Abstract
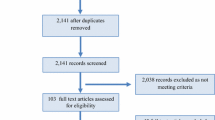
Conducted Electrical Weapons (CEWs) are being used as the preferred non-lethal force option for police and special forces worldwide. This new technology challenges an exposed opponent similarly to the way they would be challenged by physical exercise combined with emotional stress. While adrenergic and metabolic effects have been meta-analyzed and reviewed, there has been no systematic review of the effects of CEWs on skeletal and cardiac muscle. A systematic and careful search of the MedLine database was performed to find publications describing pathophysiological cardiac and skeletal muscle effects of CEWs. For skeletal muscle effects, we analyzed all publications providing changes in creatine kinase, myoglobin and potassium. For cardiac effects, we analyzed reported troponin changes and arrhythmias related to short dart-to-heart-distances. Conducted electrical weapons satisfy all relevant electrical safety standards and there are, to date, no proven electrocution incidents caused by CEWs. A potential cardiovascular risk has been recognized by some of the experimental animal data. The effects on the heart appear to be limited to instances when there is a short dart-to-heart-distance. The effect on the skeletal muscle system appears to be negligible. A responsible use of a CEW on a healthy adult, within the guidelines proposed by the manufacturer, does not imply a significant health risk for that healthy adult.

Similar content being viewed by others
References
Koscove EM. The Taser weapon: a new emergency medicine problem. Ann Emerg Med. 1985;14:1205–8.
Stopyra JP, Winslow JE, Fitzgerald DM, Bozeman WP. Intracardiac electrocardiographic assessment of precordial TASER shocks in human subjects: a pilot study. J Forensic Legal Med. 2017;52:70–4.
Underwriters Laboratories. UL standard for electric fence controllers. In: Laboratories U, UL69, vol UL 69, 10th ed. Northbrook: Underwriters Laboratories; 2009.
Nimunkar AJ, Webster JG. Safety of pulsed electric devices. Physiol Meas. 2009;30:101–14.
International Electrotechnical Commission. Household and similar electrical appliances – Safety – IEC 60335-2-76: Particular requirements for electric fence energizers. 2.1 ed: IEC, Geneva, Switzerland; 2006.
Nanthakumar K, Billingsley IM, Masse S, Dorian P, Cmeron D, Chauhan VS, et al. Cardiac electrophysiological consequences of neuromuscular incapacitating device discharges. J Am Coll Cardiol. 2006;48:798–804.
Walcott GP, Kroll MW, Ideker RE. Ventricular fibrillation threshold of rapid short pulses. Conf Proc IEEE EMBC. 2011;33:255–8.
Rahko PS. Evaluation of the skin-to-heart distance in the standing adult by two-dimensional echocardiography. J Am Soc Echocardiogr. 2008;21:761–4.
Horowitz LN, Spear JF, Moore EN. Relation of the endocardial and epicardial ventricular fibrillation thresholds of the right and left ventricle. Am J Cardiol. 1981;48:698–701.
Horowitz LN, Spear JF, Moore EN. Relationship of the endocardial and epicardial ventricular fibrillation thresholds of the right and left ventricle. Am J Cardiol. 1981;48:698–701.
Horowitz LN, Spear JF, Josephson ME, Kastor JA, Moore EN. The effects of coronary artery disease on the ventricular fibrillation threshold in man. Circulation. 1979;60:792–7.
Allison JS, Qin H, Dosdall DJ, Huang J, Newton JC, Smith WM, et al. The transmural activation sequence in porcine and canine left ventricle is markedly different during long-duration ventricular fibrillation. J Cardiovasc Electrophysiol. 2007;18:1306–12.
Brave MA, Lakkireddy DR, Kroll MW. Validity of the small swine model for human electrical safety risks. Conf Proc IEEE EMBC. 2016;38:2343–8.
Hamlin RL, Burton RR, Leverett SD, Burns JW. Ventricular activation process in minipigs. J Electrocardiol. 1975;8:113–6.
Kano M, Toyoshi T, Iwasaki S, Kato M, Shimizu M, Ota T. QT PRODACT: usability of miniature pigs in safety pharmacology studies: assessment for drug-induced QT interval prolongation. J Pharmacol Sci. 2005;99:501–11.
Walcott GP, Kroll MW, Ideker RE. Ventricular fibrillation: are swine a sensitive species? J Interv Card Electrophysiol. 2015;42:83–9.
Valentino DJ, Walter RJ, Dennis AJ, Margeta B, Starr F, Nagy KK, et al. Taser X26 discharges in swine: ventricular rhythm capture is dependent on discharge vector. J Trauma. 2008;65:1478–85. discussion 1485-77
Geddes LA, Cabler P, Moore AG, Rosborough J, Tacker WA. Threshold 60-Hz current required for ventricular fibrillation in subjects of various body weights. IEEE Trans Biomed Eng. 1973;20:465–8.
Han J, Garciadejalon P, Moe GK. Adrenergic effects on ventricular vulnerability. Circ Res. 1964;14:516–24.
Papp JG, Szekeres L. Analysis of the mechanism of adrenergic actions on ventricular vulnerability. Eur J Pharmacol. 1968;3:15–26.
Wu JY, Sun H, O'Rourke AP, Huebner SM, Rahko PS, Will JA, et al. Taser blunt probe dart-to-heart distance causing ventricular fibrillation in pigs. IEEE Trans Biomed Eng. 2008;55:2768–7.
Lakkireddy D, Wallick D, Verma A, Ryschon K, Kowalewski W, Wazni O, et al. Cardiac effects of electrical stun guns: does position of barbs contact make a difference? Pacing Clin Electrophysiol. 2008;31:398–408.
Lakkireddy D, Wallick D, Ryschon K, Chung MK, Butany J, Martin D, et al. Effects of cocaine intoxication on the threshold for stun gun induction of ventricular fibrillation. J Am Coll Cardiol. 2006;48:805–11.
Kroll MW, Lakkireddy D, Rahko PS, Panescu D. Ventricular fibrillation risk estimation for conducted electrical weapons: critical convolutions. Conf Proc IEEE Eng Med Biol Soc. 2011;33:271–7.
Walcott GP, Kroll M, Ideker RE. Relationship of the swine to the human ventricular fibrillation threshold. J Interv Card Electrophysiol. 2015;42:83–9.
Panescu D, Kroll M, Brave M. Cardiac fibrillation risks with TASER conducted electrical weapons. Conf Proc IEEE EMBC. 2015;37:323–9.
Kunz SN, Aronshtam J, Trankler HR, Kraus S, Graw M, Peschel O. Cardiac changes due to electronic control devices? A computer-based analysis of electrical effects at the human heart caused by an ECD pulse applied to the body's exterior. J Forensic Sci. 2014;59:659–64.
Sun H, Haemmerich D, Rahko PS, Webster JG. Estimating the probability that the Taser directly causes human ventricular fibrillation. J Med Eng Technol. 2010;34:178–91.
Panescu D, Kroll MW, Efimov IR, Sweeney JD. Finite element modeling of electric field effects of TASER devices on nerve and muscle. Conf Proc IEEE EMBC. 2006;28:1277–9.
Stratbucker RA, Kroll MW, McDaniel W, Panescu D. Cardiac current density distribution by electrical pulses from TASER devices. Conf Proc IEEE EMBC. 2006;28:6305–7.
Panescu D, Kroll MW, Stratbucker RA. Theoretical possibility of ventricular fibrillation during use of TASER neuromuscular incapacitation devices. Conf Proc IEEE EMBC. 2008;30:5671–4.
Leitgeb N, Niedermayr F, Neubauer R, Loos G. Numerically simulated cardiac exposure to electric current densities induced by TASER X-26 pulses in adult men. Phys Med Biol. 2010;55:6187–95.
Dawes DM, Ho JD, Reardon RF, Miner JR. The cardiovascular, respiratory, and metabolic effects of a long duration electronic control device exposure in human volunteers. Forensic Sci Med Pathol. 2010;6:268–74.
Ho JD, Dawes DM, Reardon RF, Strote SR, Kunz SN, Nelson RS, et al. Human cardiovascular effects of a new generation conducted electrical weapon. Forensic Sci Int. 2011;204:50–7.
Ideker RE, Dosdall DJ. Can the direct cardiac effects of the electric pulses generated by the TASER X26 cause immediate or delayed sudden cardiac arrest in normal adults? Am J Forensic Med Pathol. 2007;28:195–201.
Bozeman WP, Hauda WE 2nd, Heck JJ, Graham DD Jr, Martin BP, Winslow JE. Safety and injury profile of conducted electrical weapons used by law enforcement officers against criminal suspects. Ann Emerg Med. 2009;53:480–9.
Kim PJ, Franklin WH. Ventricular fibrillation after stun-gun discharge. N Engl J Med. 2005;353:958–9.
Schwarz ES, Barra M, Liao MM. Successful resuscitation of a patient in asystole after a TASER injury using a hypothermia protocol. Am J Emerg Med. 2009;27(515):e511–2.
Zipes DP. Sudden cardiac arrest and death following application of shocks from a TASER electronic control device. Circulation. 2012;125:2417–22.
Zipes D. Are you tasing me? TASERS can cause fatal [ventricular tachy] arrhythmias: HRS debate. 2010. http://www.heartrhythmondemand.org/.2009. Accessed 15 Jan 2010.
Naunheim RS, Treaster M, Aubin C. Ventricular fibrillation in a man shot with a Taser. Emerg Med. 2010;27:645–6.
Swerdlow CD, Fishbein MC, Chaman L, Lakkireddy DR, Tchou P. Presenting rhythm in sudden deaths temporally proximate to discharge of TASER conducted electrical weapons. Acad Emerg Med. 2009;16:726–39.
Kroll MW, Fish RM, Calkins H, Halperin H, Lakkireddy D, Panescu D. Defibrillation success rates for electrically-induced fibrillation: hair of the dog. Conf Proc IEEE EMBC. 2012;34:689–93.
Haouzi P, Ahmadpour N, Bell HJ, Artman S, Banchs J, Samii S, et al. Breathing patterns during cardiac arrest. J Appl Physiol. 2010;109:405–11.
Zuercher M, Ewy GA, Otto CW, HJilwig RW, Bobrow BJ, Clark L, et al. Gasping in response to basic resuscitation efforts: observation in a swine model of cardiac arrest. Crit Care Res Prac. 2010;10:1–7.
Goudge S. The health effects of conducted energy weapons: The Expert Panel on the Medical and Physiological Impacts of Conducted Energy Weapons. Council of Canadian Academies. 2013. http://www.scienceadvice.ca/en/assessments/completed/cew.aspx. Accessed 2 May 2017.
Kroll MW, Lakkireddy DR, Stone JR. Luceri RM. TASER electronic control devices and cardiac arrests: coincidental or causal? Circulation. 2014;129:93–100.
Vilke GM, Sloane CM, Bouton KD, Kolkhorst FW, Levine SD, NeumanTS, et al. Physiological effects of a conducted electrical weapon on human subjects. Ann Emerg Med. 2007;50:569–75.
Sloane CM, Chan TC, Levine SD, Dunford JV, Neuman T, Vilke GM. Serum troponin I measurement of subjects exposed to the Taser X-26. J Emerg Med. 2008;35:29–32.
Dawes D, Ho J, Miner J. The neuroendocrine effects of the TASERX26®: a brief report. Forensic Sci Int. 2009;183:14–9.
Ho JD, Dawes DM, Heegaard WG, Calkins HG, Moscati RM, Miner JR. Absence of electrocardiographic change after prolonged application of a conducted electrical weapon in physically exhausted adults. J Emerg Med. 2011;41:466–72.
Moscati R, Ho JD, Dawes DM, Miner JR. Physiologic effects of prolonged conducted electrical weapon discharge in ethanol-intoxicated adults. Am J Emerg Med. 2010;28:582–7.
Ho J, Dawes D, Nelson RS, Lundin EJ, Ryan FJ. Acidosis and catecholamine evaluation following simulated enforcement `use of force´ encounters. Acad Emerg Med. 2010;17:60–8.
VanMeenen KM, Cherniack NS, Bergen MT, Gleason LA, Teichman R, Servatius RJ. Cardiovascular evaluation of electronic control device exposure in law enforcement trainees: a multisite study. J Occup Environ Med. 2010;52:197–201.
Ho JD, Miner JR, Lakireddy DR, Bultman LL, Heegard WG. Cardiovascular and physiologic effects of conducted electrical weapon discharge in resting adults. Acad Emerg Med. 2006;13:589–95.
FDA Modernization Act of 1997: modifications to the list of recognized standards; availability; withdrawal of draft guidance "Use of IEC 60601 standards; medical electrical equipment"--FDA. Notice. Federal register. 1998;63:55617–55630.
Bills E. Risk management for IEC 60601-1 third edition. Biomed Instrum Technol. 2006;40:390–2.
Lakkireddy D, Khasnis A, Antenacci J, Ryshcon K, Chung MK, Wallick D, et al. Do electrical stun guns (TASER X26) affect the functional integrity of implanted pacemakers and defibrillators? Europace. 2007;9:551–6.
Vanga S, Vacek J, Berenbom L, Lakkireddy D. Conducted electrical weapons and implantable cardiac devices. In: Kroll M, Ho J, editors. TASER conducted electrical weapons: physiology, pathology, and law. New York City: Springer-Kluwer; 2009. p. 223–34.
Lakkireddy D, Biria M, Baryun E, Berenbom L, Pimentel R, Emert M, et al. Can electrical-conductive weapons (TASER®) alter the functional integrity of pacemakers and defibrillators and cause rapid myocardial capture? Heart Rhythm. 2008;5:S97.
Vanga SR, Bommana S, Kroll MW, Swerdlow C, Lakkireddy D. TASER conducted electrical weapons and implanted pacemakers and defibrillators. Conf Proc IEEE Eng Med Biol Soc. 2009;31:3199–204.
Cao M, Shinbane JS, Gillberg JM, Saxon LA, Swerdlow CD. Taser-induced rapid ventricular myocardial capture demonstrated by pacemaker intracardiac electrograms. J Cardiovasc Electrophysiol. 2007;18:876–9.
Haegeli LM, Sterns LD, Adam DC, Leather RA. Effect of a Taser shot to the chest of a patient with an implantable defibrillator. Heart Rhythm. 2006;3:339–41.
Paninski RJ, Marshall ME. Link MS. ICD oversensing caused by TASER. J Cardiovasc Electrophysiol. 2013;24:101.
Khaja A, Govindarajan G, McDaniel W, Flaker G. Cardiac safety of conducted electrical devices in pigs and their effect on pacemaker function. Am J Emerg Med. 2011;29:1089–96.
Calton R, Cameron D, Masse S, Nanthakumar K. Images in cardiovascular medicine. Duration of discharge of neuromuscular incapacitating device and inappropriate implantable cardioverter-defibrillator detections. Circulation. 2007;115:e472–4.
Adedipe A, Maher P, Strote J. Injuries associated with law enforcement use of force. Trauma. 2012;15:99–106.
Strote J, Walsh M, Angelidids M, Basta A, Hutson HR. Conducted electrical weapon use by law enforcement: an evaluation of safety and injury. J Trauma. 2010;68:1239–46.
Jauchem JR, Cook MC, Beason CW. Blood factors of Susscrofa following a series of three TASER electronic control device exposures. Forensic Sci Int. 2008;175:166–70.
Jauchem JR, Sherry CJ, Fines DA, Cook MC. Acidosis, lactate, electrolytes, muscle enzymes, and other factors in the blood of Susscrofa following repeated TASER exposures. Forensic Sci Int. 2006;161:20–30.
Jauchem JR, Beason CW, Cook MC. Acute effects of an alternative electronic-control-device waveform in swine. Forensic Sci Med Pathol. 2009;5:2–10.
Dennis AJ, Valentino DJ, Walter RJ, Nagy KK, Winners J, Bokhari F, et al. Acute effects of TASER X26 discharges in swine model. J Trauma. 2007;63:581–90.
Dawes DM, Ho JD, Sweeney JD, Lundin EJ, Kunz SN, Miner JR. The effect of an electronic control device on muscle injury as determined by creatine kinase enzyme. Forensic Sci Med Pathol. 2011;7:3–8.
Ho JD, Dawes DM, Chang RJ, Nelson RS, Miner JR. Physiologic effects of a new generation conducted electrical weapon on human volunteers. J Emerg Med. 2014;46:428–35.
Sanford JM, Jacobs GJ, Roe EJ, Terndrup TE. Two patients subdued with a TASER device: cases and review of complications. J Emerg Med. 2011;40:28–32.
Ho JD. Dawes DM. TASER device-induced rhabdomyolysis is unlikely. J Emerg Med. 2011;40:68–9.
Dawes D, Ho J, Readon F, Strote S, Nelson R, Lundin E, et al. The respiratory, metabolic, and neuroendocrine effects of a new generation electronic control device. Forensic Sci Int. 2010;207:55–60.
Ho J, Dawes D, Bultman L, Moscati R, Janchar T, Miner J. Prolonged TASER use on exhausted humans does not worsen markers of acidosis. Am J Emerg Med. 2009;27:413–8.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
This paper is a result of literature research, which was not funded. SNK, HC, and MWK are members of the scientific medical advisory board of Axon Int. (fka TASER). MWK also is on Axon corporate board. HC & MWK have been expert witnesses in law-enforcement litigation and HC has been an expert witness in cases of arrest related deaths involving CEWs.
J. Adamec has no conflict to declare.
Rights and permissions
About this article
Cite this article
Kunz, S.N., Calkins, H., Adamec, J. et al. Cardiac and skeletal muscle effects of electrical weapons. Forensic Sci Med Pathol 14, 358–366 (2018). https://doi.org/10.1007/s12024-018-9997-3
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12024-018-9997-3