on coverslips were pretreated for 1 h with either 60 μM MW-181 or MW-108, and the medium was removed and saved. After 1 h OGD treatment, the old culture media was then added back into appropriate wells for 24 h, followed by measurement of neuronal survival and neurite damage. a OGD induced ~50 % neuronal death in both p38β KO and WT neurons, with no significant differences between the two groups. In contrast, p38α inhibition by MW-181 or MW-108 significantly reduced the neuronal death after OGD insult. b OGD induced a similar degree of neurite damage (~33 %) in both p38β KO and WT neurons. In contrast, p38α inhibition by MW-181 or MW-108 significantly protected neurites against OGD-induced damage. c Representative photomicrographs of MAP2 immunocytochemistry show the morphology of neurons after 24 h. Arrows point to the appearance of damaged neurites induced by OGD in both p38β KO and WT neurons (****p < 0.0001 vs. control; #p < 0.05 vs. OGD; ##p < 0.01 vs. OGD, Bonferroni’s multiple comparison test). Data are from three independent experiments. Scale bar 10 μm
Discussion
In this study, we tested the respective contribution of the p38α and p38β MAPK isoforms in the neurodegeneration induced by three neurotoxic insults, and addressed the question if targeting a single kinase is sufficient to provide neuroprotective effects. Our results demonstrate that targeting p38α MAPK in neurons provides significant protection against three different neurotoxic insults, while loss of neuronal p38β MAPK does not affect the neurodegenerative responses to any of the three insults. These findings complement and extend our previous studies (Xing et al. 2011; Xing et al. 2013) that documented the importance of glial p38α MAPK in stressor-induced proinflammatory cytokine production and microglia-mediated neuron death. Altogether, our data demonstrate key roles of p38α MAPK signaling in both glial and neuronal responses that are linked to neuronal dysfunction, and continue to indicate the potential of this kinase as a CNS drug discovery target.
A number of previous studies have suggested that activation of p38 MAPK signaling in neurons in response to disease-relevant cellular stressors contributes to neuron dysfunction and neuron death, and that inhibition of p38 MAPK in the neuron is neuroprotective. For example, the p38 MAPK pathway has been implicated in neuron death induced by a number of agents, including excitotoxic stimuli (Cao et al. 2004; Semenova et al. 2007; Chaparro-Huerta et al. 2008), nerve injury (Wang et al. 2005; Wittmack et al. 2005), hypoxia/ischemia (Wang et al. 2002; Guo & Bhat 2007), and potassium deprivation (Yeste-Velasco et al. 2009). Neuronal p38 MAPK has also been reported to be involved in diabetic neuropathy (Sweitzer et al. 2004), hyperpolarization-activated and voltage-gated channel activation after injury (Wittmack et al. 2005; Wynne 2006), neurofilament pathology in amyotrophic lateral sclerosis (Ackerley et al. 2004), hyperalgesia and spinal pain (Svensson et al. 2005), activity-induced dendritic spine reduction (Sugiura et al. 2009), kainite-induced seizures and neuronal damage (Namiki et al. 2007), presynaptic serotonin transporter activity (Zhu et al. 2006), and various cytokine-mediated neuronal damage responses (Li et al. 2003; Wang et al. 2005; Chaparro-Huerta et al. 2008; Xing et al. 2011). Almost all the mechanistic data supporting the role of p38 in neuron dysfunction has been generated using small molecule p38 inhibitors such as SB203580. The commercial availability of SB203580 has led to its widespread use; however, SB203580 is not selective for the p38α versus p38β isoform or even for the p38 family alone. SB203580 and second-generation SB compounds such as SB202190 inhibit multiple other kinases, including casein kinase-1 delta, glycogen synthase kinase-3beta, protein kinase A, receptor interacting protein-2, and cyclin G-associated kinase (Clerk & Sugden 1998; Lali et al. 2000; Godl et al. 2003; Bain et al. 2007). Thus, despite the extensive evidence provided by work using SB compounds that inhibiting p38 is neuroprotective, the relative role of p38α and p38β in the neuroprotective responses and whether targeting a single kinase (p38α or p38β) is sufficient to exert the neuroprotective effects had not been tested. To address these important questions, we utilized our recently developed, highly selective p38α inhibitors, MW-181 and MW-108 (Watterson et al. 2013), as well as a global p38β knockout mouse. The use of these reagents in primary cortical neuron cultures allowed us to directly demonstrate for the first time the involvement of neuronal p38α, and not p38β, in the neurotoxic responses to glutamate, SNP, and OGD.
Glutamate is a major CNS excitatory neurotransmitter, but excessive glutamate release and overstimulation of glutamate receptors can induce excitotoxic neuron death. Activation of neuronal p38 MAPK signaling is a well-characterized response to glutamate insult, but few previous studies have explored the importance of p38α versus p38β in excitotoxic neuron death. One relevant study (Cao et al. 2004) implicated p38α in glutamate-induced damage of primary cerebellar granule neurons in culture through the use of a dominant-negative p38α construct, but did not explore p38β involvement because no p38β was detected in the cultured neurons. Our results demonstrating the involvement of p38α in primary cortical neurons are consistent with this study, and also show that p38β is not required for glutamate-induced neuron death.
Nitric oxide overproduction has been linked to neuron death in acute and chronic neurological disorders (Dawson & Dawson 1996; Dawson et al. 1996; Lee et al. 1999; Sattler et al. 1999; Arundine & Tymianski 2004). Several studies have utilized nitric oxide donors as a neurotoxic stimulus and p38 MAPK inhibitors such as SB203580 to explore the role of p38 MAPK in mediating neurodegenerative responses of cultured neurons to nitrosative stress. In general, these studies have demonstrated neuroprotection against nitric oxide insult, through several proposed mechanisms including reduced mitochondrial dysfunction and inhibition of peroxynitrite/reactive oxygen species formation (Ghatan et al. 2000; Lin et al. 2001; Bossy-Wetzel et al. 2004; Thomas et al. 2008; Nashida et al. 2011). However, as far as we are aware, no previous study tested specific isoforms of p38 MAPK in the neurotoxic responses.
We also investigated the role of p38 MAPK in neurotoxicity induced by OGD, a model of hypoxia-ischemia. Several previous reports have implicated p38 MAPK signaling in OGD-induced neurotoxicity through the use of the multi-kinase SB family of inhibitors. For example, SB239063 protects neuron-enriched forebrain cultures against OGD insult (Legos et al. 2002), SB203580 reduces OGD-induced death in PC12 cells (Li et al. 2009), and SB203580 or expression of an antisense p38 MAPK construct only in neuronal cells reduces oxidative stress and neuron death in hippocampal slice cultures (Lu et al. 2011). Importantly, a seminal paper (Guo & Bhat 2007) used p38 isoform-specific siRNAs to show that p38α and not p38β was a major contributor to OGD-induced death in the NSC34 motoneuron cell line. Our results reported here using highly specific p38α inhibitors in WT primary cortical neuron cultures and using neurons cultured from the p38β global knockout mouse are consistent with that study, and extend the results to primary neurons.
Although the dispensable role of p38β MAPK in cortical neurons in our study might be attributed to its relatively low expression in these cells compared to the expression of p38α MAPK, the data are consistent with our previous study showing that p38β KO microglia did not provide neuroprotection for co-cultured WT neurons upon lipopolysaccharide treatment (Xing et al. 2013). We did not explore other potential mechanisms or cell types where p38β MAPK may contribute. However, some studies have suggested that p38β MAPK may be more important in glial cells, rather than neurons. For example, studies using transient global ischemia, transient focal ischemia, and kainic acid-induced seizure models all showed a delayed activation of astrocytes with p38β MAPK immunoreactivity, but not p38α (Che et al. 2001; Piao et al. 2002; Piao et al. 2003). In addition, p38β was upregulated after injury in different cell types with different temporal profiles, with an early and transient induction of p38β in neurons, followed by a later and prolonged induction in astrocytes (Piao et al. 2003). Furthermore, the strong substrate preference of ATF2 by p38β compared to p38α and differential regulation by upstream kinases (Jiang et al. 1996) also suggest that the two kinases may act on different downstream targets and exert different functions in response to injury. The available data suggest a more restricted repertoire of functions of p38β MAPK that might be cell-specific and signaling-specific temporally and spatially in the CNS.
It should be noted that our understanding of the role of neuronal p38α and p38β MAPK signaling in neurotoxic responses is in its infancy. From the literature, it appears that the quantitative importance of the p38 MAPK pathway relative to other stress-induced signaling pathways can vary depending on the cell type, developmental status, toxic stimulus, timing of activation, and cell-cell interactions. For example, even in the same neuronal cell type at the same developmental stage, the involvement of p38 can be dependent on the neurotoxic stimulus. Specifically, p38 was reported to be involved in glutamate-induced death of cerebellar granule neurons, whereas death induced by withdrawal of trophic support involved JNK but not p38 (Cao et al. 2004). It is also clear that multiple signaling pathways can be induced in response to specific stimuli, and therefore the importance of one particular pathway may depend on the time points analyzed. Another important consideration is that glial p38 signaling in response to toxic stimuli can affect neuronal viability (Izumi et al. 2009; Xing et al. 2011), which can complicate the interpretation of results in slice cultures or in vivo models. Finally, discrepant results could also be due to technical issues, such as different culture conditions, animal strains, type or age of neurons, and/or stimulus paradigm. For example, the expression of the glutamate NMDA receptor subunit NR1 in neurons cultured for DIV7 is less than that in DIV11 neurons (Schubert & Piasecki 2001), the neuronal death induced by SNP is increased in DIV21 versus DIV14 neurons (Dawson et al. 1993), and hippocampal neurons are more vulnerable than cortical neurons to OGD treatment (Jiang et al. 2004). Nevertheless, even with the above caveats, our results using three different neurotoxic insults in the same type (primary cortical neurons) and age (DIV7) cultures clearly document that suppression of p38α with highly specific kinase inhibitors provides neuroprotection whereas lack of p38β in the knockout mouse has no effect. The availability of these reagents should allow future exploration of the importance of p38 MAPK signaling in other models of neuronal death.
Conclusions
Activation of neuronal p38 MAPK occurs in response to a number of disease-relevant stressors, and pharmacological inhibition of p38 MAPK is neuroprotective in both cell and animal models. However, the relative contribution of neuronal p38α and p38β to neurodegenerative responses had not been addressed previously. In this study, we used p38α- and p38β-specific reagents to demonstrate that inhibition of neuronal p38α provides significant neuroprotection against three different toxic insults, but that loss of neuronal p38β has no effect. These results demonstrate isoform-specific functions of these p38 kinases in the neuron, and support an important role of the p38α isoform in neurodegenerative responses to injury.
References
Ackerley S, Grierson AJ, Banner S et al (2004) p38alpha stress-activated protein kinase phosphorylates neurofilaments and is associated with neurofilament pathology in amyotrophic lateral sclerosis. Mol Cell Neurosci 26:354–364
Adams RH, Porras A, Alonso G et al (2000) Essential role of p38alpha MAP kinase in placental but not embryonic cardiovascular development. Mol Cell 6:109–116
Allen M, Svensson L, Roach M, Hambor J, McNeish J, Gabel CA (2000) Deficiency of the stress kinase p38alpha results in embryonic lethality: characterization of the kinase dependence of stress responses of enzyme-deficient embryonic stem cells. J Exp Med 191:859–870
Arundine M, Tymianski M (2004) Molecular mechanisms of glutamate-dependent neurodegeneration in ischemia and traumatic brain injury. Cell Mol Life Sci 61:657–668
Bachstetter AD, Van Eldik LJ (2010) The p38 MAP kinase family as regulators of proinflammatory cytokine production in degenerative diseases of the CNS. Aging Dis 1:199–211
Bain J, Plater L, Elliott M et al (2007) The selectivity of protein kinase inhibitors: a further update. Biochem J 408:297–315
Bakuridze K, Savli E, Gongadze N, Bas DB, Gepdiremen A (2009) Protection in glutamate-induced neurotoxicity by imidazoline receptor agonist moxonidine. Int J Neurosci 119:1705–1717
Beardmore VA, Hinton HJ, Eftychi C et al (2005) Generation and characterization of p38beta (MAPK11) gene-targeted mice. Mol Cell Biol 25:10454–10464
Borsch-Haubold AG, Pasquet S, Watson SP (1998) Direct inhibition of cyclooxygenase-1 and -2 by the kinase inhibitors SB 203580 and PD 98059. SB 203580 also inhibits thromboxane synthase. J Biol Chem 273:28766–28772
Bossy-Wetzel E, Talantova MV, Lee WD et al (2004) Crosstalk between nitric oxide and zinc pathways to neuronal cell death involving mitochondrial dysfunction and p38-activated K + channels. Neuron 41:351–365
Cao J, Semenova MM, Solovyan VT, Han J, Coffey ET, Courtney MJ (2004) Distinct requirements for p38alpha and c-Jun N-terminal kinase stress-activated protein kinases in different forms of apoptotic neuronal death. J Biol Chem 279:35903–35913
Chaparro-Huerta V, Flores-Soto ME, Gudino-Cabrera G, Rivera-Cervantes MC, Bitzer-Quintero OK, Beas-Zarate C (2008) Role of p38 MAPK and pro-inflammatory cytokines expression in glutamate-induced neuronal death of neonatal rats. Int J Dev Neurosci 26:487–495
Che Y, Yu YM, Han PL, Lee JK (2001) Delayed induction of p38 MAPKs in reactive astrocytes in the brain of mice after KA-induced seizure. Brain Res Mol Brain Res 94:157–165
Chen RW, Qin ZH, Ren M, Kanai H, Chalecka-Franaszek E, Leeds P, Chuang DM (2003) Regulation of c-Jun N-terminal kinase, p38 kinase and AP-1 DNA binding in cultured brain neurons: roles in glutamate excitotoxicity and lithium neuroprotection. J Neurochem 84:566–575
Choi DW, Maulucci-Gedde M, Kriegstein AR (1987) Glutamate neurotoxicity in cortical cell culture. J Neurosci 7:357–368
Clerk A, Sugden PH (1998) The p38-MAPK inhibitor, SB203580, inhibits cardiac stress-activated protein kinases/c-Jun N-terminal kinases (SAPKs/JNKs). FEBS Lett 426:93–96
Correa SA, Eales KL (2012) The Role of p38 MAPK and Its Substrates in Neuronal Plasticity and Neurodegenerative Disease. J Signal Transduct 2012:649079
Dawson VL, Dawson TM (1996) Nitric oxide neurotoxicity. J Chem Neuroanat 10:179–190
Dawson VL, Dawson TM, Bartley DA, Uhl GR, Snyder SH (1993) Mechanisms of nitric oxide-mediated neurotoxicity in primary brain cultures. J Neurosci 13:2651–2661
Dawson VL, Kizushi VM, Huang PL, Snyder SH, Dawson TM (1996) Resistance to neurotoxicity in cortical cultures from neuronal nitric oxide synthase-deficient mice. J Neurosci 16:2479–2487
Ghatan S, Larner S, Kinoshita Y, Hetman M, Patel L, Xia Z, Youle RJ, Morrison RS (2000) p38 MAP kinase mediates bax translocation in nitric oxide-induced apoptosis in neurons. J Cell Biol 150:335–347
Godl K, Wissing J, Kurtenbach A et al (2003) An efficient proteomics method to identify the cellular targets of protein kinase inhibitors. Proc Natl Acad Sci U S A 100:15434–15439
Guo G, Bhat NR (2007) p38alpha MAP kinase mediates hypoxia-induced motor neuron cell death: a potential target of minocycline's neuroprotective action. Neurochem Res 32:2160–2166
Hall-Jackson CA, Goedert M, Hedge P, Cohen P (1999) Effect of SB 203580 on the activity of c-Raf in vitro and in vivo. Oncogene 18:2047–2054
Izumi Y, Yamamoto N, Matsuo T, Wakita S, Takeuchi H, Kume T, Katsuki H, Sawada H, Akaike A (2009) Vulnerability to glutamate toxicity of dopaminergic neurons is dependent on endogenous dopamine and MAPK activation. J Neurochem 110:745–755
Jiang X, Mu D, Manabat C, Koshy AA, Christen S, Tauber MG, Vexler ZS, Ferriero DM (2004) Differential vulnerability of immature murine neurons to oxygen-glucose deprivation. Exp Neurol 190:224–232
Jiang Y, Chen C, Li Z, Guo W, Gegner JA, Lin S, Han J (1996) Characterization of the structure and function of a new mitogen-activated protein kinase (p38beta). J Biol Chem 271:17920–17926
Kaku DA, Goldberg MP, Choi DW (1991) Antagonism of non-NMDA receptors augments the neuroprotective effect of NMDA receptor blockade in cortical cultures subjected to prolonged deprivation of oxygen and glucose. Brain Res 554:344–347
Kawasaki H, Morooka T, Shimohama S, Kimura J, Hirano T, Gotoh Y, Nishida E (1997) Activation and involvement of p38 mitogen-activated protein kinase in glutamate-induced apoptosis in rat cerebellar granule cells. J Biol Chem 272:18518–18521
Lali FV, Hunt AE, Turner SJ, Foxwell BM (2000) The pyridinyl imidazole inhibitor SB203580 blocks phosphoinositide-dependent protein kinase activity, protein kinase B phosphorylation, and retinoblastoma hyperphosphorylation in interleukin-2-stimulated T cells independently of p38 mitogen-activated protein kinase. J Biol Chem 275:7395–7402
Lee JM, Zipfel GJ, Choi DW (1999) The changing landscape of ischaemic brain injury mechanisms. Nature 399:A7–A14
Legos JJ, McLaughlin B, Skaper SD, Strijbos PJ, Parsons AA, Aizenman E, Herin GA, Barone FC, Erhardt JA (2002) The selective p38 inhibitor SB-239063 protects primary neurons from mild to moderate excitotoxic injury. Eur J Pharmacol 447:37–42
Li CT, Zhang WP, Lu YB et al (2009) Oxygen-glucose deprivation activates 5-lipoxygenase mediated by oxidative stress through the p38 mitogen-activated protein kinase pathway in PC12 cells. J Neurosci Res 87:991–1001
Li Y, Liu L, Barger SW, Griffin WS (2003) Interleukin-1 mediates pathological effects of microglia on tau phosphorylation and on synaptophysin synthesis in cortical neurons through a p38-MAPK pathway. J Neurosci 23:1605–1611
Lin S, Zhang Y, Dodel R, Farlow MR, Paul SM, Du Y (2001) Minocycline blocks nitric oxide-induced neurotoxicity by inhibition p38 MAP kinase in rat cerebellar granule neurons. Neurosci Lett 315:61–64
Lu Q, Rau TF, Harris V, Johnson M, Poulsen DJ, Black SM (2011) Increased p38 mitogen-activated protein kinase signaling is involved in the oxidative stress associated with oxygen and glucose deprivation in neonatal hippocampal slice cultures. Eur J Neurosci 34:1093–1101
Molz S, Decker H, Dal-Cim T, Cremonez C, Cordova FM, Leal RB, Tasca CI (2008) Glutamate-induced toxicity in hippocampal slices involves apoptotic features and p38 MAPK signaling. Neurochem Res 33:27–36
Mudgett JS, Ding J, Guh-Siesel L, Chartrain NA, Yang L, Gopal S, Shen MM (2000) Essential role for p38alpha mitogen-activated protein kinase in placental angiogenesis. Proc Natl Acad Sci U S A 97:10454–10459
Namiki K, Nakamura A, Furuya M et al (2007) Involvement of p38alpha in kainate-induced seizure and neuronal cell damage. J Recept Signal Transduct Res 27:99–111
Nashida T, Takuma K, Fukuda S, Kawasaki T, Takahashi T, Baba A, Ago Y, Matsuda T (2011) The specific Na(+)/Ca(2+) exchange inhibitor SEA0400 prevents nitric oxide-induced cytotoxicity in SH-SY5Y cells. Neurochem Int 59:51–58
O'Keefe SJ, Mudgett JS, Cupo S et al (2007) Chemical genetics define the roles of p38alpha and p38beta in acute and chronic inflammation. J Biol Chem 282:34663–34671
Pi R, Li W, Lee NT et al (2004) Minocycline prevents glutamate-induced apoptosis of cerebellar granule neurons by differential regulation of p38 and Akt pathways. J Neurochem 91:1219–1230
Piao CS, Che Y, Han PL, Lee JK (2002) Delayed and differential induction of p38 MAPK isoforms in microglia and astrocytes in the brain after transient global ischemia. Brain Res Mol Brain Res 107:137–144
Piao CS, Yu YM, Han PL, Lee JK (2003) Dynamic expression of p38beta MAPK in neurons and astrocytes after transient focal ischemia. Brain Res 976:120–124
Sattler R, Xiong Z, Lu WY, Hafner M, MacDonald JF, Tymianski M (1999) Specific coupling of NMDA receptor activation to nitric oxide neurotoxicity by PSD-95 protein. Science 284:1845–1848
Schubert D, Piasecki D (2001) Oxidative glutamate toxicity can be a component of the excitotoxicity cascade. J Neurosci 21:7455–7462
Semenova MM, Maki-Hokkonen AM, Cao J, Komarovski V, Forsberg KM, Koistinaho M, Coffey ET, Courtney MJ (2007) Rho mediates calcium-dependent activation of p38alpha and subsequent excitotoxic cell death. Nat Neurosci 10:436–443
Strassburger M, Braun H, Reymann KG (2008) Anti-inflammatory treatment with the p38 mitogen-activated protein kinase inhibitor SB239063 is neuroprotective, decreases the number of activated microglia and facilitates neurogenesis in oxygen-glucose-deprived hippocampal slice cultures. Eur J Pharmacol 592:55–61
Sugiura H, Tanaka H, Yasuda S, Takemiya T, Yamagata K (2009) Transducing neuronal activity into dendritic spine morphology: new roles for p38 MAP kinase and N-cadherin. Neuroscientist 15:90–104
Svensson CI, Fitzsimmons B, Azizi S, Powell HC, Hua XY, Yaksh TL (2005) Spinal p38beta isoform mediates tissue injury-induced hyperalgesia and spinal sensitization. J Neurochem 92:1508–1520
Sweitzer SM, Medicherla S, Almirez R, Dugar S, Chakravarty S, Shumilla JA, Yeomans DC, Protter AA (2004) Antinociceptive action of a p38alpha MAPK inhibitor, SD-282, in a diabetic neuropathy model. Pain 109:409–419
Tabakman R, Jiang H, Schaefer E, Levine RA, Lazarovici P (2004) Nerve growth factor pretreatment attenuates oxygen and glucose deprivation-induced c-Jun amino-terminal kinase 1 and stress-activated kinases p38alpha and p38beta activation and confers neuroprotection in the pheochromocytoma PC12 Model. J Mol Neurosci MN 22:237–250
Tamura K, Sudo T, Senftleben U, Dadak AM, Johnson R, Karin M (2000) Requirement for p38alpha in erythropoietin expression: a role for stress kinases in erythropoiesis. Cell 102:221–231
Thomas T, Timmer M, Cesnulevicius K, Hitti E, Kotlyarov A, Gaestel M (2008) MAPKAP kinase 2-deficiency prevents neurons from cell death by reducing neuroinflammation—relevance in a mouse model of Parkinson's disease. J Neurochem 105:2039–2052
Wang X, Xu L, Wang H, Young PR, Gaestel M, Feuerstein GZ (2002) Mitogen-activated protein kinase-activated protein (MAPKAP) kinase 2 deficiency protects brain from ischemic injury in mice. J Biol Chem 277:43968–43972
Wang XJ, Kong KM, Qi WL, Ye WL, Song PS (2005) Interleukin-1 beta induction of neuron apoptosis depends on p38 mitogen-activated protein kinase activity after spinal cord injury. Acta Pharmacol Sin 26:934–942
Watterson DM, Grum-Tokars VL, Roy SM et al (2013) Development of novel chemical probes to address CNS protein kinase involvement in synaptic dysfunction. PLoS ONE 8:e66226
Wittmack EK, Rush AM, Hudmon A, Waxman SG, Dib-Hajj SD (2005) Voltage-gated sodium channel Nav1.6 is modulated by p38 mitogen-activated protein kinase. J Neurosci 25:6621–6630
Wynne P (2006) p38 mitogen-activated protein kinase: a novel modulator of hyperpolarization-activated cyclic nucleotide-gated channels and neuronal excitability. J Neurosci 26:11253–11254
Xie Z, Smith CJ, Van Eldik LJ (2004) Activated glia induce neuron death via MAP kinase signaling pathways involving JNK and p38. Glia 45:170–179
Xing B, Bachstetter AD, Van Eldik LJ (2011) Microglial p38alpha MAPK is critical for LPS-induced neuron degeneration, through a mechanism involving TNFalpha. Mol Neurodegener 6:84
Xing B, Bachstetter AD, Van Eldik LJ (2013) Deficiency in p38beta MAPK fails to inhibit cytokine production or protect neurons against inflammatory insult in in vitro and in vivo mouse models. PLoS ONE 8:e56852
Yeste-Velasco M, Folch J, Pallas M, Camins A (2009) The p38(MAPK) signaling pathway regulates neuronal apoptosis through the phosphorylation of the retinoblastoma protein. Neurochem Int 54:99–105
Zhu CB, Blakely RD, Hewlett WA (2006) The proinflammatory cytokines interleukin-1beta and tumor necrosis factor-alpha activate serotonin transporters. Neuropsychopharmacology 31:2121–2131
Acknowledgments
We thank Ms. Danielle Goulding for assistance with breeding and maintenance of the mouse colonies, and Dr. Gregory Bix, Dr. Aileen Marcelo, and Dr. Jill Roberts for technical advice on the OGD assay. We are also grateful to Dr. D. Martin Watterson for providing the p38α inhibitors MW-181 and MW-108, and to Dr. Stephen O’Keefe for p38β KO mice.
Competing Interests
The authors declare that they have no competing interests.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
Open Access This article is distributed under the terms of the Creative Commons Attribution License which permits any use, distribution, and reproduction in any medium, provided the original author(s) and the source are credited.
About this article
Cite this article
Xing, B., Bachstetter, A.D. & Van Eldik, L.J. Inhibition of Neuronal p38α, but not p38β MAPK, Provides Neuroprotection Against Three Different Neurotoxic Insults. J Mol Neurosci 55, 509–518 (2015). https://doi.org/10.1007/s12031-014-0372-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12031-014-0372-x