Abstract
Background
Cholangiocarcinoma (CCA) is a malignant disease of the epithelial cells of the intrahepatic and extrahepatic bile ducts. This review focuses on various aspects of cholangiocarcinoma such as its associated causes, treatment criteria, and more.
Methods
Although it remains a rare malignancy and is the second most common primary malignancy of the liver, the incidence is increasing, especially the incidence of intrahepatic CCA. Several studies suggested that surgery is not only solution; recently, reported targeted drugs may have the potential to become an alternative option.
Results
This review provides an overview of the current scenario of targeted therapies for CCA, which were tabulated with their current status and it also included its associated causes and its treatment criteria.
Conclusion
Because of its rarity and complexity, surgery remains the preferred treatment in resectable patients. Howerver, the studies suggested that the recently reported drugs may have the potential to be an alternative option for the treatment of CCA and related complications. In addition, this review will certainly benefit the community and researcher for further investigation.
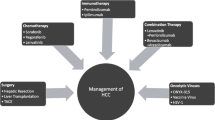
Graphical abstract

Similar content being viewed by others
Abbreviations
- CCA:
-
Cholangiocarcinoma
- iCCA:
-
Intrahepatic cholangiocarcinoma
- pCCA:
-
Perihilar cholangiocarcinoma
- dCCA:
-
Distal cholangiocarcinoma
- WHO:
-
World Health Organization
- AJCC:
-
American Joint Committee of Cancer
- eCCA:
-
Extrahepatic cholangiocarcinoma
- LNM:
-
Lymph node metastasis
- PSC:
-
Primary sclerosing cholangitis
- IDH:
-
Isocitrate dehydrogenase
- FGFR:
-
Fibroblast growth factor receptor
- VEGFR:
-
Vascular endothelial growth factor receptor
- HGFR:
-
Hepatocyte growth factor receptor
References
Katkhuda R, Chun YS. Epidemiology and risk factors. Intrahepatic Cholangiocarcinoma. 2019;1–0.
Rizvi S, Khan SA, Hallemeier CL, et al. Cholangiocarcinoma—evolving concepts and therapeutic strategies. Nat Rev Clin Oncol. 2018;15:95.
Abbasi A, Rahnemai-Azar AA, Ronnekleiv-Kelly SM, et al. Clinical presentation and diagnosis. iCCA. Springer, Cham; 2019. p. 11–20.
Razumilava N, Gores GJ. Combination of gemcitabine and cisplatin for biliary tract cancer: a platform to build on. J Hepatol. 2011;1(54):577–8.
Nakanuma Y, Sato Y, Harada K, et al. Pathological classification of intrahepatic cholangiocarcinoma based on a new concept. World J Hepatol. 2010;27(2):419.
Banales JM, Cardinale V, Carpino G, et al. Expert consensus document: cholangiocarcinoma: current knowledge and future perspectives consensus statement from the European Network for the Study of Cholangiocarcinoma (ENS-CCA). Nat Rev Gastroenterol Hepatol. 2016;13:261–80.
Okuda K, Nakanuma Y, Miyazaki M. Cholangiocarcinoma: recent progress. Part 1: epidemiology and etiology. J Gastroenterol Hepatol. 2002;17(10):1049–55.
Brücher BL, Jamall IS. Chronic inflammation evoked by pathogenic stimulus during carcinogenesis. 4open. 2019;2:8.
Tyson GL, El-Serag HB. Risk factors for cholangiocarcinoma Hepatol. 2011;54:173–84.
Cillo U, Fondevila C, Donadon M, et al. Surgery for cholangiocarcinoma. Liver Int. 2019;39:143–55.
Rizvi S, Borad MJ, Patel T, et al. Cholangiocarcinoma: molecular pathways and therapeutic opportunities. In: Seminars in liver disease, vol. 34, No. 4. NIH Public Access; 2014. p. 456.
Loosen SH, Roderburg C, Kauertz KL, et al. Elevated levels of circulating osteopontin are associated with a poor survival after resection of cholangiocarcinoma. J Hepatol. 2017;1(67):749–57.
Khan SA, Thomas HC, Davidson BR, et al. Cholangiocarcinoma Lancet. 2005;366:1303–14.
Aljiffry M, Abdulelah A, Walsh M, et al. Evidence-based approach to cholangiocarcinoma: a systematic review of the current literature. J Am Coll Surg. 2009;208:134–47.
Shaib YH, Davila JA, McGlynn K, et al. Rising incidence of intrahepatic cholangiocarcinoma in the United States: a true increase? J Hepatol. 2004;40:472–7.
Rahman SU, Sana MK, Tahir Z, et al. Paraneoplastic syndromes in cholangiocarcinoma. World J Hepatol. 2020;12:897.
Bertuccio P, Malvezzi M, Carioli G, et al. Global trends in mortality from intrahepatic and extrahepatic cholangiocarcinoma. J Hepatol. 2019;71:104–14.
Okabayashi T, Yamamoto J, Kosuge T, et al. A new staging system for mass-forming intrahepatic cholangiocarcinoma: analysis of preoperative and postoperative variables. Cancer. 2001;92:2374–83.
Amin MB, Greene FL, Edge SB, et al. The eighth edition AJCC cancer staging manual: continuing to build a bridge from a population-based to a more “personalized” approach to cancer staging. CA: Cancer J Clin. 2017;67:93–9.
Murakami Y, Uemura K, Sudo T, et al. Is para-aortic lymph node metastasis a contraindication for radical resection in biliary carcinoma? World J Surg. 2011;35:1085–93.
Nagino M, Ebata T, Yokoyama Y, et al. Evolution of surgical treatment for perihilar cholangiocarcinoma: a single-center 34-year review of 574 consecutive resections. Ann Surg. 2013;258:129–40.
Nagoya Surgical Oncology Group, Shimoyama Y, Fukami Y, Miyake H, et al. Prognostic impact of lymph node metastasis in distal cholangiocarcinoma. Br J Surg. 2015;102(4):399–406.
DeOliveira ML, Cunningham SC, Cameron JL, et al. holangiocarcinoma: thirty-one-year experience with 564 patients at a single institution. Ann Surg. 2007;245:755.
Kitagawa Y, Nagino M, Kamiya J, et al. Lymph node metastasis from hilar cholangiocarcinoma: audit of 110 patients who underwent regional and paraaortic node dissection. Ann Surg. 2001;233:385.
Komuta M, Govaere O, Vandecaveye V, et al. Histological diversity in cholangiocellular carcinoma reflects the different cholangiocyte phenotypes. Hepatol. 2012;55:1876–88.
Roskams T. Liver stem cells and their implication in hepatocellular and cholangiocarcinoma. Oncogene. 2006;25:3818–22.
Akiba J, Nakashima O, Hattori S, et al. linicopathologic analysis of combined hepatocellular-cholangiocarcinoma according to the latest WHO classification. Am J Surg Pathol. 2013;37:496–505.
Khan SA, Emadossadaty S, Ladep NG, et al. Rising trends in cholangiocarcinoma: is the ICD classification system misleading us? J Hepatol. 2012;56:848–54.
McLean L, Patel T. Racial and ethnic variations in the epidemiology of intrahepatic cholangiocarcinoma in the United States. Liver Int. 2006;26:1047–53.
Tyson GL, El-Serag HB. Risk factors for cholangiocarcinoma. Hepatology. 2011;54:173–84.
Shaib Y, El-Serag HB. The epidemiology of cholangiocarcinoma. In Seminars in liver disease 2004 May (Vol. 24, No. 02, pp. 115–125). Copyright© 2004 by Thieme Medical Publishers, Inc., 333 Seventh Avenue, New York, NY 10001, USA.
Everhart JE, Ruhl CE. Burden of digestive diseases in the United States Part III: liver, biliary tract, and pancreas. Gastroenterol. 2009;136:1134–44.
Khan SA, Davidson BR, Goldin RD, et al. Guidelines for the diagnosis and treatment of cholangiocarcinoma: an update. Gut. 2012;61:1657–69.
Welzel TM, Mellemkjaer L, Gloria G, et al. Risk factors for intrahepatic cholangiocarcinoma in a low-risk population: a nationwide case-control study. Int J Cancer. 2007;1(120):638–41.
Donato F, Gelatti U, Tagger A, et al. Intrahepatic cholangiocarcinoma and hepatitis C and B virus infection, alcohol intake, and hepatolithiasis: a case–control study in Italy. Cancer Causes Control. 2001;12:959–64.
El-Serag HB, Engels EA, Landgren O, et al. Risk of hepatobiliary and pancreatic cancers after hepatitis C virus infection: a population-based study of US veterans. Hepatol. 2009;49:116–23.
Shaib YH, El-Serag HB, Davila JA, et al. Risk factors of intrahepatic cholangiocarcinoma in the United States: a case-control study. Gastroenterol. 2005;128:620–6.
Lee TY, Lee SS, Jung SW, et al. Hepatitis B virus infection and intrahepatic cholangiocarcinoma in Korea: a case-control study. Am J Gastroenterol. 2008;103:1716–20.
Zhou YM, Yin ZF, Yang JM, et al. Risk factors for intrahepatic cholangiocarcinoma: a case-control study in China. World J Gastroenterol: WJG. 2008;14:632.
Yamamoto S, Kubo S, Hai S, et al. Hepatitis C virus infection as a likely etiology of intrahepatic cholangiocarcinoma. Cancer Sci. 2004;95:592–5.
Chapman MH, Webster GJ, Bannoo S, et al. Cholangiocarcinoma and dominant strictures in patients with primary sclerosing cholangitis; a 25-year single centre experience. Eur J Gastroenterol Hepatol. 2012;24:1051.
Chung BK, Karlsen TH, Folseraas T. Cholangiocytes in the pathogenesis of primary sclerosing cholangitis and development of cholangiocarcinoma. Biochimica et Biophysica Acta (BBA)-Molecular Basis of Disease. 2018;1864(4):1390–400.
Claessen MM, Vleggaar FP, Tytgat KM, et al. High lifetime risk of cancer in primary sclerosing cholangitis J Hepatol. 2009;50:158–64.
Boberg KM, Bergquist A, Mitchell S, et al. Cholangiocarcinoma in primary sclerosing cholangitis: risk factors and clinical presentation. Scand J Gastroenterol. 2002;37:1205–11.
European Association for The Study of The Liver. EASL Clinical Practice Guidelines: management of cholestatic liver diseases. J Hepatol. 2009;51:237–67.
Razumilava N, Gores GJ, Lindor KD. Cancer surveillance in patients with primary sclerosing cholangitis. Hepatology. 2011;54:1842–52.
Söreide K, Körner H, Havnen J, et al. Bile duct cysts in adults. Br J Plast Surg. 2004;91:1538–48.
Kaewpitoon N, Kaewpitoon SJ, Pengsaa P, et al. Opisthorchisviverrini: the carcinogenic human liver fluke. World J Gastroenterol. 2008;14:666–74.
Shin HR, Lee CU, Park HJ, et al. Hepatitis B and C virus, Clonorchissinensis for the risk of liver cancer: a case-control study in Pusan. Korea Int J Epidemiol. 1996;25:933–40.
Huang MH, Chen CH, Yen CM, et al. Relation of hepatolithiasis to helminthic infestation. J Gastroenterol Hepatol. 2005;20:141–6.
Devulapalli KK, Fidelman N, Soulen MC, et al. 90Y Radioembolization for hepatic malignancy in patients with previous biliary intervention: multicenter analysis of hepatobiliary infections. Radiology. 2018;288(3):774–81.
Palmer WC, Patel T. Are common factors involved in the pathogenesis of primary liver cancers? A meta-analysis of risk factors for intrahepatic cholangiocarcinoma. J Hepatol. 2012;57:69–76.
Welzel TM, Graubard BI, Zeuzem S, El-Serag HB, Davila JA, McGlynn KA. Metabolic syndrome increases the risk of primary liver cancer in the United States: a study in the SEER-Medicare database. Hepatol. 2011;54:463–71.
Benson AB, D’Angelica MI, Abbott DE, et al. Hepatobiliary Cancers, Version 2.2021, NCCN Clinical Practice Guidelines in Oncology. J Natl Compr Cancer Netw. 2021;19(5):541–65.
Bridgewater J, Galle PR, Khan SA, et al. Guidelines for the diagnosis and management of intrahepatic cholangiocarcinoma. J Hepatol. 2014;60(6):1268–89.
Khan SA, Davidson BR, Goldin RD, et al. Guidelines for the diagnosis and treatment of cholangiocarcinoma: an update. Gut. 2012;61(12):1657–69.
Valle J, Wasan H, Palmer DH, et al. Cisplatin plus gemcitabine versus gemcitabine for biliary tract cancer. N Engl J Med. 2010;362(14):1273–81.
Grassian AR, Pagliarini R, Chiang DY. Mutations of isocitrate dehydrogenase 1 and 2 in intrahepatic cholangiocarcinoma. Curr Opi Gastroenterol. 2014;30:295–302.
Turcan S, Rohle D, Goenka A, et al. IDH1 mutation is sufficient to establish the gliomahypermethylator phenotype. Nature. 2012;483:479–83.
Saha SK, Parachoniak CA, Ghanta KS, et al. Mutant IDH inhibits HNF-4α to block hepatocyte differentiation and promote biliary cancer. Nature. 2014;513:110–4.
Borger DR, Goyal L, Yau T, et al. Circulating oncometabolite 2-hydroxyglutarate is a potential surrogate biomarker in patients with isocitrate dehydrogenase-mutant intrahepatic cholangiocarcinoma. Clin Cancer Res. 2014;20:1884–90.
Kipp BR, Voss JS, Kerr SE, et al. Isocitrate dehydrogenase 1 and 2 mutations in cholangiocarcinoma. Human Pathol. 2012;43:1552–8.
Borger DR, Tanabe KK, Fan KC, et al. Frequent mutation of isocitrate dehydrogenase (IDH) 1 and IDH2 in cholangiocarcinoma identified through broad-based tumor genotyping. Oncologist. 2012;17:72.
Lowery MA, Burris HA III, Janku F, et al. Safety and activity of ivosidenib in patients with IDH1-mutant advanced cholangiocarcinoma: a phase 1 study. Lancet Gastroenterol Hepatol. 2019;4:711–20.
Rahnemai-Azar AA, Pawlik TM. Cholangiocarcinoma: shedding light on the most promising drugs in clinical development. Expert opinion on investigational drugs. 2021.
O’Rourke CJ, Munoz-Garrido P, Andersen JB. Molecular targets in cholangiocarcinoma. Hepatology. 2021;73:62–74.
Eder JP, Doroshow DB, Do KT, et al. Clinical Efficacy of Olaparib in IDH1/IDH2-Mutant Mesenchymal Sarcomas. JCO Precis Oncol. 2021;5:466–72.
Aitcheson G, Mahipal A, John BV. Targeting FGFR in intrahepatic cholangiocarcinoma [iCCA]: Leading the way for precision medicine in biliary tract cancer [BTC]? Expert Opin Investig Drugs. 2021;30(4):463–77.
Pauff JM, Papadopoulos KP, Janku F, et al. A phase I study of LY3410738, a first-in-class covalent inhibitor of mutant IDH1 in cholangiocarcinoma and other advanced solid tumors. J Clin Oncol. 2021;39(3): TPS350-TPS350.
Xu X, Zhao J, Xu Z, et al. Structures of human cytosolic NADP-dependent isocitrate dehydrogenase reveal a novel self-regulatory mechanism of activity. J Biol Chem. 2004;279:33946–57.
Turner N, Grose R. Fibroblast growth factor signalling: from development to cancer. Nat Rev Cancer. 2010;10:116–29.
Churi CR, Shroff R, Wang Y, et al. Mutation profiling in cholangiocarcinoma: prognostic and therapeutic implications. PloS one. 2014;9:e115383.
Wu YM, Su F, Kalyana-Sundaram S, et al. Identification of targetable FGFR gene fusions in diverse cancers. Cancer discov. 2013;3(6):636–47.
Busset MD, Shaib WL, Mody K, et al. 47P Derazantinib for patients with intrahepatic cholangiocarcinoma harboring FGFR2 fusions/rearrangements: primary results from the phase II study FIDES-01. Ann Oncol. 2021;32:S376.
Botrus G, Raman P, Oliver T, et al. Infigratinib (BGJ398): an investigational agent for the treatment of FGFR-altered intrahepatic cholangiocarcinoma. Expert Opin Investig Drugs. 2021;30(4):309–16.
Abou-Alfa GK, Sahai V, Hollebecque A, et al. Pemigatinib for previously treated, locally advanced or metastatic cholangiocarcinoma: a multicentre, open-label, phase 2 study. The Lancet Oncol. 2020;21:671–84.
Rizzo A, Ricci AD, Brandi G. Pemigatinib: hot topics behind the first approval of a targeted therapy in cholangiocarcinoma. Cancer Treat Res Commun. 2021;18:100337.
Dietrich D. FGFR-targeted therapy in head and neck carcinomas. HNO. 2021;69:172–84.
Weaver A, Bossaer JB. Fibroblast growth factor receptor (FGFR) inhibitors: A review of a novel therapeutic class. J Oncol Pharm Pract. 2021;27(3):702–10.
Rizzo A, Ricci AD, Brandi G. Futibatinib, an investigational agent for the treatment of intrahepatic cholangiocarcinoma: Evidence to date and future perspectives. Expert Opin Investig Drugs. 2021;30(4):317–24.
https://pubchem.ncbi.nlm.nih.gov/compound/Fisogatinib [accessed on 1305/2021].
Nault JC, Villanueva A. Biomarkers for hepatobiliary cancers Hepatol. 2021;73:115–27.
Paliogiannis P, Attene F, Cossu A, et al. Impact of tissue type and content of neoplastic cells of samples on the quality of epidermal growth factor receptor mutation analysis among patients with lung adenocarcinoma. Mol Med Rep. 2015;12:187–91.
Han W, Lo HW. Landscape of EGFR signaling network in human cancers: biology and therapeutic response in relation to receptor subcellular locations. Cancer Lett. 2012;318:124–34.
Wieduwilt MJ, Moasser M. The epidermal growth factor receptor family: biology driving targeted therapeutics. Cell Mol Life Sci. 2008;65(10):1566–84.
Samatiwat P, Tabtimmai L, Suphakun P, et al. The Effect of the EGFR-Targeting Compound 3-[(4-Phenylpyrimidin-2-yl) Amino] Benzene-1-Sulfonamide (13f) against Cholangiocarcinoma Cell Lines. Asian Pac J Cancer Prev. 2021;22:381–90.
https://pubchem.ncbi.nlm.nih.gov/compound/Lapatinib [accessed on 13/05/2021].
Sahu R, Mishra R, Majee C. An insight into primary biliary cholangitis and its recent advances in treatment: semi-synthetic analogs to combat ursodeoxycholic-acid resistance. Expert Rev Gastroenterol Hepatol. 2020;14(10):985–98.
Yoshikawa D, Ojima H, Kokubu A, et al. Vandetanib (ZD6474), an inhibitor of VEGFR and EGFR signalling, as a novel molecular-targeted therapy against cholangiocarcinoma. Br J Cancer. 2009;100:1257–66.
Sardar M, Shroff RT. Biliary cancer: gateway to comprehensive molecular profiling. Clin Adv Hematol Oncol: H&O. 2021;19:27–34.
Shitara K, Yamanaka T, Denda T, et al. REVERCE: a randomized phase II study of regorafenib followed by cetuximab versus the reverse sequence for previously treated metastatic colorectal cancer patients. Ann Oncol. 2019;30(2):259–65.
Martinelli E, De Palma R, Orditura M, et al. Anti-epidermal growth factor receptor monoclonal antibodies in cancer therapy. Clin Exp Immunol. 2009;158(1):1–9.
Hirata H, Kuwatani M, Nakajima K, et al. Near-infrared photoimmunotherapy (NIR-PIT) on cholangiocarcinoma using a novel catheter device with light emitting diodes. Cancer Sci. 2021;112:828.
Yarlagadda B, Kamatham V, Ritter A, et al. Trastuzumab and pertuzumab in circulating tumor DNA ERBB2-amplified HER2-positive refractory cholangiocarcinoma. NPJ JCO Precis Oncol. 2019;3:1–5.
Yoshikawa D, Ojima H, Iwasaki M, et al. Clinicopathological and prognostic significance of EGFR, VEGF, and HER2 expression in cholangiocarcinoma. Br J Cancer. 2008;98.
Tang D, Nagano H, Yamamoto H, et al. Angiogenesis in cholangiocellular carcinoma: expression of vascular endothelial growth factor, angiopoietin-1/2, thrombospondin-1 and clinicopathological significance. Oncol reports. 2006;15(3):525–32.
Amin NE, Hansen TF, Fernebro E, et al. Randomized phase II trial of combination chemotherapy with panitumumab or bevacizumab for patients with inoperable biliary tract cancer without KRAS exon 2 mutations. Int J Cancer. 2021;149(1):119–26.
Wang M, Chen Z, Guo P, et al. Therapy for advanced cholangiocarcinoma: current knowledge and future potential. J Cell Mol Med. 2021;25:618–28.
Di Federico A, Rizzo A, Ricci AD, et al. Nivolumab: an investigational agent for the treatment of biliary tract cancer. Expert Opin Investig Drugs. 2021;30(4):325–32.
Mao J, Yang X, Lin J, et al. Apatinib as non-first-line treatment in patients with Intrahepatic Cholangiocarcinoma. J Cancer. 2021;12:1555.
Rahnemai-Azar AA, Weisbrod AB, Dillhoff M, et al. Intrahepatic cholangiocarcinoma: current management and emerging therapies. Expert Rev Gastroenterol Hepatol. 2017;11:439–49.
Sahu R, Mishra R, Kumar R, et al. Pyridine moiety: an insight into recent advances in treatment of cancer. Mini-Rev Med Chem. 2021.
Lu M, Qin X, Zhou Y, et al. Long non-coding RNA LINC00665 promotes gemcitabine resistance of cholangiocarcinoma cells via regulating EMT and stemness properties through miR-424-5p/BCL9L axis. Cell Death Dis. 2021;12:1–7.
Fischmann TO, Smith CK, Mayhood TW, et al. Crystal structures of MEK1 binary and ternary complexes with nucleotides and inhibitors. Biochemistry. 2009;48(12):2661–74.
Halle BR, Johnson DB. Defining and Targeting BRAF Mutations in Solid Tumors. Curr Treat Options Oncol. 2021;22:1–5.
O’Neil BH, Goff LW, Kauh JS, et al. Phase II study of the mitogen-activated protein kinase 1/2 inhibitor selumetinib in patients with advanced hepatocellular carcinoma. J Clin Oncol. 2011;29:2350.
George TJ, DeRemer DL, Lee JH, et al. Phase II trial of the PARP inhibitor, niraparib, in BRCA1-Associated Protein 1 (BAP1) and other DNA damage response (DDR) pathway deficient neoplasms including cholangiocarcinoma. J Clin Oncol. 2021;39:3, TPS354-TPS354.
Acknowledgements
The authors would like to thank Prof. (Dr.) Pramod Kumar Sharma, Dean, School of Medical and Allied Sciences, Galgotias University, Greater Noida (201310), for providing technical supports.
Author information
Authors and Affiliations
Contributions
I, Rakesh Sahu (corresponding author), have done the entire work. The preparation of this manuscript is contributed by Dr. Praveen Sharma and Dr. Ajay Kumar.
Ethics declarations
Conflict of Interest
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Sahu, R., Sharma, P. & Kumar, A. An Insight into Cholangiocarcinoma and Recent Advances in its Treatment. J Gastrointest Canc 54, 213–226 (2023). https://doi.org/10.1007/s12029-021-00728-5
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12029-021-00728-5